Abstract
Purpose
Positive affect has demonstrated unique benefits in the context of health-related stress and is emerging as an important target for psychosocial interventions. The primary objective of this meta-analysis was to determine whether psychosocial interventions increase positive affect in cancer survivors.
Methods
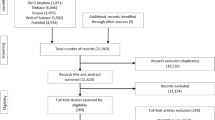
We coded 28 randomized controlled trials of psychosocial interventions assessing 2082 cancer survivors from six electronic databases. We calculated 76 effect sizes for positive affect and conducted synthesis using random effects models with robust variance estimation. Tests for moderation included demographic, clinical, and intervention characteristics.
Results
Interventions had a modest effect on positive affect (g = 0.35, 95% CI [0.16, 0.54]) with substantial heterogeneity of effects across studies (\( \hat{\tau}=0.40 \); I2 = 78%). Three significant moderators were identified: in-person interventions outperformed remote interventions (P = .046), effects were larger when evaluated against standard of care or wait list control conditions versus attentional, educational, or component controls (P = .009), and trials with survivors of early-stage cancer diagnoses yielded larger effects than those with advanced-stage diagnoses (P = .046). We did not detect differential benefits of psychosocial interventions across samples varying in sex, age, on-treatment versus off-treatment status, or cancer type. Although no conclusive evidence suggested outcome reporting biases (P = .370), effects were smaller in studies with lower risk of bias.
Conclusions
In-person interventions with survivors of early-stage cancers hold promise for enhancing positive affect, but more methodological rigor is needed.
Implications for Cancer Survivors
Positive affect strategies can be an explicit target in evidence-based medicine and have a role in patient-centered survivorship care, providing tools to uniquely mobilize human strengths.


Similar content being viewed by others
References
Hart SL, et al. Meta-analysis of efficacy of interventions for elevated depressive symptoms in adults diagnosed with cancer. J Natl Cancer Inst. 2012;104(13):990–1004.
Sheinfeld Gorin S, et al. Meta-analysis of psychosocial interventions to reduce pain in patients with cancer. J Clin Oncol. 2012;30(5):539–47.
Mustian KM, et al. Comparison of pharmaceutical, psychological, and exercise treatments for cancer-related fatigue: a meta-analysis. JAMA Oncol. 2017;3(7):961–8.
Stanton AL. Psychosocial concerns and interventions for cancer survivors. J Clin Oncol. 2006;24(32):5132–7.
Pressman SD, Cohen S. Does positive affect influence health? Psychol Bull. 2005;131(6):925–71.
Fredrickson BL. The role of positive emotions in positive psychology: the broaden-and-build theory of positive emotions. Am Psychol. 2001;56(3):218–26.
Moskowitz JT, Acree M, Epel ES. Positive affect uniquely predicts lower risk of mortality in people with diabetes. Health Psychol. 2008;27(1 Suppl):S73–82.
Moskowitz JT. Positive affect predicts lower risk of AIDS mortality. Psychosom Med. 2003;65(4):620.
Chida Y, Steptoe A. Positive psychological well-being and mortality: a quantitative review of prospective observational studies. Psychosom Med. 2008;70(7):741–56.
Moskowitz JT, et al. Randomized controlled trial of a positive affect intervention for people newly diagnosed with HIV. J Consult Clin Psychol. 2017;85(5):409–23.
Charlson ME, et al. Randomized controlled trials of positive affect and self-affirmation to facilitate healthy behaviors in patients with cardiopulmonary diseases: rationale, trial design, and methods. Contemp Clin Trials. 2007;28(6):748–62.
Ogedegbe GO, et al. A randomized controlled trial of positive-affect intervention and medication adherence in hypertensive African Americans. Arch Intern Med. 2012;172(4):322–6.
Peterson JC, et al. Translating basic behavioral and social science research to clinical application: the EVOLVE mixed methods approach. J Consult Clin Psychol. 2013;81(2):217–30.
Boutin-Foster C, et al. Results from the trial using motivational interviewing, positive affect, and self-affirmation in african americans with hypertension (TRIUMPH). Ethn Dis. 2016;26(1):51–60.
Diener E, Emmons RA. The independence of positive and negative affect. J Pers Soc Psychol. 1984;47(5):1105–17.
Craske MG, et al. Positive affect treatment for depression and anxiety: a randomized clinical trial for a core feature of anhedonia. J Consult Clin Psychol. 2019;87(5):457–71.
Danner DD, Snowdon DA, Friesen WV. Positive emotions in early life and longevity: findings from the nun study. J Pers Soc Psychol. 2001;80(5):804–13.
Fredrickson BL, Levenson RW. Positive emotions speed recovery from the cardiovascular sequelae of negative emotions. Cognit Emot. 1998;12(2):191–220.
Richman LS, et al. Positive emotion and health: going beyond the negative. Health Psychol. 2005;24(4):422–9.
Diener E. Subjective well-being. The science of happiness and a proposal for a national index. Am Psychol. 2000;55(1):34–43.
Koizumi M, et al. Effect of having a sense of purpose in life on the risk of death from cardiovascular diseases. J Epidemiol. 2008;18(5):191–6.
Verduin PJ, et al. Purpose in life in patients with rheumatoid arthritis. Clin Rheumatol. 2008;27(7):899–908.
Mascaro N, Rosen DH. Existential meaning’s role in the enhancement of hope and prevention of depressive symptoms. J Pers. 2005;73(4):985–1013.
Stauber S, et al. Health-related quality of life is associated with positive affect in patients with coronary heart disease entering cardiac rehabilitation. J Clin Psychol Med Settings. 2013;20(1):79–87.
Eaton RJ, Bradley G, Morrissey S. Positive predispositions, quality of life and chronic illness. Psychol Health Med. 2014;19(4):473–89.
Sharma A, et al. Patient personality predicts postoperative stay after colorectal cancer resection. Color Dis. 2008;10(2):151–6.
Bruce J, et al. Psychological, surgical, and sociodemographic predictors of pain outcomes after breast cancer surgery: a population-based cohort study. Pain. 2014;155(2):232–43.
Voogt E, et al. Positive and negative affect after diagnosis of advanced cancer. Psycho-Oncology. 2005;14(4):262–73.
Ritterband LM, Spielberger CD. Depression in a cancer patient population. J Clin Psychol Med Settings. 2001;8(2):85–93.
Hou WK, Law CC, Fu YT. Does change in positive affect mediate and/or moderate the impact of symptom distress on psychological adjustment after cancer diagnosis? A prospective analysis. Psychol Health. 2010;25(4):417–31.
Salsman J, et al. Development and validation of the positive affect and well-being scale for the neurology quality of life (Neuro-QOL) measurement system. Qual Life Res. 2013;22(9):2569–80.
Calhoun LG, Tedeschi RG. Handbook of posttraumatic growth: research and practice. Routledge; 2014.
Rasmussen H, Scheier M, Greenhouse J. Optimism and physical health: a meta-analytic review. Ann Behav Med. 2009;37(3):239–56.
Howell RT, Kern ML, Lyubomirsky S. Health benefits: meta-analytically determining the impact of well-being on objective health outcomes. Health Psychol Rev. 2007;1(1):83–136.
Watson D, Clark LA, Tellegen A. Development and validation of brief measures of positive and negative affect: the PANAS scales. J Pers Soc Psychol. 1988;54(6):1063–70.
Bradburn NM. The structure of psychological well-being. Chicago: Aldine Publishing; 1969.
Fredrickson BL, et al. What good are positive emotions in crises? A prospective study of resilience and emotions following the terrorist attacks on the United States on September 11th, 2001. J Pers Soc Psychol. 2003;84(2):365–76.
Ruini C. Positive psychology in the clinical domains: research and practice. Springer; 2017.
Adler NE, A. Page, and S. Institute of Medicine Committee on Psychosocial Services to Cancer Patients/Families in a Community. Cancer care for the whole patient : meeting psychosocial health needs. Washington, D.C.: National Academies Press; 2008.
Mancuso CA, et al. Increasing physical activity in patients with asthma through positive affect and self-affirmation: a randomized trial. Arch Intern Med. 2012;172(4):337–43.
Cohn MA, et al. An online positive affect skills intervention reduces depression in adults with type 2 diabetes. J Posit Psychol. 2014;9(6):523–34.
Sin NL, Lyubomirsky S. Enhancing well-being and alleviating depressive symptoms with positive psychology interventions: a practice-friendly meta-analysis. J Clin Psychol. 2009;65(5):467–87.
Bolier L, et al. Positive psychology interventions: a meta-analysis of randomized controlled studies. BMC Public Health. 2013;13:119.
Moyer A, et al. Characteristics and methodological quality of 25 years of research investigating psychosocial interventions for cancer patients. Cancer Treat Rev. 2009;35(5):475–84.
Haynes RB, et al. Optimal search strategies for retrieving scientifically strong studies of treatment from Medline: analytical survey. BMJ. 2005;330(7501):1179.
Montori VM, et al. Optimal search strategies for retrieving systematic reviews from Medline: analytical survey. BMJ. 2005;330(7482):68.
Higgins JP, Green S. Cochrane handbook for systematic reviews of interventions version 5.1. 0. The cochrane Collab. 2011;5(0).
Higgins JPT, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343.
Hedges LV. Distribution theory for Glass’s estimator of effect size and related estimators. J Educ Stat. 1981;6(2):107–28.
Schnur JB, et al. A randomized trial of a cognitive-behavioral therapy and hypnosis intervention on positive and negative affect during breast cancer radiotherapy. J Clin Psychol. 2009;65(4):443–55.
Tukey JW. Exploratory data analysis. 1977.
Hedges LV, Tipton E, Johnson MC. Robust variance estimation in meta-regression with dependent effect size estimates. Res Synth Methods. 2010;1(1):39–65.
Borenstein M, et al. Basics of meta-analysis: I2 is not an absolute measure of heterogeneity. Res Synth Methods. 2017;8(1):5–18.
Pigott T. Advances in meta-analysis. Springer Science & Business Media; 2012.
Pustejovsky JE, Rodgers MA. Testing for funnel plot asymmetry of standardized mean differences. Res Synth Methods. 2019;10(1):57–71.
Viechtbauer W. Conducting meta-analyses in R with the metafor package. J Stat Softw. 2010;36(3):1–48.
Pustejovsky J. clubSandwich: cluster-robust (sandwich) variance estimators with small-sample corrections. R package version 0.0. 0.9000. 2015. URL: https://github.com/jepusto/clubSandwich.
Moher D, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097.
Antoni MH, et al. How stress management improves quality of life after treatment for breast cancer. J Consult Clin Psychol. 2006;74(6):1143–52.
Badger T, et al. Telephone interpersonal counseling with women with breast cancer: symptom management and quality of life. Oncol Nurs Forum. 2005;32(2):273–9.
Badger TA, et al. Psychosocial interventions to improve quality of life in prostate cancer survivors and their intimate or family partners. Qual Life Res. 2011;20(6):833–44.
Bower JE, et al. Mindfulness meditation for younger breast cancer survivors: a randomized controlled trial.[Erratum appears in Cancer. 2015 Jun 1;121(11):1910]. Cancer. 2015;121(8):1231–40.
Branstrom R, et al. Self-report mindfulness as a mediator of psychological well-being in a stress reduction intervention for cancer patients-a randomized study. Ann Behav Med. 2010;39(2):151–61.
Burns DS, et al. Music imagery for adults with acute leukemia in protective environments: a feasibility study. Support Care Cancer. 2008;16(5):507–13.
Cadmus LA, et al. Exercise and quality of life during and after treatment for breast cancer: results of two randomized controlled trials. Psycho-Oncology. 2009;18(4):343–52.
Carpenter KM, et al. An online stress management workbook for breast cancer. J Behav Med. 2014;37(3):458–68.
Cheung EO, et al. A randomized pilot trial of a positive affect skill intervention (lessons in linking affect and coping) for women with metastatic breast cancer. Psychooncology. 2016.
Cole B., et al. A randomized controlled trial of spiritually-focused meditation in patients newly diagnosed with acute leukemia. Blood. 2010;116(21).
Cole BS, et al. A randomised clinical trial of the effects of spiritually focused meditation for people with metastatic melanoma. Ment Health Relig Cult. 2012;15(2):161–74.
Cook EL, Silverman MJ. Effects of music therapy on spirituality with patients on a medical oncology/hematology unit: a mixed-methods approach. Arts Psychother. 2013;40(2):239–44.
Danhauer SC, et al. Restorative yoga for women with breast cancer: findings from a randomized pilot study. Psycho-Oncology. 2009;18(4):360–8.
Donnelly C, et al. A randomised controlled trial testing the feasibility of a physical activity intervention in managing fatigue with gynaecological cancer survivors. Physiotherapy (United Kingdom). 2011;97:eS294–5.
Fauver R. The healing wisdom within: a preliminary experimental trial of psycho-spiritual integrative therapy for people with cancer. 2012;73:3948–3948.
Fredenburg HA, Silverman MJ. Effects of music therapy on positive and negative affect and pain with hospitalized patients recovering from a blood and marrow transplant: a randomized effectiveness study. Arts Psychother. 2014;41(2):174–80.
Gadler D. The effects of written emotional expression on health-related quality of life and cognitive processing in early-stage breast cancer patients: an exploratory study. 2006;66:6269–6269.
Helgeson V, et al. Education and peer discussion group interventions and adjustment to breast cancer. Arch Gen Psychiatry. 1999;56(4):340–7.
Hoffman DL. The effects of a practice of gratitude on quality of life and depression in head and neck cancer survivors. 2016, ProQuest Information & Learning: US
Jafari N, et al. Spiritual therapy to improve the spiritual well-being of Iranian women with breast cancer: a randomized controlled trial. Evid Based Complement Alternat Med. 2013;2013:353262.
Kovacs AH. The design and evaluation of a brief intervention to enhance well-being among women with breast cancer completing chemotherapy. 2003;64:2924–2924.
Larson MR, et al. A presurgical psychosocial intervention for breast cancer patients: psychological distress and the immune response. J Psychosom Res. 2000;48(2):187–94.
Mutrie N, et al. Benefits of supervised group exercise programme for women being treated for early stage breast cancer: pragmatic randomised controlled trial. BMJ. 2007;334(7592):517.
Nakamura Y, et al. Investigating efficacy of two brief mind–body intervention programs for managing sleep disturbance in cancer survivors: a pilot randomized controlled trial. J Cancer Surviv. 2013;7(2):165–82.
Shao D, Gao W, Cao FL. Brief psychological intervention in patients with cervical cancer: a randomized controlled trial. Health Psychol. 2016;35(12):1383–91.
Victoria Cerezo M, et al. Positive psychology group intervention for breast cancer patients: a randomised trial. Psychol Rep. 2014;115(1):44–64.
Wise M, et al. Suffering in advanced cancer: a randomized control trial of a narrative intervention. J Palliat Med. 2018;21(2):200–7.
Mroczek DK, Kolarz CM. The effect of age on positive and negative affect: a developmental perspective on happiness. J Pers Soc Psychol. 1998;75(5):1333–49.
Adler NE, et al. Additional validation of a scale to assess positive states of mind. Psychosom Med. 1998;60(1):26–32.
Horowitz M, Adler N, Kegeles S. A scale for measuring the occurrence of positive states of mind: a preliminary report. Psychosom Med. 1988;50(5):477–83.
Peterman AH, et al. Measuring spiritual well-being in people with cancer: the functional assessment of chronic illness therapy--spiritual well-being scale (FACIT-Sp). Ann Behav Med. 2002;24(1):49–58.
Weiss LA, Westerhof GJ, Bohlmeijer ET. Can we increase psychological well-being? The effects of interventions on psychological well-being: a meta-analysis of randomized controlled trials. PLoS One. 2016;11(6):e0158092.
Glare P, et al. Predicting survival in patients with advanced disease. Eur J Cancer. 2008;44(8):1146–56.
Kim Y, Given BA. Quality of life of family caregivers of cancer survivors: across the trajectory of the illness. Cancer. 2008;112(11):2556–68.
Kuhl D. Exploring the lived experience of having a terminal illness. J Palliat Care. 2011;27(1):43–52.
Cohen SR, Leis A. What determines the quality of life of terminally ill cancer patients from their own perspective? J Palliat Care. 2002;18(1):48–58.
Austin P, MacLeod R. Finding peace in clinical settings: a narrative review of concept and practice. Palliat Support Care. 2016;15(4):490–8.
Deckx L, van den Akker M, Buntinx F. Risk factors for loneliness in patients with cancer: a systematic literature review and meta-analysis. Eur J Oncol Nurs. 2014;18(5):466–77.
Freedland KE, et al. Usual and unusual care: existing practice control groups in randomized controlled trials of behavioral interventions. Psychosom Med. 2011;73(4):323–35.
Schueller SM. Person–activity fit in positive psychological interventions. The Wiley Blackwell handbook of positive psychological interventions, 2014: p. 385–402.
ClinicalTrials.gov. Changes from current practice described in the final rule. 2016 [cited 2018 14 Feb]; Available from: https://prsinfo.clinicaltrials.gov/FinalRuleChanges-16Sept2016.pdf.
Low CA, et al. Estimation of symptom severity during chemotherapy from passively sensed data: exploratory study. J Med Internet Res. 2017;19(12):e420.
Nasi G, Cucciniello M, Guerrazzi C. The performance of mHealth in cancer supportive care: a research agenda. J Med Internet Res. 2015;17(1):e9.
Scheibe S, et al. Striving to feel good: ideal affect, actual affect, and their correspondence across adulthood. Psychol Aging. 2013;28(1):160–71.
Funding
This research was supported by National Cancer Institute Grant No. R03 CA184560 (PI: Salsman). Dr. McLouth was supported by National Cancer Institute R25 CA122061 (PI: Avis). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Study authors received exempt approval from the Wake Forest University School of Medicine Institutional Review Board under IRB00034301. Study procedures described by the authors did not meet the federal definition of research involving human subjects, and research described in this manuscript constituted secondary analysis of published, de-identified data. Thus, informed consent was not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Portions of this manuscript were presented as part of a symposium at the 2017 Annual Meeting of the Society of Behavioral Medicine: Moskowitz, J. T., Pustejovsky, J. E., Hernandez, R., Schueller, S. M., Berendsen, M., Salsman, J. M. (2017). Don’t worry, be happy? Meta-analysis of intervention trials on positive affect in cancer patients and survivors. In J.M. Salsman (Chair), Promoting psychological well-being in cancer patients and survivors: Meta-analyses of randomized clinical trials. Annals of Behavioral Medicine, 51(Suppl.): S1624.
Electronic supplementary material
ESM 1
(DOCX 30 kb)
Rights and permissions
About this article
Cite this article
Salsman, J.M., Pustejovsky, J.E., Schueller, S.M. et al. Psychosocial interventions for cancer survivors: A meta-analysis of effects on positive affect. J Cancer Surviv 13, 943–955 (2019). https://doi.org/10.1007/s11764-019-00811-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-019-00811-8