Abstract
Background
Surgical treatment has proved to be effective for weight loss, improving the quality of life of obese individuals. However, metabolic and nutritional deficiencies may occur during the late postoperative period. The objective of the present study was to assess the metabolic and nutritional profile of grade III obese individuals for 12 months after Roux-en-Y gastric bypass (RYGBP).
Methods
Forty-eight patients with mean body mass index (BMI) of 51.9 ± 7.8 kg/m2 were submitted to RYGBP. Anthropometric, food intake, and biochemical data were obtained before and for 12 months after surgery.
Results
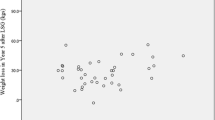
There was an average weight and body fat reduction of 35% and 46%, respectively. Calorie intake was reduced, ranging from 773 ± 206 to 1035 ± 345 kcal during the study. Protein intake remained below recommended values throughout follow-up, corresponding to 0.5 ± 0.3 g/kg/current body weight/day during the 12th month. Iron and fiber intake was significantly reduced, remaining below recommended levels throughout the study. Serum cholesterol, low-density lipoprotein cholesterol, and glycemia were reduced. Albumin deficiency was present in 15.6% of subjects at the beginning of the study vs 8.9% at the end, calcium deficiency was present in 3.4% vs 16.7%, and iron deficiency was present in 12.2% vs 14.6%.
Conclusions
RYGBP was effective for weight loss and for the reduction of obesity rates and risk factors for comorbidities. The diet of these patients, who frequently present inadequate intake of macronutrients and micronutrients, should receive special attention. Patient follow-up and assessment at short intervals are necessary for an early correction of nutritional deficiencies.

Similar content being viewed by others
References
World Health Organization. Preventing and managing the global epidemic of obesity. Report of the World Health Organization Consultation of Obesity. Geneva: World Health Organization; 1998.
Rashid MN, Fuentes F, Touchon RC, et al. Obesity and risk for cardiovascular diseases. Prev Cardiol 2003;6:42–7.
Buchwald H. Overview of bariatric surgery. J Am Coll Surg 2002;194:367–75.
Steinbrook R. Surgery for severe obesity. N Engl J Med 2004;350:1075–9.
Ferraro DR. Management of the bariatric surgery lifelong postoperative care. Clin Rev 2004;14:73–9.
Maggard MA, Sugarman LR, Suttorp M, et al. Meta-analysis: surgical treatment of obesity. Ann Intern Med 2005;142:547–59.
Bult MJ, Van Dalen T, Muller AF. Surgical treatment of obesity. Eur J Endocrinol 2008;158:135–45.
Fobi MAL, Lee H, Fleming AW. The surgical technique of the banded Roux-en-Y gastric bypass. J Obes Weight Regul 1989;8:99–102.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA 2004;292:1724–37.
Anção MS, Cuppari L, Draibe AS, et al. Programa de Apoio à Nutrição-NutWin. Versão 1.5. São Paulo: Departamento de Informática em Saúde-SPDM-Unifesp/EPN, 2002. CD-ROM.
Pories WJ, Swanson MS, MacDonald KG, et al. Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg 1995;222:339–52.
Das SK, Roberts SB, Kehayas JJ, et al. Body composition assessment in extreme obesity and after massive weight loss induced by gastric bypass surgery. Am J Physiol Endocrinol Metab 2003;284:E1080–8.
Giusti V, Suter M, Heraief E, et al. Effects of laparoscopic gastric banding on body composition, metabolic profile and nutritional status of obese women: 12-months follow-up. Obes Surg 2004;14:239–45.
Von Mach MA, Stoeckli R, Bilz S, et al. Changes in bone mineral content after surgical treatment of morbid obesity. Metabolism 2004;53:918–21.
Moize V, Geliebter A, Gluck ME, et al. Obese patients have inadequate protein intake related to protein intolerance up to 1 year following Roux-en-Y gastric bypass. Obes Surg 2003;13:23–8.
Brolin RE, Leung M. Surgery of vitamin and mineral supplementation after gastric bypass and biliopancreatic diversion for mordid obesity. Obes Surg 1999;9:150–4.
MacLean LD, Rhode BM, Forse RA. Late results of vertical banded gastroplastry for morbid super obesity. Surgery 1990;107:20–7.
Avinoach E, Ovnat A, Charuzi I. Nutritional status 7 years after Roux-en-Y gastric bypass surgery. Surgery 1992;111:137–42.
Love AL, Billett HH. Obesity, bariatric surgery, and iron deficiency: true, true, true and related. Am J Hematol 2008;83:403–9.
Dias MCG, Ribeiro AG, Scabim VM, et al. Dietary intake of female bariatric patients after anti-obesity gastroplasty. Clinics 2006;61:93–8.
Kaidar-Person O, Person B, Szomstein S, et al. Nutritional deficiencies in morbidly obese patients: a new form of malnutrition? Part A: vitamins. Obes Surg 2008;18:870–6.
Kaidar-Person O, Person B, Szomstein S, et al. Nutritional deficiencies in morbidly obese patients: a new form of malnutrition? Part B: minerals. Obes Surg 2008;18:1028–34.
Tucker ON, Szomstein S, Rosenthal RJ. Nutritional consequences of weight-loss surgery. Med Clin N Am 2007;91:499–514.
Cristou NV, Sampalis JS, Liberman M, et al. Surgery decreases long-term mortality, morbidy, and health care use in morbidly obese patients. Ann Surg 2004;240:416–24.
Torgerson JS, Sjostrom L. The Swedish Obese Subjects (SOS) study rationale and results. Int J Obes Relat Metab Disord 2001;25:S2–4.
Sjomstrom CD, Peltonen M, Wedel H, et al. Differentiated long-term effects of intentional weight loss on diabetes and hypertension. Hypertension 2000;36:20–5.
Busetto L, Pisent C, Rinaldi D, et al. Variation in lipid levels in morbidly obese patient operated with LAP-BAND adjustable gastric banding system: effects of different levels of weight loss. Obes Surg 2000;10:569–77.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bavaresco, M., Paganini, S., Lima, T.P. et al. Nutritional Course of Patients Submitted to Bariatric Surgery. OBES SURG 20, 716–721 (2010). https://doi.org/10.1007/s11695-008-9721-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-008-9721-6