Abstract
Introduction and hypothesis
The unexpected absence of urodynamic stress incontinence (USI) in women planning surgery for stress urinary incontinence (SUI) is a challenge to surgeons. We examined the prevalence and clinical and demographic factors associated at baseline (preoperatively) with the unexpected absence of USI among study participants of two multicenter randomized clinical trials of surgery for treating SUI.
Methods
Women with SUI symptoms and positive stress tests on physical examination enrolled in two separate clinical trials—one comparing the autologous fascial sling with the Burch colposuspension [Stress Incontinence Surgical Treatment Efficacy Trial (SISTEr), and the other comparing the retropubic mid-urethral sling with the transobturator midurethral sling [Trial of Mid-Urethral Slings (TOMUS)]—were evaluated for USI preoperatively. The association of clinical, demographic, and urodynamic parameters was examined in women without USI in univariate and multivariate analyses.
Results
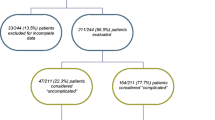
Overall, 144 of 1,233 women (11.7 %) enrolled in the two studies showed no USI. These women had a significantly lower mean volume at maximum cystometric capacity than those with USI (347.5 vs. 395.8 in SISTEr, p = 0.012), (315.2 vs. 358.2 in TOMUS, p = 0.003) and a lower mean number of daily accidents reported on a 3-day diary (2.2 vs 2.7 in SISTEr, p = 0.030) (1.7 vs 2.7 in TOMUS, p < 0.001). Additionally, those without demonstrable USI were more likely to have Pelvic Organ Prolapse Quantification (POP-Q) stage III/IV (31.7 % vs 14.4 % in SISTEr, p = 0.002), (15.5 % vs 6.9 % in TOMUS, p = 0.025). SUI severity as recorded on the Urogenital Distress Inventory (UDI) correlated strongly with the presence of USI in both studies.
Conclusions
We observed that about one of eight women planning surgery for SUI does not show USI. Stage 3/4 POP was strongly associated with the unexpected absence of USI. A diminished urodynamic bladder capacity among women who did not display USI may reflect an inability to reach the limits of capacity during urodynamics, at which these women normally leak.
Similar content being viewed by others
References
Weidner AC, Myers ER, Visco AG, Cundiff GW, Bump RC (2001) Which women with stress incontinence require urodynamic testing? Am J Obst and Gyn 184:20–27
Rahmanou P, Chalihah C, Kulinskaya E, Khullar V (2008) Reliability of urodynamics, pressure flow studies and cough leak point pressure in women with urodynamic stress incontinence with and without detrusor overactivity. Int Urogyn J 19:933–938
Albo ME, Richter HE, Brubaker L, Norton P, Kraus SR, Zimmern PE, Chai TC, Zyczynski H, Diokno AC, Tennstedt S, Nager C, Lloyd LK, FitzGerald M, Lemack GE, Johnson HW, Leng W, Mallett V, Stoddard AM, Menefee S, Varner RE, Kenton K, Moalli P, Sirls L, Dandreo KJ, Kusek JW, Nyberg LM, Steers W, for the Urinary Incontinence Treatment Network (2007) Burch colposuspension versus fascial sling to reduce urinary stress incontinence. NEJM 356:2143–2155
Bump RC, Fantl JA, Hurt WG (1988) The mechanism of urinary continence in women with severe uterovaginal prolapse: results of barrier studies. Obs Gyn 72:291–295
Richter HE, Albo ME, Zyczynski HM, Kenton K, Norton PA, Sirls LT, Kraus SR, Chai TC, Lemack GE, Dandreo KJ, Varner RE, Menefee S, Ghetti C, Brubaker L, Nygaard I, Khandwala S, Rozanski TA, Johnson H, Schaffer J, Stoddard AM, Holley RL, Nager CW, Moalli P, Mueller E, Arisco AM, Corton M, Tennstedt S, Chang TD, Gormley EA, Litman HJ, for the Urinary Incontinence Treatment Network (2010) Retropubic versus transobturator midurethral slings for stress incontinence. NEJM 362:2066–2076
Akaike H (1974) A new look at the statistical model identification. IEEE Trans Autom Control 19:716–723
Mueller ER, Kenton K, Mahajan S, Fitzgerald MP, Brubaker L (2007) Urodynamic prolapse reduction alters urethral pressure but not filling or pressure flow parameters. J Urol 177:600–603
Baseman AG, Baseman JG, Zimmern PE, Lemack GE (2002) Effect of 6F urethral catheterization on urinary flow rates during repeated pressure-flow studies in healthy female volunteers. Urology 59:843–846
Visco AG, Brubaker L, Nygaard I, Richter HE, Cundiff G, Fine P, Zyczynski H, Brown MB, Weber AM (2008) Pelvic Floor Disorders Network. The role of preoperative urodynamic testing in stress continent women undergoing sacrocolpopexy: the Colpopexy and urinary reduction efforts randomized surgical trial. IntUrogyn J 19:607–614
Nager CW, FitzGerald M, Kraus SR, Chai TC, Zyczynski H, Sirls L, Lemack GE, Lloyd LK, Litman HJ, Stoddard AM, Baker J, Steers W (2008) Urinary Incontinence Treatment Network. Urodynamic measures do not predict stress continence outcomes after surgery for stress urinary incontinence in selected women. J Urol 179:1470–1474
Nager CW, Sirls L, Litman HJ, Richter H, Nygaard I, Chai T, Kraus S, Zyczynski H, KentonK HL, Kusek J, Lemack G (2011) Baseline urodynamic predictors of treatment failure 1 year after mid urethral sling surgery. Urinary Incontinence Treatment Network. J Urol 186:597–603
Urinary Incontinence: The management of Urinary Incontinence in Women. The National Institute for Health and Clinical Excellence. NICE clinical guideline 40. October 2006
Nager CW, Brubaker L, Daneshgari F, Litman HJ, Dandreo KJ, Sirls L, Lemack GE, Richter HE, Leng W, Norton P, Kraus SR, Chai TC, Chang D, Amundsen CL, Stoddard AM, Tennstedt SL, for the Urinary Incontinence Treatment Network (2009) Design of the Value of Urodynamic Evaluation (ValUE) trial: A non-inferiority randomized trial of preoperative urodynamic investigations. Cont Clin Tr 30:531–539
Conflicts of interest
None.
Author information
Authors and Affiliations
Consortia
Corresponding author
Rights and permissions
About this article
Cite this article
Lemack, G.E., Litman, H.J., Nager, C. et al. Preoperative clinical, demographic, and urodynamic measures associated with failure to demonstrate urodynamic stress incontinence in women enrolled in two randomized clinical trials of surgery for stress urinary incontinence. Int Urogynecol J 24, 269–274 (2013). https://doi.org/10.1007/s00192-012-1821-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1821-0