Abstract
Background
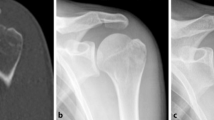
Isolated greater tuberosity fractures are uncommon and account for approximately 2-19% [Emerg Radiol. 2018;25(3):235-246] of all proximal humerus fractures. Surgical treatment is the prevailing recommendation in cases of displacement of more than 5 mm for the general healthy population, while conservative treatment is considered to result in inferior outcomes and is not recommended. However, high-grade evidence is lacking for these recommendations.
Methods
Twenty patients with conservatively treated isolated greater tuberosity fracture were evaluated prospectively as part of a registry study. Morphological Mutch classification, displacement in millimeters, and direction of displacement were determined by computed tomography (CT). Degree of fragment displacement was classified (nondisplaced to minor: ≤ 5 mm; moderate: 6–10 mm; major: > 10 mm). Constant score (CS), age- and sex-adjusted Constant score (adj. CS), subjective shoulder value (SSV), and radiographic follow-up were compared at a minimum follow-up of 12 months. For statistical analysis, quantitative data were compared using Mann–Whitney U t-test. Statistical significance was set at p ≤ 0.05.
Results
Ninteen patients reached the minimum follow-up at an average of 19 months (range, 12–35 months). 13 patients were women. Average age at the time of injury was 51 years (range, 22–75 years). CS and adj. CS averaged 79 ± 17.5 points, and 91 ± 17.7 points, respectively. The SSV averaged 87 ± 17%. No statistically significant difference in clinical outcomes could be observed with respect to the degree of displacement among the three groups.
Conclusion
The outcomes of conservatively treated displaced isolated greater tuberosity fractures are underestimated, and current indications for surgical treatment should be questioned. Further studies with larger numbers of patients and longer lengths of follow-up are needed. The protocol of this observational study is registered at ClinicalTrials.gov (NCT03060876). Date of registration: June 8, 2016.






Similar content being viewed by others
Data availability
The manuscript has associated data in a data repository.
Code availability
Not applicable.
References
White EA, Skalski MR, Patel DB, et al. Isolated greater tuberosity fractures of the proximal humerus: anatomy, injury patterns, multimodality imaging, and approach to management. Emerg Radiol. 2018;25(3):235–46. https://doi.org/10.1007/s10140-018-1589-8.
Constant CR, Gerber C, Emery RJH, Søjbjerg JO, Gohlke F, Boileau P. A review of the Constant score: modifications and guidelines for its use. J Shoulder Elb Surg. 2008;17:355–61.
Santee HE. Fractures about the upper end of the humerus. Ann Surg. 1924;80:103–14.
Platzer P, Kutscha-Lissberg F, Lehr S, Vecsei V, Gaebler C. The influence of displacement on shoulder function in patients with minimally displaced fractures of the greater tuberosity. Injury. 2005;36:1185–9.
Park TS, Choi IY, Kim YH, Park MR, Shon JH, Kim SI. A new suggestion for the treatment of minimally displaced fractures of the greater tuberosity of the proximal humerus. Bull (Hospital for Jt Diseases (New York NY)). 1997;56:171–6.
George MS. Fractures of the greater tuberosity of the humerus. J Am Acad Orthop Surg. 2007;15:607–13.
Lill H, Ellwein A, Katthagen C, Voigt C. Osteoporotic fractures of the proximal humerus. Chirurg. 2012;83:858–65.
Burkhart KJ, Dietz SO, Bastian L, Thelen U, Hoffmann R, Muller LP. The treatment of proximal humeral fracture in adults. Dtsch Arztebl Int. 2013;110:591–7.
Bono CM, Renard R, Levine RG, Levy AS. Effect of displacement of fractures of the greater tuberosity on the mechanics of the shoulder. J Bone Jt Surg Br. 2001;83:1056–62.
Resch H, Thoni H. Dislocation fractures of the shoulder. Special status and therapeutic concepts. Der Orthopade. 1992;21:131–9.
Green A, Izzi J Jr. Isolated fractures of the greater tuberosity of the proximal humerus. J Shoulder Elbow Surg. 2003;12:641–9.
Kristiansen B, Christensen SW. Proximal humeral fractures. Late results in relation to classification and treatment. Acta Orthop Scand. 1987;58:124–7.
Mattyasovszky SG, Burkhart KJ, Ahlers C, Proschek D, Dietz SO, Becker I, et al. Isolated fractures of the greater tuberosity of the proximal humerus: a long-term retrospective study of 30 patients. Acta Orthop. 2011;82:714–20.
Neer CS 2nd. Displaced proximal humeral fractures. Part I. Classification and evaluation. By Charles S. Neer I, 1970. Clin Orthop Relat Res. 1987;223:3–10.
Mills HJ, Horne G. Fractures of the proximal humerus in adults. J Trauma. 1985;25:801–5.
Chun JM, Groh GI, Rockwood CA Jr. Two-part fractures of the proximal humerus. J Shoulder Elbow Surg. 1994;3:273–87.
McLaughlin HL. Dislocation of the shoulder with tuberosity fracture. Surg Clin North Am. 1963;43:1615–20.
Young TB, Wallace WA. Conservative treatment of fractures and fracture-dislocations of the upper end of the humerus. J Bone Jt Surg Br. 1985;67:373–7.
Platzer P, Thalhammer G, Oberleitner G, Kutscha-Lissberg F, Wieland T, Vecsei V, et al. Displaced fractures of the greater tuberosity: a comparison of operative and nonoperative treatment. J Trauma. 2008;65:843–8.
Keene JS, Huizenga RE, Engber WD, Rogers SC. Proximal humeral fractures: a correlation of residual deformity with long-term function. Orthopedics. 1983;6:173–8.
Jakob RPKT, Mayo K, Ganz R, Muller ME. Classification and aspects of treatment of fractures of the proximal Humerus. In: BJW RP, editor. Surgery of the shoulder. Philadelphia: CV mosby Co; 1984. p. 330–343.
Levy DM, Erickson BJ, Harris JD, Bach BR Jr, Verma NN Jr, Romeo AA. Management of isolated greater tuberosity fractures: a systematic review. Am J Orthop (Belle Mead NJ). 2017;46:E445–E453.
Verdano MA, Aliani D, Pellegrini A, Baudi P, Pedrazzi G, Ceccarelli F. Isolated fractures of the greater tuberosity in proximal humerus: does the direction of displacement influence functional outcome? An analysis of displacement in greater tuberosity fractures. Acta Biomed. 2014;84:219–28.
Gallo RA, Sciulli R, Daffner RH, Altman DT, Altman GT. Defining the relationship between rotator cuff injury and proximal humerus fractures. Clin Orthop Relat Res. 2007;458:70–7.
Maman E, Dolkart O, Chechik O, Amar E, Rak O, Rath E, et al. Arthroscopic findings of coexisting lesions with greater tuberosity fractures. Orthopedics. 2014;37:e272–e277277.
Kim SH, Ha KI. Arthroscopic treatment of symptomatic shoulders with minimally displaced greater tuberosity fracture. Arthroscopy. 2000;16:695–700.
Acknowledgements
The authors would like to thank all the participating patients, physiotherapists, the study nurses Mrs. Greeske and Arens, our data manager Mr. Tim Licker, the secretaries Mrs. Assaid and Karataban and the whole trauma team of the Hannover Medical School, Germany. Furthermore, we would like to thank our inhouse Traumastiftung gGmbH as a collaborator enabling this study.
Funding
This study was funded by our inhouse Traumastiftung gGmbH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study is authorized by the local ethical committee as part of an observational registry study (Hannover Humerus Registry—HHR) (journalno. 322-2016) and was carried out in accordance with the Ethical standards of the 1964 Declaration of Helsinki as updated in 2004.
Informed consent
All patients gave written informed consent.
Consent for publication
The manuscript does not include images or information that may identify any person.
Rights and permissions
About this article
Cite this article
Razaeian, S., Hawi, N., Zhang, D. et al. Conservative treatment of displaced isolated proximal humerus greater tuberosity fractures: preliminary results of a prospective, CT-based registry study. Eur J Trauma Emerg Surg 48, 4531–4543 (2022). https://doi.org/10.1007/s00068-020-01453-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01453-7