Abstract
Inquiry into fatigue and human performance in the field explore the mechanisms through which performance declines in individuals and groups consequent to fatiguing influences including sleep loss and the circadian timing of sleep. These studies generally examine real-life changes in the industries of transportation and emergency work in order to determine how fatigue is manifested in these environments.
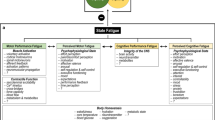
In earlier chapters, definitions and classifications of fatigue have been discussed. This chapter will review ways in which the effects of fatigue, one of the major mediators of which is sleepiness, sleep loss, and inappropriate timing of sleep, have been demonstrated in the field. Concepts of fatigue vary greatly from field to field. In the nursing field, “compassion fatigue” is one of the most prominent areas of research, while “burnout” is caused by work hours alone, and patient volume is a greater focus in research on medical residents and staff.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Akerstedt T, Wright KP Jr. Sleep loss and fatigue in shift work and shift work disorder. Sleep Med Clin. 2009;4:257–71.
Deary IJ, Tait R. Effects of sleep disruption on cognitive performance and mood in medical house officers. Br Med J (Clin Res Ed). 1987;295:1513–6.
Owens J. Medical resident/physician performance. In: Kushida C, editor. Sleep deprivation: clinical issues, pharmacology, and sleep loss effects. Monticello: Marcel Dekker; 2005. p. 335–62.
Rose M, Manser T, Ware JC. Effects of call on sleep and mood in internal medicine residents. Behav Sleep Med. 2008;6:75–88.
Adams EF, Lee AJ, Pritchard CW, White RJ. What stops us from healing the healers: a survey of help-seeking behaviour, stigmatisation and depression within the medical profession. Int J Soc Psychiatry. 2010;56:359–70.
Jewett ME, Wyatt JK, Ritz-De CA, Khalsa SB, Dijk DJ, Czeisler CA. Time course of sleep inertia dissipation in human performance and alertness. J Sleep Res. 1999;8:1–8.
West CP, Tan AD, Habermann TM, Sloan JA, Shanafelt TD. Association of resident fatigue and distress with perceived medical errors. JAMA. 2009;302:1294–300.
McCormick F, Kadzielski J, Landrigan CP, Evans B, Herndon JH, Rubash HE. Surgeon fatigue: a prospective analysis of the incidence, risk, and intervals of predicted fatigue-related impairment in residents. Arch Surg. 2012;147:430–5.
Horne JA. Why we sleep: the functions of sleep in humans and other mammals. Oxford: Oxford University Press; 1988.
Goldman LI, McDonough MT, Rosemond GP. Stresses affecting surgical performance and learning. I. Correlation of heart rate, electrocardiogram, and operation simultaneously recorded on videotapes. J Surg Res. 1972;12:83–6.
Taffinder NJ, McManus IC, Gul Y, Russell RC, Darzi A. Effect of sleep deprivation on surgeons’ dexterity on laparoscopy simulator. Lancet. 1998;352:1191.
Samkoff JS, Jacques CH. A review of studies concerning effects of sleep deprivation and fatigue on residents’ performance. Acad Med. 1991;66:687–93.
Marcus CL, Loughlin GM. Effect of sleep deprivation on driving safety in housestaff. Sleep. 1996;19:763–6.
Hawkins MR, Vichick DA, Silsby HD, Kruzich DJ, Butler R. Sleep and nutritional deprivation and performance of house officers. J Med Educ. 1985;60:530–5.
Sawyer RG, Tribble CG, Newberg DS, Pruett TL, Minasi JS. Intern call schedules and their relationship to sleep, operating room participation, stress, and satisfaction. Surgery. 1999;126:337–42.
Arnedt JT, Owens J, Crouch M, Stahl J, Carskadon MA. Neurobehavioral performance of residents after heavy night call vs after alcohol ingestion. JAMA. 2005;294:1025–33.
Barger LK, Ayas NT, Cade BE, et al. Impact of extended-duration shifts on medical errors, adverse events, and attentional failures. PLoS Med. 2006;3:e487.
McCall TB. The impact of long working hours on resident physicians. N Engl J Med. 1988;318:775–8.
Poulton EC, Hunt GM, Carpenter A, Edwards RS. The performance of junior hospital doctors following reduced sleep and long hours of work. Ergonomics. 1978;21:279–95.
Wilkinson RT. After effect of sleep deprivation. J Exp Psychol. 1990;66:439–42.
Richardson GS, Wyatt JK, Sullivan JP, et al. Objective assessment of sleep and alertness in medical house staff and the impact of protected time for sleep. Sleep. 1996;19:718–26.
Friedman RC, Bigger JT, Kornfeld DS. The intern and sleep loss. N Engl J Med. 1971;285:201–3.
Hart RP, Buchsbaum DG, Wade JB, Hamer RM, Kwentus JA. Effect of sleep deprivation on first-year residents’ response times, memory, and mood. J Med Educ. 1987;62:940–2.
Lingenfelser T, Kaschel R, Weber A, Zaiser-Kaschel H, Jakober B, Kuper J. Young hospital doctors after night duty: their task-specific cognitive status and emotional condition. Med Educ. 1994;28:566–72.
Malmberg B, Kecklund G, Karlson B, Persson R, Flisberg P, Orbaek P. Sleep and recovery in physicians on night call: a longitudinal field study. BMC Health Serv Res. 2010;10:239.
Schwartz AJ, Black ER, Goldstein MG, Jozefowicz RF, Emmings FG. Levels and causes of stress among residents. J Med Educ. 1987;62:744–53.
Owens JA. Sleep loss and fatigue in healthcare professionals. J Perinat Neonatal Nurs. 2007;21:92–100.
Gold DR, Rogacz S, Bock N, et al. Rotating shift work, sleep, and accidents related to sleepiness in hospital nurses. Am J Public Health. 1992;82:1011–4.
Rogers DJ, Stark MM. Think drink, think drugs, think overdoses. J Clin Forensic Med. 1998;5:147–9.
Saleh AM, Awadalla NJ, El-masri YM, Sleem WF. Impacts of nurses’ circadian rhythm sleep disorders, fatigue, and depression on medication administration errors. Egypt J Chest Dis Tuberc. 2013;63:145–53.
Ramirez AJ, Graham J, Richards MA, et al. Burnout and psychiatric disorder among cancer clinicians. Br J Cancer. 1995;71:1263–9.
Smart D, English A, James J, et al. Compassion fatigue and satisfaction: a cross-sectional survey among US healthcare workers. Nurs Health Sci. 2013;16(1):3–10.
Webb JR, Valasek MA, North CS. Prevalence of stimulant use in a sample of US medical students. Ann Clin Psychiatry. 2013;25:27–32.
Hughes PH, Brandenburg N, Baldwin DC Jr, et al. Prevalence of substance use among US physicians. JAMA. 1992;267:2333–9.
Van Dongen HP, Maislin G, Mullington JM, Dinges DF. The cumulative cost of additional wakefulness: dose-response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation. Sleep. 2003;26:117–26.
Sexton JB, Thomas EJ, Helmreich RL. Error, stress, and teamwork in medicine and aviation: cross sectional surveys. BMJ. 2000;320:745–9.
Bushey D, Tononi G, Cirelli C. Sleep and synaptic homeostasis: structural evidence in Drosophila. Science. 2011;332:1576–81.
Kuerer HM, Eberlein TJ, Pollock RE, et al. Career satisfaction, practice patterns and burnout among surgical oncologists: report on the quality of life of members of the Society of Surgical Oncology. Ann Surg Oncol. 2007;14:3043–53.
Levine AC, Adusumilli J, Landrigan CP. Effects of reducing or eliminating resident work shifts over 16 hours: a systematic review. Sleep. 2010;33:1043–53.
Landrigan CP, Czeisler CA, Barger LK, Ayas NT, Rothschild JM, Lockley SW. Effective implementation of work-hour limits and systemic improvements. Jt Comm J Qual Patient Saf. 2007;33:19–29.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer Science+Business Media, LLC, part of Springer Nature
About this chapter
Cite this chapter
Rose, M. (2018). Studies of Fatigue and Human Performance in the Field. In: Sharafkhaneh, A., Hirshkowitz, M. (eds) Fatigue Management. Springer, New York, NY. https://doi.org/10.1007/978-1-4939-8607-1_4
Download citation
DOI: https://doi.org/10.1007/978-1-4939-8607-1_4
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4939-8605-7
Online ISBN: 978-1-4939-8607-1
eBook Packages: MedicineMedicine (R0)