Abstract
Background
Ultrasound (US) is the preferred imaging modality for evaluating suspected pediatric appendicitis. However, borderline appendiceal enlargement or questionable inflammatory changes can confound interpretation and lead to equivocal exams.
Objective
The purpose of this study was to determine which findings on equivocal US exams are most predictive of appendicitis.
Materials and methods
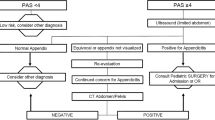
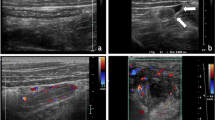
All US exams performed for suspected pediatric appendicitis from July 1, 2013, through July 9, 2014, were initially interpreted using a risk-stratified scoring system. Two blinded pediatric radiologists independently reviewed US exams designated as equivocal and recorded the following findings: increased wall thickness, loss of mural stratification, peri-appendiceal fat inflammation, peri-appendiceal fluid, appendicolith and maximum appendiceal diameter. A third pediatric radiologist resolved discrepancies. US features were correlated with the final diagnosis via multivariate analysis.
Results
During the study period, 162/3,750 (4.3%) children had US exams initially interpreted as equivocal (mean age 9.8 +/- 3.8 years). Five outpatients were lost to follow-up. Forty-eight of the remaining 157 (30.6%) children had an operative diagnosis of appendicitis. Findings significantly associated with appendicitis were loss of mural stratification (odds ratio [OR] = 6.7, P=0.035), peri-appendiceal fat inflammation (OR = 10.0, P<0.0001) and appendicolith (OR = 15.8, P=0.025). While appendiceal diameter tended to be larger in patients with appendicitis, the difference was not statistically significant.
Conclusion
Loss of mural stratification, peri-appendiceal fat inflammation and an appendicolith are significant predictors of appendicitis in children with otherwise equivocal US exams. While maximum appendiceal diameter is not statistically associated with appendicitis in our study, mean appendiceal diameter of 6.7 mm in those without appendicitis suggests that the customary upper normal limit of 6 mm is too sensitive.




Similar content being viewed by others
References
Linam LE, Munden M (2012) Sonography as the first line of evaluation in children with suspected acute appendicitis. J Ultrasound Med 31:1153–1157
Smith MP, Katz DS, Lalani T et al (2014) ACR appropriateness criteria(R) right lower quadrant pain-suspected appendicitis. Ultrasound Q 31:85–91
Trout AT, Sanchez R, Ladino-Torres MF et al (2012) A critical evaluation of US for the diagnosis of pediatric acute appendicitis in a real-life setting: how can we improve the diagnostic value of sonography? Pediatr Radiol 42:813–823
Mittal MK, Dayan PS, Macias CG et al (2013) Performance of ultrasound in the diagnosis of appendicitis in children in a multicenter cohort. Acad Emerg Med 20:697–702
Emil S, Mikhail P, Laberge JM et al (2001) Clinical versus sonographic evaluation of acute appendicitis in children: a comparison of patient characteristics and outcomes. J Pediatr Surg 36:780–783
Kaiser S, Jorulf H, Soderman E et al (2004) Impact of radiologic imaging on the surgical decision-making process in suspected appendicitis in children. Acad Radiol 11:971–979
Koo HS, Kim HC, Yang DM et al (2013) Does computed tomography have any additional value after sonography in patients with suspected acute appendicitis? J Ultrasound Med 32:1397–1403
Krishnamoorthi R, Ramarajan N, Wang NE et al (2011) Effectiveness of a staged US and CT protocol for the diagnosis of pediatric appendicitis: reducing radiation exposure in the age of ALARA. Radiology 259:231–239
Thirumoorthi AS, Fefferman NR, Ginsburg HB et al (2012) Managing radiation exposure in children — reexamining the role of ultrasound in the diagnosis of appendicitis. J Pediatr Surg 47:2268–2272
Herliczek TW, Swenson DW, Mayo-Smith WW (2013) Utility of MRI after inconclusive ultrasound in pediatric patients with suspected appendicitis: retrospective review of 60 consecutive patients. AJR Am J Roentgenol 200:969–973
Orth RC, Guillerman RP, Zhang W et al (2014) Prospective comparison of MR imaging and US for the diagnosis of pediatric appendicitis. Radiology 272:233–240
Fallon SC, Orth RC, Guillerman RP et al (2015) Development and validation of an ultrasound scoring system for children with suspected acute appendicitis. Pediatr Radiol 45:1945–1952
Fallon SC, Kim ME, Hallmark CA et al (2015) Correlating surgical and pathological diagnoses in pediatric appendicitis. J Pediatr Surg 50:638–641
Correa J, Jimeno J, Vallverdu H et al (2015) Correlation between intraoperative surgical diagnosis of complicated acute appendicitis and the pathology report: clinical implications. Surg Infect 16:41–44
Wiersma F, Toorenvliet BR, Bloem JL et al (2009) US examination of the appendix in children with suspected appendicitis: the additional value of secondary signs. Eur Radiol 19:455–461
Blumfield E, Nayak G, Srinivasan R et al (2013) Ultrasound for differentiation between perforated and nonperforated appendicitis in pediatric patients. AJR Am J Roentgenol 200:957–962
Stewart JK, Olcott EW, Jeffrey BR (2012) Sonography for appendicitis: nonvisualization of the appendix is an indication for active clinical observation rather than direct referral for computed tomography. J Clin Ultrasound 40:455–461
Trout AT, Sanchez R, Ladino-Torres MF (2012) Reevaluating the sonographic criteria for acute appendicitis in children: a review of the literature and a retrospective analysis of 246 cases. Acad Radiol 19:1382–1394
Estey A, Poonai N, Lim R (2013) Appendix not seen: the predictive value of secondary inflammatory sonographic signs. Pediatr Emerg Care 29:435–439
Jeffrey RB Jr, Laing FC, Townsend RR (1988) Acute appendicitis: sonographic criteria based on 250 cases. Radiology 167:327–329
Puylaert JB (1986) Acute appendicitis: US evaluation using graded compression. Radiology 158:355–360
Goldin AB, Khanna P, Thapa M et al (2011) Revised ultrasound criteria for appendicitis in children improve diagnostic accuracy. Pediatr Radiol 41:993–999
Trout AT, Towbin AJ, Fierke SR et al (2015) Appendiceal diameter as a predictor of appendicitis in children: improved diagnosis with three diagnostic categories derived from a logistic predictive model. Eur Radiol 25:2231–2238
Bliss D, McKee J, Cho D et al (2010) Discordance of the pediatric surgeon’s intraoperative assessment of pediatric appendicitis with the pathologists report. J Pediatr Surg 45:1398–1403
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Dr. Orth received salary support through the Association of University Radiologists General Electric Radiology Research Academic Fellowship Award.
Rights and permissions
About this article
Cite this article
Telesmanich, M.E., Orth, R.C., Zhang, W. et al. Searching for certainty: findings predictive of appendicitis in equivocal ultrasound exams. Pediatr Radiol 46, 1539–1545 (2016). https://doi.org/10.1007/s00247-016-3645-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-016-3645-4