Abstract
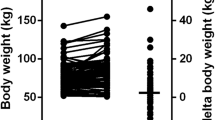
Acromegaly is a severe slow-developing disease associated with a poor prognosis for cardiovascular disease. To evaluate the impact of age and gender on the severity of the disease, 151 de novo patients with acromegaly (79 women, 72 men, age range 19–77 yr) were included in this open retrospective multi-center cohort study. Basal GH and IGF-I levels, GH response after glucose load and maximal tumor diameter at MRI were measured in all patients at diagnosis. Fasting GH levels and maximal tumor diameter were similar in women and men, while serum IGF-I levels were lower (664.9±24.9 vs 755.9±32 μg/l; p=0.02) and GH nadir after glucose load was higher (27.5±3.7 vs 18.5±2.2 μg/l; p=0.04) in women than in men. In both sexes, patients’ age was negatively correlated with basal and nadir GH, IGF-I levels and tumor size; fasting GH levels were positively correlated with IGF-I levels and nadir GH after glucose. No interaction between age and gender was found on biochemical and morphological parameters. At diagnosis, elderly patients with acromegaly have lower GH and IGF-I levels, lower GH nadir after glucose load and smaller adenomas than young patients. Women have lower IGF-I levels but higher GH nadir after glucose load than men. These age and gender differences should be considered to appropriately evaluate the activity of acromegaly throughout a life-span.
Similar content being viewed by others
References
Colao A., Lombardi G. Growth-hormone and prolactin excess. Lancet 1998, 352: 1455–1461.
Ezzat S. Acromegaly. Endocrinol. Metab. Clin. North Am. 1997, 26: 703–723.
Melmed S., Ho K., Klibanski A., Reichlin S., Thorner M.O. Recent advances in pathogenesis, diagnosis and management of acromegaly. J. Clin. Endocrinol. Metab. 1995, 80: 3395–3402.
Losa M. Pituitary tumors in the elderly. Eur. J. Endocrinol. 1999, 140: 378–380.
Lamberts S.W.J., van der Lely A.J., de Herder W.W. Clinical and medical diagnosis of acromegaly. Metabolism 1995, 44: 15–19.
Bates A.S., Van’t Hoff W., Jones J.M., Clayton R.N. An audit of outcome of treatment in acromegaly. Q. J. Med. 1993, 86: 293–299.
Bengtsson B.A., Edén S., Ernest I., Oden A., Sjögren B. Epidemiology and long term survival in acromegaly. Acta Med. Scand. 1988, 223: 327–335.
Orme S.M., McNally R.J.Q., Cartwright R.A., Belchetz P.E. Mortality and cancer incidence in acromegaly: a retrospective cohort study. J. Clin. Endocrinol. Metab. 1998, 83: 2730–2734.
Rajasoorya C, Holdaway I.M., Wrightson P., Scott D.J., Ibbertson H.K. Determinants of clinical outcome and survival in acromegaly. Clin. Endocrinol. (Oxf.) 1994, 41: 95–102.
Wright A.D., Hill D.M., Lowy C, Russell Fraser T. Mortality in acromegaly. Q.J.M. 1970, 153: 1–16.
Ghigo E., Aimaretti G., Gianotti L., Bellone J., Arvat E., Camanni F. New approach to the diagnosis of growth hormone deficiency in adults. Eur. J. Endocrinol. 1996, 134: 352–356.
Zadik Z., Chalew S.A., McCarter R.J. Jr., Meistas M., Kowarski A.A. The influence of age on the 24 hour integrated concentration of growth hormone in normal individuals. J. Clin. Endocrinol. Metab. 1985, 60: 513–516.
Giustina A., Barkan A., Casanueva F.F., et al. Criteria for cure of acromegaly: a consensus statement. J. Clin. Endocrinol. Metab. 2000, 85: 526–529.
Mancini A., Zuppi P., Fiumara C, et al. GH response to oral and intravenous glucose load in acromegalic patients. Horm. Metab. Res. 1995, 27: 322–325.
Melmed S., Jackson I., Kleinberg D., Klibanski A. Current treatment guidelines for acromegaly. J. Clin. Endocrinol. Metab. 1998, 83: 2646–2652.
Turner H.E., Adams C.B.T., Wass J.A.H. Pituitary tumours in the elderly: a 20 year experience. Eur. J. Endocrinol. 1999, 140: 383–389.
van der Lely A.J., Harris A.G., Lamberts S.W. The sensitivity of growth hormone secretion to medical treatment in acromegalic patients: influence of age and sex. Clin. Endocrinol. (Oxf.) 1992, 37: 181–185.
Frantz A.G., Rabkin M.T. Effects of estrogen and sex difference on secretion of human growth hormone. J. Clin. Endocrinol. Metab. 1965, 25: 1470–1480.
Ho K.Y., Evans W.S., Blizzard R.M., et al. Effects of sex and age on the 24-hour profile of growth hormone secretion in man: importance of endogenous estradiol concentrations. J. Clin. Endocrinol. Metab. 1987, 64: 51–58.
Thompson R.G., Rodriguez A., Kowarski, A., Blizzard R.M. Growth hormone: metabolic clearance rates, integrated concentrations, and production rates in normal adults and the effects of prednisone. J. Clin. Invest. 1972, 51: 3193–3199.
Burman P., Johansson A., Siegbahn A., Vesby B., Karlsson F.A. Growth hormone (GH)-deficient men are more responsive to GH replacement therapy than women. J. Clin. Endocrinol. Metab. 1997, 82: 550–555.
Johansson A.G. Gender difference in growth hormone response in adults. J. Endocrinol. Invest. 1999, 22: 58–60.
Johansson A.G., Engstrom B.E., Ljunghall S., Karlsson F.A., Burman P. Gender differences in the effects of long term growth hormone (GH) treatment on bone in adults with GH deficiency. J. Clin. Endocrinol. Metab. 1999, 84: 2002–2007.
Kaltsas G.A., Mukherjee J.J., Jenkins P.J., et al. Menstrual irregularity in women with acromegaly. J. Clin. Endocrinol. Metab. 1999, 84: 2731–2735.
Colao A., Ferone D., Lastoria S., et al. Prediction of efficacy of octreotide therapy in patients with acromegaly. J. Clin. Endocrinol. Metab. 1996, 81: 2356–2362.
Colao A., Merola B., Ferone D., Lombardi G. Acromegaly. J. Clin. Endocrinol. Metab. 1997, 82: 2777–2781.
Smals A.E.M., Pieters G.F.F.M., Smals A.G.H., Kloppen-borg P.W.C. Sex difference in the relation between sellar volume and basal and GH-releasing hormone stimulated GH in acromegaly. Acta Endocrinol. 1988, 117: 387–391.
Winer L.M., Shaw M.A., Baumann G. Basal plasma growth hormone levels in man: new evidence for rhythmicity of growth hormone secretion. J. Clin. Endocrinol. Metab. 1990, 70: 1678–1686.
van den Berg G., Veldhuis J.D., Frolich M., Roelfsema F. An amplitude-specific divergence in the pulsatile mode of growth hormone (GH) secretion underlies the gender difference in mean GH concentrations in men and pre-menopausal women. J. Clin. Endocrinol. Metab. 1996, 81: 2460–2467.
Gatford K.L., Egan A.R., Clarke I.J., Owens P.C. Sexual dimorphism of the somatotrophic axis. J. Endocrinol. 1998, 157: 373–389.
Jaffe C.A., Ocampo-Lim B., Guo W., et al. Regulatory mechanisms of growth hormone secretion are sexually dimorphic. J. Clin. Invest. 1998, 102: 153–164.
Chapman I.M., Hartmann M.L., Straume M., et al. Enhanced sensitivity growth hormone (GH) chemilumi-nescence assay reveals lower postglucose nadir GH concentrations in men than women. J. Clin. Endocrinol. Metab. 1994, 78: 1312–1319.
Ferone D., Colao A., van der Lely A.J., Lamberts S.W.J. Pharmacotherapy or surgery as primary treatment for acromegaly? Drugs 2000, 17: 81–92.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Colao, A., Amato, G., Pedroncelli, A.M. et al. Gender- and age-related differences in the endocrine parameters of acromegaly. J Endocrinol Invest 25, 532–538 (2002). https://doi.org/10.1007/BF03345496
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03345496