Abstract
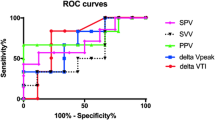
Continuous noninvasive cardiac output monitoring (NICOM) is a clinically useful tool in the pediatric setting. This study compared the ability of stroke volume variation (SVV) measured by NICOM with that of respiratory variations in the velocity of aortic blood flow (△Vpeak) and central venous pressure (CVP) to predict of fluid responsiveness in mechanically ventilated children after ventricular septal defect repair. The study investigated 26 mechanically ventilated children after the completion of surgery. At 30 min after their arrival in an intensive care unit, a colloid solution of 10 ml/kg was administrated for volume expansion. Hemodynamic variables, including CVP, stroke volume, and △Vpeak in addition to cardiac output and SVV in NICOM were measured before and 10 min after volume expansion. The patients with a stroke volume increase of more than 15 % after volume expansion were defined as responders. The 26 patients in the study consisted of 13 responders and 13 nonresponders. Before volume expansion, △Vpeak and SVV were higher in the responders (both p values <0.001). The areas under the receiver operating characteristic curves of △Vpeak, SVV, and CVP were respectively 0.956 (95 % CI 0.885–1.00), 0.888 (95 % CI 0.764–1.00), and 0.331 (95 % CI 0.123–0.540). This study showed that SVV by NICOM and △Vpeak by echocardiography, but not CVP, reliably predicted fluid responsiveness during mechanical ventilation after ventricular septal defect repair in children.


Similar content being viewed by others
References
Ballestero Y, López-Herce J, Urbano J et al (2011) Measurement of cardiac output in children by bioreactance. Pediatr Cardiol 32:469–472
Choi DY, Kwak HJ, Park HY, Kim YB, Choi CH, Lee JY (2010) Respiratory variation in aortic blood flow velocity as a predictor of fluid responsiveness in children after repair of ventricular septal defect. Pediatr Cardiol 31:1166–1170
Chung E, Cannesson M (2012) Using noninvasive dynamic parameters of fluid responsiveness in children: there is still much to learn. J Clin Monit Comput 26:153–155
Conway DH, Hussain OA, Gall I (2013) A comparison of noninvasive bioreactance with oesophageal Doppler estimation of stroke volume during open abdominal surgery: an observational study. Eur J Anaesthesiol 30:501–508
de Souza Pereira, Neto E, Grousson S, Duflo F et al (2011) Predicting fluid responsiveness in mechanically ventilated children under general anaesthesia using dynamic parameters and transthoracic echocardiography. Br J Anaesth 106:856–864
Durand P, Chevret L, Essouri S, Haas V, Devictor D (2008) Respiratory variations in aortic blood flow predict fluid responsiveness in ventilated children. Intensive Care Med 34:888–894
Fagnoul D, Vincent JL, Backer DD (2012) Cardiac output measurements using the bioreactance technique in critically ill patients. Crit Care 16:460
Hanley JA, McNeil BJ (1982) The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 143:29–36
Keren H, Burkhoff D, Squara P (2007) Evaluation of a noninvasive continuous cardiac output monitoring system based on thoracic bioreactance. Am J Physiol Heart Circ Physiol 293:H583–H589
Lafanechère A, Albaladejo P, Raux M et al (2006) Cardiac output measurement during infrarenal aortic surgery: echo-esophageal Doppler versus thermodilution catheter. J Cardiothorac Vasc Anesth 20:26–30
Loupec T, Nanadoumgar H, Frasca D et al (2011) Pleth variability index predicts fluid responsiveness in critically ill patients. Crit Care Med 39:294–299
Marik PE, Baram M, Vahid B (2008) Does central venous pressure predict fluid responsiveness? A systematic review of the literature and the tale of seven mares. Chest 134:172–178
Marik PE, Cavallazzi R, Vasu T, Hirani A (2009) Dynamic changes in arterial waveform derived variables and fluid responsiveness in mechanically ventilated patients: a systematic review of the literature. Crit Care Med 37:2642–2647
Obuchowski NA, McClish DK (1997) Sample size determination for diagnostic accuracy studies involving binormal ROC curve indices. Stat Med 16:1529–1542
Renner J, Gruenewald M, Meybohm P et al (2008) Effect of elevated PEEP on dynamic variables of fluid responsiveness in a pediatric animal model. Paediatr Anaesth 18:1170–1177
Renner J, Cavus E, Meybohm P et al (2008) Pulse pressure variation and stroke volume variation during different loading conditions in a paediatric animal model. Acta Anaesthesiol Scand 52:374–380
Renner J, Broch O, Gruenewald M et al (2011) Noninvasive prediction of fluid responsiveness in infants using Pleth variability index. Anaesthesia 66:582–589
Renner J, Broch O, Duetschke P et al (2012) Prediction of fluid responsiveness in infants and neonates undergoing congenital heart surgery. Br J Anaesth 108:108–115
Squara P, Denjean D, Estagnasie P, Brusset A, Dib JC, Dubois C (2007) Noninvasive cardiac output monitoring (NICOM): a clinical validation. Intensive Care Med 33:1191–1194
Vistisen ST, Koefoed-Nielsen J, Larsson A (2010) Should dynamic parameters for prediction of fluid responsiveness be indexed to the tidal volume? Acta Anaesthesiol Scand 54:191–198
Weisz DE, Jain A, McNamara PJ, EL-Khuffash A (2012) Noninvasive cardiac output monitoring in neonates using bioreactance: a comparison with echocardiography. Neonatology 102:61–67
Acknowledgments
This study protocol was approved by the institutional review board of Gil Medical Center, Gachon University (IRB No. GIRBA 2738-2012).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, J.Y., Kim, J.Y., Choi, C.H. et al. The Ability of Stroke Volume Variation Measured by a Noninvasive Cardiac Output Monitor to Predict Fluid Responsiveness in Mechanically Ventilated Children. Pediatr Cardiol 35, 289–294 (2014). https://doi.org/10.1007/s00246-013-0772-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-013-0772-7