Abstract
Introduction
While minimally invasive left pancreatectomy has become more widespread and generally accepted over the last decade, opinions on modality of minimally invasive approach (robotic or laparoscopic) remain mixed with few institutions performing a significant portion of both operative approaches simultaneously.
Methods
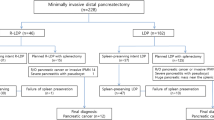
247 minimally invasive left pancreatectomies were retrospectively identified in a prospectively maintained institutional REDCap™ database, 135 laparoscopic left pancreatectomy (LLP) and 108 robotic-assisted left pancreatectomy (RLP). Demographics, intraoperative variables, postoperative outcomes, and OR costs were compared between LLP and RLP with an additional subgroup analysis for procedures performed specifically for pancreatic adenocarcinoma (35 LLP and 23 RLP) focusing on pathologic outcomes and 2-year actuarial survival.
Results
There were no significant differences in preoperative demographics or indications between LLP and RLP with 34% performed for chronic pancreatitis and 23% performed for pancreatic adenocarcinoma. While laparoscopic cases were faster (p < 0.001) robotic cases had a higher rate of splenic preservation (p < 0.001). Median length of stay was 5 days for RLP and LLP, and rate of clinically significant grade B/C pancreatic fistula was approximately 20% for both groups. Conversion rates to laparotomy were 4.3% and 1.8% for LLP and RLP approaches respectively. RLP had a higher rate of readmission (p = 0.035). Pathologic outcomes and 2-year actuarial survival were similar between LLP and RLP. LLP on average saved $206.67 in OR costs over RLP.
Conclusions
This study demonstrates that at a high-volume center with significant minimally invasive experience, both LLP and RLP can be equally effective when used at the discretion of the operating surgeon. We view the laparoscopic and robotic platforms as tools for the modern surgeon, and at our institution, given the technical success of both operative approaches, we will continue to encourage our surgeons to approach a difficult operation with their tool of choice.
Graphical abstract


Similar content being viewed by others
References
Konstantinidis IT, Lewis A, Lee B et al (2017) Minimally invasive distal pancreatectomy: greatest benefit for the frail. Surg Endosc 31:5234–5240
de Rooij T, van Hilst J, Boerma D et al (2016) Impact of a nationwide training program in minimally invasive distal pancreatectomy (LAELAPS). Ann Surg 264(5):754–762
Matsuoka L, Parekh D (2012) The minimally invasive approach to surgical management of pancreatic diseases. Gastroenterol Clin North Am 41(1):77–101
Boggi U, Napoli N, Costa F et al (2016) Robotic-assisted pancreatic resections. World J Surg 40(10):2497–2506
Plotkin A, Ceppa EP, Zarzaur BL, Kilbane EM, Riall TS, Pitt HA (2017) Reduced morbidity with minimally invasive distal pancreatectomy for pancreatic adenocarcinoma. HPB 19(3):279–285
Selby LV, DeMatteo RP, Tholey RM et al (2017) Evolving application of minimally invasive cancer operations at a tertiary cancer center. J Surg Oncol 115(4):365–370
Zureikat AH, Moser AJ, Boone BA, Bartlett DL, Zenati M, Zeh HJ III (2013) 250 robotic pancreatic resections: safety and feasibility. Ann Surg 258(4):554–559 (discussion 559–562)
de Rooij T, Besselink MG, Shamali A et al (2016) Pan-European survey on the implementation of minimally invasive pancreatic surgery with emphasis on cancer. HPB 18(2):170–176
Gavriilidis P, Lim C, Menahem B, Lahat E, Salloum C, Azoulay D (2016) Robotic versus laparoscopic distal pancreatectomy—the first meta-analysis. HPB 18(7):567–574
Daouadi M, Zureikat AH, Zenati MS et al (2013) Robot-assisted minimally invasive distal pancreatectomy is superior to the laparoscopic technique. Ann Surg 257(1):128–132
Goh BK, Chan CY, Soh HL et al (2017) A comparison between robotic-assisted laparoscopic distal pancreatectomy versus laparoscopic distal pancreatectomy. Int J Med Robot 13(1):e1733
Liu R, Liu Q, Zhao ZM, Tan XL, Gao YX, Zhao GD (2017) Robotic versus laparoscopic distal pancreatectomy: a propensity score-matched study. J Surg Oncol 116:461–469
Lee SY, Allen PJ, Sadot E et al (2015) Distal pancreatectomy: a single institution’s experience in open, laparoscopic, and robotic approaches. J Am Coll Surg 220(1):18–27
Xourafas D, Ashley SW, Clancy TE (2017) Comparison of perioperative outcomes between open, laparoscopic, and robotic distal pancreatectomy: an analysis of 1815 patients from the ACS-NSQIP procedure-targeted pancreatectomy database. J Gastrointest Surg 21:1442–1452
Ielpo B, Duran H, Diaz E et al (2017) Robotic versus laparoscopic distal pancreatectomy: a comparative study of clinical outcomes and costs analysis. Int J Surg 48:300–304
Souche R, Herrero A, Bourel G et al (2018) Robotic versus laparoscopic distal pancreatectomy: a French prospective single-center experience and cost-effectiveness analysis. Surg Endosc 32:3562–3569
Gebauer F, Tachezy M, Vashist YK et al (2015) Resection margin clearance in pancreatic cancer after implementation of the Leeds Pathology Protocol (LEEPP): clinically relevant or just academic? World J Surg 39(2):493–499
Strasberg SM, Fields R (2012) Left-sided pancreatic cancer: distal pancreatectomy and its variants: radical antegrade modular pancreatosplenectomy and distal pancreatectomy with celiac axis resection. Cancer J 18(6):562–570
Chen S, Zhan Q, Chen JZ et al (2015) Robotic approach improves spleen-preserving rate and shortens postoperative hospital stay of laparoscopic distal pancreatectomy: a matched cohort study. Surg Endosc 29(12):3507–3518
Bassi C, Marchegiani G, Dervenis C et al (2017) The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery 161(3):584–591
Guerrini GP, Lauretta A, Belluco C et al (2017) Robotic versus laparoscopic distal pancreatectomy: an up-to-date meta-analysis. BMC Surg 17(1):105
Nassour I, Wang SC, Porembka MR et al (2017) Conversion of minimally invasive distal pancreatectomy: predictors and outcomes. Ann Surg Oncol 24(12):3725–3731
Wright GP, Zureikat AH (2016) Development of minimally invasive pancreatic surgery: an evidence-based systematic review of laparoscopic versus robotic approaches. J Gastrointest Surg 20(9):1658–1665
Zureikat AH, Borrebach J, Pitt HA et al (2017) Minimally invasive hepatopancreatobiliary surgery in North America: an ACS-NSQIP analysis of predictors of conversion for laparoscopic and robotic pancreatectomy and hepatectomy. HPB 19(7):595–602
Hanna EM, Rozario N, Rupp C, Sindram D, Iannitti DA, Martinie JB (2013) Robotic hepatobiliary and pancreatic surgery: lessons learned and predictors for conversion. Int J Med Robot 9(2):152–159
Adam MA, Thomas S, Youngwirth L, Pappas T, Roman SA, Sosa JA (2017) Defining a hospital volume threshold for minimally invasive pancreaticoduodenectomy in the United States. JAMA Surg 152(4):336–342
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Lyman reports grants from Intuitive Surgical, outside the submitted work. Dr. Iannitti reports personal fees from Ethicon, grants and personal fees from Medtronic, outside the submitted work. Dr. Vrochides reports personal fees from Ethicon, grants from Intuitive Surgical, outside the submitted work. Dr. Martinie reports grants and personal fees from Intuitive Surgical, personal fees from Ethicon, personal fees from Medtronic, outside the submitted work. Dr. Passeri, Dr. Sastry, Dr. Baker, and Ms. Cochran have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Lyman, W.B., Passeri, M., Sastry, A. et al. Robotic-assisted versus laparoscopic left pancreatectomy at a high-volume, minimally invasive center. Surg Endosc 33, 2991–3000 (2019). https://doi.org/10.1007/s00464-018-6565-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6565-6