Abstract
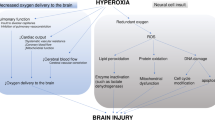
Sudden cardiac arrest is the most common lethal manifestation of cardiovascular disease. Even when successfully resuscitated and admitted to the intensive care unit (ICU), the majority of patients do not survive [1]. This disappointingly low survival rate has resulted in a shift of focus from interventions that improve success of cardiopulmonary resuscitation (CPR) to factors that may modify outcome favorably after return of spontaneous circulation (ROSC) [2]. Whilst early restoration of blood flow to ischemic tissues is essential to halt progression of cellular damage, it is now clear that reperfusion initiates a complex series of reactions that paradoxically injure tissues. This global ischemia/reperfusion response is responsible for the post-cardiac arrest syndrome observed in survivors of cardiac arrest [3]. The brain is particularly vulnerable to ischemia/reperfusion and postcardiac arrest brain injury is the most common cause of death and disability [4]. The recent success of therapeutic hypothermia has emphasized that the course of reperfusion injury can be mitigated and as such the search for other interventions that may further attenuate injury and improve outcome has focused recently on the high concentrations of oxygen administered routinely during CPR and for prolonged periods after ROSC.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Preview
Unable to display preview. Download preview PDF.
Similar content being viewed by others
References
Nolan JP, Soar J (2010) Postresuscitation care: entering a new era. Curr Opin Crit Care 16: 216–222
Peberdy MA, Callaway CW, Neumar RW, et al (2010) Part 9: Post-cardiac arrest care: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 122: S768–786
Nolan JP, Neumar RW, Adrie C, et al (2008) Post-cardiac arrest syndrome: epidemiology, pathophysiology, treatment, and prognostication. A Scientific Statement from the International Liaison Committee on Resuscitation; the American Heart Association Emergency Cardiovascular Care Committee; the Council on Cardiovascular Surgery and Anesthesia; the Council on Cardiopulmonary, Perioperative, and Critical Care; the Council on Clinical Cardiology; the Council on Stroke. Resuscitation 79: 350–379
Laver S, Farrow C, Turner D, Nolan J (2004) Mode of death after admission to an intensive care unit following cardiac arrest. Intensive Care Med 30: 2126–2128
Lewen A, Matz P, Chan PH (2000) Free radical pathways in CNS injury. J Neurotrauma 17: 871–890
Fiskum G, Danilov CA, Mehrabian Z, et al (2008) Postischemic oxidative stress promotes mitochondrial metabolic failure in neurons and astrocytes. Ann NY Acad Sci 1147: 129–138
Nakka VP, Gusain A, Mehta SL, Raghubir R (2008) Molecular mechanisms of apoptosis in cerebral ischemia: multiple neuroprotective opportunities. Mol Neurobiol 37: 7–38
Wolbarsht ML, Fridovich I (1989) Hyperoxia during reperfusion is a factor in reperfusion injury. Free Radic Biol Med 6: 61–62
Imberti R, Bellinzona G, Riccardi F, Pagani M, Langer M (2003) Cerebral perfusion pressure and cerebral tissue oxygen tension in a patient during cardiopulmonary resuscitation. Intensive Care Med 29: 1016–1019
Gerschman R, Gilbert DL, Nye SW, Dwyer P, Fenn WO (1954) Oxygen poisoning and xirradiation: a mechanism in common. Science 119: 623–626
Davis PG, Tan A, O’Donnell CPF, Schulze A (2004) Resuscitation of newborn infants with 100 % oxygen or air: a systematic review and meta-analysis. Lancet 364: 1329–1333
Conti CR (2011) Is hyperoxic ventilation important to treat acute coronary syndromes such as myocardial infarction? Clin Cardiol 34: 132–133
Michalski D, Hartig W, Schneider D, Hobohm C (2011) Use of normobaric and hyperbaric oxygen in acute focal cerebral ischemia — a preclinical and clinical review. Acta Neurol Scand 123: 85–97
Neumar RW (2011) Optimal oxygenation during and after cardiopulmonary resuscitation. Curr Opin Crit Care 17: 236–240
Nolan JP, Soar J, Zideman DA, et al (2010) European Resuscitation Council Guidelines for Resuscitation 2010 Section 1. Executive summary. Resuscitation 81: 1219–1276
O’Driscoll BR, Howard LS, Davison AG (2008) BTS guideline for emergency oxygen use in adult patients. Thorax 63 (Suppl) 6: vi1–68
Marsala J, Marsala M, Vanicky I, Galik J, Orendacova J (1992) Post cardiac arrest hyperoxic resuscitation enhances neuronal vulnerability of the respiratory rhythm generator and some brainstem and spinal cord neuronal pools in the dog. Neurosci Lett 146: 121–124
Liu Y, Rosenthal RE, Haywood Y, Miljkovic-Lolic M, Vanderhoek JY, Fiskum G (1998) Normoxic ventilation after cardiac arrest reduces oxidation of brain lipids and improves neurological outcome. Stroke 29: 1679–1686
Richards EM, Rosenthal RE, Kristian T, Fiskum G (2006) Postischemic hyperoxia reduces hippocampal pyruvate dehydrogenase activity. Free Radic Biol Med 40: 1960–1970
Vereczki V, Martin E, Rosenthal RE, Hof PR, Hoffman GE, Fiskum G (2006) Normoxic resuscitation after cardiac arrest protects against hippocampal oxidative stress, metabolic dysfunction, and neuronal death. J Cereb Blood Flow Metab 26: 821–835
Richards EM, Fiskum G, Rosenthal RE, Hopkins I, Mckenna MC (2007) Hyperoxic reperfusion after global ischemia decreases hippocampal energy metabolism. Stroke 38: 1578–1584
Mickel HS, Vaishnav YN, Kempski O, von Lubitz D, Weiss JF, Feuerstein G (1987) Breathing 100% oxygen after global brain ischemia in Mongolian Gerbils results in increased lipid peroxidation and increased mortality. Stroke 18: 426–430
Feng ZC, Sick TJ, Rosenthal M (1998) Oxygen sensitivity of mitochondrial redox status and evoked potential recovery early during reperfusion in post-ischemic rat brain. Resuscitation 37: 33–41
Walson KH, Tang M, Glumac A, et al (2011) Normoxic versus hyperoxic resuscitation in pediatric asphyxial cardiac arrest: effects on oxidative stress. Crit Care Med 39: 335–343
Balan IS, Fiskum G, Hazelton J, Cotto-Cumba C, Rosenthal RE (2006) Oximetry-guided reoxygenation improves neurological outcome after experimental cardiac arrest. Stroke 37: 3008–3013
Brucken A, Kaab AB, Kottmann K, et al (2010) Reducing the duration of 100 % oxygen ventilation in the early reperfusion period after cardiopulmonary resuscitation decreases striatal brain damage. Resuscitation 81: 1698–1703
Hazelton JL, Balan I, Elmer GI, et al (2010) Hyperoxic reperfusion after global cerebral ischemia promotes inflammation and long-term hippocampal neuronal death. J Neurotrauma 27: 753–762
Zwemer CF, Whitesall SE, D’Alecy LG (1994) Cardiopulmonary-cerebral resuscitation with 100 % oxygen exacerbates neurological dysfunction following nine minutes of normothermic cardiac arrest in dogs. Resuscitation 27: 159–170
Douzinas EE, Patsouris E, Kypriades EM, et al (2001) Hypoxaemic reperfusion ameliorates the histopathological changes in the pig brain after a severe global cerebral ischaemic insult. Intensive Care Med 27: 905–910
Lipinski CA, Hicks SD, Callaway CW (1999) Normoxic ventilation during resuscitation and outcome from asphyxial cardiac arrest in rats. Resuscitation 42: 221–229
Douzinas EE, Andrianakis I, Pitaridis MT, et al (2001) The effect of hypoxemic reperfusion on cerebral protection after a severe global ischemic brain insult. Intensive Care Med 27: 269–275
Zwemer CF, Whitesall SE, D’Alecy LG (1995) Hypoxic cardiopulmonary-cerebral resuscitation fails to improve neurological outcome following cardiac arrest in dogs. Resuscitation 29: 225–236
Kuisma M, Boyd J, Voipio V, Alaspää A, Roine RO, Rosenberg P (2006) Comparison of 30 and the 100 % inspired oxygen concentrations during early post-resuscitation period: a randomised controlled pilot study. Resuscitation 69: 199–206
Kilgannon JH, Jones AE, Shapiro NI, et al (2010) Association Between arterial hyperoxia following resuscitation from cardiac arrest and in-hospital mortality. JAMA 303: 2165–2171
Bellomo R, Bailey M, Eastwood GM, et al (2011) Arterial hyperoxia and in-hospital mortality after resuscitation from cardiac arrest. Crit Care 15: R90
Kilgannon JH, Jones AE, Parrillo JE, et al (2011) Relationship between supranormal oxygen tension and outcome after resuscitation from cardiac arrest. Circulation 123: 2717–2722
Rosenthal RE, Silbergleit R, Hof PR, Haywood Y, Fiskum G (2003) Hyperbaric oxygen reduces neuronal death and improves neurological outcome after canine cardiac arrest. Stroke 34: 1311–1316
Eltzschig HK, Carmeliet P (2011) Hypoxia and inflammation. N Engl J Med 364: 656–665
Iscoe S, Beasley R, Fisher JA (2011) Supplementary oxygen for nonhypoxemic patients: O2 much of a good thing? Crit Care 15: 305
Farquhar H, Weatherall M, Wijesinghe M, et al (2009) Systematic review of studies of the effect of hyperoxia on coronary blood flow. Am Heart J 158: 371–377
Bourassa MG, Campeau L, Bois MA, Rico O (1969) The effects of inhalation of 100 percent oxygen on myocardial lactate metabolism in coronary heart disease. Am J Cardiol 24: 172–177
Rawles JM, Kenmure AC, (1976) Controlled trial of oxygen in uncomplicated myocardial infarction. BMJ 1: 1121–1123
Wijesinghe M, Perrin K, Ranchord A, Simmonds M, Weatherall M, Beasley R (2009) Routine use of oxygen in the treatment of myocardial infarction: systematic review. Heart 95: 198–202
Cabello JB, Burls A, Emparanza JI, Bayliss S, Quinn T (2010) Oxygen therapy for acute myocardial infarction. Cochrane Database Syst Rev 6: CD007160
Vento M, Asensi M, Sastre J, Garcia-Sala F, Pallardo FV, Vina J (2001) Resuscitation with room air instead of 100 % oxygen prevents oxidative stress in moderately asphyxiated term neonates. Pediatrics 107: 642–647
Saugstad OD, Ramji S, Soll RF, Vento M (2008) Resuscitation of newborn infants with 21 % or 100 % oxygen: an updated systematic review and meta-analysis. Neonatology 94: 176–182
Saugstad OD (2007) Optimal oxygenation at birth and in the neonatal period. Neonatology 91: 319–322
Bennett MH, Wasiak J, Schnabel A, Kranke P, French C (2005) Hyperbaric oxygen therapy for acute ischaemic stroke. Cochrane Database Syst Rev CD004954
Adams HP Jr, del Zoppo G, Alberts MJ, et al (2007) Guidelines for the early management of adults with ischemic stroke: a guideline from the American Heart Association/American Stroke Association Stroke Council, Clinical Cardiology Council, Cardiovascular Radiology and Intervention Council, and the Atherosclerotic Peripheral Vascular Disease and Quality of Care Outcomes in Research Interdisciplinary Working Groups: The American Academy of Neurology affirms the value of this guideline as an educational tool for neurologists. Circulation 115: e478–534
Singhal AB, Benner T, Roccatagliata L, et al (2005) A pilot study of normobaric oxygen therapy in acute ischemic stroke. Stroke 36: 797–802
Singhal AB, Ratai E, Benner T, et al (2007) Magnetic resonance spectroscopy study of oxygen therapy in ischemic stroke. Stroke 38: 2851–2854
Chiu EH, Liu CS, Tan TY, Chang KC (2006) Venturi mask adjuvant oxygen therapy in severe acute ischemic stroke. Arch Neurol 63: 741–744
Ronning OM, Guldvog B (1999) Should stroke victims routinely receive supplemental oxygen? A quasi-randomized controlled trial. Stroke 30: 2033–2037
Singhal AB, Lo EH, Dalkara T, Moskowitz MA (2005) Advances in stroke neuroprotection: hyperoxia and beyond. Neuroimaging Clin N Am 15: 697–720
Rink C, Roy S, Khan M, Ananth P, Kuppusamy P, Sen CK, Khanna S (2010) Oxygen-sensitive outcomes and gene expression in acute ischemic stroke. J Cereb Blood Flow Metab 30: 1275–1287
Rha JH, Saver JL (2007) The impact of recanalization on ischemic stroke outcome: a metaanalysis. Stroke 38: 967–973
Diringer MN (2008) Hyperoxia: good or bad for the injured brain? Current Opinion in Critical Care 14: 167–171
Altemeier WA, Sinclair SE (2007) Hyperoxia in the intensive care unit: why more is not always better. Curr Opin Crit Care 13: 73–78
de Jonge E, Peelen L, Keijzers PJ, et al (2008) Association between administered oxygen, arterial partial oxygen pressure and mortality in mechanically ventilated intensive care unit patients. Crit Care 12: R156
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2012 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Hommers, C.E., Nolan, J.P. (2012). Controlled Oxygenation after Cardiac Arrest. In: Vincent, JL. (eds) Annual Update in Intensive Care and Emergency Medicine 2012. Annual Update in Intensive Care and Emergency Medicine, vol 2012. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-25716-2_47
Download citation
DOI: https://doi.org/10.1007/978-3-642-25716-2_47
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-642-25715-5
Online ISBN: 978-3-642-25716-2
eBook Packages: MedicineMedicine (R0)