Abstract
The concept of radiotheragnotics is employed at many nuclear medicine entities worldwide, where 68Ga and 177Lu are the most commonly used radiometals for PET imaging and radionuclide therapy, respectively.
The application of radionuclides of the same element (i.e., radioisotopes) would enable the preparation of chemically identical radiopharmaceuticals for both imaging and therapy. At the Paul Scherrer Institute, the realization of this concept has been a major research focus over the last decade. Among several interesting metals, terbium is of particular relevance. It comprises four radioisotopes suitable for nuclear medicine purposes, including imaging using single photon emission computed tomography (SPECT; terbium-155) and positron emission tomography (PET; terbium-152), respectively, as well as targeted radionuclide therapy using α-particles (terbium-149) and β¯-particles (terbium-161).
This chapter presents the birth of the terbium “sisters” at PSI and briefly summarizes the most important achievements obtained with each of the four sisters. Future perspectives and challenges with regard to clinical translation of the “terbium sister concept” are presented and discussed.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
- Terbium
- Terbium-149
- Terbium-152
- Terbium-155
- Terbium-161
- Theragnostics
- SPECT
- PET
- Radionuclide therapy
- Alpha
- Beta
- Auger electrons
- SPECT/CT
- PET/CT
- β¯-therapy
- α-therapy
23.1 Introduction
Currently, the concept of radiotheragnotics—referring to therapy and diagnosis—is well implemented at many nuclear medicine entities worldwide [1]. In this context, various tumor-targeting agents, labeled with diagnostic and therapeutic radionuclides, are currently being used for nuclear imaging and radionuclide therapy, respectively. Since PET has become the imaging methodology of choice, 68Ga has become the most important radiometal for imaging purposes, whereas radionuclide therapy is mostly performed with 177Lu, a medium-energy β¯-particle emitter [2]. The co-emission of a low percentage of γ-radiation also enables its use for pre-therapeutic dosimetry purposes.
While the concept of 68Ga/177Lu-radiotheragnostics using somatostatin receptor-targeted peptides has shown promise for the treatment of neuroendocrine tumors [3], more recently, PSMA-targeted small molecules have been extensively investigated with this pair of radionuclides for patients suffering from metastatic castration-resistant prostate cancer (mCRPC) [4, 5].
At Paul Scherrer Institute (PSI), we have focused on the concept of using radionuclides of the same element (i.e., radioisotopes) with the aim to prepare chemically identical radiopharmaceuticals for both imaging and therapy. In this regard, we have performed extensive work with the scandium family and set up the production of scandium-44 using the research cyclotron at PSI [6]. Prof. Richard Baum’s group was the first worldwide to use the cyclotron-produced scandium-44 for a patient scan with [44Sc]Sc-DOTATOC [7]. This was the start of our fruitful collaboration with Prof. Baum and colleagues at Zentralklinik Bad Berka, Germany.
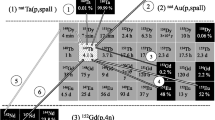
A major focus of our work at PSI over the last decade has been the production and investigation of the terbium “sisters.” Terbium comprises four radioisotopes of interest for nuclear imaging, using single photon emission computed tomography (SPECT; terbium-155) and positron emission tomography (PET; terbium-152), respectively, as well as for α-particle (terbium-149) and β¯-particle-based (terbium-161) radionuclide therapy [8]. The production and a preliminary preclinical application of all four terbium sisters was demonstrated in a collaborative study between the Paul Scherrer Institute (PSI) and ISOLDE/CERN, Geneva, Switzerland, and published in 2012 [9]. Terbium-161 was produced at PSI according to the method previously published by Lehenberger et al. [10], while the three other terbium sisters were obtained by spallation reaction and subsequent online mass separation at CERN, followed by chemical separation at PSI [9]. The activity obtained was low; however, it was possible to perform proof-of-concept SPECT and PET imaging experiments and α- and β¯-radionuclide therapy in a small number of mice [9]. The unique feature of terbium raised the idea of calling it a “Swiss Army Knife” (originated from Prof. R. Schibli, head of Center of Radiopharmaceutical Sciences at PSI), as it combines all functions of nuclear medicine in just one element like a Swiss army knife—a multifunctional device. In order to specify the origin of the quadruplet of terbium radioisotopes for nuclear medicine applications more precisely, the term has been modified to “PSI’s Swiss Army Knife” (Fig. 23.1).
Each of the four terbium sisters was investigated more in depth by our research groups at PSI and in collaboration with internal and external partners. In this chapter, we briefly summarize the achievements in the field of research with the four terbium sisters.
23.2 The PET Sister: Terbium-152
PET is the preferred imaging modality over SPECT due to the higher resolution and increased sensitivity as demonstrated by the high-quality PET scans obtained with 68Ga-labeled somatostatin analogues, which has basically replaced the use of 111In-octreotide for SPECT [11, 12]. Terbium-152 is the only radiolanthanide that emits β+-particles useful for PET imaging without co-emission of α- or β¯-particles. Although the β+-energy is quite high (Eβ+av = 1140 keV, I = 20.3%) and the decay accompanied by several γ-ray emissions, it was our goal to demonstrate the concept of “bench-to-bedside” with this particular terbium sister (Scheme 23.1).
The terbium-152 sister’s personality. (Figurine ©Ekaterina Zimodro/123RF)
Terbium-152 was used to label to DOTANOC and the radiopeptide was employed in a proof-of-concept PET imaging study in AR42J tumor-bearing mice [13]. In collaboration with the university hospital of Lausanne (CHUV), Switzerland, a microPET-based dosimetry study was performed in tumor-bearing mice using a 152Tb-labeled antibody fragment ([152Tb]Tb-CHX-DTPA-scFv78-Fc) [14]. Finally, [152Tb]Tb-PSMA-617 was also employed for PET imaging of a prostate cancer mouse model for comparison of the distribution with its 177Lu-labeled counterpart (Fig. 23.2) [15].
Nuclear images shown as maximum intensity projections of PC-3 PIP/flu tumor-bearing mice at 2 h and 15 h post injection of the radioligand. (a) PET/CT scans of a mouse injected with [152Tb]Tb-PSMA-617 and (b) SPECT/CT scan of a mouse injected with [177Lu]Lu-PSMA-617. PSMA+ PSMA-positive PC-3 PIP tumor, PSMA− PSMA-negative PC-3 flu tumor, Bl urinary bladder. (This figure was reproduced from Müller et al. 2019 EJNMMI Res [15])
Terbium-152 was the first of all four terbium sisters to be used for a clinical application in a patient [15, 16]. [152Tb]Tb-DOTATOC, prepared at Zentralklinik Bad Berka, Germany, was administered to a 67-year-old patient with metastatic well-differentiated functional neuroendocrine neoplasm of the ileum, presented for restaging 8 years after the sixth cycle of peptide receptor radionuclide therapy (PRRT) [16]. PET images visualized even the smaller metastases, with increased tumor-to-background contrast over time. The relatively long half-life of terbium-152 (T1/2 = 17.5 h) made it feasible to scan the patient over an extended period, a feature which would be useful for dosimetry purposes prior to radiolanthanide-based radionuclide therapy [16]. In a subsequent attempt to demonstrate the potential of performing clinical PET, terbium-152 was shipped to Zentralklinik Bad Berka, Germany, where it was used for the labeling of PSMA-617 [15]. [152Tb]Tb-PSMA-617 was administered to a patient suffering from mCRPC, and the resultant PET scans were of diagnostic quality (Fig. 23.3). In particular, the images obtained at late time points enabled the visualization of the same metastatic lesions and of the local recurrent tumor as previously detected by [68Ga]Ga-PSMA-11 [15].
PET/CT scans, shown as transversal slices through the upper abdomen at the level of the liver and spleen, obtained over time. (a) PET/CT scan acquired at 50 min, (b) 2.0 h, (c) 18.5 h, and (d) 25 h, respectively, after injection of 140 MBq [152Tb]Tb-PSMA-617. The images clearly demonstrated a PSMA-avid bone metastasis in the ventrolateral part of the left seventh rib (red arrow), where maximum uptake was determined at 18.5 h and 25 h post injection. (This figure was reproduced from Müller et al. 2019 EJNMMI Res [15])
The production of this radionuclide is challenging and, hence, the chances to make it available in large quantities in the near future rather small. Nevertheless, the clinical application of terbium-152 conducted by Prof. Richard Baum and his team paved the way towards translating terbium sisters to clinical application [15, 16].
23.3 The SPECT Sister: Terbium-155
SPECT imaging is still the most commonly used nuclear imaging technology, because of the established technetium-99m kits and imaging protocols for multiple applications [17]. 111In has served as a diagnostic match to yttrium-90 and lutetium-177 for many years [18]. Although PET imaging using gallium-68 has become the preferred technology for diagnostic imaging using tumor-targeted peptides and small molecules, there are still many nuclear medicine sites worldwide without PET scanners. Importantly, the technology of SPECT has improved over the years, enabling the generation of SPECT images of decent quality [19]. In this context, terbium-155 (Eγ = 86 keV I = 32%; 105 keV, I = 25%) may have a role to play in future, as another diagnostic lanthanide match to therapeutic radiolanthanides (Scheme 23.2). Due to its long half-life (T1/2 = 5.32 days), it may be useful for pre-therapeutic dosimetry and/or have a role to play for labeling of long-circulating tumor-targeting agents including albumin-binding small molecules and antibodies.
The terbium-155 sister’s personality. (Figurine ©Ekaterina Zimodro/123RF)
The excellent imaging capability of this novel SPECT nuclide has been demonstrated preclinically with a series of biomolecules of interest at PSI [20]. It included an albumin-binding DOTA-folate ligand, a minigastrin analogue and a L1-CAM-targeting antibody, as well as the clinically employed DOTATOC. Current investigations at PSI are focused on the production of terbium-155 via various nuclear reactions using a cyclotron as a potential option to make it more freely available and in sufficient quantities for future clinical application.
23.4 The Alpha Therapy Sister: Terbium-149
Targeted α-radionuclide therapy (TAT) has garnered interest due to the promising results recently obtained with 225Ac-based radioligand therapy (RLT) of mCRPC patients [21,22,23,24]. An open question refers to potential long-term undesired side effects to the kidneys and other radiosensitive organs and tissue, in which the (α- and β¯-particle-emitting) daughter nuclides of actinium-225 may accumulate. On the other hand, it was found to be superior over the use of bismuth-213 with regard to the therapeutic index for the treatment of mCRPC patients [25]. Terbium-149 may be an alternative α-particle emitter to the currently employed actinium-225 and bismuth-213, respectively (Scheme 23.3). Terbium-149’s half-life of 4.1 h lies between those of bismuth-213 (T1/2 = 45 min) and actinium-225 (T1/2 = 9.9 days). Importantly, the daughter nuclides do not emit α-particles, which may be advantageous with regard to the safety profile of this radionuclide. Even though several production routes were proposed [26], the preparation of substantial quantities of this radionuclide remains a major challenge and would require the construction of dedicated facilities, including mass separation, required to avoid the production of a mixture of terbium radioisotopes.
The terbium-149 sister’s personality. (Figurine ©Ekaterina Zimodro/123RF)
From an application perspective, there are a limited number of preclinical studies with terbium-149 reported in the literature [27, 28]. Beyer et al. performed preclinical experiments, in which 149Tb-labeled rituximab was applied to sterilize single circulating cancer cells in a leukemia mouse model [27]. The treatment led to almost complete remission of mice over a period of 4 months, while untreated control mice developed tumor disease and had to be euthanized as a consequence [27]. At PSI, we have investigated terbium-149 in a proof-of-concept study using a DOTA-folate conjugate in a small number of KB tumor-bearing mice [28]. A dose-dependent inhibition of the tumor growth was observed and, as a consequence, an increased survival time of treated mice as compared to untreated controls [28]. More recently, we were able to conduct a study to investigate [149Tb]Tb-PSMA-617 with several groups of PC-3 PIP tumor-bearing mice [29]. The resulting tumor growth curves revealed a favorable effect of two injections (2 × 3 MBq) as compared to only one injection (1 × 6 MBq). The study indicated the need for more frequent injections, which would most likely also be the case in a clinical setting. Terbium-149 is particularly attractive due to the emission of β+-particles (Eβ+average = 730 keV, I = 7.1%), which enables PET imaging and would allow the monitoring of applied α-therapy [29]. This has been exemplified using [149Tb]Tb-DOTANOC and a mouse model of somatostatin-expressing tumors (Fig. 23.4) [30].
PET/CT images of an AR42J tumor-bearing mouse 2 h after injection of [149Tb]Tb-DOTANOC (7 MBq). (a, b) Maximal intensity projections (MIP) showing distinct accumulation of radioactivity in tumor xenografts (Tu) and residual radioactivity in kidneys (Ki) and urinary bladder (Bl). (This figure was reproduced from Müller et al. 2016 EJNMMI Radiopharm Chem [30])
23.5 The Beta TherapyPLUS Sister (β¯/Conversion/Auger-e¯): Terbium-161
Lutetium-177 is an almost ideal β¯-particle-emitting radionuclide for targeted radionuclide therapy [2]. While it was initially employed with receptor-targeted peptides such as somatostatin analogues [31], it has recently found widespread application in combination with small-molecular-weight PSMA targeting agents [32,33,34]. The medium energy β¯-particles (Eβ¯average = 134 keV; T1/2 = 6.65 days) was determined to be favorable for the treatment of smaller metastases, while preventing radionephrotoxicity previously observed when using yttrium-90, which emits high-energy β¯-particles [35]. Moreover, the co-emission of γ-radiation (Eγ = 113 keV, I = 6.2% and 208 keV, I = 10.4%) enables visualization of the radioligand’s tissue distribution using SPECT.
The concept of using terbium-161 may be seen as a beta therapyPLUS approach: this implies that terbium-161 shares largely all the characteristics of lutetium-177; however, it provides additional features which may make it more effective in cancer therapy (Scheme 23.4).
The terbium-161 sister’s personality. (Figurine ©Ekaterina Zimodro/123RF)
More specifically, the decay properties of terbium-161 are almost identical to those of lutetium-177 in terms of the β¯-energy (Eβ¯average = 154 keV) and half-life (T1/2 = 6.953 days, recently determined by Duran et al. [36]). Like lutetium-177, terbium-161 also emits γ-radiation useful for SPECT imaging. Terbium-161 may, however, have significant advantages with regard to the emission of low-energy electrons. It emits a substantial number of conversion and Auger electrons, which may be of particular value regarding the absorbed dose to single tumor cells. According to published calculations, the mean absorbed dose to small spheres (diameter: 10–20 μm) would increase approximately three to fourfold when using terbium-161 instead of lutetium-177 [37,38,39,40].
The comparison between the effects of terbium-161 and lutetium-177 was performed for the first time in a study using a DOTA-folate ligand [41]. More recently, another comparison was also performed with PSMA-617. It was experimentally demonstrated that [161Tb]Tb-PSMA-617 was more effective in the killing of tumor cells in vitro compared to [177Lu]Lu-PSMA-617 (Fig. 23.5) [42].
Results of an in vitro study demonstrating the favorable effect of terbium-161 over lutetium-177. The bars represent the percentage of PC-3 PIP tumor cell viability after exposure to [161Tb]Tb-PSMA-617 and [177Lu]Lu-PSMA-617, respectively, compared to untreated control cells (set to 100% viability; average ± SD). (This figure was reproduced from Müller et al. 2019 Eur J Nucl Med Mol Imaging [42])
Extensive investigations were performed with human phantoms by Prof. Peter Bernhardt, University of Gothenburg, Sweden, in order to develop a reconstruction code which enables the preparation of high-quality images based on the γ-radiation emitted by terbium-161 (unpublished data). The first SPECT scan using [161Tb]Tb-DOTATOC in a patient with neuroendocrine cancer was performed recently by Prof. Baum at Zentralklinik Bad Berka (unpublished data).
In contrast to the other three terbium sisters, terbium-161 can be produced in large quantities using the 160Gd(n,γ)161Gd → 161Tb nuclear reaction in analogy to the no-carrier-added lutetium-177, as reported by Lehenberger et al. [10]. At PSI, we have developed the production method further over the years to make the radionuclide available at excellent quality that enables labeling of DOTA-functionalized biomolecules at molar activities >100 MBq/nmol [43]. The quantity that can be produced is limited to 20 GBq by the current restriction of the international air transport agency (IATA); however, this restriction is expected to be lifted soon. The current situation regarding the production opportunities is most promising in view of the feasibility to make the radionuclide available for clinical studies in the near future.
23.6 Conclusion and Outlook
Having focused on the investigation of “PSI’s Swiss Army Knife” over the last decade, we have been approached with increased interest from researchers and physicians worldwide over the years. We have performed a number of preclinical studies with the terbium sisters at PSI in collaboration with external partners in Switzerland and abroad. These endeavors enabled the improvement of procedures and results on each level: (1) The production, including targetry and chemical separation, was optimized; (2) radiolabeling of biomolecules was achieved at high molar activities; (3) more detailed preclinical in vitro and in vivo investigations were performed with relevant quantities of activity; (4) human phantom studies were performed with terbium-161 and (5) finally also proof-of-concept clinical applications were achieved with terbium-152 and terbium-161. Thanks to our collaborators in several countries throughout Europe, most prominently, Prof. Richard Baum, the “PSI’s Swiss Army Knife” is becoming a tool of international interest beyond Switzerland and Europe, hence a “United Nations’ Army Knife” (Fig. 23.6). Researchers and clinicians from all other continents including North and South America, Africa, Asia and Australia are interested in using the terbium sisters for nuclear medicine applications.
Based on the results we have achieved over the last decade investigating terbium sisters and according to numerous discussions with researchers and physicians from different fields, it is likely that terbium-161 will be translated to clinical application in the near future. This radionuclide may be also the first to be produced in large quantities for a worldwide application, as is currently the case for lutetium-177. While physicists were the first to propose terbium-161 as a valid alternative to lutetium-177, radiochemists developed the production routes and (radio)pharmacists and biologists experimentally demonstrated the superiority of this radionuclide in preclinical settings. Now, it is time for the nuclear medicine physicians and oncologists to demonstrate the benefit of low-energy electrons in the treatment of disseminated disease by means of clinical studies. Since the production methods for the other three terbium sisters are more challenging and not yet established for large-scale production, success with regard to clinical translation will critically depend on the investment in production facilities.
Finally, it remains to be said that the terbium sisters owe their current popularity in the medical community to Prof. Richard Baum’s efforts to support the translation from bench to bedside.
Our terbium sisters have just started their career in the community. They are still young and, consequently, full of dreams and desires for their future lives in the interdisciplinary environment of research and medical activities. We will continue educating and supporting them to make their future bright and successful and wish them all the best on their future career journey.
References
Jadvar H, Chen X, Cai W, Mahmood U. Radiotheranostics in cancer diagnosis and management. Radiology. 2018;286:388–400. https://doi.org/10.1148/radiol.2017170346.
Banerjee S, Pillai MR, Knapp FF. Lutetium-177 therapeutic radiopharmaceuticals: linking chemistry, radiochemistry, and practical applications. Chem Rev. 2015;115:2934–74. https://doi.org/10.1021/cr500171e.
Gabriel M, Decristoforo C, Kendler D, Dobrozemsky G, Heute D, Uprimny C, et al. 68Ga-DOTA-Tyr3-octreotide PET in neuroendocrine tumors: comparison with somatostatin receptor scintigraphy and CT. J Nucl Med. 2007;48:508–18.
Scarpa L, Buxbaum S, Kendler D, Fink K, Bektic J, Gruber L, et al. The 68Ga/177Lu theragnostic concept in PSMA targeting of castration-resistant prostate cancer: correlation of SUVmax values and absorbed dose estimates. Eur J Nucl Med Mol Imaging. 2017;44:788–800. https://doi.org/10.1007/s00259-016-3609-9.
Heinzel A, Boghos D, Mottaghy FM, Gärtner F, Essler M, von Mallek D, et al. 68Ga-PSMA PET/CT for monitoring response to 177Lu-PSMA-617 radioligand therapy in patients with metastatic castration-resistant prostate cancer. Eur J Nucl Med Mol Imaging. 2019;46:1054–62. https://doi.org/10.1007/s00259-019-4258-6.
van der Meulen NP, Bunka M, Domnanich KA, Müller C, Haller S, Vermeulen C, et al. Cyclotron production of 44Sc: from bench to bedside. Nucl Med Biol. 2015;42:745–51. https://doi.org/10.1016/j.nucmedbio.2015.05.005.
Singh A, van der Meulen NP, Müller C, Klette I, Kulkarni HR, Türler A, et al. First-in-human PET/CT imaging of metastatic neuroendocrine neoplasms with cyclotron-produced 44Sc-DOTATOC: a proof-of-concept study. Cancer Biother Radiopharm. 2017;32:124–32. https://doi.org/10.1089/cbr.2016.2173.
Müller C, Domnanich KA, Umbricht CA, van der Meulen NP. Scandium and terbium radionuclides for radiotheranostics: current state of development towards clinical application. Br J Radiol. 2018;91:20180074. https://doi.org/10.1259/bjr.20180074.
Müller C, Zhernosekov K, Köster U, Johnston K, Dorrer H, Hohn A, et al. A unique matched quadruplet of terbium radioisotopes for PET and SPECT and for a- and b−-radionuclide therapy: an in vivo proof-of-concept study with a new receptor-targeted folate derivative. J Nucl Med. 2012;53:1951–9. https://doi.org/10.2967/jnumed.112.107540.
Lehenberger S, Barkhausen C, Cohrs S, Fischer E, Grünberg J, Hohn A, et al. The low-energy beta− and electron emitter 161Tb as an alternative to 177Lu for targeted radionuclide therapy. Nucl Med Biol. 2011;38:917–24. https://doi.org/10.1016/j.nucmedbio.2011.02.007.
Buchmann I, Henze M, Engelbrecht S, Eisenhut M, Runz A, Schäfer M, et al. Comparison of 68Ga-DOTATOC PET and 111In-DTPAOC (Octreoscan) SPECT in patients with neuroendocrine tumours. Eur J Nucl Med Mol Imaging. 2007;34:1617–26. https://doi.org/10.1007/s00259-007-0450-1.
Srirajaskanthan R, Kayani I, Quigley AM, Soh J, Caplin ME, Bomanji J. The role of 68Ga-DOTATATE PET in patients with neuroendocrine tumors and negative or equivocal findings on 111In-DTPA-octreotide scintigraphy. J Nucl Med. 2010;51:875–82. https://doi.org/10.2967/jnumed.109.066134.
Müller C, Vermeulen C, Johnston K, Köster U, Schmid R, Türler A, et al. Preclinical in vivo application of 152Tb-DOTANOC: a radiolanthanide for PET imaging. EJNMMI Res. 2016;6:35. https://doi.org/10.1186/s13550-016-0189-4.
Cicone F, Gnesin S, Denoel T, Stora T, van der Meulen NP, Müller C, et al. Internal radiation dosimetry of a 152Tb-labeled antibody in tumor-bearing mice. EJNMMI Res. 2019;9:53. https://doi.org/10.1186/s13550-019-0524-7.
Müller C, Singh A, Umbricht CA, Kulkarni HR, Johnston K, Benešová M, et al. Preclinical investigations and first-in-human application of 152Tb-PSMA-617 for PET/CT imaging of prostate cancer. EJNMMI Res. 2019;9:68. https://doi.org/10.1186/s13550-019-0538-1.
Baum RP, Singh A, Benešová M, Vermeulen C, Gnesin S, Köster U, et al. Clinical evaluation of the radiolanthanide terbium-152: first-in-human PET/CT with 152Tb-DOTATOC. Dalton Trans. 2017;46:14638–46. https://doi.org/10.1039/c7dt01936j.
Israel O, Pellet O, Biassoni L, De Palma D, Estrada-Lobato E, Gnanasegaran G, et al. Two decades of SPECT/CT - the coming of age of a technology: an updated review of literature evidence. Eur J Nucl Med Mol Imaging. 2019;46:1990–2012. https://doi.org/10.1007/s00259-019-04404-6.
Kwekkeboom DJ, Bakker WH, Kooij PP, Konijnenberg MW, Srinivasan A, Erion JL, et al. [177Lu-DOTA0Tyr3]octreotate: comparison with [111In-DTPA0]octreotide in patients. Eur J Nucl Med. 2001;28:1319–25.
Ljungberg M, Pretorius PH. SPECT/CT: an update on technological developments and clinical applications. Br J Radiol. 2018;91:20160402. https://doi.org/10.1259/bjr.20160402.
Müller C, Fischer E, Behe M, Köster U, Dorrer H, Reber J, et al. Future prospects for SPECT imaging using the radiolanthanide terbium-155—production and preclinical evaluation in tumor-bearing mice. Nucl Med Biol. 2014;41(Suppl):e58–65. https://doi.org/10.1016/j.nucmedbio.2013.11.002.
Kratochwil C, Bruchertseifer F, Giesel FL, Apostolidis C, Haberhorn U, Morgenstern A. 225Ac-PSMA-617 for PSMA targeting alpha-radiation therapy of 28 patients with mCRPC. Eur J Nucl Med Mol Imaging. 2016;43:S137.
Kratochwil C, Bruchertseifer F, Giesel FL, Weis M, Verburg FA, Mottaghy F, et al. 225Ac-PSMA-617 for PSMA-targeted a-radiation therapy of metastatic castration-resistant prostate cancer. J Nucl Med. 2016;57:1941–4. https://doi.org/10.2967/jnumed.116.178673.
Kratochwil C, Bruchertseifer F, Rathke H, Hohenfellner M, Giesel FL, Haberkorn U, et al. Targeted alpha therapy of mCRPC with 225Actinium-PSMA-617: swimmer-plot analysis suggests efficacy regarding duration of tumor-control. J Nucl Med. 2018;59:795. https://doi.org/10.2967/jnumed.117.203539.
Sathekge M, Bruchertseifer F, Knoesen O, Reyneke F, Lawal I, Lengana T, et al. 225Ac-PSMA-617 in chemotherapy-naive patients with advanced prostate cancer: a pilot study. Eur J Nucl Med Mol Imaging. 2019;46:129–38. https://doi.org/10.1007/s00259-018-4167-0.
Kratochwil C, Schmidt K, Afshar-Oromieh A, Bruchertseifer F, Rathke H, Morgenstern A, et al. Targeted alpha therapy of mCRPC: dosimetry estimate of 213Bismuth-PSMA-617. Eur J Nucl Med Mol Imaging. 2018;45:31–7. https://doi.org/10.1007/s00259-017-3817-y.
Beyer GJ, Comor JJ, Dakovic M, Soloviev D, Tamburella C, Hagebo E, et al. Production routes of the alpha emitting 149Tb for medical application. Radiochim Acta. 2002;90:247–52. https://doi.org/10.1524/ract.2002.90.5_2002.247.
Beyer GJ, Miederer M, Vranjes-Duric S, Comor JJ, Kunzi G, Hartley O, et al. Targeted alpha therapy in vivo: direct evidence for single cancer cell kill using 149Tb-rituximab. Eur J Nucl Med Mol Imaging. 2004;31:547–54. https://doi.org/10.1007/s00259-003-1413-9.
Müller C, Reber J, Haller S, Dorrer H, Köster U, Johnston K, et al. Folate receptor targeted alpha-therapy using terbium-149. Pharmaceuticals (Basel). 2014;7:353–65. https://doi.org/10.3390/ph7030353.
Umbricht CA, Köster U, Bernhardt P, Gracheva N, Johnston K, Schibli R, et al. Alpha-PET for prostate cancer: preclinical investigation using 149Tb-PSMA-617. Sci Rep. 2019;9:17800. https://doi.org/10.1038/s41598-019-54150-w.
Müller C, Vermeulen C, Köster U, Johnston K, Türler A, Schibli R, et al. Alpha-PET with terbium-149: evidence and perspectives for radiotheragnostics. Eur J Nucl Med Mol Imaging Radiopharm Chem. 2017;1:5.
Strosberg J, El-Haddad G, Wolin E, Hendifar A, Yao J, Chasen B, et al. Phase 3 trial of 177Lu-DOTATATE for midgut neuroendocrine tumors. N Engl J Med. 2017;376:125–35. https://doi.org/10.1056/NEJMoa1607427.
Baum RP, Kulkarni HR, Schuchardt C, Singh A, Wirtz M, Wiessalla S, et al. 177Lu-labeled prostate-specific membrane antigen radioligand therapy of metastatic castration-resistant prostate cancer: safety and efficacy. J Nucl Med. 2016;57:1006–13. https://doi.org/10.2967/jnumed.115.168443.
Rahbar K, Ahmadzadehfar H, Kratochwil C, Haberkorn U, Schäfers M, Essler M, et al. German multicenter study investigating 177Lu-PSMA-617 radioligand therapy in advanced prostate cancer patients. J Nucl Med. 2017;58:85–90. https://doi.org/10.2967/jnumed.116.183194.
Bräuer A, Grubert LS, Roll W, Schrader AJ, Schäfers M, Bögemann M, et al. 177Lu-PSMA-617 radioligand therapy and outcome in patients with metastasized castration-resistant prostate cancer. Eur J Nucl Med Mol Imaging. 2017;44:1663–70. https://doi.org/10.1007/s00259-017-3751-z.
Valkema R, Pauwels SA, Kvols LK, Kwekkeboom DJ, Jamar F, de Jong M, et al. Long-term follow-up of renal function after peptide receptor radiation therapy with 90Y-DOTA0,Tyr3-octreotide and 177Lu-DOTA0,Tyr3-octreotate. J Nucl Med. 2005;46(Suppl 1):83S–91S.
Duran MT, Juget F, Nedjadi Y, Bochud F, Grundler PV, Gracheva N, et al. Determination of 161Tb half-life by three measurement methods. Appl Radiat Isot. 2020;159:109085. https://doi.org/10.1016/j.apradiso.2020.109085.
Bernhardt P, Benjegard SA, Kolby L, Johanson V, Nilsson O, Ahlman H, et al. Dosimetric comparison of radionuclides for therapy of somatostatin receptor-expressing tumors. Int J Radiat Oncol Biol Phys. 2001;51:514–24.
Hindie E, Zanotti-Fregonara P, Quinto MA, Morgat C, Champion C. Dose deposits from 90Y, 177Lu, 111In, and 161Tb in micrometastases of various sizes: implications for radiopharmaceutical therapy. J Nucl Med. 2016;57:759–64. https://doi.org/10.2967/jnumed.115.170423.
Champion C, Quinto MA, Morgat C, Zanotti-Fregonara P, Hindie E. Comparison between three promising b−-emitting radionuclides, 67Cu, 47Sc and 161Tb, with emphasis on doses delivered to minimal residual disease. Theranostics. 2016;6:1611–8. https://doi.org/10.7150/thno.15132.
Alcocer-Avila ME, Ferreira A, Quinto MA, Morgat C, Hindie E, Champion C. Radiation doses from 161Tb and 177Lu in single tumour cells and micrometastases. EJNMMI Phys. 2020;7:33. https://doi.org/10.1186/s40658-020-00301-2.
Müller C, Reber J, Haller S, Dorrer H, Bernhardt P, Zhernosekov K, et al. Direct in vitro and in vivo comparison of 161Tb and 177Lu using a tumour-targeting folate conjugate. Eur J Nucl Med Mol Imaging. 2014;41:476–85. https://doi.org/10.1007/s00259-013-2563-z.
Müller C, Umbricht CA, Gracheva N, Tschan VJ, Pellegrini G, Bernhardt P, et al. Terbium-161 for PSMA-targted radionuclide therapy of prostate cancer. Eur J Nucl Med Mol Imaging. 2019;46:1919. https://doi.org/10.1007/s00259-019-04345-0.
Gracheva N, Müller C, Talip Z, Heinitz S, Köster U, Zeevaart JR, et al. Production and characterization of no-carrier-added 161Tb as an alternative to the clinically-applied 177Lu for radionuclide therapy. EJNMMI Radiopharm Chem. 2019;4:12. https://doi.org/10.1186/s41181-019-0063-6.
Acknowledgments
The authors thank researchers and technical staff members at the Center for Radiopharmaceutical Sciences and the Laboratory of Radiochemistry at PSI for all the work and effort they have placed into the research with the terbium sisters. They would also like to thank all external collaborators, particularly Dr. Karl Johnston and his team at ISOLDE/CERN, Dr. Claude Bailat and his team at the Institute of Radiation Physics (IRA) Lausanne, Switzerland; Prof. Peter Bernhardt and his team at the University of Gothenburg, Sweden; Dr. Ulli Köster and his team at the reactor facility Institute Lau-Langevin, Grenoble, France and Dr. Jan Rijn Zeevaart and his team at the SAFARI-1 reactor facility at Necsa, Pelindaba, South Africa. The authors would like to thank Prof. Richard Baum and his team of physicians and medical physicists for their interest in the terbium sisters and are grateful for all the efforts of the nursing staff, as well as nuclear medicine technologists of the Theranostics Center for Molecular Radiotherapy and Precision Oncology for patient management at Zentralklinik Bad Berka, Germany.
Funding
The research conducted with terbium sisters was supported by several funding institutions which are gratefully acknowledged: the Swiss National Science Foundation (SNSF: IZLIZ3_156800, 310030–156803); the Neuroendocrine Tumor Research Foundation (NETRF; Petersen Investigator Award 2018); the Personalized Health and Related Technology (PHRT-301), the Swiss Cancer Research Foundation (KFS-4678-02-2019-R) and the ENSAR2 (EU H2020 project N° 654002).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2024 The Author(s)
About this chapter
Cite this chapter
Müller, C., van der Meulen, N.P. (2024). Terbium “Sisters”: More Than just a “Swiss Army Knife”. In: Prasad, V. (eds) Beyond Becquerel and Biology to Precision Radiomolecular Oncology: Festschrift in Honor of Richard P. Baum. Springer, Cham. https://doi.org/10.1007/978-3-031-33533-4_23
Download citation
DOI: https://doi.org/10.1007/978-3-031-33533-4_23
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-33532-7
Online ISBN: 978-3-031-33533-4
eBook Packages: MedicineMedicine (R0)