Abstract
Purpose
The age-related decline of the testosterone-to-estrogen (T-to-E2) ratio in serum is associated with the increased prevalence of prostatic inflammation. The goal of the study was to induce prostatic inflammation with E2 and androgen treatment and to explore the inflammatory markers and apoptosis on prostatitis.
Methods
Castrated SD rats were treated with E2 and different doses of androgens to achieve an elevated concentration of E2 and a wide range of the androgen-to-E2 ratio in serum. Inflammatory markers TNF-α, COX-2 and MIP-1α were immunohistochemically stained. Apoptosis detection was evaluated by TUNEL staining. E2, T and DHT concentrations in serum were measured, and the relative weight of the prostate and seminal vesicles were determined.
Results
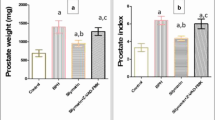
T was anti-inflammatory at the doses which normalized or over stimulated the growth of the prostate and seminal vesicles. Experimentally, prostatitis induced by E2 alone increased the prostatic levels of the inflammatory markers TNF-a, COX-2 and MIP-1a. As signs of anti-estrogenic actions, androgens dose-dependently decreased the expression of TNF-α, COX-2 and MIP-1α. Prostatitis induced by E2 alone caused extensive apoptosis in the castrate-resistant cells and E2-induced apoptosis occurred dependently of T manipulation.
Conclusions
Estrogen-alone-induced inflammatory response could promote the expression of inflammatory markers; however, T supplementation reduces the expression of inflammatory markers and E2-induced apoptosis occurs dependently on T manipulation in prostatitis.






Similar content being viewed by others
References
Kim DS, Lee EJ, Cho KS, Yoon SJ, Lee YH, Hong SJ (2009) Preventive effects of oligomerized polyphenol on estradiol-induced prostatitis in rats. Yonsei Med J 50(3):391–398
McNaughton Collins M, Pontari MA, O’Leary MP, Calhoun EA, Santanna J, Landis JR, Kusek JW, Litwin MS (2001) Quality of Life Is Impaired in Men with Chronic Prostatitis the Chronic Prostatitis Collaborative Research Network*. J Gen Intern Med 16(10):656–662
Turner JA, Ciol MA, Von Korff M, Berger R (2005) Health concerns of patients with nonbacterial prostatitis/pelvic pain. Arch Intern Med 165(9):1054–1059
Foster P (2006) Disruption of reproductive development in male rat offspring following in utero exposure to phthalate esters. Int J Androl 29(1):140–147
Foster PM, Mcintyre BS (2002) Endocrine active agents: implications of adverse and non-adverse changes. Toxicol Pathol 30(1):59–65
Kelce WR, Wilson EM (1997) Environmental antiandrogens: developmental effects, molecular mechanisms, and clinical implications. J Mol Med 75(3):198–207
Vermeulen A, Kaufman J, Goemaere S, Van Pottelberg I (2002) Estradiol in elderly men. Aging Male 5(2):98–102
Kaufman JM, Vermeulen A (2005) The decline of androgen levels in elderly men and its clinical and therapeutic implications. Endocr Rev 26(6):833–876
Bernoulli J, Yatkin E, Konkol Y, Talvitie EM, Santti R, Streng T (2008) Prostatic inflammation and obstructive voiding in the adult Noble rat: impact of the testosterone to estradiol ratio in serum. Prostate 68(12):1296–1306
Straub RH (2007) The complex role of estrogens in inflammation. Endocr Rev 28(5):521–574
Schneider G, Kirschner MA, Berkowitz R, Ertel NH (1979) Increased Estrogen Production in Obese Men*. J Clin Endocrinol Metab 48(4):633–638
Cowin PA, Foster P, Pedersen J, Hedwards S, McPherson SJ, Risbridger GP (2008) Early-onset endocrine disruptor induced prostatitis in the rat. Environ Health Perspect 116(7):923–929
Vykhovanets E, Resnick M, MacLennan G, Gupta S (2007) Experimental rodent models of prostatitis: limitations and potential. Prostate Cancer Prostatic Dis 10(1):15–29
Naslund MJ, Strandberg J, Coffey D (1988) The role of androgens and estrogens in the pathogenesis of experimental nonbacterial prostatitis. J Urol 140(5):1049–1053
Vignozzi L, Morelli A, Sarchielli E, Comeglio P, Filippi S, Cellai I, Maneschi E, Serni S, Gacci M, Carini M (2012) Testosterone protects from metabolic syndrome-associated prostate inflammation: an experimental study in rabbit. J Endocrinol 212(1):71–84
Yatkin E, Bernoulli J, Lammintausta R, Santti R (2008) Fispemifene [Z-2-{2-[4-(4-chloro-1, 2-diphenylbut-1-enyl)-phenoxy] ethoxy}-ethanol], a novel selective estrogen receptor modulator, attenuates glandular inflammation in an animal model of chronic nonbacterial prostatitis. J Pharmacol Exp Ther 327(1):58–67
Sugimoto M, Oka M, Tsunemori H, Yamashita M, Kakehi Y (2011) Effect of a phytotherapeutic agent, Eviprostat®, on prostatic and urinary cytokines/chemokines in a rat model of nonbacterial prostatitis. Prostate 71(4):438–444
Seiji MYK, Michiko O et al (2013) Bladder function in 17 β-estradiol- induced nonbacterial prostatitis model in Wister rats. Int Urol Nephrol 45:749–754
Bebo BF, Schuster JC, Vandenbark AA, Offner H (1999) Androgens alter the cytokine profile and reduce encephalitogenicity of myelin-reactive T cells. J Immunol 162(1):35–40
Fijak M, Schneider E, Klug J, Bhushan S, Hackstein H, Schuler G, Wygrecka M, Gromoll J, Meinhardt A (2011) Testosterone replacement effectively inhibits the development of experimental autoimmune orchitis in rats: evidence for a direct role of testosterone on regulatory T cell expansion. J Immunol 186(9):5162–5172
Isaacs JT (1984) Antagonistic effect of androgen on prostatic cell death. Prostate 5(5):545–557
Schleipen B, Hertrampf T, Fritzemeier K, Kluxen F, Lorenz A, Molzberger A, Velders M, Diel P (2011) ERβ-specific agonists and genistein inhibit proliferation and induce apoptosis in the large and small intestine. Carcinogenesis 32(11):1675–1683
English HF, Santen RJ, Lsaacs JT (1987) Response of glandular versus basal rat ventral prostatic epithelial cells to androgen withdrawal and replacement. Prostate 11(3):229–242
Hussain S, Lawrence MG, Taylor RA, Lo CY-W, BioResource A, Frydenberg M, Ellem SJ, Furic L, Risbridger GP (2012) Estrogen receptor β activation impairs prostatic regeneration by inducing apoptosis in murine and human stem/progenitor enriched cell populations. PLoS One 7(7):e40732
McPherson SJ, Hussain S, Balanathan P, Hedwards SL, Niranjan B, Grant M, Chandrasiri UP, Toivanen R, Wang Y, Taylor RA (2010) Estrogen receptor–β activated apoptosis in benign hyperplasia and cancer of the prostate is androgen independent and TNFα mediated. Proc Natl Acad Sci 107(7):3123–3128
Acknowledgments
This work was supported by National Science and Technology Major Project of Original New Drug Research of China (Grant No.2011ZX09301-005) and Shanghai “Innovative Action Plan” Experimental Animal Study (Grant No.11140901300 and 11140901303).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Jia, Yl., Liu, X., Yan, Jy. et al. The alteration of inflammatory markers and apoptosis on chronic prostatitis induced by estrogen and androgen. Int Urol Nephrol 47, 39–46 (2015). https://doi.org/10.1007/s11255-014-0845-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-014-0845-4