Abstract
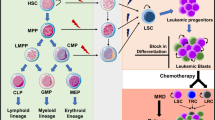
Accumulating evidence indicates that the interaction of human LSCs (leukemic stem cells) with the hematopoietic microenvironment, mediated by the thrombopoietin (TPO)/c-MPL pathway, may be an underlying mechanism for resistance to cell cycle–dependent cytotoxic chemotherapy. However, the role of TPO/c-MPL signaling in AML (acute myelogenous leukemia) chemotherapy resistance hasn’t been fully understood. The c-MPL and TPO levels in different AML samples were measured by flow cytometry and ELISA. We also assessed the TPO levels in the osteoblasts derived from bone mesenchymal stem cells (BMSCs). The survival rate of an AML cell line that had been co-cultured with different BMSC-derived osteoblasts was measured to determine the IC50 of an AML chemotherapy drug daunorubicin (DNR). The levels of TPO/c-MPL in the initial and relapse AML patients were significantly higher than that in the control (P < 0.05). The osteoblasts derived from AML patients’ BMSCs secreted more TPO than the osteoblasts derived from normal control BMSCs (P < 0.05). A strong positive correlation between the TPO level and c-MPL expression was found in the bone marrow mononuclear cells of the relapse AML patients. More importantly, the IC50 of DNR in the HEL + AML-derived osteoblasts was the highest among all co-culture systems. High level of TPO/c-MPL signaling may protect LSCs from chemotherapy in AML. The effects of inhibition of the TPO/c-MPL pathway on enhancing the chemotherapy sensitivity of AML cells, and on their downstream effector molecules that direct the interactions between patient-derived blasts and leukemia repopulating cells need to be further studied.






Similar content being viewed by others
References
She M, Niu X, Chen X, Li J, Zhou M, He Y, Le Y, Guo K (2012) Resistance of leukemic stem-like cells in AML cell line KG1a to natural killer cell-mediated cytotoxicity. Cancer Lett 318(2):173–179. doi:10.1016/j.canlet.2011.12.017
Nervi B, Ramirez P, Rettig MP, Uy GL, Holt MS, Ritchey JK, Prior JL, Piwnica-Worms D, Bridger G, Ley TJ, DiPersio JF (2009) Chemosensitization of acute myeloid leukemia (AML) following mobilization by the CXCR4 antagonist AMD3100. Blood 113(24):6206–6214. doi:10.1182/blood-2008-06-162123
Saito Y, Kitamura H, Hijikata A, Tomizawa-Murasawa M, Tanaka S, Takagi S, Uchida N, Suzuki N, Sone A, Najima Y, Ozawa H, Wake A, Taniguchi S, Shultz LD, Ohara O, Ishikawa F (2010) Identification of therapeutic targets for quiescent, chemotherapy-resistant human leukemia stem cells. Sci Transl Med 2(17):17ra19. doi:10.1126/scitranslmed.3000349
Lane SW, Scadden DT, Gilliland DG (2009) The leukemic stem cell niche: current concepts and therapeutic opportunities. Blood 114(6):1150–1157. doi:10.1182/blood-2009-01-202606
Blanco TM, Mantalaris A, Bismarck A, Panoskaltsis N (2010) The development of a three-dimensional scaffold for ex vivo biomimicry of human acute myeloid leukaemia. Biomaterials 31(8):2243–2251. doi:10.1016/j.biomaterials.2009.11.094
Ishikawa FYS, Saito Y, Hijikata A, Kitamura H, Tanaka S, Nakamura R, Tanaka T, Tomiyama H, Saito N, Fukata M, Miyamoto T, Lyons B, Ohshima K, Uchida N, Taniguchi S, Ohara O, Akashi K, Harada M, Shultz LD (2007) Chemotherapy-resistant human AML stem cells home to and engraft within the bone-marrow endosteal region. Nat Biotechnol 25:1315–1321
Zeng Z, Shi YX, Samudio IJ, Wang RY, Ling X, Frolova O, Levis M, Rubin JB, Negrin RR, Estey EH, Konoplev S, Andreeff M, Konopleva M (2009) Targeting the leukemia microenvironment by CXCR4 inhibition overcomes resistance to kinase inhibitors and chemotherapy in AML. Blood 113(24):6215–6224. doi:10.1182/blood-2008-05-158311
Jawad MSC, Mony U, Grundy M, Russell NH, Pallis M (2010) Analysis of factors that affect in vitro chemosensitivity of leukaemic stem and progenitor cells to gemtuzumab ozogamicin (Mylotarg) in acute myeloid leukaemia. Leukemia 24:74–80
Parmar A, Marz S, Rushton S, Holzwarth C, Lind K, Kayser S, Dohner K, Peschel C, Oostendorp RA, Gotze KS (2011) Stromal niche cells protect early leukemic FLT3-ITD+ progenitor cells against first-generation FLT3 tyrosine kinase inhibitors. Cancer Res 71(13):4696–4706. doi:10.1158/0008-5472.CAN-10-4136
Lane SW, Wang YJ, Lo Celso C, Ragu C, Bullinger L, Sykes SM, Ferraro F, Shterental S, Lin CP, Gilliland DG, Scadden DT, Armstrong SA, Williams DA (2011) Differential niche and Wnt requirements during acute myeloid leukemia progression. Blood 118(10):2849–2856. doi:10.1182/blood-2011-03-345165
Guo YBS, Luo M (1999) Study of thrombopoietin and its recptor in the acute myeloid leukemia. Zhonghua Xue Ye Xue Za Zhi 20:120–123
Schroder JK, Kolkenbrock S, Tins J, Kasimir-Bauer S, Seeber S, Schutte J (2000) Analysis of thrombopoietin receptor (c-mpl) mRNA expression in de novo acute myeloid leukemia. Leuk Res 24(5):401–409
Li L, Xie T (2005) Stem cell niche: structure and function. Annu Rev Cell Dev Biol 21:605–631. doi:10.1146/annurev.cellbio.21.012704.131525
Adams GB, Scadden DT (2006) The hematopoietic stem cell in its place. Nat Immunol 7(4):333–337
LE Wilson A, Trumpp A (2009) Balancing dormant and self-renewing hematopoietic stem cells. Curr Opin Genet Dev 19:461–468
Yoshihara HAF, Hosokawa K, Hagiwara T, Takubo K, Nakamura Y, Gomei Y, Iwasaki H, Matsuoka S, Miyamoto K, Miyazaki H, Takahashi T, Suda T (2007) Thrombopoietin/MPL signaling regulates hematopoietic stem cell quiescence and interaction with the osteoblastic niche. Cell Stem Cell 1:685–697
Matsumura IKY, Kato T, Ikeda H, Ishikawa J, Horikawa Y, Hashimoto K, Moriyama Y, Tsujimura T, Nishiura T (2005) Growth response of acute myeloblastic leukemia cells to recombinant human thrombopoietin. Blood 86:703–709
Corazza FHC, D’Hondt S, Ferster A, Kentos A, Benoît Y, Sariban E (2006) Circulating thrombopoietin as an in vivo growth factor for blast cells in acute myeloid leukemia. Blood 107:2525–2530
Kaushansky K (2005) The molecular mechanisms that control thrombopoiesis. J Clin Invest 115:3339–3347
Sitnicka E, Lin N, Priestley GV, Fox N, Broudy VC, Wolf NS, Kaushansky K (1996) The effect of thrombopoietin on the proliferation and differentiation of murine hematopoietic stem cells. Blood 87(12):4998–5005
Ku H, Yonemura Y, Kaushansky K, Ogawa M (1996) Thrombopoietin, the ligand for the Mpl receptor, synergizes with steel factor and other early acting cytokines in supporting proliferation of primitive hematopoietic progenitors of mice. Blood 87(11):4544–4551
Fox N, Priestley G, Papayannopoulou T, Kaushansky K (2002) Thrombopoietin expands hematopoietic stem cells after transplantation. J Clin Invest 110(3):389–394. doi:10.1172/JCI15430
Wu YX, Wang HY, Wang W (2010) Measurement and clinical significance of serum TPO and LDH levels in patients with myelodysplastic syndrome and acute leukemia. Zhongguo Shi Yan Xue Ye Xue Za Zhi 18(3):671–674
Wetzler MBM, Bernstein SH, Blumenson L, Stewart C, Barcos M, Mrózek K, Block AW, Herzig GP, Bloomfield CD (1997) Expression of c-mpl mRNA, the receptor for thrombopoietin, in acute myeloid leukemia blasts identifies a group of patients with poor response to intensie chemotherapy. Clin Oncol 15:2262–2268
Arai F, Yoshihara H, Hosokawa K, Nakamura Y, Gomei Y, Iwasaki H, Suda T (2009) Niche regulation of hematopoietic stem cells in the endosteum. Ann N Y Acad Sci 1176:36–46. doi:10.1111/j.1749-6632.2009.04561.x
Acknowledgments
The study was funded by grants from Military Natural Science foundation of China (06-MB238), Natural Science fund of Chongqing (2009BB5151) and National Natural Science Foundation of China (81000195).
Conflict of Interest
All authors have no conflict of interest to state.
Author information
Authors and Affiliations
Corresponding author
Additional information
Zeng Dong-Feng and Zhang Yong should be regard as the co-first author.
Rights and permissions
About this article
Cite this article
Dong-Feng, Z., Ting, L., Yong, Z. et al. The TPO/c-MPL Pathway in the Bone Marrow may Protect Leukemia Cells from Chemotherapy in AML Patients. Pathol. Oncol. Res. 20, 309–317 (2014). https://doi.org/10.1007/s12253-013-9696-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12253-013-9696-z