Abstract
Purpose
There is a growing interest in the intraoperative and intensive care use of inhaled epoprostenol (PGI2) for the treatment of pulmonary hypertension (PHT) and hypoxia of cardiac or noncardiac origin. We report our experience with this form of therapy.
Methods
A retrospective chart review of all patients who received inhaled PGI2 over a one-year period was undertaken. Demographic, hemodynamic, oxygenation status, mode of administration, side effects, duration of hospital stay, and mortality were noted.
Results
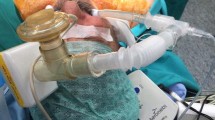
Thirty-five patients, of which 33 (92%) were in the intensive care unit, received inhaled PGI2. Of the 27 patients whose pulmonary artery pressure (PAP) was monitored, a significant decrease in mean PAP from 34.8 ± 11.8 mmHgto 32.1 ± 11.8 mmHg was observed within one hour after the start of therapy (P = 0.0017). Selective pulmonary vasodilatation occurred in 77.8% of the patients. Thirty-three patients had arterial blood gases before and after therapy. There was an improvement in the PaO2/FiO2 ratio in 88% of these with a 175% improvement on average. The ratio of PaO2/FiO2 improved from 108 ± 8 to 138 ± 105 (P = 0.001). Six patients (17%) presented hypotension, two had subsequent pneumothorax, one had bronchospasm and in one patient PGI2 inhalation was stopped because of increasing peak pulmonary pressures from the secondary flow coming from the nebulizer. Mortality of the cohort was 54%.
Conclusion
Inhaled PGI2 can be useful in the treatment of patients with PHT and severe hypoxia. It can however be associated with systemic side effects.
Résumé
Objectif
Il y a un intérêt croissant pour l’utilisation de l’époprosténol (PGI2) inhalé comme traitement de l’hypertension pulmonaire (HTP) et de l’hypoxie d’origine cardiaque ou non survenant en salle d’opération ou aux soins intensifs. Nous rendons compte de notre expérience avec cette forme de thérapie.
Méthode
On a procédé à l’examen rétrospectif de tous les dossiers des patients qui ont reçu de la PGI2 par inhalation au cours d’une année. Les données démographiques et hémodynamiques, l’état de l’oxygénation, le mode d’administration, les effets secondaires, la durée du séjour hospitalier et la mortalité ont été enregistrés.
Résultats
Trente-cinq patients, dont 33 (92 %) étaient à l’unité des soins intensifs, ont reçu de la PGI2 par inhalation. Chez 27 patients dont on a surveillé la tension artérielle pulmonaire (TAP), une baisse significative de la TAP moyenne a été observée passant de 34,8 ± 11,8 mmHg à 32,1 ± 11,8 mmHg pendant la première heure de la thérapie (P = 0,0017). La vasodilatation pulmonaire sélective est survenue chez 77,8 % des patients. Trente-trois patients ont eu une gazométrie du sang artériel avant et après la thérapie. Une amélioration du ratio PaO2/FiO2 a été notée chez 88 % d’entre eux et une amélioration de 175 % en moyenne. Le ratio PaO2/FiO2 s’est amélioré, de 108 ± 8 à 138 ± 105 (P = 0,001). Six patients (17 %) ont présenté de l’hypotension, deux ont eu un pneumothorax subséquent, un a souffert de bronchospasme et chez un autre patient l’inhalation de PGI2 a été stoppée à la suite de la hausse des pics de pressions pulmonaires provenant du flux secondaire du nébuliseur. La mortalité a été de 54 % dans cette cohorte.
Conclusion
La PGI2 inhalée peut être utile comme traitement de patients atteints d’HTP et d’hypoxie sévère. Il peut toutefois provoquer des effets secondaires systémiques.
Article PDF
Similar content being viewed by others
References
Moncada S, Korbut R, Bunting S, Vane JR. Prostacyclin is a circulating hormone. Nature 1978; 273: 767–8.
Kerins DM, Murray R, FitzGerald GA. Prostacyclin and prostaglandin E1: molecular mechanisms and therapeutic utility. Prog Hemost Thromb 1991; 10: 307–37.
Olschewski H, Ghofrani HA, Walmrath D, et al. Inhaled prostacyclin and iloprost in severe pulmonary hypertension secondary to lung fibrosis. Am J Respir Crit Care Med 1999; 160: 600–7.
Walmrath D, Schneider T, Pilch J, Grimminger F, Seeger W. Aerosolised prostacyclin in adult respiratory distress syndrome. Lancet 1993; 342: 961–2.
Bernard GR, Artigas A, Brigham KL, et al. Report of the American-European Consensus conference on acute respiratory distress syndrome: definitions, mechanisms, relevant outcomes, and clinical trial coordination. Consensus Committee. J Crit Care 1994; 9: 72–81.
Domenighetti G, Stricker H, Waldispuehl B. Nebulized prostacyclin (PGI2) in acute respiratory distress syndrome: impact of primary (pulmonary injury) and secondary (extrapulmonary injury) disease on gas exchange response. Crit Care Med 2001; 29: 57–62.
Walmrath D, Schermuly R, Pilch J, Grimminger F, Seeger W. Effects of inhaled versus intravenous vasodilators in experimental pulmonary hypertension. Eur Respir J 1997; 10: 1084–92.
Welte M, Zwissler B, Habazettl H, Messmer K. PGI2 aerosol versus nitric oxide for selective pulmonary vasodilation in hypoxic pulmonary vasoconstriction. Eur Surg Res 1993; 25: 329–40.
Zobel G, Dacar D, Rodl S, Friehs I. Inhaled nitric oxide versus inhaled prostacyclin and intravenous versus inhaled prostacyclin in acute respiratory failure with pulmonary hypertension in piglets. Pediatr Res 1995; 38: 198–204.
Zwissler B, Welte M, Messmer K. Effects of inhaled prostacyclin as compared with inhaled nitric oxide on right ventricular performance in hypoxic pulmonary vasoconstriction. J Cardiothorac Vasc Anesth 1995; 9: 283–9.
Booke M, Bradford DW, Hinder F, {aeet al.} Effects of inhaled nitric oxide and nebulized prostacyclin on hypoxic pulmonary vasoconstriction in anesthetized sheep. Crit Care Med 1996; 24: 1841–8.
Kleen M, Habler O, Hofstetter C, et al. Efficacy of inhaled prostanoids in experimental pulmonary hypertension. Crit Care Med 1998; 26: 1103–9.
Hill LL, Pearl RG. Combined inhaled nitric oxide and inhaled prostacyclin during experimental chronic pulmonary hypertension. J Appl Physiol 1999; 86: 1160–4.
Pappert D, Busch T, Gerlach H, Lewandowski K, Radermacher P, Rossaint R. Aerosolized prostacyclin versus inhaled nitric oxide in children with severe acute respiratory distress syndrome. Anesthesiology 1995; 82: 1507–11.
Hardy CC, Bradding P, Robinson C, Holgate ST. Bronchoconstrictor and antibronchoconstrictor properties of inhaled prostacyclin in asthma. J Appl Physiol 1988; 64: 1567–74.
Burghuber OC, Silberbauer K, Haber P, Sinzinger H, Elliott M, Leithner C. Pulmonary and antiaggregatory effects of prostacyclin after inhalation and intravenous infusion. Respiration 1984; 45: 450–4.
Olschewski H, Walmrath D, Schermuly R, Ghofrani A, Grimminger F, Seeger W. Aerosolized prostacyclin and iloprost in severe pulmonary hypertension. Ann Intern Med 1996; 124: 820–4.
Walmrath D, Schneider T, Pilch J, Schermuly R, Grimminger F, Seeger W. Effects of aerosolized prostacyclin in severe pneumonia. Impact of fibrosis. Am J Respir Crit Care Med 1995; 151: 724–30.
Troncy E, Francoeur M, Blaise G. Inhaled nitric oxide: clinical applications, indications, and toxicology. Can J Anaesth 1997; 44: 973–88.
Zwissler B, Kemming G, Habler O, et al. Inhaled prostacyclin (PGI2) versus inhaled nitric oxide in adult respiratory distress syndrome. Am J Respir Crit Care Med 1996; 154: 1671–7.
Mikhail G, Gibbs J, Richardson M, et al. An evaluation of nebulized prostacyclin in patients with primary and secondary pulmonary hypertension. Eur Heart J 1997; 18: 1499–504.
Haraldsson A, Kieler-Jensen N, Nathorst-Westfelt U, Bergh CH, Ricksten SE. Comparison of inhaled nitric oxide and inhaled aerosolized prostacyclin in the evaluation of heart transplant candidates with elevated pulmonary vascular resistance. Chest 1998; 114: 780–6.
van Heerden PV, Gibbs NM, Michalopoulos N. Effect of low concentrations of prostacyclin on platelet function in vitro. Anaesth Intensive Care 1997; 25: 343–6.
Thomas SH, O’Doherty MJ, Fidler HM, Page CJ, Treacher DF, Nunan TO. Pulmonary deposition of a nebulised aerosol during mechanical ventilation. Thorax 1993; 48: 154–9.
MacIntyre NR, Silver RM, Miller CW, Schuler F, Coleman RE. Aerosol delivery in intubated, mechanically ventilated patients. Crit Care Med 1985; 13: 81–4.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by the “Plan de Pratique des Anesthésistes” of the Montreal Heart Institute.
Rights and permissions
About this article
Cite this article
Haché, M., Denault, A.Y., Bélisle, S. et al. Inhaled prostacyclin (PGI2) is an effective addition to the treatment of pulmonary hypertension and hypoxia in the operating room and intensive care unit. Can J Anesth 48, 924–929 (2001). https://doi.org/10.1007/BF03017361
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03017361