Abstract
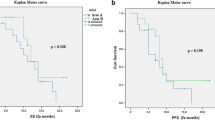
Diffuse brainstem glioma is a rare disease in adults. Radiotherapy (RT) is usually considered to be the standard treatment. However, the role of chemotherapy in treating relapses after RT is unclear, and this study aimed to assess the use of temozolomide (TMZ) in this situation. We conducted a retrospective analysis of patients from our database with “low grade” adult diffuse infiltrating brainstem glioma who received TMZ at relapse after failing RT. The patients were diagnosed by histology or MRI criteria compatible with a low-grade glioma. The tumors were localized in the pons, medulla oblongata or midbrain, excluding supratentorial or infratentorial tumors that had infiltrated the brainstem secondarily. The patients’ clinical and radiological responses were assessed, and their progression free survival (PFS) and overall survival (OS) time were estimated. Fifteen adult patients (median age 34 years) fulfilled the inclusion criteria. Histological analysis was available in 5 cases and showed grade II oligodendroglioma (2 cases), grade II oligoastrocytoma (2 cases), and grade II astrocytoma (1 case). Ten patients were selected by MRI criteria only. All patients received RT as initial treatment and had a median PFS of 34.2 months (95 % CI 24.1–44.2). The median KPS at the time of relapse was 80. TMZ was administered orally at 150–200 mg/m2 for 5 days, every 28 days. Clinical improvement after TMZ was observed in 9 cases (60 %), whereas radiological assessment detected responses in 6/15 cases, including 4 partial and 2 minor responses. The estimated median PFS after TMZ was 9.5 months (95 % CI 7.9–11), and the median OS was 14.4 months (95 % CI 10.5–18.2). Grade 3 thrombopenia was observed in 26 % of cases. TMZ could be useful after RT failure in adult patients with recurrent diffuse “low grade” brainstem glioma.


Similar content being viewed by others
References
Selvapandian S, Rajshekhar V, Chandy MJ (1999) Brainstem glioma: comparative study of clinico-radiological presentation, pathology and outcome in children and adults. Acta Neurochir (Wien) 141(7):721–727
Chassot A, Canale S, Varlet P, Puget S, Roujeau T, Negretti L et al (2012) Radiotherapy with concurrent and adjuvant temozolomide in children with newly diagnosed diffuse intrinsic pontine glioma. J Neurooncol 106(2):399–407
Guillamo JS, Monjour A, Taillandier L, Devaux B, Varlet P, Haie-Meder C et al (2001) Brainstem gliomas in adults: prognostic factors and classification. Brain 124:2528–2539
Hargrave D, Chuang N, Bouffet E (2008) Conventional MRI cannot predict survival in childhood diffuse intrinsic pontine glioma. J Neurooncol 86(3):313–319
Salmaggi A, Fariselli L, Milanesi I, Lamperti E, Silvani A, Bizzi A et al (2008) Natural history and management of brainstem gliomas in adults. A retrospective Italian study. J Neurol 255(2):171–177
Taal W, Dubbink HJ, Zonnenberg CBL, Zonnenberg BA, Postma TJ, Gijtenbeek JMM et al (2011) First-line temozolomide chemotherapy in progressive low-grade astrocytomas after radiotherapy: molecular characteristics in relation to response. Neuro-Oncol 13(2):235–241
Wen PY, Macdonald DR, Reardon DA, Cloughesy TF, Sorensen AG, Galanis E et al (2010) Updated response assessment criteria for high-grade gliomas: response assessment in neuro-oncology working group. J Clin Oncol 10 28(11):1963–1972
Van den Bent MJ, Wefel JS, Schiff D, Taphoorn MJ, Jaeckle K, Junck L et al (2011) Response assessment in neuro-oncology (a report of the RANO group): assessment of outcome in trials of diffuse low-grade gliomas. Lancet Oncol 12(6):583–593
Bailey S, Howman A, Wheatley K, Wherton D, Boota N, Pizer B et al (2013) Diffuse intrinsic pontine glioma treated with prolonged temozolomide and radiotherapy–results of a United Kingdom phase II trial (CNS 2007 04). Eur J Cancer 49(18):3856–3862
Reyes-Botero G, Giry M, Mokhtari K, Labussière M, Idbaih A, Delattre JY, Laigle-Donadey F, Sanson M (2014) Molecular analysis of diffuse intrinsic brainstem gliomas in adults. J Neurooncol 116(2):405–411
Sturm D, Witt H, Hovestadt V, Khuong-Quang D-A, Jones DTW, Konermann C et al (2012) Hotspot mutations in H3F3A and IDH1 define distinct epigenetic and biological subgroups of glioblastoma. Cancer Cell 22(4):425–437
Schwartzentruber J, Korshunov A, Liu X-Y, Jones DTW, Pfaff E, Jacob K et al (2012) Driver mutations in histone H3.3 and chromatin remodelling genes in paediatric glioblastoma. Nature 482(7384):226–231
Khuong-Quang D-A, Rakopoulos P, Liu X-Y, Fontebasso AM, Bouffet E et al (2012) K27 M mutation in histone H3.3 defines clinically and biologically distinct subgroups of pediatric diffuse intrinsic pontine gliomas. Acta Neuropathol 124(3):439–447
Buczkowicz P, Hoeman C, Roakopoulos P, Pajovic S, Letourneau L, Dzamba M, Morrison A, Lewis P, Bouffet E, Bartels U et al (2014) Genomic analysis of diffuse intrinsic pontine gliomas identifies three molecular subgroups and recurrent activating ACVR1 mutations. Nat Genet 46:451–456. doi:10.1038/ng.2936
Taylor KR, Mackay A, Truffaux N, Butterfield YS, Morozova O, Philippe C et al (2014) Recurrent activating ACVR1 mutations in diffuse intrinsic pontine glioma. Nat Genet 46(5):457–461
White ML, Zhang Y, Kirby P, Ryken TC (2005) Can tumor contrast enhancement be used as a criterion for differentiating tumor grades of oligodendrogliomas? AJNR 26(4):784–790
Dellaretti M, Touzet G, Reyns N, Dubois F, Gusmão S, Pereira JLB et al (2012) Correlation between magnetic resonance imaging findings and histological diagnosis of intrinsic brainstem lesions in adults. Neuro-Oncol 14(3):381–385
Guzmán-De-Villoria JA, Ferreiro-Argüelles C, Fernández-García P (2010) Differential diagnosis of T2 hyperintense brainstem lesions: part 2. Diffuse lesions. Semin Ultrasound CT MR 31(3):260–274
Prabhu SP, Ng S, Vajapeyam S, Kieran MW, Pollack IF, Geyer R et al (2011) DTI assessment of the brainstem white matter tracts in pediatric BSG before and after therapy: a report from the Pediatric Brain Tumor Consortium. Childs Nerv Syst 27(1):11–18
Zukotynski KA, Fahey FH, Kocak M, Alavi A, Wong TZ, Treves ST et al (2011) Evaluation of 18F-FDG PET and MRI associations in pediatric diffuse intrinsic brain stem glioma: a report from the Pediatric Brain Tumor Consortium. J Nucl Med 52(2):188–195
Gonçalves-Ferreira AJ, Herculano-Carvalho M, Pimentel J (2003) Stereotactic biopsies of focal brainstem lesions. Surg Neurol 60(4):311–320
Dellaretti M, Reyns N, Touzet G, Dubois F, Gusmão S, Pereira JLB et al (2012) Stereotactic biopsy for brainstem tumors: comparison of transcerebellar with transfrontal approach. Stereotact Funct Neurosurg 90(2):79–83
Acknowledgments
This work was made possible thanks to the ARTC (Association pour la Recherche sur les tumeurs cérébrales).
Conflict of interest
The authors have no conflict of interest to declare. The funding sources had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Funding
German Reyes-Botero was funded by the ARTC (Association pour la Recherche sur les tumeurs cérébrales). The research leading to these results has received funding from the program “Investissements d’avenir” ANR-10-IAIHU-06.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Reyes-Botero, G., Laigle-Donadey, F., Mokhtari, K. et al. Temozolomide after radiotherapy in recurrent “low grade” diffuse brainstem glioma in adults. J Neurooncol 120, 581–586 (2014). https://doi.org/10.1007/s11060-014-1589-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-014-1589-9