Abstract
Purpose
Decompressive craniectomy is an effective measure to reduce a pathologically elevated intracranial pressure. Patients’ survival and life quality following this surgery have been a subject of several studies and significantly differ according to the primary diagnosis. Since this operation is often associated with a wide spectrum of possibly serious complications, we aimed to describe their incidence and possible associated risk factors.
Methods
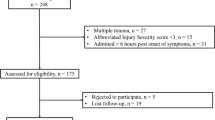
We evaluated 118 patients who underwent decompressive craniectomy at our clinic during years 2013–2017. The indications included traumatic brain injuries, ischaemic or haemorrhagic strokes and postoperative complications of planned neurosurgical procedures. Subsequently, we assessed the incidence of early postoperative complications (occurring during the first 3 postoperative weeks). The results were statistically analysed with relation to a wide selection of possible risk factors.
Results
At least one early surgical postoperative complication occurred in 87 (73.73%) patients, the most frequent being a development of an extraaxial fluid collection in 41 (34.75%) patients. We were able to identify risk factors linked with extraaxial fluid collections, subcutaneous and extradural haematomas, postoperative seizures and meningitis. An overall need for reoperation was 13.56%. Neither the duration of the surgery nor the qualification of the operating surgeon had any effect on the complications’ occurrence.
Conclusions
Decompressive craniectomy is associated with numerous early postoperative complications with a various degree of severity. Most cases of complications can, however, be managed in a conservative way. The risk factors linked with postoperative complications should be taken into account during the indication process in each individual patient.



Similar content being viewed by others
Abbreviations
- CI:
-
Confidence interval
- CSF:
-
Cerebrospinal fluid
- CT:
-
Computed tomography
- DC:
-
Decompressive craniectomy
- GCS:
-
Glasgow Coma Scale
- ICH:
-
Intracerebral haemorrhage
- ICP:
-
Intracranial pressure
- INR:
-
International Normalised Ratio
- OR:
-
Odds ratio
References
Jaeger M, Soehle M, Meixensberger J. Effects of decompressive craniectomy on brain tissue oxygen in patients with intracranial hypertension. J Neurol Neurosurg Psychiatry. 2003;74(4):513–5.
Frank JI, Schumm LP, Wroblewski K, Chyatte D, Rosengart AJ, Kordeck C, Thisted RA, HeADDFIRST Trialists. Hemicraniectomy and durotomy upon deterioration from infarction-related swelling trial: randomized pilot clinical trial. Stroke. 2014;45(3):781–7.
Vahedi K, Hofmeijer J, Juettler E, Vicaut E, George B, Algra A, Amelink GJ, Schmiedeck P, Schwab S, Rothwell PM, Bousser MG, van der Worp HB, Hacke W, DECIMAL, DESTINY, and HAMLET investigators. Early decompressive surgery in malignant infarction of the middle cerebral artery: a pooled analysis of three randomised controlled trials. Lancet Neurol. 2007;6(3):215–2.
Mraček J. Indikace dekompresivní kraniektomie. Cesk Slov Neurol N. 2016;79/112(1):7–21.
Carney N, Totten A, O'Reilly C, Ullman JS, Hawryluk GWJ, Bell MJ, Bratton SL, Chesnut R, Harris OA, Kissoon N, Rubiano AM, Shutter L, Tasker RC, Vavilala MS, Wilberger J, Wright DW, Ghajar J. Guidelines for the management of severe traumatic brain injury, Fourth Edition. Neurosurgery. 2017;80(1):6–15.
Hutchinson PJA, Kolias AG, Timofeev IS, Corteen EA, Czosnyka M, Timothy J, Anderson I, Bulters DO, Belli A, Eynon CA, Wadley J, Mendelow AD, Mitchell PM, Wilson MH, Critchley G, Sahuquillo J, Unterberg A, Servadei F, Teasdale GM, Pickard JD, Menon DK, Murray GD, Kirkpatrick PJ, for the RESCUEicp Trial Collaborators. Trial of decompressive craniectomy for traumatic intracranial hypertension. N Engl J Med. 2016;375:1119–30.
Kolias AG, Adams H, Timofeev IS, Czosnyka M, Corteen EA, Pickard JD, Turner C, Bregson BA, Kirkpatrick PJ, Murray GD, Menon DK, Hutchinson PJ. Decompressive craniectomy following traumatic brain injury: developing the evidence base. Br J Neurosurg. 2016;30(2):246–50.
Kolias AG, Belli A, Li LM, Timofeev I, Corteen EA, Santarius T, Menon DK, Pickard JD, Kirkpatrick PJ, Hutchinson PJ. Primary decompressive craniectomy for acute subdural haematomas: results of an international survey. Acta Neurochir. 2012;154(9):1563–5.
Gopalakrishnan MS, Shanbhag NC, Shukla DP, Konar SK, Bhat DI, Devi BI. Complications of decompressive craniectomy. Front Neurol. 2018. https://doi.org/10.3389/fneur.2018.00977.
Stiver SI. Complications of decompressive craniectomy for traumatic brain injury. Neurosurg Focus. 2009. https://doi.org/10.3171/2009.4.FOCUS0965.
Akins PT, Guppy KH. Sinking skin flaps, paradoxical herniation, and external brain tamponade: a review of decompressive craniectomy management. Neurocrit Care. 2008;9(2):269–76.
Hu PJ, Pittet JF, Kerby JD, Bosarge PL, Wagener BM. Acute brain trauma, lung injury, and pneumonia: more than just altered mental status and decreased airway protection. Am J Physiol Lung Cell Mol Physiol. 2017. https://doi.org/10.1152/ajplung.00485.2016.
Santarsieri M, Kumar RG, Kochanek PM, Berga S, Wagner AK. Variable neuroendocrine-immune dysfunction in individuals with unfavorable outcome after severe traumatic brain injury. Brain Behav Immun. 2015;45:15–27.
Quintard H, Ichai C, Payen JF. The stress response after traumatic brain injury: metabolic and hormonal aspects. In: Preiser JC (eds.) The stress response of critical illness: metabolic and hormonal aspects. Cham:Springer; pp. 197–206.
Yang XF, Wen L, Shen F, Li G, Lou R, Liu WG, Zhan RY. Surgical complications secondary to decompressive craniectomy in patients with a head injury: a series of 108 consecutive cases. Acta Neurochir (Wien). 2008;150(12):1241–8.
Sheskin DJ. Handbook of parametric and nonparametric statistical procedures. 3rd ed. Boca Raton: Chapman & Hall/CRC; 2003.
Kurland DB, Khaladj-Ghom A, Stokum JA, Carusillo B, Karimy JK, Gerzanich V, Sahuquillo J, Simard JM. Complications associated with decompressive craniectomy: a systematic review. Neurocrit Care. 2015;23(2):292–304.
Aarabi B, Chesler D, Maulucci C, Blacklock T, Alexander M. Dynamics of subdural hygroma following decompressive craniectomy: a comparative study. Neurosurg Focus. 2009. https://doi.org/10.3171/2009.3.FOCUS0947.
Kim BO, Kim JY, Whang K, Cho SM, Oh JW, Koo YM, Hu C, Pyen JS, Choi JW. The risk factors of subdural hygroma after decompressive craniectomy. Korean J Neurotrauma. 2018;14(2):93–8.
Mraček J. Dekompresivní kraniektomie. Praha: Galén; 2016.
Salunke P, Garg R, Kapoor A, Chhabra R, Mukherjee KK. Symptomatic contralateral subdural hygromas after decompressive craniectomy: plausible causes and management protocols. J Neurosurg. 2015;122(3):602–9.
De Bonis P, Sturiale CL, Anile C, Gaudino S, Mangiola A, Martucci M, Colosimo C, Rigante L, Pompucci A. Decompressive craniectomy, interhemispheric hygroma and hydrocephalus: a timeline of events? Clin Neurol Neurosurg. 2013;115(8):1308–12.
Feng J, Jiang J, Bao Y, Liang Y, Pan Y. Traumatic subdural effusion evolves into chronic subdural hematoma: two stages of the same inflammatory reaction? Med Hypotheses. 2008;70(6):1147–9.
Zanini MA, de Lima Resende LA, de Souza Faleiros AT, Gabarra EC. Traumatic subdural hygromas: proposed pathogenesis based classification. J Trauma. 2008;64(3):705–13.
Fattahian R, Bagheri SR, Sadeghi M. Development of posttraumatic hydrocephalus requiring ventriculoperitoneal shunt after decompressive craniectomy for traumatic brain injury: a systematic review and meta-analysis of retrospective studies. Med Arch. 2018;72(3):214–9.
Nasi D, Gladi M, Di Rienzo A, di Somma L, Moriconi E, Iacoangeli M, Dobran M. Risk factors for post-traumatic hydrocephalus following decompressive craniectomy. Acta Neurochir (Wien). 2018;160(9):1691–8.
Di G, Hu Q, Liu D, Jiang X, Chen J, Liu H. Risk factors predicting posttraumatic hydrocephalus after decompressive craniectomy in traumatic brain injury. World Neurosurg. 2018. https://doi.org/10.1016/j.wneu.2018.04.216.
Vedantam A, Yamal JM, Hwang H, Robertson CS, Gopinath SP. Factors associated with shunt-dependent hydrocephalus after decompressive craniectomy for traumatic brain injury. J Neurosurg. 2018;128(5):1547–52.
De Bonis P, Pompucci A, Mangiola A, Rigante L, Anile C. Post-traumatic hydrocephalus after decompressive craniectomy: an underestimated risk factor. J Neurotrauma. 2010;27(11):1965–70.
Wang QP, Ma JP, Zhou ZM, You Ch. Impact of operation details on hydrocephalus after decompressive craniectomy. Neurosciences (Riyadh). 2016;21(1):10–6.
Seifman MA, Lewis PM, Rosenfeld JV, Hwang PY. Postoperative intracranial haemorrhage: a review. Neurosurg Rev. 2011;34(4):393–407.
Su TM, Lee TH, Chen WF. Contralateral acute epidural hematoma after decompressive surgery of acute subdural hematoma: clinical features and outcome. J Trauma. 2008;65(6):1298–302.
Carnevale JA, Segar DJ, Powers AY, Shah M, Doberstein C, Drapcho B, Morrison JF, Williams JR, Collins S, Monteiro K, Asaad WF. Blossoming contusions: identifying factors contributing to the expansion of traumatic intracerebral hemorrhage. J Neurosurg. 2018;129(5):1305–16.
Joseph B, Pandit V, Aziz H, Kulvatunyou N, Hashmi A, Tang A, O'Keeffe T, Wynne J, Vercruysse G, Friese RS, Rhee P. Clinical outcomes in traumatic brain injury patients on preinjury clopidogrel: a prospective analysis. J Trauma Acute Care Surg. 2014;76(3):817–20.
Desai VR, Grossman R, Sparrow H. Incidence of intracranial hemorrhage after a cranial operation. Cureus. 2016. https://doi.org/10.7759/cureus.616.
Nasi D, di Somma L, Gladi M, Moriconi E, Scerrati M, Iacoangeli M, Dobran M. New or blossoming hemorrhagic contusions after decompressive craniectomy in traumatic brain injury: analysis of risk factors. Front Neurol. 2018. https://doi.org/10.3389/fneur.2018.01186.
Flint AC, Manley GT, Gean AD, Hemphill JC 3rd, Rosenthal G. Post-operative expansion of hemorrhagic contusions after unilateral decompressive hemicraniectomy in severe traumatic brain injury. J Neurotrauma. 2008;25(5):503–12.
Lonjaret L, Ros M, Boetto S, Fourcade O, Geeraerts T. Brainstem haemorrhage following decompressive craniectomy. J Clin Neurosci. 2012;19(9):1293–5.
Hanko M, Kolarovszki B, Varga K, Opšenák R, Snopko P, Hanzel R, Zeleňák K. Secondary (Duret) brainstem haemorrhage may not always represent a fatal event. Roman Neurosurg. 2019;33(2):166–73.
Mraček J, Mraček Z, Choc M. Poznámky k operační taktice a technice dekompresivní kraniotomie—přehledný referát. Rozhl Chir. 2007;86(5):217–23.
Yamaura A, Makino H. Neurological deficits in the presence of the sinking skin flap following decompressive craniectomy. Neurol Med Chir (Tokyo). 1977;17:1743–53.
Sakamoto S, Eguchi K, Kiura Y, Arita K, Kurisu A. CT perfusion imaging in the syndrome of the sinking skin flap before and after cranioplasty. Clin Neurol Neurosurg. 2006;108(6):583–5.
Güresir E, Vatter H, Schuss P, Oszvald A, Raabe A, Seifert V, Beck J. Rapid closure technique in decompressive craniectomy. J Neurosurg. 2011;114(4):954–60.
Di Rienzo A, Pangrazi PP, Riccio M. Skin flap complications after decompressive craniectomy and cranioplasty: proposal of classification and treatment options. Surg Neurol Int. 2016. https://doi.org/10.4103/2152-7806.193724.
Malliti M, Page P, Gury C, Chomette E, Nataf F, Roux FX. Comparison of deep wound infection rates using a synthetic dural substitute (neuro-patch) or pericranium graft for dural closure: a clinical review of 1 year. Neurosurgery. 2004;54(3):599–604.
Ding K, Gupta PK, Diaz-Arrastia R. Epilepsy after traumatic brain injury. In: Laskowitz D, Grant G (eds.) Translational research in traumatic brain injury. Boca Raton: CRC Press/Taylor and Francis Group; pp. 299–314.
Huang YH, Liao CC, Chen WF, Ou CY. Characterization of acute post-craniectomy seizures in traumatically brain-injured patients. Seizure. 2015;25:150–4.
Seicean A, Kumar P, Seicean S, Neuhauser D, Selman WR, Bambakidis NC. Impact of resident involvement in neurosurgery: An American College of Surgeons’ National Surgical Quality Improvement Program Database Analysis of 33,977 patients. Neurospine. 2018;15(1):54–65.
Lim S, Parsa AT, Kim BD, Rosenow JM, Kim JYS. Impact of resident involvement in neurosurgery: an analysis of 8748 patients from the 2011 American College of Surgeons National Surgical Quality Improvement Program database. J Neurosurg. 2015;122(4):962–70.
Funding
This work was supported by following grants: the application of PACS (Picture Archiving and Communication System) in the research and development, ITMS 26210120004 (Structural project of the European Union with a funding to the Government of the Slovak Republic). Dynamics and risk factors of progression in posttraumatic intracerebral haematomas—a comparison of surgical and conservative treatment, UK/136/2019 (Grant of the Comenius University in Bratislava, Slovak Republic).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers' bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Hanko, M., Soršák, J., Snopko, P. et al. Incidence and risk factors of early postoperative complications in patients after decompressive craniectomy: a 5-year experience. Eur J Trauma Emerg Surg 47, 1635–1647 (2021). https://doi.org/10.1007/s00068-020-01367-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01367-4