Abstract
Purpose
Although excessive daytime sleepiness (EDS) is one of the key symptoms of obstructive sleep apnea (OSA), associations between OSA and EDS have been inconsistent, even in patients with severe OSA. To that end, our goal was to investigate factors associated with EDS based on the Epworth Sleepiness Scale (ESS) score in a large clinical population with severe OSA (apnea–hypopnea index ≥30).
Methods
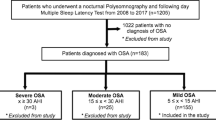
This cross-sectional study included 1,126 consecutive adult patients referred for their first in-laboratory polysomnogram for suspicion of OSA. All patients completed a routine questionnaire including demographics, race, co-morbidities, sleep history, ESS, short-form quality of life questionnaire-12 (SF-12), the Center for Epidemiologic Studies Depression scale, and medications used. Severe OSA was diagnosed in 498 patients. After excluding patients taking narcotics, hypnotics, benzodiazepines, antidepressants, or those with diagnosis of depression, 355 patients remained in the final analytic cohort. Patients were divided into quartiles based on the ESS and comparisons were made between the lowest quartile (ESS ≤ 6; n = 105) and highest quartile (ESS ≥ 13; n = 97).
Results
Compared to the ESS ≤ 6 group, patients in the ESS ≥ 13 group had a significantly higher 3 % oxygen desaturation index and a significantly lower oxygen saturation nadir during sleep (p < 0.05). Moreover, patients with severe OSA in the highest quartile of ESS had higher depressive symptomatology.
Conclusions
In patients with severe OSA, intermittent hypoxemia and depressive symptoms are important contributing factors to EDS.

Similar content being viewed by others
References
Kapur VK, Resnick HE, Gottlieb DJ (2008) Sleep disordered breathing and hypertension: does self-reported sleepiness modify the association? Sleep 31(8):1127–1132
Feng J, He QY, Zhang XL, Chen BY (2012) Epworth Sleepiness Scale may be an indicator for blood pressure profile and prevalence of coronary artery disease and cerebrovascular disease in patients with obstructive sleep apnea. Sleep Breath 16(1):31–40
Barcelo A, Barbe F, de la Pena M, Martinez P, Soriano JB, Pierola J, Agusti AG (2008) Insulin resistance and daytime sleepiness in patients with sleep apnoea. Thorax 63(11):946–950
Nena E, Steiropoulos P, Papanas N, Tsara V, Fitili C, Froudarakis ME, Maltezos E, Bouros D (2012) Sleepiness as a marker of glucose deregulation in obstructive sleep apnea. Sleep Breath 16(1):181–186
Gooneratne NS, Richards KC, Joffe M, Lam RW, Pack F, Staley B, Dinges DF, Pack AI (2011) Sleep disordered breathing with excessive daytime sleepiness is a risk factor for mortality in older adults. Sleep 34(4):435–442
Gottlieb DJ, Whitney CW, Bonekat WH, Iber C, James GD, Lebowitz M, Nieto FJ, Rosenberg CE (1999) Relation of sleepiness to respiratory disturbance index: the Sleep Heart Health Study. Am J Respir Crit Care Med 159(2):502–507
Bixler EO, Vgontzas AN, Lin HM, Calhoun SL, Vela-Bueno A, Kales A (2005) Excessive daytime sleepiness in a general population sample: the role of sleep apnea, age, obesity, diabetes, and depression. J Clin Endocrinol Metab 90(8):4510–4515
Eiseman NA, Westover MB, Mietus JE, Thomas RJ, Bianchi MT (2011) Classification algorithms for predicting sleepiness and sleep apnea severity. J Sleep Res 21(1):101–112
Kapur VK, Baldwin CM, Resnick HE, Gottlieb DJ, Nieto FJ (2005) Sleepiness in patients with moderate to severe sleep-disordered breathing. Sleep 28(4):472–477
Bausmer U, Gouveris H, Selivanova O, Goepel B, Mann W (2010) Correlation of the Epworth Sleepiness Scale with respiratory sleep parameters in patients with sleep-related breathing disorders and upper airway pathology. Eur Arch Otorhinolaryngol 267(10):1645–1648
Sun Y, Ning Y, Huang L, Lei F, Li Z, Zhou G, Tang X (2012) Polysomnographic characteristics of daytime sleepiness in obstructive sleep apnea syndrome. Sleep Breath 16(2):375–381
Chen R, Xiong KP, Lian YX, Huang JY, Zhao MY, Li JX, Liu CF (2011) Daytime sleepiness and its determining factors in Chinese obstructive sleep apnea patients. Sleep Breath 15(1):129–135
Chervin RD, Aldrich MS (1998) Characteristics of apneas and hypopneas during sleep and relation to excessive daytime sleepiness. Sleep 21(8):799–806
Mediano O, Barcelo A, de la Pena M, Gozal D, Agusti A, Barbe F (2007) Daytime sleepiness and polysomnographic variables in sleep apnoea patients. Eur Respir J 30(1):110–113
Chervin RD, Burns JW, Ruzicka DL (2005) Electroencephalographic changes during respiratory cycles predict sleepiness in sleep apnea. Am J Respir Crit Care Med 171(6):652–658
Lombardi C, Parati G, Cortelli P, Provini F, Vetrugno R, Plazzi G, Vignatelli L, Di Rienzo M, Lugaresi E, Mancia G, Montagna P, Castiglioni P (2008) Daytime sleepiness and neural cardiac modulation in sleep-related breathing disorders. J Sleep Res 17(3):263–270
Ye L (2011) Factors influencing daytime sleepiness in Chinese patients with obstructive sleep apnea. Behav Sleep Med 9(2):117–127
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Radloff LS (1977) The CES-D Scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1(3):385–401
Iber C, Ancoli-Israel S, Chesson A, Quan SF (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications, 1st edn. American Academy of Sleep Medicine, Westchester
Khawaja IS, Olson EJ, van der Walt C, Bukartyk J, Somers V, Dierkhising R, Morgenthaler TI (2010) Diagnostic accuracy of split-night polysomnograms. J Clin Sleep Med 6(4):357–362
Gozal D, Kheirandish L (2005) Sleepiness and neurodegeneration in sleep-disordered breathing: convergence of signaling cascades. Am J Respir Crit Care Med 171(12):1325–1327
Veasey SC, Davis CW, Fenik P, Zhan G, Hsu YJ, Pratico D, Gow A (2004) Long-term intermittent hypoxia in mice: protracted hypersomnolence with oxidative injury to sleep–wake brain regions. Sleep 27(2):194–201
Zhan G, Fenik P, Pratico D, Veasey SC (2005) Inducible nitric oxide synthase in long-term intermittent hypoxia: hypersomnolence and brain injury. Am J Respir Crit Care Med 171(12):1414–1420
Zhan G, Serrano F, Fenik P, Hsu R, Kong L, Pratico D, Klann E, Veasey SC (2005) NADPH oxidase mediates hypersomnolence and brain oxidative injury in a murine model of sleep apnea. Am J Respir Crit Care Med 172(7):921–929
Canessa N, Castronovo V, Cappa SF, Aloia MS, Marelli S, Falini A, Alemanno F, Ferini-Strambi L (2011) Obstructive sleep apnea: brain structural changes and neurocognitive function before and after treatment. Am J Respir Crit Care Med 183(10):1419–1426
Yaffe K, Laffan AM, Harrison SL, Redline S, Spira AP, Ensrud KE, Ancoli-Israel S, Stone KL (2011) Sleep-disordered breathing, hypoxia, and risk of mild cognitive impairment and dementia in older women. JAMA 306(6):613–619
Aloia MS, Arnedt JT, Smith L, Skrekas J, Stanchina M, Millman RP (2005) Examining the construct of depression in obstructive sleep apnea syndrome. Sleep Med 6(2):115–121
Harris M, Glozier N, Ratnavadivel R, Grunstein RR (2009) Obstructive sleep apnea and depression. Sleep Med Rev 13(6):437–444
Pamidi S, Knutson KL, Ghods F, Mokhlesi B (2011) Depressive symptoms and obesity as predictors of sleepiness and quality of life in patients with REM-related obstructive sleep apnea: cross-sectional analysis of a large clinical population. Sleep Med 12(9):827–831
Benca RM, Obermeyer WH, Thisted RA, Gillin JC (1992) Sleep and psychiatric disorders. A meta-analysis. Arch Gen Psychiatry 49(8):651–668, discussion 669–670
Berger M, van Calker D, Riemann D (2003) Sleep and manipulations of the sleep–wake rhythm in depression. Acta Psychiatr Scand 108(418):83–91
Mendlewicz J (2009) Sleep disturbances: core symptoms of major depressive disorder rather than associated or comorbid disorders. World J Biol Psychiatry 10(4):269–275
Ohayon MM (2003) The effects of breathing-related sleep disorders on mood disturbances in the general population. J Clin Psychiatry 64(10):1195–1200, quiz, 1274–1276
Sharafkhaneh A, Giray N, Richardson P, Young T, Hirshkowitz M (2005) Association of psychiatric disorders and sleep apnea in a large cohort. Sleep 28(11):1405–1411
Vandeputte M, de Weerd A (2003) Sleep disorders and depressive feelings: a global survey with the Beck depression scale. Sleep Med 4(4):343–345
Katon WJ (2003) Clinical and health services relationships between major depression, depressive symptoms, and general medical illness. Biol Psychiatry 54(3):216–226
McCall WV, Harding D, O’Donovan C (2006) Correlates of depressive symptoms in patients with obstructive sleep apnea. J Clin Sleep Med 2(4):424–426
Shepertycky MR, Banno K, Kryger MH (2005) Differences between men and women in the clinical presentation of patients diagnosed with obstructive sleep apnea syndrome. Sleep 28(3):309–314
Wahner-Roedler DL, Olson EJ, Narayanan S, Sood R, Hanson AC, Loehrer LL, Sood A (2007) Gender-specific differences in a patient population with obstructive sleep apnea–hypopnea syndrome. Gend Med 4(4):329–338
Bardwell WA, Ancoli-Israel S, Dimsdale JE (2007) Comparison of the effects of depressive symptoms and apnea severity on fatigue in patients with obstructive sleep apnea: a replication study. J Affect Disord 97(1–3):181–186
Eyre H, Baune BT (2012) Neuroplastic changes in depression: a role for the immune system. Psychoneuroendocrinology; Apr 21 [Epub ahead of print] PMID: 22525700
King AC, Belenky G, Van Dongen HP (2009) Performance impairment consequent to sleep loss: determinants of resistance and susceptibility. Curr Opin Pulm Med 15:559–564
Landolt HP (2008) Genotype-dependent differences in sleep, vigilance, and response to stimulants. Curr Pharm Des 14(32):3396–3407
Tafti M (2009) Genetic aspects of normal and disturbed sleep. Sleep Med 10(Suppl 1):S17–S21
Gozal D, Khalyfa A, Capdevila OS, Kheirandish-Gozal L, Khalyfa AA, Kim J (2012) Cognitive function in prepubertal children with obstructive sleep apnea: a modifying role for NADPH oxidase p22 subunit gene polymorphisms? Antioxid Redox Signal 16(2):171–177
Khalyfa A, Serpero LD, Kheirandish-Gozal L, Capdevila OS, Gozal D (2011) TNF-alpha gene polymorphisms and excessive daytime sleepiness in pediatric obstructive sleep apnea. J Pediatr 158(1):77–82
Gass N, Ollila HM, Utge S, Partonen T, Kronholm E, Pirkola S, Suhonen J, Silander K, Porkka-Heiskanen T, Paunio T (2010) Contribution of adenosine related genes to the risk of depression with disturbed sleep. J Affect Disord 126(1–2):134–139
Utge SJ, Soronen P, Loukola A, Kronholm E, Ollila HM, Pirkola S, Porkka-Heiskanen T, Partonen T, Paunio T (2010) Systematic analysis of circadian genes in a population-based sample reveals association of TIMELESS with depression and sleep disturbance. PLoS One 5(2):e9259
Source of funding
This study is supported in part by NIH grant HD057796.
Conflict of Interest
None of the authors have a conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jacobsen, J.H., Shi, L. & Mokhlesi, B. Factors associated with excessive daytime sleepiness in patients with severe obstructive sleep apnea. Sleep Breath 17, 629–635 (2013). https://doi.org/10.1007/s11325-012-0733-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-012-0733-z