Background
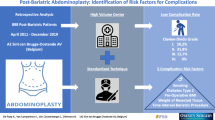
In this prospective study, we followed patients after laparoscopic adjustable gastric banding for morbid obesity who underwent abdominoplasty for body contouring. Our purposes were: 1) to determine if a significant relationship between cigarette smoking and postoperative wound infections existed, 2) the relative risk conferred by cigarettes and 3) a cut-off value for the increased risk.
Methods
Patients scheduled for body contouring abdominoplasty were considered eligible. We excluded those with ongoing clinical infections, recent antibiotic administration, those within 1 year from their bariatric surgery and those with systemic diseases. Smokers were asked to stop smoking at least 4 weeks before surgery.
Results
Since November 2004, we recruited 60 patients. Postoperative infections were present in 25% (n=15) of patients and 86.7% of these (n=13) were superficial. All except one occurred in smokers (P=0.0001): 47% of smokers and 3% of nonsmokers developed infections. Significant differences between infections vs infection-free patients were present for the number of cigarettes smoked per day (P<0.001), years of smoking (P<0.001), overall estimated cigarettes smoked and the number of pack years (P=0.001). A cut-off value of −62,000 overall estimated cigarettes (8.5 pack years) distinguished between infections vs infection-free patients (6.2% false positives and 7.1% false negatives). Relative risk conferred by smoking was 14 (95% confidence intervals 13.3–16.7).
Conclusions
The incidence of infections in postbariatric patients undergoing body contouring abdominoplasties is 25%. The relative risk conferred by smoking was 14 and the cut-off value was 62,000 overall cigarettes (8.5 pack years).
Similar content being viewed by others
References
Kryger ZB, Fine NA, Mustoe TA. The outcome of abdominoplasty performed under conscious sedation: six-year experience in 153 consecutive cases. Plast Reconstr Surg 2004; 113: 1807–17.
Spiegelman JI, Levine RH. Abdominoplasty: a comparison of outpatient and inpatient procedures shows that it is a safe and effective procedure for outpatients in an office-based surgery clinic. Plast Reconstr Surg 2006; 118: 517–22.
Sanger C, David LR. Impact of significant weight loss on outcome of body-contouring surgery. Ann Plast Surg 2006; 56: 9–13.
Vastine VL, Morgan RF, Williams GS et al. Wound complications of abdominoplasty in obese patients. Ann Plast Surg 1999; 42: 34–9.
Mosely LH, Finseth F. Cigarette smoking: impairment of digital blood flow and wound healing in the hand. Hand 1977; 9: 97–101.
Mosely LH, Finseth F, Goody M. Nicotine and its effect on wound healing. Plast Reconstr Surg 1978; 61: 570–5.
Rees TD, Liverett DM, Guy CL. The effect of cigarette smoking on skin-flap survival in the face lift patient. Plast Reconstr Surg 1984; 73: 911–5.
Krueger JK, Rohrich RJ. Clearing the smoke: the scientific rationale for tobacco abstention with plastic surgery. Plast Reconstr Surg 2001; 108: 1063–73.
Rogliani M, Labardi L, Silvi E et al. Smokers: risks and complications in abdominal dermolipectomy. Aesthetic Plast Surg 2006; 30: 422–4.
Chan LK, Withey S, Butler PE. Smoking and wound healing problems in reduction mammaplasty: is the introduction of urine nicotine testing justified? Ann Plast Surg 2006; 56: 111–5.
Manassa EH, Hertl CH, Olbrisch RR. Wound healing problems in smokers and nonsmokers after 132 abdominoplasties. Plast Reconstr Surg 2003; 111: 2082–7.
WHO MONICA Manual: Smoking questionnaire. WHO MONICA Project (1992). URL: http://www.ktl.fi/publications/monica/manual/part3/iii-1.htm.
Stewart KJ, Stewart DA, Coghlan B et al. Complications of 278 consecutive abdominoplasties. J Plast Reconstr Aesthet Surg 2006; 59: 1152–5.
Spiegelman JI, Levine RH. Abdominoplasty: a comparison of outpatient and inpatient procedures shows that it is a safe and effective procedure for outpatients in an office-based surgery clinic. Plast Reconstr Surg 2006; 118: 517–22.
Chaouat M, Levan P, Lalanne B et al. Abdominal dermolipectomies: early postoperative complications and long-term unfavorable results. Plast Reconstr Surg 2000 Dec; 106: 1614–8.
Moher D, Schulz KF, Altman DG. The CONSORT statement: revised recommendations for improving the quality of reports of parallel-group randomised trials. Lancet 2001; 357: 1191–4.
Kaufman T, Eichenlaub EH, Levin M et al. Tobacco smoking: Impairment of experimental flap survival. Ann Plast Surg 1984; 13: 468–72.
Lawrence WT, Murphy RC, Robson MC et al. The detrimental effect of cigarette smoking on flap survival: an experimental study in the rat. Br J Plast Surg 1984; 37: 216–9.
van Adrichem LN, Hoegen R, Hovius SE et al. The effect of cigarette smoking on the survival of free vascularized and pedicled epigastric flaps in the rat. Plast Reconstr Surg 1996; 97: 86–96.
Chang LD, Buncke G, Slezak S et al. Cigarette smoking, plastic surgery, and microsurgery. J Reconstr Microsurg 1996; 12: 467–74.
Black CE, Huang N, Neligan PC et al. Effect of nicotine on vasoconstrictor and vasodilator responses in human skin vasculature. Am J Physiol Regul Integr Comp Physiol 2001; 281: R1097–104.
Astrup P, Kjeldsen K. Carbon monoxide, smoking, and atherosclerosis. Med Clin North Am 1974; 58: 323–50.
Birnstingl MA, Brinson K, Chakrabarti BK. The effect of short-term exposure to carbon monoxide on platelet stickiness. Br J Surg 1971; 58: 837–9.
Dintenfass L. Elevation of blood viscosity, aggregation of red cells, haematocrit values and fibrinogen levels with cigarette smokers. Med J Aust 1975; 1: 617–20.
Meade TW, Chakrabarti R, Haines AP et al. Characteristics affecting fibrinolytic activity and plasma fibrinogen concentrations. Br Med J 1979; 1: 153–6.
Chaouat M, Levan P, Lalanne B et al. Abdominal dermolipectomies: early postoperative complications and long-term unfavorable results. Plast Reconstr Surg 2000; 106: 1614–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gravante, G., Araco, A., Sorge, R. et al. Wound Infections in Post-bariatric Patients undergoing Body Contouring Abdominoplasty: the Role of Smoking. OBES SURG 17, 1325–1331 (2007). https://doi.org/10.1007/s11695-007-9236-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-007-9236-6