Summary
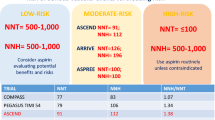
According to metaanalysis and the results of the two studies with the highest power, aspirin is effective in primary prevention of coronary heart disease. These beneficial effects, however, are at least partially out-weight by unwanted effects—such as intense gastrointestinal bleeding and hemorrhagic stroke. These side effects remain constant with increasing risk of coronary heart disease, whereas the protective effects increase. If an annual risk of coronary heart disease of ≤0.6% exists, aspirin is normally not indicated; for a risk of 0.7–1.4% the facts should be discussed with the patient. If a risk of ≥1.5% exists, aspirin should be given.
Problems of aspirin therapy—such as “aspirin paradox” and “aspirin resistance”—have been documented for secondary prevention; they might, however, have likewise clinical implications in primary prevention.
Zusammenfassung
In der Metaanalyse sowie nach den Ergebnissen der beiden Studien mit der höchsten Power zeigt Aspirin einen protektiven Effekt in der Primärprävention der koronaren Herzerkrankung. Dieser günstigen Wirkung stehen unerwünschte—wie stärkere gastrointestinale Blutungen oder hämorrhagische Schlaganfälle—entgegen. Diese bleiben jedoch mit steigendem koronarem Herzerkrankungsrisiko konstant, während die protektiven Effekte zunehmen. Bei einem jährlichen KHK-Risiko von 0,6% ist deshalb die Indikation für die Gabe von Aspirin in der Regel nicht gegeben; bei einem Risiko von 0,7–1,4% sollte die Problematik mit dem Patienten besprochen werden. Bei einem Risiko ≥1,5% sollte Aspirin gegeben werden. Probleme der Aspirintherapie wie das „Aspirinparadox“ und die „Aspirinresistenz“ wurden im Rahmen der Sekundärprävention aufgezeigt, sie dürften aber auch für die Primärprävention von Bedeutung sein.
Similar content being viewed by others
References
Alexander JH, Harrington RA, Tuttle RH et al. (1999) Prior aspirin use predicts worse outcomes in patients with non-ST-elevation acute coronary syndromes. Am J Cardiol 83:1147–1151
Collaborative Group of the Primary Prevention Project (2001) Low-dose aspirin and vitamin E in people at cardiovascular risk: a randomised trial in general practice. Lancet 357:89–95
Gaspoz JM, Coxson PG, Goldman PA, Williams LW, Kuntz KM, Hunink MG (2002) Cost effectiveness of aspirin, clopidogrel or both for secondary prevention of coronary heart disease. N Engl J Med 346:1800–1806
Gum PA, Kottke-Marchant K, Welsh PA et al (2003) A prospective, blinded determination of the natural history of aspirin resistance among stable patients with cardiovasvular disease. J Am Coll Cardiol 41:961–965
Gurbel, PA, Bliden KP, Hiatt BL et al (2003) Clopidogrel for coronary stenting: response variability, drug resistance, and the effect of pretreatment platelet reactivity. Circulation 107:2908–2913
Hansson L, Zanchetti A, Carruthers SG et al (1998) Effects of intensive blood-pressure lowering and lowdose aspirin in patients with hypertension: principal results of the hypertension optimal treamtent (HOT) randomised trial. Lancet 351:1755–1762
Hayden M, Pignone M, Phillips C, Mulrow C (2002) Aspirin for the primary prevention of cardiovascular events: a summary of the evidence for the US Preventive Services Task Force. Ann Intern Med 136:161–172
Helgason CM, Bolin KM, Hoff JA et al (1994) Development of aspirin resistance in persons with previous ischemic stroke. Stroke 25:2331–2336
Kurth T, Glynn RJ, Walker AM et al. (2003) Inhibition of clinical benefits of aspirin on first myocardial infarction by nonsteroidal antiinflammatory drugs. Circulation 108:1191–1195
Lancaster GI, Lancaster CJ, Radley D, Cohen M (2001) Prior aspirin use in unstable angina predisposes to higher risk. The aspirin paradox. Int J Cardiol 80:201–207
Lau WC, Waskell LA, Watkins PB et al (2003) Atorvastatin reduces the ability of clopidogrel to inhibit platelet aggregation: a new drug-drug interaction. Circulation 107:32–37
Lauer MS (2002) Aspirin for primary prevention of coronary events. N Engl J Med 346:1468–1474
MacDonald TM, Wei L (2003) Effect of ibuprofen on cardiovascular effect of aspirin. Lancet 361:573–574
O’Donnell CJ, Larson MG, Feng D et al (2001) Genetic and environmental contributions to platelet aggregation: the Framingham Heart Study. Circulation 103:3051–3056
Peto R, Gray R, Collins R et al (1988) Randomised trial of prophylactic daily aspirin in British male doctors. BMJ 296:313–316
Quinn MJ, Topol EJ (2001) Common variations in platelet glycoproteins: pharmacogenomic implications. Pharmacogenomics 2:341–352
Santopinto J, Gurfinktel EP, Torres V et al (2001) Prior aspirin users with acute non-ST-elevation coronary syndromes are at increased risk of cardiac events and benefit from enoxaparin. Am Heart J 141:566–572
Saw J, Steinhubl SR, Berger PB et al (2003) Lack of adverse clopidogrelatorvastatin clinical interaction from secondary analysis of a randomized, placebo-controlled clopidogrel trial. Circulation 108:921–924
Schafer AI (2003) Genetic and acquired determinants of indivual variability of response to antiplatelet drugs. Circulation 108:910–911
Soffer D, Moussa I, Harjai KJ et al (2003) Impact of angina class on inhibition of platelet aggregation following clopidogrel loading in patients undergoing intervention: do we need more aggressive dosing regimens in unstable angina? Cath Cardiovasc Intervent 59:21–25
Steering Committee of the Physicians’ Health Study Research Group (1989) Final report on the aspirin component of the ongoing physicians’ health study. N Engl J Med 321:129–135
The Medical Research Council’s General Practice Research Framework (1998) Thrombosis prevention trial: randomised trial of low-intensity oral anticoagulation with warfarin and low-dose aspirin in the primary prevention of ischemic heart disease in men at increased risk. Lancet 351:233–241
USPST (2002) Aspirin for the primary prevention of cardiovascular events: US Preventive Services Task Force. Ann Intern Med 136:157–160
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kübler, W., Darius, H. Primäre Prävention der koronaren Herzkrankheit mit Aspirin. ZS Kardiologie 94 (Suppl 3), iii66–iii73 (2005). https://doi.org/10.1007/s00392-005-1309-8
Issue Date:
DOI: https://doi.org/10.1007/s00392-005-1309-8