Abstract
Purpose
Meniscal graft extrusion is a concern following meniscal allograft transplantation (MAT). MAT surgical techniques continue to evolve in an effort to reduce extrusion; however, improvements remain difficult to measure in vivo. A novel MRI-compatible in vitro loading device capable of applying physiologically relevant loads has been developed, allowing for the measurement of extrusion under a variety of controllable conditions. The objective of this study was to compare maximal medial MAT extrusion (1) with and (2) without an additional peripheral third point of fixation on the tibial plateau.
Methods
Twelve human cadaveric knees underwent medial MAT, utilizing soft tissue anterior and posterior root fixation via transosseous suture, with a third transosseous suture tied over a button providing peripheral fixation on the tibial plateau. The joint was positioned at 5 degrees of flexion and loaded to 1 × body weight (647.7 ± 159.0 N) during MR image acquisition, with and without peripheral fixation. The joint was then positioned at 30 degrees of flexion and the process was repeated. Maximal coronal extrusion was measured.
Results
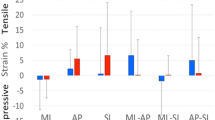
An increase in maximal coronal meniscal extrusion was noted between the unloaded and loaded states. At 30 degrees of flexion, with the addition of a peripheral fixation point, a statistically significant difference in absolute extrusion (p = 0.02) and relative percent extrusion (p = 0.04) between the unloaded and loaded state was found. The addition of a peripheral fixation suture resulted in an overall mean percent difference of − 2.49% (SD 14.1; 95% CI − 11.95, 6.97; n.s.) in extrusion at 5 degrees of flexion and a mean percent difference of − 0.95% (SD 7.3; 95% CI − 5.62, 3.71; n.s.) in extrusion at 30 degrees of flexion. These differences were not statistically significant.
Conclusion
These results suggest that the addition of a peripheral anchor in medial MAT does not reduce the amount of maximal coronal extrusion and, therefore, may not confer any clinical benefit. Surgical techniques utilized to reduce MAT extrusion need further investigation to understand if the added technical difficulty and potential expense is warranted.





Similar content being viewed by others
References
Horneff J (2014) Meniscectomy: the basics. In: Kelly JD IV (ed) Meniscal injuries. Springer, Berlin, pp 39–44
McDermott ID, Amis AA (2006) The consequences of meniscectomy. J Bone Joint Surg Br 88:1549–1556
Hergan D, Thut D, Sherman O, Day MS (2011) Meniscal allograft transplantation. Arthroscopy 27:101–112
ElAttar M, Dhollander A, Verdonk R, Almqvist KF, Verdonk P (2011) Twenty-six years of meniscal allograft transplantation: is it still experimental? A meta-analysis of 44 trials. Knee Surg Sports Traumato Arthrosc 19:147–157
Lee D-H, Lee C-R, Jeon J-H, Kim K-A, Bin S-I (2015) Graft extrusion in both the coronal and sagittal planes is greater after medial compared with lateral meniscus allograft transplantation but is unrelated to early clinical outcomes. Am J Sports Med 43:213–219
De Coninck T, Huysse W, Verdonk R, Verstraete K, Verdonk P (2013) Open versus arthroscopic meniscus allograft transplantation: magnetic resonance imaging study of meniscal radial displacement. Arthroscopy 29:514–521
Van Arkel ER, De Boer HH (1992) Human meniscus transplantation. Agents Actions Suppl 39:243–246
Noyes FR, Heckmann TP, Barber-Westin SD (2012) Meniscus repair and transplantation: a comprehensive update. J Orthop Sports Phys Ther 42:274–290
Abat F, Gelber PE, Erquicia JI, Pelfort X, Gonzalez-Lucena G, Monllau JC (2012) Suture-only fixation technique leads to a higher degree of extrusion than bony fixation in meniscal allograft transplantation. Am J Sports Med 40:1591–1596
Abat F, Gelber PE, Erquicia JI, Tey M, Gonzalez-Lucena G, Monllau JC (2013) Prospective comparative study between two different fixation techniques in meniscal allograft transplantation. Knee Surg Sports Traumatol Arthrosc 21:1516–1522
Verdonk PCM, Verstraete KL, Almqvist KF, De Cuyper K, Veys EM, Verbruggen G et al (2006) Meniscal allograft transplantation: long-term clinical results with radiological and magnetic resonance imaging correlations. Knee Surg Sports Traumatol Arthrosc 14:694–706
Lee DW, Park JH, Chung KS, Ha JK, Kim JG (2017) Arthroscopic lateral meniscal allograft transplantation with the key-hole technique. Arthrosc Tech 6:e1815–e1820
Masferrer-Pino A, Monllau JC, Ibanez M, Erquicia JI, Pelfort X, Gelber PE (2018) Capsulodesis versus bone trough technique in lateral meniscal allograft transplantation: graft extrusion and functional results. Arthroscopy 34:1879–1888
Woodmass JM, Johnson NR, Levy BA, Stuart MJ, Krych AJ (2017) Lateral meniscus allograft transplantation: the bone plug technique. Arthrosc Tech 6:e1215–e1220
Zacchilli MA, Dai AZ, Strauss EJ, Jazrawi LM, Meislin RJ (2017) Bone trough lateral meniscal allograft transplantation: the tapered teardrop technique. Arthrosc Tech 6:e2301–e2312
Zhang YD, Hou SX, Zhong HB, Zhang YC, Luo DZ (2018) Meniscal allograft transplantation using a novel all-arthroscopic technique with specifically designed instrumentation. Exp Ther Med 15:3020–3027
Stone KR, Walgenbach AW (2003) Meniscal allografting: the three-tunnel technique. Arthroscopy 19:426–430
Chen L, Gordon K, Hurtig M (2014) Design and validation of a cadaveric knee joint loading device compatible with magnetic resonance imaging and computed tomography. Med Eng Phys 36:1346–1351
Pollard ME, Kang Q, Berg EE (1995) Radiographic sizing for meniscal transplantation. Arthroscopy 11:684–687
Kim G, Jung HJ, Lee HJ, Lee JS, Koo S, Chang SH (2012) Accuracy and reliability of length measurements on three-dimensional computed tomography using open-source OsiriX software. J Digit Imaging 25:486–491
Ha JK, Shim JC, Kim DW, Lee YS, Ra HJ, Kim JG (2010) Relationship between meniscal extrusion and various clinical findings after meniscus allograft transplantation. Am J Sports Med 38:2448–2455
Fleiss JL (1981) The measurement of interrater agreement. Stat Methods Rates Proportions 2:212–236
Jang SH, Kim JG, Ha JG, Shim JC (2011) Reducing the size of the meniscal allograft decreases the percentage of extrusion after meniscal allograft transplantation. Arthroscopy 27:914–922
Koh YG, Moon HK, Kim YC, Park YS, Jo SB, Kwon SK (2012) Comparison of medial and lateral meniscal transplantation with regard to extrusion of the allograft, and its correlation with clinical outcome. J Bone Joint Surg Br 94:190–193
Lee D-H, Kim S-B, Kim T-H, Cha E-J, Bin S-I (2010) Midterm outcomes after meniscal allograft transplantation comparison of cases with extrusion versus without extrusion. Am J Sports Med 38:247–254
Noyes FR, Barber-Westin SD (2015) A systematic review of the incidence and clinical significance of postoperative meniscus transplant extrusion. Knee Surg Sports Traumatol Arthrosc 23:290–302
Harper KW, Helms CA, Lambert Iii HS, Higgins LD (2005) Radial meniscal tears: significance, incidence, and MR appearance. AJR 185:1429–1434
Milanese S, Gordon S, Buettner P, Flavell C, Ruston S, Coe D et al (2014) Reliability and concurrent validity of knee angle measurement: smart phone app versus universal goniometer used by experienced and novice clinicians. Man Ther 19:569–574
Funding
This study was supported by a research grant from the Musculoskeletal Transplant Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Ethical approval
This laboratory study was performed under the standard Western University institutional approval for the use of anonymous human cadaveric tissue.
Informed consent
For this type of study informed consent was not required.
Rights and permissions
About this article
Cite this article
Hewison, C., Kolaczek, S., Caterine, S. et al. Peripheral fixation of meniscal allograft does not reduce coronal extrusion under physiological load. Knee Surg Sports Traumatol Arthrosc 27, 1924–1930 (2019). https://doi.org/10.1007/s00167-018-5305-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-5305-8