Abstract
Background
OSA-patients with persistent excessive daytime sleepiness (EDS) despite CPAP treatment are challenging in daily clinical life. To rule out residual sleep-disordered breathing (SDB), CPAP device-derived data are used in outpatient setting. In case of no pathological finding, a more intensive work-up with is necessary. 6-channel portable monitoring (6Ch-PM) is frequently used to exclude residual SDB. Peripheral arterial tonometry (PAT), as embodied in the WatchPAT device, represents an alternative technique for detecting SDB based on changes in autonomic tone. We wanted to investigate whether PAT might be a useful tool to improve diagnostic work-up in this specific patient group by better identifying residual SDB due to insufficient CPAP-adjustment.
Methods
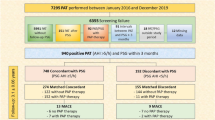
Forty-nine OSA patients (39 male, 10 female) with sufficient CPAP treatment according to device-derived data were consecutively recruited. EDS was assessed by Epworth Sleepiness Scale (ESS). All patients underwent home-based CPAP therapy control by 6Ch-PM and portable monitoring using PAT technology on two consecutive nights. A sequence of both types of monitoring was randomized to prevent possible first night effect bias.
Results
Twelve out of 49 patients showed persistent EDS according to ESS (ESS > 10 points). 6Ch-PM showed a residually increased AHI under CPAP-treatment in 2 of those 12 subjects (positive predictive value, PPV = 16.7%). PAT-PM revealed 5 patients of those 12 with residual SDB (PPV = 41.7%).
Conclusion
PAT could detect significantly more residual SDB under CPAP treatment than 6Ch-PM. Diagnostic work-up of CPAP-treated OSA patients with persistent EDS might be optimized, as insufficient pressure level adjustments could be recognized more precisely in time, possibly preventing more resource-consuming procedures, and potentially increased morbidity.
Clinical trial registration
DRKS00007705



Similar content being viewed by others
References
Lévy P, Kohler M, McNicholas WT, Barbé F, McEvoy RD, Somers VK, Lavie L, Pépin JL (2015) Obstructive sleep apnoea syndrome. Nat Rev Dis Primers 1:15015
Oldenburg O, Arzt M, Börgel J, Penzel T, Skobel CE, Fox H, Schöbel C, Bitter T, Stellbrink C (2017) Addendum zum Positionspapier “Schlafmedizin in der Kardiologie. Update 2014”. Somnologie 21:51–52
Mayer G, Arzt M, Braumann B et al (2017) German S3 Guideline Nonrestorative Sleep/Sleep Disorders, chapter “Sleep-Related Breathing Disorders in Adults,” short version. German Sleep Society (Deutsche Gesellschaft für Schlafforschung und Schlafmedizin, DGSM) Somnologie (in press); https://doi.org/10.1007/s11818-017-0136-2
Kushida CA, Chediak A, Berry RB, Brown LK, Gozal D, Iber C, Parthasarathy S, Quan SF, Rowley JA (2008) Clinical guidelines for the manual titration of positive airway pressure in patients with obstructive sleep apnea. J Clin Sleep Med 4:157–171
Rosenberg R, Doghramji P (2009) Optimal treatment of obstructive sleep apnea and excessive sleepiness. Adv Ther 26:295–312
Dongol EM, Williams AJ (2016) Residual excessive sleepiness in patients with obstructive sleep apnea on treatment with continuous positive airway pressure. Curr Opin Pulm Med 22:589–594
Pillar G, Bar A, Betito M, Schnall RP, Dvir I, Sheffy J, Lavie P (2003) An automatic ambulatory device for detection of AASM defined arousals from sleep: the WP100. Sleep Med 4:207–212
Yalamanchali S, Farajian V, Hamilton C, Pott TR, Samuelson CG, Friedman M (2013) Diagnosis of obstructive sleep apnea by peripheral arterial tonometry: meta-analysis. JAMA Otolaryngol Head Neck Surg 139:1343–1350
Hedner J, White DP, Malhotra A, Herscovici S, Pittman SD, Zou D, Grote L, Pillar G (2011) Sleep staging based on autonomic signals: a multi-center validation study. J Clin Sleep Med 7:301–306
Pittman SD, Pillar G, Berry RB, Malhotra A, MacDonald MM, White DP (2006) Follow-up assessment of CPAP efficacy in patients with obstructive sleep apnea using an ambulatory device based on peripheral arterial tonometry. Sleep Breath 10:123–131
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM, American Academy of Sleep Medicine (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events: deliberations of the sleep apnea definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8:597–619
Prasad B, Carley DW, Herdegen JJ (2010) Continuous positive airway pressure device-based automated detection of obstructive sleep apnea compared to standard laboratory polysomnography. Sleep Breath 14:101–107
Edwards BA, Landry S, Joosten SA, Hamilton GS (2016) Personalized medicine for obstructive sleep apnea therapies: are we there yet? Sleep Med Clin 11:299–311
Lim DC, Sutherland K, Cistulli PA, Pack AI (2017) P4 medicine approach to obstructive sleep apnoea. Respirology 22:849–860
Choi JH, Kim EJ, Kim YS, Choi J, Kim TH, Kwon SY, Lee HM, Lee SH, Shin C, Lee SH (2010) Validation study of portable device for the diagnosis of obstructive sleep apnea according to the new AASM scoring criteria: Watch-PAT 100. Acta Otolaryngol 130:838–843
Jonas DE, Amick HR, Feltner C, Weber RP, Arvanitis M, Stine A, Lux L, Harris RP (2017) Screening for obstructive sleep apnea in adults: evidence report and systematic review for the US Preventive Services Task Force. JAMA 317:415–433
Funding
Itamar Medical Ltd. (Caesarea, Israel) provided support in the form of funding of the WatchPAT 200 devices and sensors. No compensation had been paid to any staff members or participating patients. The sponsor had no role in the design or performance of this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Thomas Penzel has received research grants from ImThera Medical. All other authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (ethical committee of Charité—Universitätsmedizin Berlin, Germany) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Schöbel, C., Knorre, S., Glos, M. et al. Improved follow-up by peripheral arterial tonometry in CPAP-treated patients with obstructive sleep apnea and persistent excessive daytime sleepiness. Sleep Breath 22, 1153–1160 (2018). https://doi.org/10.1007/s11325-018-1668-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-018-1668-9