Abstract
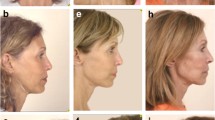
Parotidectomy defect reconstruction requires an understanding of facial form and function. The main goals for the reconstructive surgeon include restoring facial contour and symmetry with stable tissue volumes, avoiding Frey’s syndrome, ensuring adequate skin coverage, and providing reconstruction of the facial nerve functional deficit. There are many reconstructive options available, and here we discuss strategies for addressing defects created by the superficial parotidectomy, total parotidectomy, and radical parotidectomy.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Abbreviations
- ADM:
-
Acellular dermal matrix
- ALT:
-
Anterolateral thigh
- RF:
-
Radial forearm
- SAI:
-
Supraclavicular artery island
- SIF:
-
Submental island flap
- SMAS:
-
Superficial muscular aponeurotic system
References
Lu GN, et al. Analysis of facial reanimation procedures performed concurrently with total parotidectomy and facial nerve sacrifice. JAMA Facial Plast Surg. 2019;21(1):50–5.
Fiacchini G, et al. Frey syndrome, first bite syndrome, great auricular nerve morbidity, and quality of life following parotidectomy. Eur Arch Otorhinolaryngol. 2018;275(7):1893–902.
Nitzan D, et al. Quality of life following parotidectomy for malignant and benign disease. Plast Reconstr Surg. 2004;114(5):1060–7.
Frey L. Le syndrome du nerf auriculo-temporal. Rev Neurol. 1923;2:97–104.
Ghanem T. Parotid defects. Facial Plast Surg Clin North Am. 2009;17(2):263–9.
Govindaraj S, et al. The use of acellular dermis in the prevention of Frey's syndrome. Laryngoscope. 2001;111(11 Pt 1):1993–8.
Lee CC, Chan RC, Chan JY. Predictors for Frey syndrome development after parotidectomy. Ann Plast Surg. 2017;79(1):39–41.
Manola M, et al. The effectiveness of sternocleidomastoid flap versus superficial musculoaponeurotic system flap for the prevention of Frey syndrome and facial depressed deformity in parotid surgery for pleomorphic adenoma. Ann Plast Surg. 2018;80(2):125–9.
Motz KM, Kim YJ. Auriculotemporal syndrome (Frey syndrome). Otolaryngol Clin N Am. 2016;49(2):501–9.
Conger BT, Gourin CG. Free abdominal fat transfer for reconstruction of the total parotidectomy defect. Laryngoscope. 2008;118(7):1186–90.
Vico PG, Delange A, De Vooght A. Autologous fat transfer: an aesthetic and functional refinement for parotidectomy. Surg Res Pract. 2014;2014:873453.
Loyo M, Gourin CG. Free abdominal fat transfer for partial and total parotidectomy defect reconstruction. Laryngoscope. 2016;126(12):2694–8.
Honeybrook A, et al. Free dermal fat graft reconstruction of the head and neck: an alternate reconstructive option. Am J Otolaryngol. 2017;38(3):291–6.
Fasolis M, et al. Dermofat graft after superficial parotidectomy to prevent Frey syndrome and depressed deformity. J Craniofac Surg. 2013;24(4):1260–2.
Harada T, et al. Dermis-fat graft after parotidectomy to prevent Frey's syndrome and the concave deformity. Ann Plast Surg. 1993;31(5):450–2.
Nosan DK, Ochi JW, Davidson TM. Preservation of facial contour during parotidectomy. Otolaryngol Head Neck Surg. 1991;104(3):293–8.
Curry JM, et al. Superficial musculoaponeurotic system elevation and fat graft reconstruction after superficial parotidectomy. Laryngoscope. 2008;118(2):210–5.
Sinha UK, et al. Use of AlloDerm implant to prevent Frey syndrome after parotidectomy. Arch Facial Plast Surg. 2003;5(1):109–12.
Zeng XT, et al. AlloDerm implants for prevention of Frey syndrome after parotidectomy: a systematic review and meta-analysis. Mol Med Rep. 2012;5(4):974–80.
Wang S, et al. Effects of free fat grafting on the prevention of Frey’s syndrome and facial depression after parotidectomy: a prospective randomized trial. Laryngoscope. 2016;126(4):815–9.
Jost G, Legent F, Baupelot S. Filling of residual depressions after parotidectomy by a sterno-cleido-mastoid strip. Ann Otolaryngol Chir Cervicofac. 1968;85(4):357–60.
Ariyan S. One-stage reconstruction for defects of the mouth using a sternomastoid myocutaneous flap. Plast Reconstr Surg. 1979;63(5):618–25.
Irvine LE, Larian B, Azizzadeh B. Locoregional parotid reconstruction. Otolaryngol Clin North Am. 2016;49(2):435–46.
Fee WE, Tran LE. Functional outcome after total parotidectomy reconstruction. Laryngoscope. 2004;114(2):223–6.
Casler JD, Conley J. Sternocleidomastoid muscle transfer and superficial musculoaponeurotic system plication in the prevention of Frey's syndrome. Laryngoscope. 1991;101(1 Pt 1):95–100.
Sanabria A, et al. Sternocleidomastoid muscle flap in preventing Frey's syndrome after parotidectomy: a systematic review. Head Neck. 2012;34(4):589–98.
Alvarez GE, Escamilla JT, Carranza A. The split sternocleidomastoid myocutaneous flap. Br J Plast Surg. 1983;36(2):183–6.
Naunheim M, Seth R, Knott PD. Sternocleidomastoid contour restoration: an added benefit of the anterolateral thigh free flap during facial reconstruction. Am J Otolaryngol. 2016;37(2):139–43.
Kerawala CJ, McAloney N, Stassen LF. Prospective randomised trial of the benefits of a sternocleidomastoid flap after superficial parotidectomy. Br J Oral Maxillofac Surg. 2002;40(6):468–72.
Zhao HW, et al. Preventing post-surgical complications by modification of parotidectomy. Int J Oral Maxillofac Surg. 2008;37(4):345–9.
Allison GR, Rappaport I. Prevention of Frey's syndrome with superficial musculoaponeurotic system interposition. Am J Surg. 1993;166(4):407–10.
Barberá R, et al. Superficial musculoaponeurotic system flap in partial parotidectomy and clinical and subclinical Frey's syndrome. Cosmesis and quality of life. Head Neck. 2014;36(1):130–6.
Dulguerov N, Makni A, Dulguerov P. The superficial musculoaponeurotic system flap in the prevention of Frey syndrome: a meta-analysis. Laryngoscope. 2016;126(7):1581–4.
Dell'aversana Orabona G, et al. Reconstructive techniques of the parotid region. J Craniofac Surg. 2014;25(3):998–1002.
Ahmed OA, Kolhe PS. Prevention of Frey's syndrome and volume deficit after parotidectomy using the superficial temporal artery fascial flap. Br J Plast Surg. 1999;52(4):256–60.
Kazanjian VH, Converse JM. The surgical treatment of facial injuries. Baltimore: Williams & Wilkins; 1949. xiv, 574 p.
Pallua N, et al. The fasciocutaneous supraclavicular artery island flap for releasing postburn mentosternal contractures. Plast Reconstr Surg. 1997;99(7):1878–84; discussion 1885–6.
Emerick KS, et al. Supraclavicular artery island flap for reconstruction of complex parotidectomy, lateral skull base, and total auriculectomy defects. JAMA Otolaryngol Head Neck Surg. 2014;140(9):861–6.
Kokot N, et al. Use of the supraclavicular artery island flap for reconstruction of cervicofacial defects. Otolaryngol Head Neck Surg. 2014;150(2):222–8.
Martin D, et al. The submental island flap: a new donor site. Anatomy and clinical applications as a free or pedicled flap. Plast Reconstr Surg. 1993;92(5):867–73.
Moubayed SP, Rahal A, Ayad T. The submental island flap for soft-tissue head and neck reconstruction: step-by-step video description and long-term results. Plast Reconstr Surg. 2014;133(3):684–6.
Barton BM, et al. The submental island flap is a viable reconstructive option for a variety of head and neck ablative defects. Ochsner J. 2018;18(1):53–8.
Bayon R, Davis AB. Submental flap for soft tissue reconstruction following radical parotidectomy. Otolaryngol Head Neck Surg. 2019;160(6):1130–2. https://doi.org/10.1177/0194599819827822.
Patel AV, et al. Submental artery island flap versus free flap reconstruction of lateral facial soft tissue and parotidectomy defects: comparison of outcomes and patient factors. Oral Oncol. 2018;78:194–9.
Baker DC, Shaw WW, Conley J. Reconstruction of radical parotidectomy defects. Am J Surg. 1979;138(4):550–4.
Wells JH, Edgerton MT. Correction of severe hemifacial atrophy with a free dermis-flat from the lower abdomen. Plast Reconstr Surg. 1977;59(2):223–30.
Cannady SB, et al. Total parotidectomy defect reconstruction using the buried free flap. Otolaryngol Head Neck Surg. 2010;143(5):637–43.
Revenaugh PC, et al. Minimizing morbidity in microvascular surgery: small-caliber anastomotic vessels and minimal access approaches. JAMA Facial Plast Surg. 2015;17(1):44–8.
Rosenthal EL, et al. Evolution of a paradigm for free tissue transfer reconstruction of lateral temporal bone defects. Head Neck. 2008;30(5):589–94.
Knott PD, et al. Short-term donor site morbidity: a comparison of the anterolateral thigh and radial forearm fasciocutaneous free flaps. Head Neck. 2016;38(Suppl 1):E945–8.
Fritz MA, Rolfes BN. Microvascular reconstruction of the parotidectomy defect. Otolaryngol Clin N Am. 2016;49(2):447–57.
Hanasono MM, Skoracki RJ, Yu P. A prospective study of donor-site morbidity after anterolateral thigh fasciocutaneous and myocutaneous free flap harvest in 220 patients. Plast Reconstr Surg. 2010;125(1):209–14.
Collins J, Ayeni O, Thoma A. A systematic review of anterolateral thigh flap donor site morbidity. Can J Plast Surg. 2012;20(1):17–23.
Cigna E, et al. An experience on primary thinning and secondary debulking of anterolateral thigh flap in head and neck reconstruction. Eur Rev Med Pharmacol Sci. 2012;16(8):1095–101.
Seth R, et al. Volume-directed facial soft tissue deficit reconstruction. Facial Plast Surg. 2010;26(6):494–503.
Elliott RM, et al. Reconstruction of complex total parotidectomy defects using the free anterolateral thigh flap: a classification system and algorithm. Ann Plast Surg. 2011;66(5):429–37.
Urken ML, et al. The neurofasciocutaneous radial forearm flap in head and neck reconstruction: a preliminary report. Laryngoscope. 1990;100(2 Pt 1):161–73.
Lin AC, Lin DT. Reconstruction of lateral skull base defects with radial forearm free flaps: the double-layer technique. J Neurol Surg B Skull Base. 2015;76(4):257–61.
Thompson NJ, et al. Reconstruction outcomes following lateral skull base resection. Otol Neurotol. 2017;38(2):264–71.
Bertelsen C, Liu C, Kokot N. Reconstruction of parotidectomy and lateral skull base defects. Curr Opin Otolaryngol Head Neck Surg. 2017;25(5):431–8.
Wax MK, et al. The role of free tissue transfer in the reconstruction of massive neglected skin cancers of the head and neck. Arch Facial Plast Surg. 2003;5(6):479.
Theriault C, Fitzpatrick PJ. Malignant parotid tumors. Prognostic factors and optimum treatment. Am J Clin Oncol. 1986;9(6):510–6.
Owusu JA, Truong L, Kim JC. Facial nerve reconstruction with concurrent masseteric nerve transfer and cable grafting. JAMA Facial Plast Surg. 2016;18(5):335–9.
Hontanilla B, Qiu SS, Marre D. Effect of postoperative brachytherapy and external beam radiotherapy on functional outcomes of immediate facial nerve repair after radical parotidectomy. Head Neck. 2014;36(1):113–9.
Reddy PG, Arden RL, Mathog RH. Facial nerve rehabilitation after radical parotidectomy. Laryngoscope. 1999;109(6):894–9.
Wax MK, Kaylie DM. Does a positive neural margin affect outcome in facial nerve grafting? Head Neck. 2007;29(6):546–9.
Humphrey CD, Kriet JD. Nerve repair and cable grafting for facial paralysis. Facial Plast Surg. 2008;24(2):170–6.
Kim J. Neural reanimation advances and new technologies. Facial Plast Surg Clin North Am. 2016;24(1):71–84.
Spector JG, et al. Facial nerve regeneration through autologous nerve grafts: a clinical and experimental study. Laryngoscope. 1991;101(5):537–54.
Gardetto A, et al. Direct coaptation of extensive facial nerve defects after removal of the superficial part of the parotid gland: an anatomic study. Head Neck. 2002;24(12):1047–53.
Yarbrough WG, Brownlee RE, Pillsbury HC. Primary anastomosis of extensive facial nerve defects: an anatomic study. Am J Otol. 1993;14(3):238–46.
Conley JJ. Facial nerve grafting in treatment of parotid gland tumors; new technique. AMA Arch Surg. 1955;70(3):359–66.
Millesi H. Nerve grafting. Clin Plast Surg. 1984;11(1):105–13.
Lee MC, et al. Functional outcomes of multiple sural nerve grafts for facial nerve defects after tumor-ablative surgery. Arch Plast Surg. 2015;42(4):461–8.
Nichols CM, et al. Effects of motor versus sensory nerve grafts on peripheral nerve regeneration. Exp Neurol. 2004;190(2):347–55.
Moradzadeh A, et al. The impact of motor and sensory nerve architecture on nerve regeneration. Exp Neurol. 2008;212(2):370–6.
Revenaugh PC, et al. Motor nerve to the vastus lateralis. Arch Facial Plast Surg. 2012;14(5):365–8.
Stennert E. I. Hypoglossal facial anastomosis: its significance for modern facial surgery. II. Combined approach in extratemporal facial nerve reconstruction. Clin Plast Surg. 1979;6(3):471–86.
Manni JJ, et al. Reanimation of the paralyzed face by indirect hypoglossal-facial nerve anastomosis. Am J Surg. 2001;182(3):268–73.
Volk GF, et al. Reconstruction of complex peripheral facial nerve defects by a combined approach using facial nerve interpositional graft and hypoglossal-facial jump nerve suture. Laryngoscope. 2011;121(11):2402–5.
Spira M. Anastomosis of masseteric nerve to lower division of facial nerve for correction of lower facial paralysis. Preliminary report. Plast Reconstr Surg. 1978;61(3):330–4.
Klebuc M. The evolving role of the masseter-to-facial (V-VII) nerve transfer for rehabilitation of the paralyzed face. Ann Chir Plast Esthet. 2015;60(5):436–41.
Fournier HD, et al. An anatomical study of the motor distribution of the mandibular nerve for a masseteric-facial anastomosis to restore facial function. Surg Radiol Anat. 1997;19(4):241–4.
Collar RM, Byrne PJ, Boahene KD. The subzygomatic triangle: rapid, minimally invasive identification of the masseteric nerve for facial reanimation. Plast Reconstr Surg. 2013;132(1):183–8.
Coombs CJ, et al. Masseteric-facial nerve coaptation--an alternative technique for facial nerve reinnervation. J Plast Reconstr Aesthet Surg. 2009;62(12):1580–8.
Murphey AW, Clinkscales WB, Oyer SL. Masseteric nerve transfer for facial nerve paralysis. JAMA Facial Plast Surg. 2018;20(2):104.
Klebuc MJ. Facial reanimation using the masseter-to-facial nerve transfer. Plast Reconstr Surg. 2011;127(5):1909–15.
McLaughlin CR. Surgical support in permanent facial paralysis. Plast Reconstr Surg (1946). 1953;11(4):302–14.
Owusu Boahene KD. Temporalis muscle tendon unit transfer for smile restoration after facial paralysis. Facial Plast Surg Clin North Am. 2016;24(1):37–45.
Burkhalter WE. Early tendon transfer in upper extremity peripheral nerve injury. Clin Orthop Relat Res. 1974;104:68–79.
Ciolek PJ, Prendes BL, Fritz MA. Comprehensive approach to reestablishing form and function after radical parotidectomy. Am J Otolaryngol. 2018;39(5):542–7.
Fritz M, Rolfes BN. Management of facial paralysis due to extracranial tumors. Facial Plast Surg. 2015;31(2):110–6.
Boahene KD. Principles and biomechanics of muscle tendon unit transfer: application in temporalis muscle tendon transposition for smile improvement in facial paralysis. Laryngoscope. 2013;123(2):350–5.
Boahene KD, et al. Minimally invasive temporalis tendon transposition. Arch Facial Plast Surg. 2011;13(1):8–13.
Boahene KD, Ishii LE, Byrne PJ. In vivo excursion of the temporalis muscle-tendon unit using electrical stimulation: application in the design of smile restoration surgery following facial paralysis. JAMA Facial Plast Surg. 2014;16(1):15–9.
Coulson SE, et al. Physiotherapy rehabilitation of the smile after long-term facial nerve palsy using video self-modeling and implementation intentions. Otolaryngol Head Neck Surg. 2006;134(1):48–55.
Lambert-Prou MP. [The temporal smile. Speech therapy for facial palsy patients after temporal lengthening myoplasty]. Rev Stomatol Chir Maxillofac 2003;104(5):274–80.
Winslow CP, Wang TD, Wax MK. Static reanimation of the paralyzed face with an acellular dermal allograft sling. Arch Facial Plast Surg. 2001;3(1):55–7.
Langille M, Singh P. Static facial slings: approaches to rehabilitation of the paralyzed face. Facial Plast Surg Clin North Am. 2016;24(1):29–35.
Rose EH. Autogenous fascia lata grafts: clinical applications in reanimation of the totally or partially paralyzed face. Plast Reconstr Surg. 2005;116(1):20–32; discussion 33–5.
Konior RJ. Facial paralysis reconstruction with Gore-Tex soft-tissue patch. Arch Otolaryngol Head Neck Surg. 1992;118(11):1188–94.
Alam D. Rehabilitation of long-standing facial nerve paralysis with percutaneous suture-based slings. Arch Facial Plast Surg. 2007;9(3):205–9.
Alam DS, et al. Sternohyoid flap for facial reanimation: a comprehensive preclinical evaluation of a novel technique. JAMA Facial Plast Surg. 2013;15(4):305–13.
Manktelow RT. Free muscle transplantation for facial paralysis. Clin Plast Surg. 1984;11(1):215–20.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
David, A.P., Knott, P.D., Seth, R. (2021). Parotidectomy Defect and Facial Nerve Reconstruction. In: Wang, S., Fung, K. (eds) Principles of Lateral Craniofacial Reconstruction. Springer, Cham. https://doi.org/10.1007/978-3-030-50291-1_8
Download citation
DOI: https://doi.org/10.1007/978-3-030-50291-1_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-50290-4
Online ISBN: 978-3-030-50291-1
eBook Packages: MedicineMedicine (R0)