Abstract
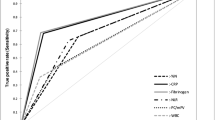
Periprosthetic infections following total knee arthroplasty (TKA) are diagnostically challenging. We evaluated the sensitivity and specificity of ESR and CRP, false negative rates, whether false negative rates differed between early post-operative and late infections, and the predictive ability of ESR and CRP to differentiate infected patients. Between 2000 and 2007, a prospectively collected database was reviewed to identify patients with suspected periprosthetic infections, and who had ESR and CRP laboratory values. One hundred and thirteen patients were identified. False negative rates were calculated. Finally, receiver operating characteristic curves were used to determine the predictive ability of ESR and CRP to differentiate infected from non-infected patients. CRP had a sensitivity of 95% and specificity of 20%. ESR had a sensitivity of 91% and a specificity of 33%. The false negative rate was 9.2% for ESR, 5.3% for CRP, and 11.1% for combined ESR and CRP. False negative rates were higher for early post-operative infections. Although ESR and CRP can be excellent adjunctive diagnostic tools, we emphasise that because some patients may not mount a sufficient immune response, the entire clinical picture must be evaluated, and periprosthetic infection should not be ruled out on the basis of ESR and CRP results alone.


Similar content being viewed by others
References
Peersman G, Laskin R, Davis J, Peterson M (2001) Infection in total knee replacement: a retrospective review of 6489 total knee replacements. Clin Orthop Relat Res 392:15–23
Kurtz S, Ong K, Lau E, Bozic K, Berry D, Parvizi J (2010) Prosthetic joint infection risk after TKA in the medicare population. Clin Orthop Relat Res 468:52–56
Austin M, Ghanem E, Joshi A, Lindsay A, Parvizi J (2008) A simple cost-effective screening protocol to rule-out periprosthetic infection. J Arthroplasty 23(1):65–68
Bare J, MacDonald SJ, Bourne RB (2006) Preoperative evaluations in revision total knee arthroplasty. Clin Orthop Relat Res 446:40–44
Blom A, Brown J, Taylor A, Pattison G, Whitehouse S, Bannister G (2004) Infection after total knee arthroplasty. J Bone Joint Surg Br 86-B(5):688–691
Ghanem E, Azzam K, Seeley M, Joshi A, Parvizi J (2009) Staged revision for knee arthroplasty infection. Clin Orthop Relat Res 467:1699–1705
Insall J, Thompson F, Brause B (1983) Two-stage reimplantation for the salvage of infected total knee arthroplasty. J Bone Joint Surg Am 65:1087–1098
Larsson S, Thelander U, Friberg S (1992) C-reactive protein (CRP) levels after elective orthopedic surgery. Clin Orthop Relat Res 275:237–242
Lentino J (2003) Prosthetic joint infections: bane of orthopaedists, challenge for infectious disease specialists. Clin Infec Dis 36(1):1157–1161
Leone J, Hanssen A (2005) Management of infection at the site of a total knee arthroplasty. J Bone Joint Surg Am 87:2335–2348
Parvizi J, Ghanem E, Sharkey P, Aggarwal A, Burnett S, Barrack R (2008) Diagnosis of infected total knee. Clin Orthop Relat Res 466(11):2628–2633
Sanzen L, Carlsson A (1989) The diagnostic value of C-reactive protein in infected total hip arthroplasties. J Bone Joint Surg Br 71-B(4):638–641
White J, Kelly M, Dunsmuir R (1998) C-reactive protein level after total hip and total knee replacement. J Bone Joint Surg Br 80-B(5):909–911
Bauer T, Parvizi J, Kobayashi N, Krebs V (2006) Diagnosis of periprosthetic infection. J Bone JOint Surg Am 88-A(4):869–882
Parvizi J, Ghanem E, Menashe S, Barrack R, Bauer T (2006) Periprosthetic infection: what are the diagnostic challenges. J Bone Joint Surg Am 88:138–147
Spangehl M, Masri B, O'Connell J, Duncan C (1999) Prospective analysis of preoperative and intraoperative investigations for the diagnosis of infection at the sites of two hundred and two revision total hip arthroplasties. J Bone Joint Surg Am 81:672–683
Ghanem E, Parvizi J, Burnett RS, Sharkey PF, Keshavarzi N, Aggarwal A, Barrack RL (2008) Cell count and differential of aspirated fluid in the diagnosis of infection at the site of total knee arthroplasty. J Bone Joint Surg Am 90(8):1637–1643. doi:10.2106/JBJS.G.00470
Schinsky MF, Della Valle CJ, Sporer SM, Paprosky WG (2008) Perioperative testing for joint infection in patients undergoing revision total hip arthroplasty. J Bone Joint Surg Am 90(9):1869–1875. doi:10.2106/JBJS.G.01255
Ghanem E, Antoci V, Pulido L, Joshi A, Hozack W, Parvizi J (2009) The use of receiver operating characteristics analysis in determining erythrocyte sedimentation rate and C-reactive protein levels in diagnosing periprosthetic infection prior to revision total hip arthroplasty. Int J Infect Dis 13:e444–e449
Conflict of interest statement
M.A.M. is a consultant for Stryker Orthopaedics and Wright Medical Technologies, and receives royalties from Stryker Orthopaedics. The remaining authors have no disclosures to make. No external funding was received specifically in support of this work.
Author information
Authors and Affiliations
Corresponding author
Additional information
Ethical board review
This study has received a waiver from an appropriate ethics committee. All patients gave their informed consent before inclusion in this study.
Rights and permissions
About this article
Cite this article
Johnson, A.J., Zywiel, M.G., Stroh, A. et al. Serological markers can lead to false negative diagnoses of periprosthetic infections following total knee arthroplasty. International Orthopaedics (SICOT) 35, 1621–1626 (2011). https://doi.org/10.1007/s00264-010-1175-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-010-1175-5