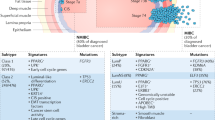
Abstract
Purpose
To provide a condensed summary of the Basic Science chapter that was included in the Third International Consultation on Bladder Cancer.
Methods
World bladder cancer basic science experts used the published literature to create summaries of recent progress in their areas of expertise.
Results
The completion of several large-scale genomics projects coupled with a strong collaborative culture within the research community and the exciting clinical activity of immune checkpoint blockade have combined to transform the bladder cancer research landscape. Bladder cancer molecular subtypes and the presence of specific DNA alterations provide important information about disease heterogeneity that has direct implications for clinical management, and some can be targeted by compounds that are already clinically available. Tests are being developed that can measure many of these alterations non-invasively in peripheral blood or urine, raising confidence that they could be used as biomarkers for surveillance and monitoring the effects of local and systemic therapies.
Conclusions
Although the bulk of the mechanistic work lies ahead, the genomics results have created a hypothesis-generating description of bladder cancer heterogeneity that has set the stage for deeper mechanistic studies, and they have already provided us with extremely attractive candidate biomarkers to guide clinical practice. Here, we will summarize the recent progress in basic bladder cancer research and highlight near-term opportunities for the future.




Similar content being viewed by others
References
Kamat AM, Hahn NM, Efstathiou JA, Lerner SP, Malmstrom PU, Choi W et al (2016) Bladder cancer. Lancet 388(10061):2796–2810
Knowles MA, Hurst CD (2015) Molecular biology of bladder cancer: new insights into pathogenesis and clinical diversity. Nat Rev Cancer 15(1):25–41
Czerniak B, Dinney C, McConkey D (2016) Origins of Bladder Cancer. Annu Rev Pathol 11:149–174
Dyrskjot L, Thykjaer T, Kruhoffer M, Jensen JL, Marcussen N, Hamilton-Dutoit S et al (2003) Identifying distinct classes of bladder carcinoma using microarrays. Nat Genet 33(1):90–96
Lindgren D, Frigyesi A, Gudjonsson S, Sjodahl G, Hallden C, Chebil G et al (2010) Combined gene expression and genomic profiling define two intrinsic molecular subtypes of urothelial carcinoma and gene signatures for molecular grading and outcome. Cancer Res 70(9):3463–3472
Sanchez-Carbayo M, Socci ND, Lozano J, Saint F, Cordon-Cardo C (2006) Defining molecular profiles of poor outcome in patients with invasive bladder cancer using oligonucleotide microarrays. J Clin Oncol 24(5):778–789
Sjodahl G, Lauss M, Lovgren K, Chebil G, Gudjonsson S, Veerla S et al (2012) A molecular taxonomy for urothelial carcinoma. Clin Cancer Res 18(12):3377–3386
Cancer Genome Atlas Research N (2014) Comprehensive molecular characterization of urothelial bladder carcinoma. Nature 507(7492):315–322
Damrauer JS, Hoadley KA, Chism DD, Fan C, Tiganelli CJ, Wobker SE et al (2014) Intrinsic subtypes of high-grade bladder cancer reflect the hallmarks of breast cancer biology. Proc Natl Acad Sci USA 111(8):3110–3115
Choi W, Porten S, Kim S, Willis D, Plimack ER, Hoffman-Censits J et al (2014) Identification of distinct basal and luminal subtypes of muscle-invasive bladder cancer with different sensitivities to frontline chemotherapy. Cancer Cell 25(2):152–165
Aine M, Eriksson P, Liedberg F, Sjodahl G, Hoglund M (2015) Biological determinants of bladder cancer gene expression subtypes. Sci Rep. 5:10957
Sjodahl G, Eriksson P, Liedberg F, Hoglund M (2017) Molecular classification of urothelial carcinoma: global mRNA classification versus tumour-cell phenotype classification. J Pathol 242(1):113–125
Hennessy BT, Gonzalez-Angulo AM, Stemke-Hale K, Gilcrease MZ, Krishnamurthy S, Lee JS et al (2009) Characterization of a naturally occurring breast cancer subset enriched in epithelial-to-mesenchymal transition and stem cell characteristics. Cancer Res 69(10):4116–4124
Robertson AG, Kim J, Al-Ahmadie H, Bellmunt J, Guo G, Cherniack AD et al (2017) Comprehensive molecular characterization of muscle-invasive bladder cancer. Cell 171(3):540-56 e25
Guo CC, Dadhania V, Zhang L, Majewski T, Bondaruk J, Sykulski M et al (2016) Gene expression profile of the clinically aggressive micropapillary variant of bladder cancer. Eur Urol 70(4):611–620
Warrick JI, Kaag M, Raman JD, Chan W, Tran T, Kunchala S et al (2017) FOXA1 and CK14 as markers of luminal and basal subtypes in histologic variants of bladder cancer and their associated conventional urothelial carcinoma. Virchows Arch 471(3):337–345
Hedegaard J, Lamy P, Nordentoft I, Algaba F, Hoyer S, Ulhoi BP et al (2016) Comprehensive transcriptional analysis of early-stage urothelial carcinoma. Cancer Cell 30(1):27–42
McConkey DJ, Choi W, Shen Y, Lee IL, Porten S, Matin SF et al (2016) A prognostic gene expression signature in the molecular classification of chemotherapy-naive urothelial cancer is predictive of clinical outcomes from neoadjuvant chemotherapy: a phase 2 trial of dose-dense methotrexate, vinblastine, doxorubicin, and cisplatin with bevacizumab in urothelial cancer. Eur Urol 69(5):855–862
Seiler R, Ashab HAD, Erho N, van Rhijn BWG, Winters B, Douglas J et al (2017) Impact of molecular subtypes in muscle-invasive bladder cancer on predicting response and survival after neoadjuvant chemotherapy. Eur Urol 72(4):544–554
Rosenberg JE, Hoffman-Censits J, Powles T, van der Heijden MS, Balar AV, Necchi A et al (2016) Atezolizumab in patients with locally advanced and metastatic urothelial carcinoma who have progressed following treatment with platinum-based chemotherapy: a single-arm, multicentre, phase 2 trial. Lancet 387(10031):1909–1920
Mariathasan S, Turley SJ, Nickles D, Castiglioni A, Yuen K, Wang Y et al (2018) TGFbeta attenuates tumour response to PD-L1 blockade by contributing to exclusion of T cells. Nature 554(7693):544–548
Dinney CP, Hansel D, McConkey D, Shipley W, Hagan M, Dreicer R et al (2014) Novel neoadjuvant therapy paradigms for bladder cancer: results from the National Cancer Center Institute Forum. Urol Oncol. 32(8):1108–1115
Ochoa AE, Choi W, Su X, Siefker-Radtke A, Czerniak B, Dinney C et al (2016) Specific micro-RNA expression patterns distinguish the basal and luminal subtypes of muscle-invasive bladder cancer. Oncotarget. 7(49):80164–80174
Ho PL, Kurtova A, Chan KS (2012) Normal and neoplastic urothelial stem cells: getting to the root of the problem. Nat Rev Urol. 9(10):583–594
Varley CL, Stahlschmidt J, Lee WC, Holder J, Diggle C, Selby PJ et al (2004) Role of PPARgamma and EGFR signalling in the urothelial terminal differentiation programme. J Cell Sci 117(Pt 10):2029–2036
Varley CL, Stahlschmidt J, Smith B, Stower M, Southgate J (2004) Activation of peroxisome proliferator-activated receptor-gamma reverses squamous metaplasia and induces transitional differentiation in normal human urothelial cells. Am J Pathol 164(5):1789–1798
Varley CL, Bacon EJ, Holder JC, Southgate J (2009) FOXA1 and IRF-1 intermediary transcriptional regulators of PPARgamma-induced urothelial cytodifferentiation. Cell Death Differ 16(1):103–114
Biton A, Bernard-Pierrot I, Lou Y, Krucker C, Chapeaublanc E, Rubio-Perez C et al (2014) Independent component analysis uncovers the landscape of the bladder tumor transcriptome and reveals insights into luminal and basal subtypes. Cell Rep. 9(4):1235–1245
Chan KS, Espinosa I, Chao M, Wong D, Ailles L, Diehn M et al (2009) Identification, molecular characterization, clinical prognosis, and therapeutic targeting of human bladder tumor-initiating cells. Proc Natl Acad Sci USA 106(33):14016–14021
He X, Marchionni L, Hansel DE, Yu W, Sood A, Yang J et al (2009) Differentiation of a highly tumorigenic basal cell compartment in urothelial carcinoma. Stem Cells. 27(7):1487–1495
Yang YM, Chang JW (2008) Bladder cancer initiating cells (BCICs) are among EMA-CD44v6 + subset: novel methods for isolating undetermined cancer stem (initiating) cells. Cancer Invest 26(7):725–733
Su Y, Qiu Q, Zhang X, Jiang Z, Leng Q, Liu Z et al (2010) Aldehyde dehydrogenase 1 A1-positive cell population is enriched in tumor-initiating cells and associated with progression of bladder cancer. Cancer Epidemiol, Biomark Prevent Publ Am Assoc Cancer Res, cosponsored by the American Society of Preventive Oncology. 19(2):327–337
Volkmer JP, Sahoo D, Chin RK, Ho PL, Tang C, Kurtova AV et al (2012) Three differentiation states risk-stratify bladder cancer into distinct subtypes. Proc Natl Acad Sci USA 109(6):2078–2083
Huang P, Watanabe M, Kaku H, Ueki H, Noguchi H, Sugimoto M et al (2013) Cancer stem cell-like characteristics of a CD133(+) subpopulation in the J82 human bladder cancer cell line. Mol Clin Oncol. 1(1):180–184
Cheah MT, Chen JY, Sahoo D, Contreras-Trujillo H, Volkmer AK, Scheeren FA et al (2015) CD14-expressing cancer cells establish the inflammatory and proliferative tumor microenvironment in bladder cancer. Proc Natl Acad Sci USA 112(15):4725–4730
Kurtova AV, Xiao J, Mo Q, Pazhanisamy S, Krasnow R, Lerner SP et al (2015) Blocking PGE2-induced tumour repopulation abrogates bladder cancer chemoresistance. Nature 517(7533):209–213
Yang Z, Li C, Fan Z, Liu H, Zhang X, Cai Z et al (2017) Single-cell sequencing reveals variants in ARID1A, GPRC5A and MLL2 driving self-renewal of human bladder cancer stem cells. Eur Urol 71(1):8–12
Li C, Wu S, Wang H, Bi X, Yang Z, Du Y et al (2015) The C228T mutation of TERT promoter frequently occurs in bladder cancer stem cells and contributes to tumorigenesis of bladder cancer. Oncotarget. 6(23):19542–19551
Gui Y, Guo G, Huang Y, Hu X, Tang A, Gao S et al (2011) Frequent mutations of chromatin remodeling genes in transitional cell carcinoma of the bladder. Nat Genet 43(9):875–878
Allory Y, Beukers W, Sagrera A, Flandez M, Marques M, Marquez M et al (2014) Telomerase reverse transcriptase promoter mutations in bladder cancer: high frequency across stages, detection in urine, and lack of association with outcome. Eur Urol 65(2):360–366
Ho PL, Lay EJ, Jian W, Parra D, Chan KS (2012) Stat3 activation in urothelial stem cells leads to direct progression to invasive bladder cancer. Can Res 72(13):3135–3142
Yang Z, He L, Lin K, Zhang Y, Deng A, Liang Y et al (2017) The KMT1A-GATA3-STAT3 circuit is a novel self-renewal signaling of human bladder cancer stem cells. Clin Cancer Res 23(21):6673–6685
Shin K, Lim A, Zhao C, Sahoo D, Pan Y, Spiekerkoetter E et al (2014) Hedgehog signaling restrains bladder cancer progression by eliciting stromal production of urothelial differentiation factors. Cancer Cell 26(4):521–533
Chan KS (2016) Molecular pathways: targeting cancer stem cells awakened by chemotherapy to abrogate tumor repopulation. Clin Cancer Res 22(4):802–806
Venkatesan S, Rosenthal R, Kanu N, McGranahan N, Bartek J, Quezada SA et al (2018) Perspective: APOBEC mutagenesis in drug resistance and immune escape in HIV and cancer evolution. Ann Oncol 29(3):563–572
Kim J, Mouw KW, Polak P, Braunstein LZ, Kamburov A, Kwiatkowski DJ et al (2016) Somatic ERCC2 mutations are associated with a distinct genomic signature in urothelial tumors. Nat Genet 48(6):600–606
Van Allen EM, Mouw KW, Kim P, Iyer G, Wagle N, Al-Ahmadie H et al (2014) Somatic ERCC2 mutations correlate with cisplatin sensitivity in muscle-invasive urothelial carcinoma. Cancer Discov 4(10):1140–1153
Li Q, Damish A, Frazier ZJ, Liu D, Reznichenko E, Kamburov A, et al (2018) ERCC2 Helicase Domain mutations confer nucleotide excision repair deficiency and drive cisplatin sensitivity in muscle-invasive bladder cancer. Clin Cancer Res
Plimack ER, Dunbrack RL, Brennan TA, Andrake MD, Zhou Y, Serebriiskii IG et al (2015) Defects in DNA repair genes predict response to neoadjuvant cisplatin-based chemotherapy in muscle-invasive bladder cancer. Eur Urol 68(6):959–967
Faltas BM, Prandi D, Tagawa ST, Molina AM, Nanus DM, Sternberg C et al (2016) Clonal evolution of chemotherapy-resistant urothelial carcinoma. Nat Genet 48(12):1490–1499
Nordentoft I, Lamy P, Birkenkamp-Demtroder K, Shumansky K, Vang S, Hornshoj H et al (2014) Mutational context and diverse clonal development in early and late bladder cancer. Cell Rep. 7(5):1649–1663
Thomsen MBH, Nordentoft I, Lamy P, Vang S, Reinert L, Mapendano CK et al (2017) Comprehensive multiregional analysis of molecular heterogeneity in bladder cancer. Sci Rep. 7(1):11702
Hurst CD, Alder O, Platt FM, Droop A, Stead LF, Burns JE et al (2017) Genomic subtypes of non-invasive bladder cancer with distinct metabolic profile and female gender bias in KDM6A mutation frequency. Cancer Cell 32(5):701–15 e7
Pietzak EJ, Bagrodia A, Cha EK, Drill EN, Iyer G, Isharwal S et al (2017) Next-generation sequencing of nonmuscle invasive bladder cancer reveals potential biomarkers and rational therapeutic targets. Eur Urol 72(6):952–959
Meeks JJ, Carneiro BA, Pai SG, Oberlin DT, Rademaker A, Fedorchak K et al (2016) Genomic characterization of high-risk non-muscle invasive bladder cancer. Oncotarget. 7(46):75176–75184
Husain H, Velculescu VE (2017) Cancer DNA in the Circulation: the Liquid Biopsy. JAMA 318(13):1272–1274
Kalluri R (2016) The biology and function of exosomes in cancer. J Clin Invest. 126(4):1208–1215
Birkenkamp-Demtroder K, Christensen E, Nordentoft I, Knudsen M, Taber A, Hoyer S et al (2018) Monitoring treatment response and metastatic relapse in advanced bladder cancer by liquid biopsy analysis. Eur Urol 73(4):535–540
Birkenkamp-Demtroder K, Nordentoft I, Christensen E, Hoyer S, Reinert T, Vang S et al (2016) Genomic alterations in liquid biopsies from patients with bladder cancer. Eur Urol 70(1):75–82
Christensen E, Birkenkamp-Demtroder K, Nordentoft I, Hoyer S, van der Keur K, van Kessel K et al (2017) Liquid biopsy analysis of FGFR3 and PIK3CA hotspot mutations for disease surveillance in bladder cancer. Eur Urol 71(6):961–969
Springer SU, Chen CH, Rodriguez Pena MDC, Li L, Douville C, Wang Y et al (2018) Non-invasive detection of urothelial cancer through the analysis of driver gene mutations and aneuploidy. Elife. 7:e32143
Smith E, Shilatifard A (2010) The chromatin signaling pathway: diverse mechanisms of recruitment of histone-modifying enzymes and varied biological outcomes. Mol Cell 40(5):689–701
Fyodorov DV, Zhou BR, Skoultchi AI, Bai Y. Emerging roles of linker histones in regulating chromatin structure and function. Nat Rev Mol Cell Biol. 2017
Jenuwein T, Allis CD (2001) Translating the histone code. Science 293(5532):1074–1080
Robertson AG, Kim J, Al-Ahmadie H, Bellmunt J, Guo G, Cherniack AD et al (2017) Comprehensive molecular characterization of muscle-invasive bladder cancer. Cell
Allis CD, Berger SL, Cote J, Dent S, Jenuwien T, Kouzarides T et al (2007) New nomenclature for chromatin-modifying enzymes. Cell 131(4):633–636
Gao J, Aksoy BA, Dogrusoz U, Dresdner G, Gross B, Sumer SO et al (2013) Integrative analysis of complex cancer genomics and clinical profiles using the cBioPortal. Sci Signal 6(269):pl1
Choi W, Ochoa A, McConkey DJ, Aine M, Hoglund M, Kim WY et al (2017) Genetic alterations in the molecular subtypes of bladder cancer: illustration in the cancer genome atlas dataset. Eur Urol 72(3):354–365
Piunti A, Shilatifard A (2016) Epigenetic balance of gene expression by polycomb and COMPASS families. Science 352(6290):9780
Miller T, Krogan NJ, Dover J, Erdjument-Bromage H, Tempst P, Johnston M et al (2001) COMPASS: a complex of proteins associated with a trithorax-related SET domain protein. Proc Natl Acad Sci USA 98(23):12902–12907
Ntziachristos P, Tsirigos A, Welstead GG, Trimarchi T, Bakogianni S, Xu L et al (2014) Contrasting roles of histone 3 lysine 27 demethylases in acute lymphoblastic leukaemia. Nature 514(7523):513–517
Ler LD, Ghosh S, Chai X, Thike AA, Heng HL, Siew EY et al (2017) Loss of tumor suppressor KDM6A amplifies PRC2-regulated transcriptional repression in bladder cancer and can be targeted through inhibition of EZH2. Sci Transl Med 9(378):eaai8312
Pietzak EJ, Bagrodia A, Cha EK, Drill EN, Iyer G, Isharwal S et al (2017) Next-generation sequencing of nonmuscle invasive bladder cancer reveals potential biomarkers and rational therapeutic targets. Eur Urol
Bitler BG, Aird KM, Garipov A, Li H, Amatangelo M, Kossenkov AV et al (2015) Synthetic lethality by targeting EZH2 methyltransferase activity in ARID1A-mutated cancers. Nat Med 21(3):231–238
Jin F, Thaiparambil J, Donepudi SR, Vantaku V, Piyarathna DWB, Maity S et al (2017) Tobacco-specific carcinogens induce hypermethylation, DNA adducts, and DNA damage in bladder cancer. Cancer Prev Res (Phila) 10(10):588–597
Shen C, Sun Z, Chen D, Su X, Jiang J, Li G et al (2015) Developing urinary metabolomic signatures as early bladder cancer diagnostic markers. OMICS 19(1):1–11
Rosevear HM, Lightfoot AJ, O’Donnell MA, Griffith TS (2009) The role of neutrophils and TNF-related apoptosis-inducing ligand (TRAIL) in bacillus Calmette–Guerin (BCG) immunotherapy for urothelial carcinoma of the bladder. Cancer Metastasis Rev 28(3–4):345–353
Ratliff TL, Ritchey JK, Yuan JJ, Andriole GL, Catalona WJ (1993) T-cell subsets required for intravesical BCG immunotherapy for bladder cancer. J Urol 150(3):1018–1023
Biot C, Rentsch CA, Gsponer JR, Birkhauser FD, Jusforgues-Saklani H, Lemaitre F et al (2012) Preexisting BCG-specific T cells improve intravesical immunotherapy for bladder cancer. Sci Transl Med 4(137):137ra72
Kavoussi LR, Brown EJ, Ritchey JK, Ratliff TL (1990) Fibronectin-mediated Calmette–Guerin bacillus attachment to murine bladder mucosa. Requirement for the expression of an antitumor response. J Clin Invest 85(1):62–67
Kamat AM, Li R, O’Donnell MA, Black PC, Roupret M, Catto JW et al (2018) Predicting response to intravesical bacillus Calmette–Guerin immunotherapy: are we there yet? A Systematic Review. Eur Urol 73(5):738–748
Lerner SP, Dinney C, Kamat A, Bivalacqua TJ, Nielsen M, O’Donnell M et al (2015) Clarification of bladder cancer disease states following treatment of patients with intravesical BCG. Bladder Cancer. 1(1):29–30
Inman BA, Sebo TJ, Frigola X, Dong H, Bergstralh EJ, Frank I et al (2007) PD-L1 (B7-H1) expression by urothelial carcinoma of the bladder and BCG-induced granulomata: associations with localized stage progression. Cancer 109(8):1499–1505
Dinney CP, Fisher MB, Navai N, O’Donnell MA, Cutler D, Abraham A et al (2013) Phase I trial of intravesical recombinant adenovirus mediated interferon-alpha2b formulated in Syn3 for Bacillus Calmette–Guerin failures in nonmuscle invasive bladder cancer. J Urol 190(3):850–856
Shore ND, Boorjian SA, Canter DJ, Ogan K, Karsh LI, Downs TM et al (2017) Intravesical rAd-IFNalpha/Syn3 for patients with high-grade, bacillus Calmette–Guerin-refractory or relapsed non-muscle-invasive bladder cancer: a phase II randomized study. J Clin Oncol 35(30):3410–3416
Powles T, Necchi A, Rosen G, Hariharan S, Apolo AB (2018) Anti-programmed cell death 1/ligand 1 (PD-1/PD-L1) antibodies for the treatment of urothelial carcinoma: state of the art and future development. Clin Genitourin Cancer. 16(2):117–129
Le DT, Durham JN, Smith KN, Wang H, Bartlett BR, Aulakh LK et al (2017) Mismatch repair deficiency predicts response of solid tumors to PD-1 blockade. Science 357(6349):409–413
Teo MY, Seier K, Ostrovnaya I, Regazzi AM, Kania BE, Moran MM et al (2018) Alterations in DNA damage response and repair genes as potential marker of clinical benefit from PD-1/PD-L1 blockade in advanced urothelial cancers. J Clin Oncol 36(17):1685–1694
Kardos J, Chai S, Mose LE, Selitsky SR, Krishnan B, Saito R et al (2016) Claudin-low bladder tumors are immune infiltrated and actively immune suppressed. JCI Insight. 1(3):e85902
Kawahara T, Furuya K, Nakamura M, Sakamaki K, Osaka K, Ito H et al (2016) Neutrophil-to-lymphocyte ratio is a prognostic marker in bladder cancer patients after radical cystectomy. BMC Cancer. 16:185
D’Andrea D, Moschini M, Gust K, Abufaraj M, Ozsoy M, Mathieu R et al (2017) Prognostic role of neutrophil-to-lymphocyte ratio in primary non-muscle-invasive bladder cancer. Clin Genitourin Cancer. 15(5):e755–e764
Sivan A, Corrales L, Hubert N, Williams JB, Aquino-Michaels K, Earley ZM et al (2015) Commensal Bifidobacterium promotes antitumor immunity and facilitates anti-PD-L1 efficacy. Science 350(6264):1084–1089
Gopalakrishnan V, Spencer CN, Nezi L, Reuben A, Andrews MC, Karpinets TV et al (2018) Gut microbiome modulates response to anti-PD-1 immunotherapy in melanoma patients. Science 359(6371):97–103
Routy B, Le Chatelier E, Derosa L, Duong CPM, Alou MT, Daillere R et al (2018) Gut microbiome influences efficacy of PD-1-based immunotherapy against epithelial tumors. Science 359(6371):91–97
Zitvogel L, Ma Y, Raoult D, Kroemer G, Gajewski TF (2018) The microbiome in cancer immunotherapy: diagnostic tools and therapeutic strategies. Science 359(6382):1366–1370
Lamont FR, Tomlinson DC, Cooper PA, Shnyder SD, Chester JD, Knowles MA (2011) Small molecule FGF receptor inhibitors block FGFR-dependent urothelial carcinoma growth in vitro and in vivo. Br J Cancer 104(1):75–82
Hahn NM, Bivalacqua TJ, Ross AE, Netto GJ, Baras A, Park JC et al (2017) A phase II trial of dovitinib in BCG-unresponsive urothelial carcinoma with FGFR3 mutations or overexpression: hoosier cancer research network trial HCRN 12-157. Clin Cancer Res 23(12):3003–3011
Pal SK, Rosenberg JE, Hoffman-Censits JH, Berger R, Quinn DI, Galsky MD et al (2018) Efficacy of BGJ398, a fibroblast growth factor receptor 1-3 inhibitor, in patients with previously treated advanced urothelial carcinoma with FGFR3 alterations. Cancer Discov 8(7):812–821
Rebouissou S, Bernard-Pierrot I, de Reynies A, Lepage ML, Krucker C, Chapeaublanc E et al (2014) EGFR as a potential therapeutic target for a subset of muscle-invasive bladder cancers presenting a basal-like phenotype. Sci Transl Med 6(244):244ra91
Choudhury NJ, Campanile A, Antic T, Yap KL, Fitzpatrick CA, Wade JL 3rd et al (2016) Afatinib activity in platinum-refractory metastatic urothelial carcinoma in patients with ERBB alterations. J Clin Oncol 34(18):2165–2171
Earl J, Rico D, Carrillo-de-Santa-Pau E, Rodriguez-Santiago B, Mendez-Pertuz M, Auer H et al (2015) The UBC-40 urothelial bladder cancer cell line index: a genomic resource for functional studies. BMC Genomics. 16:403
Saito R, Smith CC, Utsumi T, Bixby LM, Kardos J, Wobker SE et al (2018) Molecular subtype-specific immunocompetent models of high-grade urothelial carcinoma reveal differential neoantigen expression and response to immunotherapy. Cancer Res 78(14):3954–3968
Fantini D, Glaser AP, Rimar KJ, Wang Y, Schipma M, Varghese N et al (2018) A Carcinogen-induced mouse model recapitulates the molecular alterations of human muscle invasive bladder cancer. Oncogene 37(14):1911–1925
Zhang ZT, Pak J, Shapiro E, Sun TT, Wu XR (1999) Urothelium-specific expression of an oncogene in transgenic mice induced the formation of carcinoma in situ and invasive transitional cell carcinoma. Cancer Res 59(14):3512–3517
Puzio-Kuter AM, Castillo-Martin M, Kinkade CW, Wang X, Shen TH, Matos T et al (2009) Inactivation of p53 and Pten promotes invasive bladder cancer. Genes Dev 23(6):675–680
Zhang ZT, Pak J, Huang HY, Shapiro E, Sun TT, Pellicer A et al (2001) Role of Ha-ras activation in superficial papillary pathway of urothelial tumor formation. Oncogene 20(16):1973–1980
Pan CX, Zhang H, Tepper CG, Lin TY, Davis RR, Keck J et al (2015) Development and characterization of bladder cancer patient-derived xenografts for molecularly guided targeted therapy. PLoS ONE 10(8):e0134346
Sachs N, Clevers H (2014) Organoid cultures for the analysis of cancer phenotypes. Curr Opin Genet Dev 24:68–73
Lee SH, Hu W, Matulay JT, Silva MV, Owczarek TB, Kim K et al (2018) Tumor evolution and drug response in patient-derived organoid models of bladder cancer. Cell 173(2):515-28 e17
Ahmed M, Sottnik JL, Dancik GM, Sahu D, Hansel DE, Theodorescu D et al (2016) An osteopontin/CD44 axis in RhoGDI2-mediated metastasis suppression. Cancer Cell 30(3):432–443
Roth B, Jayaratna I, Sundi D, Cheng T, Melquist J, Choi W et al (2017) Employing an orthotopic model to study the role of epithelial-mesenchymal transition in bladder cancer metastasis. Oncotarget. 8(21):34205–34222
Cheung KJ, Gabrielson E, Werb Z, Ewald AJ (2013) Collective invasion in breast cancer requires a conserved basal epithelial program. Cell 155(7):1639–1651
Wang M, Yao LC, Cheng M, Cai D, Martinek J, Pan CX et al (2018) Humanized mice in studying efficacy and mechanisms of PD-1-targeted cancer immunotherapy. FASEB J. 32(3):1537–1549
Acknowledgements
This summary is based on the work of the following experts who contributed original sections to the International Consultation of Urologic Disease’s Consultation in Bladder Cancer (Basic Research section): Simon C Baker, Jack Birch Unit of Molecular Carcinogenesis, Department of Biology, University of York, York YO10 5DD, UK. Keith Syson Chan, Baylor College of Medicine, Houston, TX. Colin P.N. Dinney, Department of Urology, U.T. M.D. Anderson Cancer Center, Houston, TX 77030. Lars Dyrskjøt, Department of Clinical Medicine, Aarhus University, 8200 Aarhus N, Denmark. Ewan A Gibb, GenomeDx Biosciences, Vancouver, Canada. Carolyn D. Hurst, Section of Molecular Oncology, Leeds Institute of Cancer & Pathology, St James’s University Hospital, Beckett Street, University of Leeds, Leeds LS9 7TF, UK. Molly A. Ingersoll, Unit of Dendritic Cell Immunobiology, Department of Immunology, Institut Pasteur, 75015 Paris, France, and Inserm U1223, 75015 Paris, France. Gopa Iyer, Department of Medical Oncology, Memorial Sloan-Kettering Cancer Center, New York, NY 10065. Jaegil Kim, Broad Institute of Harvard and MIT, Technology Square, Cambridge, MA 02139. Margaret A. Knowles, Section of Molecular Oncology, Leeds Institute of Cancer & Pathology, St James’s University Hospital, Beckett Street, University of Leeds, Leeds LS9 7TF, UK. David J. Kwiatkowski, Brigham and Women’s Hospital, Boston, MA 02115. Seth P. Lerner, Scott Department of Urology, Baylor College of Medicine, Houston, TX. David J. McConkey, Johns Hopkins Greenberg Bladder Cancer Institute and Brady Urological Institute, Department of Urology, Johns Hopkins University, Baltimore, MD 21287. Joshua J. Meeks, Northwestern University, Feinberg School of Medicine, Department of Urology and Robert H. Lurie Comprehensive Cancer Center, Chicago, IL. Cathy Mendelsohn, Departments of Urology, Genetics & Development, and Pathology & Cell Biology, Columbia University College of Physicians and Surgeons, New York, NY 10032. Conan James Oliver O’Brien, Unit of Dendritic Cell Immunobiology, Department of Immunology, Institut Pasteur, 75015 Paris, France, and Inserm U1223, 75015 Paris, France. Peter O’Donnell, Department of Medicine, University of Chicago Medicine, Chicago, IL 60637. Nagireddy Putluri, Department of Molecular and Cellular Biology, Baylor College of Medicine, Houston, TX. François Radvanyi, Department of Molecular Oncology, Centre de Recherche, Institut Curie, 75248 Paris Cedex 05, France. A. Gordon Robertson, BC Cancer Agency, Vancouver, Canada. Jonathan Rosenberg, Department of Medical Oncology, Memorial Sloan-Kettering Cancer Center, New York, NY 10065. Matthieu Rousseau, Unit of Dendritic Cell Immunobiology, Department of Immunology, Institut Pasteur, 75015 Paris, France, and Inserm U1223, 75015 Paris, France. Marta Sánchez-Carbayo, Cancer Cell Biology Program, Centro Nacional de Investigaciones Oncológicas, Madrid, Spain. Arlene Siefker-Radtke, Department of Genitourinary Medical Oncology, U.T. M.D. Anderson Cancer Center, Houston, TX 77030. Gottfrid Sjödahl, Division of Urological Research, Department of Translational Medicine, Lund University, Skåne University Hospital, Malmö, Sweden. Jennifer Southgate, Jack Birch Unit of Molecular Carcinogenesis, Department of Biology, University of York, York YO10 5DD, UK. Jens Stahlschmidt, Jack Birch Unit of Molecular Carcinogenesis, Department of Biology, University of York, York YO10 5DD, UK. Dan Theodorescu, University of Colorado Comprehensive Cancer Center, Aurora, CO. Ludwik K Trejdosiewicz, Jack Birch Unit of Molecular Carcinogenesis, Department of Biology, University of York, York YO10 5DD, UK. Venkatrao Vantaku, Department of Molecular and Cellular Biology, Baylor College of Medicine, Houston, TX. Tahlita C.M. Zuiverloon, Department of Urology, Erasmus MC Rotterdam, The Netherlands, and University of Colorado Comprehensive Cancer Center, Aurora, CO.
Author information
Authors and Affiliations
Contributions
Protocol/project development: David McConkey and Seth Lerner. Data collection or management: David McConkey and Seth Lerner. Data analysis: David McConkey and Seth Lerner. Manuscript writing/editing: David McConkey and Seth Lerner.
Corresponding author
Ethics declarations
Conflict of interest
David McConkey (grant support)—Ranier Therapeutics Scientific Advisory Boards—Janssen, Ranier Therapeutics—Astra-Zeneca (grant support). Seth Lerner—Endo, FKD, Viventia, UroGen (grant support), QED Therapeutics, Nucleix, Urogen, MIR Scientific (advisory boards), Vaxiion (consulting).
Rights and permissions
About this article
Cite this article
McConkey, D.J., Lerner, S.P. SIU–ICUD consultation on bladder cancer: basic science. World J Urol 37, 15–29 (2019). https://doi.org/10.1007/s00345-018-2594-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2594-y