Abstract
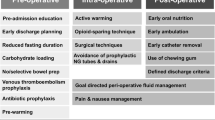
Enhanced Recovery After Surgery (ERAS) is a global surgical quality improvement initiative started by a group of European surgeons who challenged the evidence surrounding several historical perioperative practices including prolonged fasting (NPO after midnight), and mechanical bowel preparation. With the goal to minimize the stress response to surgery and bring evidence-based practice mainstream, the ERAS® Society was formed, and has now published numerous perioperative practice guidelines including those for pancreatic and liver surgery. This chapter will provide an overview of (i) the philosophy of ERAS, (ii) the pathophysiology and basis of several core ERAS practices, with special attention to those relevant to Hepato-Pancreato-Biliary (HPB) disease, (iii) clinical and financial outcomes associated with ERAS, and (iv) important considerations when starting an ERAS implementation program.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Ljungqvist O, Scott M, Fearon KC. Enhanced recovery after surgery: a review. JAMA Surg. 2017;152(3):292–8.
https://erassociety.org/. Accessed 25 Aug 2020.
Fearon KC, Ljungqvist O, Von Meyenfeldt M, et al. Enhanced recovery after surgery: a consensus review of clinical care for patients undergoing colonic resection. Clin Nutr. 2005;24(3):466–77.
Gustafsson UO, Scott MJ, Hubner M, et al. Guidelines for perioperative care in elective colorectal surgery: enhanced recovery after surgery (ERAS) society recommendations: 2018. World J Surg. 2019;43(3):659–95.
Thorell A, MacCormick AD, Awad S, et al. Guidelines for perioperative care in bariatric surgery: enhanced recovery after surgery (ERAS) society recommendations. World J Surg. 2016;40(9):2065–83.
Melloul E, Lassen K, Roulin D, et al. Guidelines for perioperative care for pancreatoduodenectomy: enhanced recovery after surgery (ERAS) recommendations 2019. World J Surg. 2020;44(7):2056–84.
Melloul E, Hübner M, Scott M, et al. Guidelines for perioperative care for liver surgery: enhanced recovery after surgery (ERAS) society recommendations. World J Surg. 2016;40(10):2425–40.
Sorensen LT. Wound healing and infection in surgery. The clinical impact of smoking and smoking cessation: a systematic review and meta-analysis. Arch Surg. 2012;147(4):373–83. https://doi.org/10.1001/archsurg.2012.5.
Eisenberg JD, Rosato EL, Lavu H, et al. Delayed gastric emptying after pancreaticoduodenectomy: an analysis of risk factors and cost. J Gastrointest Surg. 2015;19(9):1572–80.
Aoki S, Miyata H, Konno H, et al. Risk factors of serious postoperative complications after pancreaticoduodenectomy and risk calculators for predicting postoperative complications: a nationwide study of 17,564 patients in Japan. J Hepatobiliary Pancreat Sci. 2017;24(5):243–51.
Oppedal K, Moller AM, Pedersen B, et al. Preoperative alcohol cessation prior to elective surgery. Cochrane Database Syst Rev. 2012;7:CD008343.
Gianotti L, Besselink MG, Sandini M, et al. Nutritional support and therapy in pancreatic surgery: a position paper of the International Study Group on Pancreatic Surgery (ISGPS). Surgery. 2018;164(5):1035–48.
Brady M, Kinn S, Stuart P. Preoperative fasting for adults to prevent perioperative complications. Cochrane Database Syst Rev. 2003;2003(4):CD004423.
American Society of Anesthesiologists Committee. Practice guidelines for preoperative fasting and the use of pharmacologic agents to reduce the risk of pulmonary aspiration: application to healthy patients undergoing elective procedures: an updated report by the American Society of Anesthesiologists Committee on Standards and Practice Parameters. Anesthesiology. 2011;114(3):495–511.
Smith I, Kranke P, Murat I, et al. Perioperative fasting in adults and children: guidelines from the European Society of Anaesthesiology. Eur J Anaesthesiol. 2011;28(8):556–69.
Nygren J, Thorell A, Ljungqvist O. Preoperative oral carbohydrate therapy. Curr Opin Anaesthesiol. 2015;28:364–9.
Smith MD, McCall J, Plank L, et al. Preoperative carbohydrate treatment for enhancing recovery after elective surgery. Cochrane Database Syst Rev. 2014;2014(8):CD009161.
Rollins KE, Lobo DN. The controversies of mechanical bowel and oral antibiotic preparation in elective colorectal surgery. Ann Surg. 2021;273(1):e13–5.
Lavu H, Kennedy EP, Mazo R, et al. Preoperative mechanical bowel preparation does not offer a benefit for patients who undergo pancreaticoduodenectomy. Surgery. 2010;148:278–84.
Nelson R, Tse B, Edwards S. Systematic review of prophylactic nasogastric decompression after abdominal operations. Br J Surg. 2005;92:673–80.
Kunstman JW, Klemen ND, Fonseca AL, et al. Nasogastric drainage may be unnecessary after pancreaticoduodenectomy: a comparison of routine vs selective decompression. J Am Coll Surg. 2013;217(3):481–8.
Pessaux P, Regimbeau JM, Dondero F, et al. Randomized clinical trial evaluating the need for routine nasogastric decompression after elective hepatic resection. Br J Surg. 2007;94:297–303.
Gerritsen A, Besselink MG, Gouma DJ, et al. Systematic review of five feeding routes after pancreatoduodenectomy. Br J Surg. 2013;100(5):589–98.
ERAS Compliance Group. The impact of enhanced recovery protocol compliance on elective colorectal cancer resection: results from an international registry. Ann Surg. 2015;261(6):1153–9.
Pisarska M, Torbicz G, Gajewska N, et al. Compliance with the ERAS protocol and 3-year survival after laparoscopic surgery for nonmetastatic colorectal cancer. World J Surg. 2019;43:2552–60.
Savaridas T, Serrano-Pedraza I, Khan SK, et al. Reduced medium-term mortality following primary total hip and knee arthroplasty with an enhanced recovery program. A study of 4,500 consecutive procedures. Acta Orthop. 2013;84:40–3.
Roulin D, Melloul E, Wellg BE, et al. Feasibility of an enhanced recovery protocol for elective pancreatoduodenectomy: a multicenter international cohort study. World J Surg. 2020;44(8):2761–9.
Noba L, Rodgers S, Chandler C, et al. Enhanced recovery after surgery (ERAS) reduces hospital costs and improve clinical outcomes in liver surgery: a systematic review and meta-analysis. J Gastrointest Surg. 2020;24(4):918–32.
Ljungqvist O, Thanh NX, Nelson G. ERAS-value based surgery. J Surg Oncol. 2017;116(5):608–12.
Thanh NX, Nelson A, Wang X, et al. Return on investment of the enhanced recovery after surgery (ERAS) multi-guideline multi-site implementation in Alberta. Canada Can J Surg. 2020;63(6):E542–50.
Joliat GR, Hübner M, Roulin D, et al. Cost analysis of enhanced recovery programs in colorectal, pancreatic, and hepatic surgery: a systematic review. World J Surg. 2020;44(3):647–55.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Nelson, G., Ljungqvist, O. (2022). Enhanced Recovery After Surgery (ERAS): Concept and Purpose. In: Makuuchi, M., et al. The IASGO Textbook of Multi-Disciplinary Management of Hepato-Pancreato-Biliary Diseases. Springer, Singapore. https://doi.org/10.1007/978-981-19-0063-1_27
Download citation
DOI: https://doi.org/10.1007/978-981-19-0063-1_27
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-19-0062-4
Online ISBN: 978-981-19-0063-1
eBook Packages: MedicineMedicine (R0)