Abstract
Introduction
We examined the prevalence of autism spectrum disorders (ASDs) in Massachusetts (MA) comparing children born via assisted reproductive technology (ART) and children born to women with indicators of subfertility but no ART (Subfertile), to children born to women with neither ART nor indicators of subfertility (Fertile). We assessed the direct, indirect, and total effects of ART and subfertility on ASD among singletons.
Methods
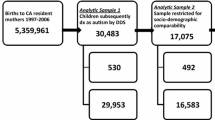
This study included 10,147 ART, 8072 Subfertile and 441,898 Fertile MA resident births from the MA Outcome Study of ART (MOSART) database linked with Early Intervention program participation data. ART included fresh in vitro fertilization (IVF), fresh intracytoplasmic sperm injection (ICSI), and frozen embryo transfer. We estimated the prevalence of ASD by fertility group. We used logistic regression to assess the natural direct effect (NDE), natural indirect effect (NIE) through preterm birth, and total effects of each fertility group on ASD.
Results
The NDE indicated that, compared to the Fertile group, the odds of ASD were not statistically higher in the ART (ORNDE 1.07; 95% CI 0.88–1.30), Subfertile (ORNDE 1.11; 95% CI 0.89–1.38), IVF (ORNDE 0.91; 95% CI 0.68–1.22), or ICSI (ORNDE 1.13; 95% CI 0.84–1.51) groups, even if the rate of preterm birth was the same across all groups. The total effect (product of NDE and NIE) was not significant for ART (ORTotal Effect 1.08; 95% CI 0.89–1.30), Subfertile (ORTotal Effect 1.11; 95% CI 0.89–1.38), IVF (ORTotal Effect 0.92; 95% CI 0.69–1.23), or ICSI (ORTotal Effect 1.13; 95% CI 0.84–1.52).
Conclusion
Compared to children born to Fertile women, children born to ART, ICSI, or IVF, or Subfertile women are not at increased risk of receiving an ASD diagnosis.


Similar content being viewed by others
References
Ananth, C. V., & Schisterman, E. F. (2017). Confounding, causality, and confusion: The role of intermediate variables in interpreting observational studies in obstetrics. American Journal of Obstetrics and Gynecology, 217(2), 167–175.
Ananth, C. V., & VanderWeele, T. J. (2011). Placental abruption and perinatal mortality with preterm delivery as a mediator: Disentangling direct and indirect effects. American Journal of Epidemiology, 174(1), 99–108.
Christensen, D. L., Baio, J., et al. (2016). Prevalence and characteristics of autism spectrum disorder among children aged 8 years—Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2012. MMWR Surveillance Summary, 65(3), 1–23.
Clements, K. M., Barfield, W. D., et al. (2006). Birth characteristics associated with early intervention referral, evaluation for eligibility, and program eligibility in the first year of life. Maternal and Child Health Journal, 10(5), 433–441.
Conti, E., Mazzotti, S., et al. (2013). Are children born after assisted reproductive technology at increased risk of autism spectrum disorders? A systematic review. Human Reproduction, 28(12), 3316–3327.
Croen, L. A., Najjar, D. V., et al. (2007). Maternal and paternal age and risk of autism spectrum disorders. Archives of Pediatrics and Adolescent Medicine, 161(4), 334–340.
Dai, Y. G., Miller, L. E., et al. (2019). Incremental utility of 24-month autism spectrum disorder screening after negative 18-month screening. Journal of Autism and Developmental Disorders. https://doi.org/10.1007/s10803-019-03959-5.
Declercq, E. R., Belanoff, C., et al. (2014). Identifying women with indicators of subfertility in a statewide population database: Operationalizing the missing link in assisted reproductive technology research. Fertility and Sterility, 101(2), 463–471.
Declercq, E., Luke, B., et al. (2015). Perinatal outcomes associated with assisted reproductive technology: The Massachusetts Outcomes Study of Assisted Reproductive Technologies (MOSART). Fertility and Sterility, 103(4), 888–895.
Diop, H., Gopal, D., et al. (2016). Assisted reproductive technology and early intervention program enrollment. Pediatrics, 137(3), e20152007.
Duby, J. C., Lipkin, P. H., et al. (2006). Identifying infants and young children with developmental disorders in the medical home: An algorithm for developmental surveillance and screening. Pediatrics, 118(1), 405–420.
First, M. B. (2013). Diagnostic and statistical manual of mental disorders, 5th edition, and clinical utility. Journal of Nervous and Mental Disease, 201(9), 727–729.
Fombonne, E., Zakarian, R., et al. (2006). Pervasive developmental disorders in Montreal, Quebec, Canada: Prevalence and links with immunizations. Pediatrics, 118(1), e139–e150.
Grether, J. K., Qian, Y., et al. (2013). Is infertility associated with childhood autism? Journal of Autism and Developmental Disorders, 43(3), 663–672.
Hvidtjorn, D., Grove, J., et al. (2011). Risk of autism spectrum disorders in children born after assisted conception: A population-based follow-up study. Journal of Epidemiology and Community Health, 65(6), 497–502.
Johnson, C. P., & Myers, S. M. (2007). Identification and evaluation of children with autism spectrum disorders. Pediatrics, 120(5), 1183–1215.
Kissin, D. M., Zhang, Y., et al. (2015). Association of assisted reproductive technology (ART) treatment and parental infertility diagnosis with autism in ART-conceived children. Human Reproduction, 30(2), 454–465.
Kotelchuck, M., Hoang, L., et al. (2014). The MOSART database: Linking the SART CORS clinical database to the population-based Massachusetts PELL reproductive public health data system. Maternal and Child Health Journal, 18(9), 2167–2178.
Kotsopoulos, S. (2015). Early diagnosis of autism: Phenotype–endophenotype. Psychiatriki, 25(4), 273–281.
Luke, B., Brown, M. B., et al. (2012). Cumulative birth rates with linked assisted reproductive technology cycles. New England Journal of Medicine, 366(26), 2483–2491.
Luke, B., Stern, J. E., et al. (2015). Birth outcomes by infertility diagnosis analyses of the Massachusetts Outcomes Study of Assisted Reproductive Technologies (MOSART). Journal of Reproductive Medicine, 60(11–12), 480–490.
Luke, B., Stern, J. E., et al. (2016a). Is the wrong question being asked in infertility research? Journal of Assisted Reproduction and Genetics, 33(1), 3–8.
Luke, B., Stern, J. E., et al. (2016b). Birth outcomes by infertility treatment: Analyses of the population-based cohort: Massachusetts Outcomes Study of Assisted Reproductive Technologies (MOSART). Journal of Reproductive Medicine, 61(3–4), 114–127.
Lyall, K., Pauls, D. L., et al. (2012). Fertility therapies, infertility and autism spectrum disorders in the Nurses’ Health Study II. Paediatric and Perinatal Epidemiology, 26(4), 361–372.
MacKinnon, D. P., Fairchild, A. J., et al. (2007). Mediation analysis. Annual Review of Psychology, 58, 593–614.
Maenner, M. J., Schieve, L. A., et al. (2013). Frequency and pattern of documented diagnostic features and the age of autism identification. Journal of the American Academy of Child and Adolescent Psychiatry, 52(4), 401–413.e408.
Maimburg, R. D., & Vaeth, M. (2007). Do children born after assisted conception have less risk of developing infantile autism? Human Reproduction, 22(7), 1841–1843.
Manning, S. E., Davin, C. A., et al. (2011). Early diagnoses of autism spectrum disorders in Massachusetts birth cohorts, 2001–2005. Pediatrics, 127(6), 1043–1051.
Muhle, R., Trentacoste, S. V., et al. (2004). The genetics of autism. Pediatrics, 113(5), e472–e486.
Nannini, A., Lazar, J., et al. (2011). Rates of hospital visits for assault during pregnancy and the year postpartum: Timing matters. Public Health Reports, 126(5), 664–668.
Newschaffer, C. J., Falb, M. D., et al. (2005). National autism prevalence trends from United States special education data. Pediatrics, 115(3), e277–e282.
Pandey, S., Shetty, A., et al. (2012). Obstetric and perinatal outcomes in singleton pregnancies resulting from IVF/ICSI: A systematic review and meta-analysis. Human Reproduction Update, 18(5), 485–503.
Parner, E. T., Schendel, D. E., et al. (2008). Autism prevalence trends over time in Denmark: Changes in prevalence and age at diagnosis. Archives of Pediatrics and Adolescent Medicine, 162(12), 1150–1156.
Perri, T., Chen, R., et al. (2001). Are singleton assisted reproductive technology pregnancies at risk of prematurity? Journal of Assisted Reproduction and Genetics, 18(5), 245–249.
Reichenberg, A., Gross, R., et al. (2010). Advancing paternal and maternal age are both important for autism risk. American Journal of Public Health, 100(5), 772–773; author reply 773.
Rogers, S. J., Vismara, L., et al. (2014). Autism treatment in the first year of life: A pilot study of infant start, a parent-implemented intervention for symptomatic infants. Journal of Autism and Developmental Disorders, 44(12), 2981–2995.
Schieve, L. A., Ferre, C., et al. (2004). Perinatal outcome among singleton infants conceived through assisted reproductive technology in the United States. Obstetrics and Gynecology, 103(6), 1144–1153.
Snow, A. V., & Lecavalier, L. (2008). Sensitivity and specificity of the Modified Checklist for Autism in Toddlers and the Social Communication Questionnaire in preschoolers suspected of having pervasive developmental disorders. Autism, 12(6), 627–644.
Sunderam, S., Kissin, D. M., et al. (2013). Assisted reproductive technology surveillance—United States, 2010. MMWR Surveillance Summary, 62(9), 1–24.
Valeri, L., & Vanderweele, T. J. (2013). Mediation analysis allowing for exposure–mediator interactions and causal interpretation: Theoretical assumptions and implementation with SAS and SPSS macros. Psychological Methods, 18(2), 137–150.
Wright, V. C., Schieve, L. A., et al. (2003). Assisted reproductive technology surveillance–United States, 2000. MMWR Surveillance Summary, 52(9), 1–16.
Acknowledgements
The authors would like to thank SART Members for providing clinical information to the SART CORS database for use by patients and researchers. Without the efforts of SART Members, this research would not have been possible. The authors also want to thank Gabriela Kernan from the Massachusetts Department of Public Health for providing technical support around EI data acquisition. This work was supported by R01HD064595 and R01HD067270. The views expressed in this article are those of the authors and do not necessarily represent the official view of the National Institutes of Health or the Massachusetts Department of Public Health.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Diop, H., Cabral, H., Gopal, D. et al. Early Autism Spectrum Disorders in Children Born to Fertile, Subfertile, and ART-Treated Women. Matern Child Health J 23, 1489–1499 (2019). https://doi.org/10.1007/s10995-019-02770-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-019-02770-z