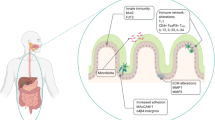
Abstract
Recently, conventional therapies for inflammatory bowel disease (IBD) have not received the same amount of attention as biologic therapies, yet they remain the backbone of therapy for IBD because of their efficacy, safety, and relatively low cost. Advances in efficacy and safety continue because of modifications in drug dosing and monitoring. Higher doses of mesalamine per pill, together with once-daily dosing, may help to optimize drug delivery and patient compliance. Budesonide, an effective agent for both induction and short-term remission maintenance in Crohn’s disease, is devoid of many of the toxicities common to corticosteroids. Assessments of thiopurine methyltransferase and metabolite levels are helping to fine-tune dose optimization for the thiopurines azathioprine and 6-mercaptopurine. The oral calcineurin inhibitors tacrolimus and cyclosporine have been shown to have expanded roles in IBD, and methotrexate may be useful in some patients with refractory ulcerative colitis. Probiotics are showing promise for maintenance of remission in Crohn’s disease, ulcerative colitis, and pouchitis.
Similar content being viewed by others
References and Recommended Reading
Kozuch PL, Hanauer SB: Treatment of inflammatory bowel disease: a review of medical therapy. World J Gastroenterol 2008, 14:354–377.
Kornbluth A, Sachar DB: Ulcerative colitis practice guidelines in adults (update): American College of Gastroenterology, Practice Parameters Committee. Am J Gastroenterol 2004, 99:1371–1385.
Regueiro M, Loftus EV Jr, Steinhart AH, Cohen RD: Medical management of left-sided ulcerative colitis and ulcerative proctitis: critical evaluation of therapeutic trials. Inflamm Bowel Dis 2006, 12:979–994.
Regueiro M, Loftus EV Jr, Steinhart AH, Cohen RD: Clinical guidelines for the medical management of left-sided ulcerative colitis and ulcerative proctitis: summary statement. Inflamm Bowel Dis 2006, 12:972–978.
Hanauer SB, Sandborn WJ, Dallaire C, et al.: Delayed-release oral mesalamine 4.8 g/day (800 mg tablets) compared to 2.4 g/day (400 mg tablets) for the treatment of mildly to moderately active ulcerative colitis: The ASCEND I trial. Can J Gastroenterol 2007, 21:827–834.
Hanauer SB, Sandborn WJ, Kornbluth A, et al.: Delayedrelease oral mesalamine at 4.8 g/day (800 mg tablet) for the treatment of moderately active ulcerative colitis: the ASCEND II trial. Am J Gastroenterol 2005, 100:2478–2485.
Brunner M, Assandri R, Kletter K, et al.: Gastrointestinal transit and 5-ASA release from a new mesalazine extended-release formulation. Aliment Pharmacol Ther 2003, 17:395–402.
Prantera C, Viscido A, Biancone L, et al.: A new oral delivery system for 5-ASA: preliminary clinical findings for MMx. Inflamm Bowel Dis 2005, 11:421–427.
Lichtenstein GR, Kamm MA, Boddu P, et al.: Effect of once-or twice-daily MMX mesalamine (SPD476) for the induction of remission of mild to moderately active ulcerative colitis. Clin Gastroenterol Hepatol 2007, 5:95–102.
Kamm MA, Sandborn WJ, Gassull M, et al.: Once-daily, high-concentration MMX mesalamine in active ulcerative colitis. Gastroenterology 2007, 132:66–75.
Lichtenstein GR, Kamm MA, Sandborn WJ, et al.: MMX mesalazine for the induction of remission of mild-to-moderately active ulcerative colitis: efficacy and tolerability in specific patient subpopulations. Aliment Pharmacol Ther 2008, 27:1094–1102.
Kamm MA, Lichtenstein GR, Sandborn WJ, et al.: Randomised trial of once-or twice-daily MMX mesalazine for maintenance of remission in ulcerative colitis. Gut 2008, 57:893–902.
Lichtenstein GR, Abreu MT, Cohen R, Tremaine W: American Gastroenterological Association Institute technical review on corticosteroids, immunomodulators, and infliximab in inflammatory bowel disease. Gastroenterology 2006, 130:940–987.
Lichtenstein GR, Abreu MT, Cohen R, Tremaine W: American Gastroenterological Association Institute medical position statement on corticosteroids, immunomodulators, and infliximab in inflammatory bowel disease. Gastroenterology 2006, 130:935–939.
Dahlberg E, Thalen A, Brattsand R, et al.: Correlation between chemical structure, receptor binding, and biological activity of some novel, highly active, 16 alpha, 17 alpha-acetal-substituted glucocorticoids. Mol Pharmacol 1984, 25:70–78.
Brattsand R: Overview of newer glucocorticosteroid preparations for inflammatory bowel disease. Can J Gastroenterol 1990, 4:407–414.
Hanauer S, Sandborn WJ, Persson A, Persson T: Budesonide as maintenance treatment in Crohn’s disease: a placebo-controlled trial. Aliment Pharmacol Ther 2005, 21:363–371.
de Jong DJ, Bac DJ, Tan G, et al.: Maintenance treatment with budesonide 6 mg versus 9 mg once daily in patients with Crohn’s disease in remission. Neth J Med 2007, 65:339–345.
Dubinsky MC, Lamothe S, Yang HY, et al.: Pharmacogenomics and metabolite measurement for 6-mercaptopurine therapy in inflammatory bowel disease. Gastroenterology 2000, 118:705–713.
Weinshilboum RM, Sladek SL: Mercaptopurine pharmacogenetics: monogenic inheritance of erythrocyte thiopurine methyltransferase activity. Am J Hum Genet 1980, 32:651–662.
Ganiere-Monteil C, Medard Y, Lejus C, et al.: Phenotype and genotype for thiopurine methyltransferase activity in the French Caucasian population: impact of age. Eur J Clin Pharmacol 2004, 60:89–96.
Rossi AM, Bianchi M, Guarnieri C, et al.: Genotypephenotype correlation for thiopurine S-methyltransferase in healthy Italian subjects. Eur J Clin Pharmacol 2001, 57:51–54.
Morales A, Salguti S, Miao CL, Lewis JD: Relationship between 6-mercaptopurine dose and 6-thioguanine nucleotide levels in patients with inflammatory bowel disease. Inflamm Bowel Dis 2007, 13:380–385.
Sparrow MP, Hande SA, Friedman S, et al.: Effect of allopurinol on clinical outcomes in inflammatory bowel disease nonresponders to azathioprine or 6-mercaptopurine. Clin Gastroenterol Hepatol 2007, 5:209–214.
Gonzalez-Lama Y, Gisbert JP, Mate J: The role of tacrolimus in inflammatory bowel disease: a systematic review. Dig Dis Sci 2006, 51:1833–1840.
Hart AL, Plamondon S, Kamm MA: Topical tacrolimus in the treatment of perianal Crohn’s disease: exploratory randomized controlled trial. Inflamm Bowel Dis 2007, 13:245–253.
Sandborn WJ, Present DH, Isaacs KL, et al.: Tacrolimus for the treatment of fistulas in patients with Crohn’s disease: a randomized, placebo-controlled trial. Gastroenterology 2003, 125:380–388.
Gonzalez-Lama Y, Abreu L, Vera MI, et al.: Long-term oral tacrolimus therapy in refractory to infliximab fistulizing Crohn’s disease: a pilot study. Inflamm Bowel Dis 2005, 11:8–15.
Ogata H, Matsui T, Nakamura M, et al.: A randomised dose finding study of oral tacrolimus (FK506) therapy in refractory ulcerative colitis. Gut 2006, 55:1255–1262.
Baumgart DC, Pintoffl JP, Sturm A, et al.: Tacrolimus is safe and effective in patients with severe steroid-refractory or steroid-dependent inflammatory bowel disease—a longterm follow-up. Am J Gastroenterol 2006, 101:1048–1056.
Ng SC, Arebi N, Kamm MA: Medium-term results of oral tacrolimus treatment in refractory inflammatory bowel disease. Inflamm Bowel Dis 2007, 13:129–134.
Yamamoto S, Nakase H, Mikami S, et al.: Long-term effect of tacrolimus therapy in patients with refractory ulcerative colitis. Aliment Pharmacol Ther 2008, 28:589–597.
Ziring DA, Wu SS, Mow WS, et al.: Oral tacrolimus for steroid-dependent and steroid-resistant ulcerative colitis in children. J Pediatr Gastroenterol Nutr 2007, 45:306–311.
Lichtiger S, Present DH, Kornbluth A, et al.: Cyclosporine in severe ulcerative colitis refractory to steroid therapy. N Engl J Med 1994, 330:1841–1845.
Weber A, Fein F, Koch S, et al.: Treatment of ulcerative colitis refractory to steroid therapy by oral microemulsion cyclosporine (Neoral). Inflamm Bowel Dis 2006, 12:1131–1135.
Cacheux W, Seksik P, Lemann M, et al.: Predictive factors of response to cyclosporine in steroid-refractory ulcerative colitis. Am J Gastroenterol 2008, 103:637–642.
Aceituno M, Garcia-Planella E, Heredia C, et al.: Steroidrefractory ulcerative colitis: predictive factors of response to cyclosporine and validation in an independent cohort. Inflamm Bowel Dis 2008, 14:347–352.
Feagan BG, Fedorak RN, Irvine EJ, et al.: A comparison of methotrexate with placebo for the maintenance of remission in Crohn’s disease. North American Crohn’s Study Group Investigators. N Engl J Med 2000, 342:1627–1632.
Feagan BG, Rochon J, Fedorak RN, et al.: Methotrexate for the treatment of Crohn’s disease. The North American Crohn’s Study Group Investigators. N Engl J Med 1995, 332:292–297.
Cummings JR, Herrlinger KR, Travis SP, et al.: Oral methotrexate in ulcerative colitis. Aliment Pharmacol Ther 2005, 21:385–389.
Ewaschuk JB, Dieleman LA: Probiotics and prebiotics in chronic inflammatory bowel diseases. World J Gastroenterol 2006, 12:5941–5950.
Miele E, Baldassano R, Pascarella F, et al.: Effect of a probiotic preparation (Vsl #3) on induction and maintenance of remission in children with ulcerative colitis [abstract 1013]. Gastroenterology 2008, 134:A–153.
Makharia GK, Sood A, Midha V, et al.: A randomized, doubleblind, placebo-controlled trial of a probiotic preparation, Vsl#3, for the treatment of mild to moderate active ulcerative colitis [abstract 701]. Gastroenterology 2008, 134:A–99.
Madsen K, Backer J, Leddin D, et al.: A randomized controlled trial of Vsl#3 for the prevention of endoscopic recurrence following surgery for Crohn’s disease [abstract M1207]. Gastroenterology 2008, 134:A–361.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schwartz, M., Cohen, R. Optimizing conventional therapy for inflammatory bowel disease. Curr Gastroenterol Rep 10, 585–590 (2008). https://doi.org/10.1007/s11894-008-0106-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11894-008-0106-8