Abstract
Background
Saskatchewan Aboriginal people are experiencing epidemics of both type 2 diabetes (T2DM) and tuberculosis (TB). The purpose of this study was to determine if a relationship exists between diabetes and TB in Saskatchewan and to establish whether there is a difference in the degree of any association between Aboriginal and non- Aboriginal people.
Methods
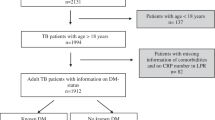
Utilizing Saskatchewan Health databases, TB incidence (cases identified from 1986–2001) was compared between four subpopulations identified from 1991–1995: Registered Indians (RI) with and without diabetes, and other Saskatchewan people (OSKP) with and without diabetes.
Results
Diabetic women aged 20–59 years had higher average annual incidence rates of TB than non-diabetic women, but within-population rate ratios of TB in diabetic versus non-diabetic women were only significant in those aged 50–59 (2.7 [CI 1.28, 5.72] in RI and 3.9 [CI 1.58, 9.67] in OSKP). No other within-population diabetic subgroup had significantly higher rates of TB. The only male diabetic group that had a higher rate of TB were RI plus OSKP men aged 50–59 years. Overall, diabetes preceded TB in 87/111 individuals with both diseases (p<0.0001).
Conclusions
Our results suggest that T2DM is a predictor for TB in Saskatchewan women aged 20–59 but particularly in RI and OSKP women aged 50–59 years. This has implications for TB screening and prevention initiatives.
Résumé
Contexte
Les Autochtones de la Saskatchewan sont aux prises avec des épidémies de diabète de type II et de tuberculose. Dans cette étude, nous avons voulu déterminer s’il existe un lien entre le diabète et la tuberculose en Saskatchewan, et s’il y a une différence entre les Autochtones et les non-Autochtones en ce qui a trait au degré d’association éventuel entre ces maladies.
Méthode
À l’aide des bases de données du ministère de la Santé de la Saskatchewan, nous avons comparé la fréquence de la tuberculose (les cas détectés de 1986 à 2001) dans quatre souspopulations définies pour la période de 1991 à 1995: les Indiens inscrits, diabétiques et non diabétiques, et les autres habitants de la Saskatchewan (AHSK), diabétiques et non diabétiques.
Résultats
Chez les femmes diabétiques de 20 à 59 ans, le taux d’incidence annuel moyen de la tuberculose était plus élevé que chez les femmes non diabétiques, mais les ratios des taux de tuberculose entre les femmes diabétiques et non diabétiques dans chaque population n’étaient significatifs que pour les femmes de 50 à 59 ans (IC de 2,7 [1,28 à 5,72] chez les Indiennes inscrites et de 3,9 [1,58 à 9,67] chez les AHSK). Aucun autre sous-groupe de diabétiques à l’intérieur d’une population n’avait de taux sensiblement plus élevés de tuberculose. Le seul groupe d’hommes diabétiques dont le taux de tuberculose était plus élevé se composait d’Indiens inscrits et d’AHSK âgés de 50 à 59 ans. Globalement, le diabète avait précédé la tuberculose chez 87 des 111 sujets ayant les deux maladies (p<0,0001).
Conclusions
Nos résultats donnent à penser que le diabète de type II est un prédicteur de la tuberculose chez les femmes de la Saskatchewan de 20 à 59 ans, mais plus particulièrement chez les Indiennes inscrites et les autres habitantes de la Saskatchewan âgées de 50 à 59 ans. Ceci aurait des conséquences pour le dépistage et les mesures de prévention de la tuberculose.
Similar content being viewed by others
References
Young TK, Reading J, Elias B, O’Neil, JD. Type diabetes mellitus in Canada’s First Nations: Status of an epidemic in progress. CMAJ 2000;163(5):561–66.
Hoeppner VH, Marciniuk, DD. Tuberculosis in Aboriginal Canadians. Can Respir J 2000;7:141–46.
Chase, LA. The trend of diabetes in Saskatchewan, 1905 to 1934. CMAJ 1937;36:366–69.
Pioro MP, Dyck RF, Gillis, DC. Diabetes prevalence rates among First Nations adults on Saskatchewan reserves in 1990: Comparison by tribal grouping, geography and with non-First Nations people. Can J Public Health 1996;87(5):325–28.
Klomp H, Chan BTB, Cascagnette P, Teare G, Sidhu N. Quality of Diabetes Management in Saskatchewan: Supplementary Tables and Figures. Saskatoon: Health Quality Council, January 2006. ISBN 1-897155-27-1.
Saskatchewan Health. Tuberculosis Control Program Annual Reports. 1996–2004.
Nichols, GP. Diabetes among young tuberculosis patients. Am Rev Tuberc Pulm Dis 1957;76:1016–30.
Root HF, Bloor, WR. Diabetes and pulmonary tuberculosis. Am Rev Tuberc 1939;39:714–37.
Banyai, AL. Diabetes and pulmonary tuberculosis. Am Rev Tuberc 1931;24:650–67.
Boucot KR, Cooper DA, Dillon ES, Meier P, Richardson R. Tuberculosis among diabetics. Am Rev Tuberc 1952;65(Suppl):1–50.
Mori MA, Leonartson G, Welty, TK. The benefits of isoniazid chemoprophylaxis and risk factors for tuberculosis among Oglala Sioux Indians. Arch Intern Med 1992;152:547–50.
Kim SJ, Hong YP, Lew WJ, Yang SC, Lee, EG. Incidence of pulmonary tuberculosis among diabetics. Tubercle Lung Dis 1995;76:529–33.
Pablos-Mendez A, Blustein J, Knirsch, CA. The role of diabetes mellitus in the higher prevalence of tuberculosis among Hispanics. Am J Public Health 1997;87:574–79.
Oluboyo PO, Erasmus, RT. The significance of glucose intolerance in pulmonary tuberculosis. Tubercle 1990;71(2):135–38.
Jawad F, Shera AS, Memon R, Ansari G. Glucose intolerance in pulmonary tuberculosis. J Pak Med Assoc 1995;45(9):237–38.
McMahon MM, Bistrian, BR. Host defences and susceptibility to infection in patients with diabetes mellitus. Infect Dis Clin North Am 1995;9(1):1–9.
Chang FY, Shaio, MF. Decreased cell-mediated immunity in patients with non-insulindependent diabetes mellitus. Diabetes Res Clin Pract 1995;28(2):137–46.
Alexiewicz JM, Kumar D, Smogorzewski M, Massry, SG. Elevated cytosolic calcium and impaired proliferation of B-Lymphocytes in Type II Diabetes Mellitus. Am J Kidney Dis 1997;30(1):98–104.
Ming Li Y, Tan AX, Vlassara H. Antibacterial activity of lysozyme and lactoferrin is inhibited by binding of advanced glycation-modified proteins to a conserved motif. Nature Med 1995;1(10):1057–61.
Downey W, Beck P, McNutt M, Stang MR, Osei W, Nichol J. Health databases in Saskatchewan. In: Strom BL (Ed.), Pharmacoepidemiology, 3rd Ed. Chichester: John Wiley and Sons, 2000;325–45.
Boctor MA, Young ER (Co-Chairs). Diabetes 2000 — Report of the Saskatchewan Advisory Committee on Diabetes. March 15, 2000.
Lin S, Shen M, Sun Y. Epidemiological characteristics of tuberculosis patients complicated with diabetes in Shanghai. Zhonghua Jie He He Hu Xi Za Zhi 1998;21:504–6.
Yamagishi F. Medical risk factors of tuberculosis and countermeasures. Kekkaku 2002;77:799–804.
Kobashi Y, Miyashita N, Niki Y, Okimoto N, Hara Y, Matsushima T. Clinical analysis of pulmonary tuberculosis detected during follow-up of other underlying diseases Kekkaku 2004;79:1–6.
Perez-Guzman C, Vargas MH, Torres-Cruz A, Perez-Padilla JR, Furuya ME, Villarreal-Velarde H. Diabetes modifies the male:female ratio in pulmonary tuberculosis. Int J Tuberc Lung Dis 2003;7(4):354–58.
Asch SM, Kerr EA, Keesey J, Adams JL, Setodji CM, Malik S, McGlynn EA. Who is at greatest risk for receiving poor quality health care? N Engl J Med 2006;354:1147–56.
Salem ML. Estrogen, a double-edged sword: Modulation of TH1 and TH2 mediated inflammations by differential regulation of TH1/TH2 cytokine population. Curr Drug Targets Inflamm Allergy 2004;3:97–104.
Barnes PF, Wizel B. Type 1 cytokines and the pathogenesis of tuberculosis. Am J Respir Crit Care Med 2000;161:1773–74.
Mohan VP, Scanga CA, Yu K, Scott HM, Tanaka KE, Tsang E. Effects of tumor necrosis factor alpha on host immune response in chronic persistent tuberculosis: Possible role for limiting pathology. Infect Immun 2001;69:1847–55.
Grange JM, Stanford JL, Rook GA. Tuberculosis and cancer: Parallels in host responses and therapeutic approaches? Lancet 1995;345:1350–52.
Wang CH, Yu CT, Lin HC, Liu CY, Kuo HP. Hypodense alveolar macrophages in patients with diabetes mellitus and active pulmonary tuberculosis. Tuberc Lung Dis 1999;79(4):235–42.
American Thoracic Society/Centers for Disease Control and Prevention. Targeted tuberculin testing and treatment of latent tuberculosis infection. Am J Respir Crit Care Med 2000;S221–S243.
Breault JL, Hoffman MG. A strategy for reducing tuberculosis among Oglala Sioux Native Americans. Am J Prev Med 1997;13:182–88.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclaimer: This study is based in part on non-identifiable data provided by the Saskatchewan Department of Health. The interpretations and conclusions contained herein do not necessarily represent those of the Government of Saskatchewan or the Saskatchewan Department of Health.
Funding: Supported by a grant from the Saskatchewan Health Research Foundation.
Rights and permissions
About this article
Cite this article
Dyck, R.F., Klomp, H., Marciniuk, D.D. et al. The Relationship Between Diabetes and Tuberculosis in Saskatchewan. Can J Public Health 98, 55–59 (2007). https://doi.org/10.1007/BF03405386
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03405386