Abstract
Introduction and hypothesis
We sought to systematically review the literature regarding the effect of postoperative restrictions on clinical outcomes after pelvic surgery.
Methods
English-language articles were identified by a MEDLINE and Cochrane Central Register of Controlled Trials search from inception to July 2010. We used key words describing various gynecologic surgical procedures and postoperative activities, including mobility, lifting, work, coitus, and exercise. Randomized and nonrandomized studies comparing interventions with outcomes of interest were included.
Results
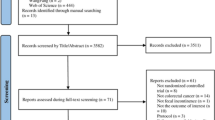
The literature search yielded of 3,491 articles; 115 full-text articles were reviewed, and 38 met eligibility criteria and are reported and analyzed here. Our analysis revealed that expedited discharge protocols and early postoperative feeding and catheter removal result in shorter hospital stay without negative health outcomes. However, there are limited data to guide many other aspects of postoperative care, particularly regarding exercise and resumption of sexual activity after surgery.
Conclusions
There is good evidence to support early postoperative feeding and catheter removal after pelvic surgery. There are limited data to guide many other aspects of postoperative care.


Similar content being viewed by others
References
Practice Bulletins – American College of Obstetricians and Gynecologists. Available at: http://www.acog.org/member_access/lists/practbul.cfm
Minig L, Trimble EL, Sarsotti C, Sebastiani MM, Spong CY (2009) Building the evidence base for postoperative and postpartum advise. Obstet Gynecol 114:892–900
Owens DK, Lohr KN, Atkins D et al. (2010) AHRQ series paper 5: grading the strength of a body of evidence when comparing medical interventions–agency for healthcare research and quality and the effective health-care program. J Clin Epidemiol 63(5):513–523
Atkins D, Best D, Briss PA, Eccles M, Falck-Ytter Y, Flottorp S et al. (2004) Grading quality of evidence and strength of recommendations. BMJ 328:1490
Jarvis SK, Hallam TK, Lujic S, Abbott JA, Vancaillie TG (2005) Peri-operative physiotherapy improves outcomes for women undergoing incontinence and or prolapse surgery: results of a randomised controlled trial. Aust N Z J Obstet Gynaecol 45(4):300–303
Maughan K, Clarke D (2001) The effect of a clinical nurse specialist in gynecological oncology on quality of life and sexuality. J Clin Nurs 10:221–229
Bradford A, Meston C (2007) Sexual outcomes and satisfaction with hysterectomy: influence of patient education. J Sex Med 4:106–114
Bergman A, Matthews L, Ballard CA (1987) Bladder training after surgery for stress urinary incontinence: is it necessary? Obstet Gynecol 70:909–912
DunnTS SJ, Forshner D (2003) Are in-dwelling catheters necessary for 24 hours after hysterectomy? Am J Obstet Gynecol 189:435–437
Alessandri F, Mistrangelo E, Lijoi D, Ferrero S, Ragni N (2006) A prospective, randomized trial comparing immediate versus delayed catheter removal following hysterectomy. Acta Obstetricia et Gynecologica 85:716–720
Ottesen M, Sorenson M, Kehlet H, Otteson B (2003) Short convalescence after vaginal prolapse surgery. Acta Obstet Gynecol Scan 82:359–366
Gerten KA, Richter HE, Wheeler TL, Pair LS, Burgio KL, Redden DT, Varner E, Hibner M (2008) Intraabdominal pressure changes associated with lifting: implications for postoperative activity restrictions. Am J Obstet Gynecol 198:306e1–306e5
Babski-Reeves KL, Tran GM (2006) Efficacy of an assistive intervention for abdominal surgery patients in postoperative care. Disabil Rehabil Assist Technol 1:191–197
Dawes HA, Docherty T, Traynor I, Gilmore DH, Jardine AG, Knill-Jones R (2007) Specialist nurse supported discharge in gynaecology: a randomised comparison and economic evaluation. Eur J Obstet Gynecol Reprod Biol 130(2):262–270
Clarke A, Rowe P, Black N (1996) Does a shorter length of hospital stay affect the outcome and costs of hysterectomy in southern England? J Epidemiol Community Health 50:545–550
Broder MS, Bovone S (2002) Improving treatment outcomes with a clinical pathway for hysterectomy and myomectomy. J Reprod Med 47(12):999–1003
Strong TH, Brown WL Jr, Brown WL, Curry CM (1993) Experience with early postcesarean hospital dismissal. Am J Obstet Gynecol 169:116–119
Steed HL, Capstick V, Flood C, Schepansky A, Schultz J, Mayes DC (2002) A randomized trial of early versus “traditional” postoperative oral intake after major abdominal gynecologic surgery. Am J Obstet Gynecol 186(5):861–865
Schilder JM, Hurteau JA, Look KY, Moore DH, Raff G, Stehman FB, Sutton GP (1997) A prospective controlled trial of early postoperative oral intake following major abdominal gynecologic surgery. Gynecol Oncol 67(3):235–240
MacMillan SL, Kammerer-Doak D, Rogers RG, Parker KM (2000) Early feeding and the incidence of gastrointestinal symptoms after major gynecologic surgery. Obstet Gynecol 96(4):604–608
Burrows WR, Gingo AJ, Rose SM, Zwick SI, Kosty DL, Dierker LJ, Mann LI (1995) Safety and efficacy of early postoperative solid food consumption after cesarean section. J Reprod Med 40(6):463–467
Soriano D, Dulitzki M, Keidar N, Barkai G, Mashiach S, Sediman DS (1996) Early oral feeding after cesarean delivery. Obstet Gynecol 87(6):1006–1008
Patolia DS, Hilliard RL, Toy EC, Baker B (2001) Early feeding after cesarean: randomized trial. Obstet Gynecol 98(1):113–116
Kovavisarach E, Atthakorn M (2005) Early versus delayed oral feeding after cesarean delivery. Int J Gynaecol Obstet 90(1):31–34
Chantarasorn V, Tannirandorn Y (2006) A comparative study of early postoperative feeding versus conventional feeding for patients undergoing cesarean section; a randomized controlled trial. J Med Assoc Thai 89(4):S11–S16
Bar G, Sheiner E, Lezerovizt A, Lazer T, Hallak M (2008) Early maternal feeding following cesarean delivery: a prospective randomized study. Acta Obstet Gynecol Scand 87(1):68–71
Mulayim B, Celik NY, Kaya S, Yanik FF (2008) Early oral hydration after cesarean delivery performed under regional anesthesia. Int J Gynaecol Obstet 101(3):273–276
Hessov I, Ryley Larsen K, Sondergaard K (1988) Improved early alimentation after radical hysterectomies without the traditional use of stomach tube. Acta Obstet Gynecol Sand 67(3):225–228
Cutillo G, Maneschi F, Franchi M, Giannice R, Scambia G, Benedetti-Panici P (1999) Early feeding compared with nasogastric decompression after major oncologic gynecologic surgery: a randomized study. Obstet Gynecol 93(1):41–45
Feng S, Chen L, Wang G, Chen A, Qiu Y (2008) Early oral intake after intra-abdominal gynecological oncology surgery. Cancer Nurs 31(3):209–213
Minig L, Biffi R, Zanagnolo V, Attanasio A, Beltrami C, Bocciolone L et al. (2009) Reduction of postoperative complication rate with the use of early oral feeding in gynecologic oncologic patients undergoing a major surgery: a randomized controlled trial. Ann Surg Oncol 16:3101–3110
Pearl ML, Valea FA, Fischer M, Mahler L, Chalas E (1998) A randomized controlled trial of early postoperative feeding in gynecologic oncology patients undergoing intra-abdominal surgery. Obstet Gynecol 92(1):94–97
Pearl ML, Frandina M, Mahler L, Valea FA, DiSilvestro PA, Chalas E (2002) A randomized controlled trial of a regular diet as the first meal in gynecologic oncology patients undergoing intraabdominal surgery. Obstet Gynecol 100(2):230–234
Patel M, Schimpf MO, O’Sullivan DM, Lasala CA (2010) The use of senna with docusate for postoperative constipation after pelvic reconstructive surgery: a randomized, double-blinded, placebo-controlled trial. Am J Obstet Gynecol 479:e1–e5
Hansen CT, Sorensen M, Moller C, Ottesen B, Kehlet H (2007) Effect of laxatives on gastrointestinal functional recovery in fast-track hysterectomy: a double blind, placebo-controlled randomized study. Am J Obstet Gynecol 196(4):311.e1–7
Demirci F, Somunkiran A, Gul OK, Demiraran Y, Ozdemir I, Gul OB (2007) Does postoperative misoprostol use induce intestinal motility? A prospective randomized double-blind trial. Aust N Z Obstet Gynaecol 47(5):410–414
Fanning J, Yu-Brekke S (1999) Prospective trial of aggressive postoperative bowel stimulation following radical hysterectomy. Gynecol Oncol 73:412–414
Kraus K, Fanning J (2000) Prospective trial of early feeding and bowel stimulation after radical hysterectomy. Am J Obstet Gynecol 182(5):996–998
Abd-El-Maeboud KH, Ibrahim MI, Shalaby DA, Fikry MF (2009) Gum chewing stimulates early return of bowel motility after caesarean section. BJOG 116(10):1334–1339
Mokate T, Wright C, Mander (2006) Hysterectomy and sexual function. J Br Menopause Soc 12(4):153–157
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5(1):13
Acknowledgements
This work is presented on behalf of the Society of Gynecologic Surgeons Systematic Review group, with special thanks to Joseph Schaffer MD.
Funding
The Society of Gynecologic Surgeons provided funding support for assistance by methods experts in systematic review and logistic support.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Murphy, M., Olivera, C., Wheeler, T. et al. Postoperative management and restrictions for female pelvic surgery: a systematic review. Int Urogynecol J 24, 185–193 (2013). https://doi.org/10.1007/s00192-012-1898-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1898-5