Abstract
Purpose
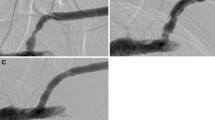
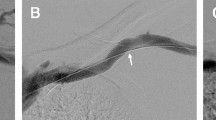
Cephalic arch stenosis (CAS) is an important and common cause of dysfunction in autogenous haemodialysis fistulas that requires multiple reinterventions and aggressive surveillance. We evaluated the safety and efficacy of the Viabahn stent-graft for the management of CAS.
Methods
Between April 2005 and October 2011, 11 consecutive patients [four men and seven women (mean age 56.7 years)] with CAS and dysfunctional fistulas were treated with insertion of 11 Viabahn stent-grafts. Six stent-grafts were inserted due to residual stenosis after angioplasty and five for fistuloplasty-induced rupture. No patient was lost to follow-up.
Results
The technical and clinical success rate was 100 %. Primary access patency rates were 81.8 % [95 % confidence interval (CI) 0.482–0.977] at 6 months and 72.7 % (95 % CI 0.390–0.939) at 12 months. Secondary access patency rates were 90.9 % at 6 months (95 % CI 0.587–0.997). There were no procedure-related complications. Mean follow-up was 543.8 days (range 156–2,282).
Conclusion
The use of the Viabahn stent-graft in the management of CAS is technically feasible and, in this small series, showed patency rates that compare favorably with historical data of angioplasty and bare stents.


Similar content being viewed by others
References
Eknoyan G, Levin NW, Eschbach JW et al (2001) Continuous quality improvement: DOQI becomes K/DOQI and is updated. National Kidney Foundation Dialysis Outcomes Initiative. Am J Kidney Dis 37:179–194
NKF-DOQI (1997) Clinical practice guidelines for vascular access. National Kidney Foundation-Dialysis Outcomes Quality Initiative. Am J Kidney Dis 30(4 Suppl 3):S150–S191
Kian K, Asif A (2008) Cephalic arch stenosis. Semin Dial 21(1):78–82
Hammes M, Funaki B, Coe FL (2008) Cephalic arch stenosis in patients with fistula access for hemodialysis: Relationship to diabetes and thrombosis. Hemodial Int 12(1):85–89
Rajan DK, Clark TW, Patel NK, Stavropoulos SW, Simons ME (2003) Prevalence and treatment of cephalic arch stenosis in dysfunctional autogenous hemodialysis fistulas. J Vasc Interv Radiol 14(5):567–573
Jaberi A, Schwartz D, Marticorena R, Dacouris N, Prabhudesai V, McFarlane P et al (2007) Risk factors for the development of cephalic arch stenosis. J Vasc Access 8(4):287–295
Bent CL, Rajan DK, Tan K, Simons ME, Jaskolka J, Kachura J et al (2010) Effectiveness of stent-graft placement for salvage of dysfunctional arteriovenous hemodialysis fistulas. J Vasc Interv Radiol 21(4):496–502
Vogel PM, Parise C (2004) SMART stent for salvage of hemodialysis access grafts. J Vasc Interv Radiol 15:1051–1060
Vogel PM, Parise C (2005) Comparison of SMART stent placement for arteriovenous graft salvage versus successful graft PTA. J Vasc Interv Radiol 16:1619–1626
Gray RJ, Sacks D, Martin LG, Trerotola SO, Society of Interventional Radiology Technology Assessment Committee (2003) Reporting standards for percutaneous interventions in dialysis access. J Vasc Interv Radiol 14:S433–S442
Fluck R, Kumwenda M (2011) Renal Association Clinical Practice Guideline on vascular access for haemodialysis. Nephron Clin Pract 118(Suppl 1):c225–c240
Tordoir J, Canaud B, Haage P et al (2007) European best practice guidelines (EBPG) on vascular access. Nephrol Dial Transpl 22(Suppl 2):ii88–ii117
Kim DS, Kim SW, Kim JC, Cho JH, Kong JH, Park CR (2011) Clinical analysis of hemodialysis vascular access: comparision of autogenous arterioveonus fistula and arteriovenous prosthetic graft. Korean J Thorac Cardiovasc Surg 44(1):25–31
Wali MA, Eid RA, Dewan M, Al-Homrany MA (2003) Intimal changes in the cephalic vein of renal failure patients before arterio-venous fistula (AVF) construction. J Smooth Muscle Res 4:95–105
Tricht IV, Wachter DD, Tordoir J, Verdonck P (2005) Hemodynamics and complications encountered with arteriovenous fistulas and grafts as vascular access for hemodialysis: a review. Ann Biomech Eng 33:1142–1157
Roy-Chaudhury P, Sukhatme VP, Cheung AK (2006) Hemodialysis vascular access dysfunction: a cellular and molecular viewpoint. J Am Soc Nephrol 17:1112–1127
Vascular Access Work Group (2006) Clinical practice guidelines for vascular access. Am J Kidney Dis 48(Suppl 1):S248–S273
Rajan DK, Bunston S, Misra S, Pinto R, Lok CE (2004) Dysfunctional autogenous hemodialysis fistulas: Outcomes after angioplasty—are there clinical predictors of patency? Radiology 232(2):508–515
Manninen HI, Kaukanen ET, Ikaheimo R et al (2001) Brachial arterial access: endovascular treatment of failing Brescia-Cimino hemodialysis fistulas—initial success and long-term results. Radiology 218:711–718
Clark TW, Hirsch DA, Jindal KJ, Veugelers PJ, LeBlanc J (2002) Outcome and prognostic factors of restenosis after percutaneous treatment of native hemodialysis fistulas. J Vasc Interv Radiol 13:51–59
Kariya S, Tanigawa N, Kojima H, Komemushi A, Shomura Y, Shiraishi T et al (2007) Primary patency with cutting and conventional balloon angioplasty for different types of hemodialysis access stenosis. Radiology 243(2):578–587
Heerwagen ST, Lönn L, Schroeder TV, Hansen MA (2010) Cephalic arch stenosis in autogenous brachiocephalic hemodialysis fistulas: results of cutting balloon angioplasty. J Vasc Access 11(1):41–45
Wu CC, Lin MC, Pu SY, Tsai KC, Wen SC (2008) Comparison of cutting balloon versus high-pressure balloon angioplasty for resistant venous stenoses of native hemodialysis fistulas. J Vasc Interv Radiol 19(6):877–883
Gray RJ, Varma JD, Cho SS, Brown LC (2008) Pilot study of cryoplasty with use of PolarCath peripheral balloon catheter system for dialysis access. J Vasc Interv Radiol 19(10):1406–1460
Chen JC, Kamal DM, Jastrzebski J, Taylor DC (2005) Venovenostomy for outflow venous obstruction in patients with upper extremity autogenous hemodialysis arteriovenous access. Ann Vasc Surg 19:629–635
Spergel LM, Ravani P, Roy-Chaudhury P, Asif A, Besarab A (2007) Surgical salvage of the autogenous arteriovenous fistula (AVF). J Nephrol 20(4):388–398
Chang CJ, Ko PJ, Hsu LA, Ko YS, Ko YL, Chen CF et al (2004) Highly increased cell proliferation activity in the restenotic hemodialysis vascular access after percutaneous transluminal angioplasty: implication in prevention of restenosis. Am J Kidney Dis 43:74–84
Hoffer EK, Sultan S, Herskowitz MM, Daniels ID, Sclafani SJ (1997) Prospective randomized trials of metallic intravascular stent in hemodialysis graft maintenance. J Vasc Interv Radiol 8:965–973
Patel RI, Peck SH, Cooper SG et al (1998) Patency of Wallstents placed across the venous anastomosis of hemodialysis grafts after percutaneous recanalization. Radiology 209:365–370
Kornfield ZN, Kwak A, Soulen MC, Patel AA, Kobrin SM, Cohen RM et al (2009) Incidence and management of percutaneous transluminal angioplasty-induced venous rupture in the “fistula first” era. J Vasc Interv Radiol 20(6):744–751
Haskal ZJ, Trerotola S, Dolmatch B, Schuman E, Altman S, Mietling S et al (2010) Stent graft versus balloon angioplasty for failing dialysis-access grafts. N Engl J Med 362(6):494–503
Chan MG, Miller FJ, Valji K, Kuo MD (2011) Evaluation of expanded polytetrafluoroethylene-covered stents for the treatment of venous outflow stenosis in hemodialysis access grafts. J Vasc Interv Radiol 22(5):647–653
Shemesh D, Goldin I, Zaghal I, Berlowitz D, Raveh D, Olsha O (2008) Angioplasty with stent graft versus bare stent for recurrent cephalic arch stenosis in autogenous arteriovenous access for hemodialysis: a prospective randomized clinical trial. J Vasc Surg 48(6):1524–1531
Acknowledgments
Nicos I. Fotiadis has received honoraria for lectures from W. L. Gore.
Conflict of interest
Dr Andrew Shawyer, Dr Girish Namagondlu, Dr Arun Ayer, Dr Mark Blunden, Dr Martin Raftery and Dr Magdi Yaqoob have no conflict of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shawyer, A., Fotiadis, N.I., Namagondlu, G. et al. Cephalic Arch Stenosis in Autogenous Haemodialysis Fistulas: Treatment With the Viabahn Stent-Graft. Cardiovasc Intervent Radiol 36, 133–139 (2013). https://doi.org/10.1007/s00270-012-0433-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-012-0433-x