Abstract
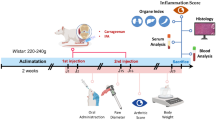
Rheumatoid arthritis (RA) is a common autoimmune disease which impacts a large number of patients worldwide, and new drugs are required for lower the disease burden. Theaflavin-3, 3′-digallate (TFDG) is polyphenol exhibiting inhibition on inflammatory factors. This study aimed to explore the attenuation of TFDG on RA. The collagen-induced arthritis (CIA) mouse model was established and administered with TFDG. The arthritis score and incidence was recorded to assess the amelioration of TFDG on arthritis. Histopathological change of the mouse joint tissues was evaluated by haemotoxylin and eosin staining. The expression of pro-inflammatory mediators including interleukin (IL)-1β, tumor necrosis factor (TNF)-α, and IL-6 was quantified by ELISA. The activation of nuclear factor (NF)-κB and mitogen-activated protein kinase (MAPK) signaling pathways in the synovium were determined by Western blotting. In comparison with the control, administration of TFDG significantly reduced arthritis score and incidence in the CIA mouse model. TFDG significantly suppressed the expression of IL-1β, TNF-α, and IL-6, as well as the levels of MMP-1, MMP-2, and MMP-3 in the synovium. TFDG also showed remarkable inhibition on the activation of NF-κB and the phosphorylation of P38, JNK2, and ERK. This study puts up evidence that TFDG exerts protection on RA via inhibiting the activation of NF-κB- and MAPK-signaling pathways.





Similar content being viewed by others
References
Agere SA, Akhtar N, Watson JM et al (2017) RANTES/CCL5 induces collagen degradation by activating MMP-1 and MMP-13 expression in human rheumatoid arthritis synovial fibroblasts. Front Immunol 8:1341
Almodovar R, Rios V, Ocana S et al (2014) Association of biomarkers of inflammation, cartilage and bone turnover with gender, disease activity, radiological damage and sacroiliitis by magnetic resonance imaging in patients with early spondyloarthritis. Clin Rheumatol 33:237–241
Bortoluzzi A, Furini F, Generali E et al (2018) One year in review 2018: novelties in the treatment of rheumatoid arthritis. Clin Exp Rheumatol 36:347–361
Campbell IK, Roberts LJ, Wicks IP (2003) Molecular targets in immune-mediated diseases: the case of tumour necrosis factor and rheumatoid arthritis. Immunol Cell Biol 81:354–366
Choy EH, Panayi GS (2001) Cytokine pathways and joint inflammation in rheumatoid arthritis. N Engl J Med 344:907–916
Cush JJ, Lipsky PE (1988) Phenotypic analysis of synovial tissue and peripheral blood lymphocytes isolated from patients with rheumatoid arthritis. Arthritis Rheum 31:1230–1238
Dayer JM (2003) The pivotal role of interleukin-1 in the clinical manifestations of rheumatoid arthritis. Rheumatology 42(Suppl 2):ii3–i10
Feldmann M, Brennan FM, Maini RN (1996) Rheumatoid arthritis. Cell 85:307–310
Finger A (1994) In-vitro studies on the effect of polyphenol oxidase and peroxidase on the formation of polyphenolic black tea constituents. J Sci Food Agric 66:293–305
Guo Q, Wang Y, Xu D et al (2018) Rheumatoid arthritis: pathological mechanisms and modern pharmacologic therapies. Bone Res 6:15
Hong C, Shen C, Ding H et al (2015) An involvement of SR-B1 mediated p38 MAPK signaling pathway in serum amyloid A-induced angiogenesis in rheumatoid arthritis. Mol Immunol 66:340–345
Hu X, Ping Z, Gan M et al (2017) Theaflavin-3,3′-digallate represses osteoclastogenesis and prevents wear debris-induced osteolysis via suppression of ERK pathway. Acta Biomater 48:479–488
Iwamoto T, Okamoto H, Toyama Y et al (2008) Molecular aspects of rheumatoid arthritis: chemokines in the joints of patients. FEBS J 275:4448–4455
Joosten LA, Helsen MM, van de Loo FA et al (2008) Anticytokine treatment of established type II collagen-induced arthritis in DBA/1 mice: a comparative study using anti-TNFalpha, anti-IL-1alpha/beta and IL-1Ra. Arthritis Rheum 58(2 Suppl):S110–S122
Kim EY, Moudgil KD (2017) Immunomodulation of autoimmune arthritis by pro-inflammatory cytokines. Cytokine 98:87–96
Ko HJ, Lo CY, Wang BJ et al (2014) Theaflavin-3, 3′-digallate, a black tea polyphenol, attenuates adipocyte-activated inflammatory response of macrophage associated with the switch of M1/M2-like phenotype. J Funct Foods 11:36–48
Kwok SK, Park MK, Cho ML et al (2012) Retinoic acid attenuates rheumatoid inflammation in mice. J Immunol 189:1062–1071
Lepenies J, Eardley KS, Kienitz T et al (2011) Renal TLR4 mRNA expression correlates with inflammatory marker MCP-1 and profibrotic molecule TGF-beta(1) in patients with chronic kidney disease. Nephron Clin Pract 119:c97–c104
Li G, Zhang Y, Qian Y et al (2013a) Interleukin-17A promotes rheumatoid arthritis synoviocytes migration and invasion under hypoxia by increasing MMP2 and MMP9 expression through NF-kappaB/HIF-1alpha pathway. Mol Immunol 53:227–236
Li GQ, Zhang Y, Liu D et al (2013b) PI3 kinase/Akt/HIF-1alpha pathway is associated with hypoxia-induced epithelial-mesenchymal transition in fibroblast-like synoviocytes of rheumatoid arthritis. Mol Cell Biochem 372:221–231
Li CH, Xu LL, Zhao JX et al (2016) CXCL16 upregulates RANKL expression in rheumatoid arthritis synovial fibroblasts through the JAK2/STAT3 and p38/MAPK signaling pathway. Inflamm Res 65:193–202
Li R, Zhang Y, Zheng X et al (2017) Synergistic suppression of autoimmune arthritis through concurrent treatment with tolerogenic DC and MSC. Sci Rep 7:43188
Marinova-Mutafchieva L, Williams RO, Mason LJ et al (1997) Dynamics of proinflammatory cytokine expression in the joints of mice with collagen-induced arthritis (CIA). Clin Exp Immunol 107:507–512
Ohyama Y, Ito J, Kitano VJ et al (2018) The polymethoxy flavonoid sudachitin suppresses inflammatory bone destruction by directly inhibiting osteoclastogenesis due to reduced ROS production and MAPK activation in osteoclast precursors. PLoS One 13:e0191192
Oka Y, Iwai S, Amano H et al (2012) Tea polyphenols inhibit rat osteoclast formation and differentiation. J Pharmacol Sci 118:55–64
Okamoto K, Fujisawa K, Hasunuma T et al (1997) Selective activation of the JNK/AP-1 pathway in Fas-mediated apoptosis of rheumatoid arthritis synoviocytes. Arthritis Rheum 40:919–926
Prodanovic S, Radunovic G, Babic D et al (2018) Matrix metalloproteinases-3 baseline serum levels in early rheumatoid arthritis patients without initial radiographic changes: a two year ultrasonographic study. Med Princ Pract 27:378–386
Singh JA, Hossain A, Mudano AS et al (2017) Biologics or tofacitinib for people with rheumatoid arthritis naive to methotrexate: a systematic review and network meta-analysis. Cochrane Database Syst Rev 5:CD012657
Viatour P, Merville MP, Bours V et al (2005) Phosphorylation of NF-kappaB and IkappaB proteins: implications in cancer and inflammation. Trends Biochem Sci 30:43–52
Wu Y, Jin F, Wang Y et al (2017) In vitro and in vivo anti-inflammatory effects of theaflavin-3,3′-digallate on lipopolysaccharide-induced inflammation. Eur J Pharmacol 794:52–60
Xu M, Liu S, Wan R et al (2018) Combined treatment with sinomenine and acupuncture on collagen-induced arthritis through the NF-kappaB and MAPK signaling pathway. Oncol Lett 15:8770–8776
Yamanishi Y, Firestein GS (2001) Pathogenesis of rheumatoid arthritis: the role of synoviocytes. Rheum Dis Clin North Am 27:355–371
Yang Z, Wang J, Pan Z et al (2018) miR-143-3p regulates cell proliferation and apoptosis by targeting IGF1R and IGFBP5 and regulating the Ras/p38 MAPK signaling pathway in rheumatoid arthritis. Exp Ther Med 15:3781–3790
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Research Involving Human Participants
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Informed Consent
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Liu, W., Li, J. Theaflavin-3, 3′-Digallate Attenuates Rheumatoid Inflammation in Mice Through the Nuclear Factor-κB and MAPK Pathways. Arch. Immunol. Ther. Exp. 67, 153–160 (2019). https://doi.org/10.1007/s00005-019-00536-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00005-019-00536-7