ABSTRACT
Purpose
The increasing incidence of endometrial cancer (EC), in younger age at diagnosis, calls for new tissue-sparing treatment options. This work aims to evaluate the potential of imiquimod (IQ) in the treatment of low-grade EC.
Methods
Effects of IQ on the viabilities of Ishikawa and HEC-1A cells were evaluated using MTT assay. The ability of IQ to induce apoptosis was evaluated by testing changes in caspase 3/7 levels and expression of cleaved caspase-3, using luminescence assay and western blot. Apoptosis was confirmed by flow cytometry and the expression of cleaved PARP. Western blot was used to evaluate the effect of IQ on expression levels of Bcl-2, Bcl-xL, and BAX. Finally, the in vivo efficacy of IQ was tested in an EC mouse model.
Results
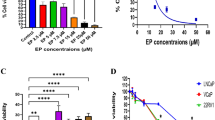
There was a decrease in EC cell viability following IQ treatment as well as increased caspase 3/7 activities, cleaved caspase-3 expression, and Annexin-V/ 7AAD positive cell population. Western blot results showed the ability of IQ in cleaving PARP, decreasing Bcl-2 and Bcl-xL expressions, but not affecting BAX expression. In vivo study demonstrated IQ’s ability to inhibit EC tumor growth and progression without significant toxicity.
Conclusions
IQ induces apoptosis in low-grade EC cells in vitro, probably through its direct effect on Bcl-2 family protein expression. In, vivo, IQ attenuates EC tumor growth and progression, without an obvious toxicity. Our study provides the first building block for the potential role of IQ in the non-surgical management of low-grades EC and encouraging further investigations.






Similar content being viewed by others
Abbreviations
- BAX:
-
Bcl-2-associated X protein gene
- Bcl-2:
-
B-cell lymphoma/leukemia-2 gen
- Bcl-xL:
-
Bcl-2 homologue B-cell lymphoma-extra large
- E2:
-
Estrogen
- EC:
-
Endometrial cancer
- EH:
-
Endometrial hyperplasia
- ER:
-
Estrogen receptors
- GnRH:
-
Gonadotropin-releasing hormone
- IQ:
-
Imiquimod
- Mcl-1:
-
Myeloid cell leukemia 1
- MAPK:
-
Mitogen-activated protein kinas
- PARP:
-
Poly (ADP-ribose) polymerase
- P4:
-
Progesterone
- TLR:
-
Toll-like receptors
REFERENCES
Ho JC, Allen PK, Jhingran A, Westin SN, Lu KH, Eifel PJ, et al. Management of nodal recurrences of endometrial cancer with IMRT. Gynecol Oncol. 2015;139(1):40–6.
Altman AD, Ferguson SE, Atenafu EG, Kobel M, McAlpine JN, Panzarella T, et al. Canadian high risk endometrial cancer (CHREC) consortium: analyzing the clinical behavior of high risk endometrial cancers. Gynecol Oncol. 2015;139(2):268–74.
Kaaks R, Lukanova A, Kurzer MS. Obesity, endogenous hormones, and endometrial cancer risk: a synthetic review. Cancer Epidemiol, Biomarkers Prev: Publ Am Assoc Cancer Res, Cosponsored Am Soc Prev Oncol. 2002;11(12):1531–43.
Felix AS, Scott McMeekin D, Mutch D, Walker JL, Creasman WT, Cohn DE, et al. Associations between etiologic factors and mortality after endometrial cancer diagnosis: the NRG Oncology/Gynecologic Oncology Group 210 trial. Gynecol Oncol. 2015;139(1):70–6.
Siegel L, Miller K, Jemal A. Cancer statistics, 2016. CA Cancer J Clin. 2016;66(1):7–30.
Matsuo K, Ramzan AA, Gualtieri MR, Mhawech-Fauceglia P, Machida H, Moeini A, et al. Prediction of concurrent endometrial carcinoma in women with endometrial hyperplasia. Gynecol Oncol. 2015;139(2):261–7.
Morice P, Leary A, Creutzberg C, Abu-Rustum N, Darai E. Endometrial cancer. Lancet. 2015.
Amant F, Moerman P, Neven P, Timmerman D, Van Limbergen E, Vergote I. Endometrial cancer. Lancet. 2005;366(9484):491–505.
Roett MA. Genital cancers in women: uterine cancer. FP Essent. 2015;438:11–7.
Reeves GK, Pirie K, Beral V, Green J, Spencer E, Bull D, et al. Cancer incidence and mortality in relation to body mass index in the Million Women Study: cohort study. BMJ. 2007;335(7630):1134.
Murali R, Soslow RA, Weigelt B. Classification of endometrial carcinoma: more than two types. Lancet Oncol. 2014;15(7):e268–78.
Mahdi H, Elshaikh MA, DeBenardo R, Munkarah A, Isrow D, Singh S, et al. Impact of adjuvant chemotherapy and pelvic radiation on pattern of recurrence and outcome in stage I non-invasive uterine papillary serous carcinoma. A multi-institution study. Gynecol Oncol. 2015;137(2):239–44.
Llaurado M, Ruiz A, Majem B, Ertekin T, Colas E, Pedrola N, et al. Molecular bases of endometrial cancer: new roles for new actors in the diagnosis and the therapy of the disease. Mol Cell Endocrinol. 2012;358(2):244–55.
Pollard JW, Pacey J, Cheng SV, Jordan EG. Estrogens and cell death in murine uterine luminal epithelium. Cell Tissue Res. 1987;249(3):533–40.
Kim JJ, Kurita T, Bulun SE. Progesterone action in endometrial cancer, endometriosis, uterine fibroids, and breast cancer. Endocr Rev. 2013;34(1):130–62.
Song J, Rutherford T, Naftolin F, Brown S, Mor G. Hormonal regulation of apoptosis and the Fas and Fas ligand system in human endometrial cells. Mol Hum Reprod. 2002;8(5):447–55.
Alexaki VI, Charalampopoulos I, Kampa M, Nifli AP, Hatzoglou A, Gravanis A, et al. Activation of membrane estrogen receptors induce pro-survival kinases. J Steroid Biochem Mol Biol. 2006;98(2–3):97–110.
Reis FM, Petraglia F, Taylor RN. Endometriosis: hormone regulation and clinical consequences of chemotaxis and apoptosis. Hum Reprod Update. 2013;19(4):406–18.
Amaral JD, Sola S, Steer CJ, Rodrigues CM. Role of nuclear steroid receptors in apoptosis. Curr Med Chem. 2009;16(29):3886–902.
Zhang R, He Y, Zhang X, Xing B, Sheng Y, Lu H, et al. Estrogen receptor-regulated microRNAs contribute to the BCL2/BAX imbalance in endometrial adenocarcinoma and precancerous lesions. Cancer Lett. 2012;314(2):155–65.
Bozdogan O, Atasoy P, Erekul S, Bozdogan N, Bayram M. Apoptosis-related proteins and steroid hormone receptors in normal, hyperplastic, and neoplastic endometrium. Int J Gynecol Pathol. 2002;21(4):375–82.
Rein DT, Schondorf T, Breidenbach M, Janat MM, Weikelt A, Gohring UJ, et al. Lack of correlation between P53 expression, BCL-2 expression, apoptosis and ex vivo chemosensitivity in advanced human breast cancer. Anticancer Res. 2000;20(6D):5069–72.
Zhou R, Yang Y, Lu Q, Wang J, Miao Y, Wang S, et al. Prognostic factors of oncological and reproductive outcomes in fertility-sparing treatment of complex atypical hyperplasia and low-grade endometrial cancer using oral progestin in Chinese patients. Gynecol Oncol. 2015.
Dorais J, Dodson M, Calvert J, Mize B, Travarelli JM, Jasperson K, et al. Fertility-sparing management of endometrial adenocarcinoma. Obstet Gynecol Surv. 2011;66(7):443–51.
Kim JJ, Chapman-Davis E. Role of progesterone in endometrial cancer. Semin Reprod Med. 2010;28(1):81–90.
Shao R. Progesterone receptor isoforms A and B: new insights into the mechanism of progesterone resistance for the treatment of endometrial carcinoma. E Cancer Med Sci. 2013;7:381.
Erkanli S, Ayhan A. Fertility-sparing therapy in young women with endometrial cancer: 2010 update. Int J Gynecol Cancer. 2010;20(7):1170–87.
Schon MP, Schon M. Imiquimod: mode of action. Br J Dermatol. 2007;157 Suppl 2:8–13.
Karnes JB, Usatine RP. Management of external genital warts. Am Fam Physician. 2014;90(5):312–8.
Smith EB, Schwartz M, Kawamoto H, You X, Hwang D, Liu H, et al. Antitumor effects of imidazoquinolines in urothelial cell carcinoma of the bladder. J Urol. 2007;177(6):2347–51.
Han JH, Lee J, Jeon SJ, Choi ES, Cho SD, Kim BY, et al. In vitro and in vivo growth inhibition of prostate cancer by the small molecule imiquimod. Int J Oncol. 2013;42(6):2087–93.
Kim JM, Lee HJ, Kim SH, Kim HS, Ko HC, Kim BS, et al. Efficacy of 5% imiquimod cream on vulvar intraepithelial neoplasia in Korea: pilot study. Ann Dermatol. 2015;27(1):66–70.
Grimm C, Polterauer S, Natter C, Rahhal J, Hefler L, Tempfer CB, et al. Treatment of cervical intraepithelial neoplasia with topical imiquimod: a randomized controlled trial. Obstet Gynecol. 2012;120(1):152–9.
Diakomanolis E, Haidopoulos D, Stefanidis K. Treatment of high-grade vaginal intraepithelial neoplasia with imiquimod cream. N Engl J Med. 2002;347(5):374.
Schon MP, Schon M. Immune modulation and apoptosis induction: two sides of the antitumoral activity of imiquimod. Apoptosis. 2004;9(3):291–8.
Sohn KC, Li ZJ, Choi DK, Zhang T, Lim JW, Chang IK, et al. Imiquimod induces apoptosis of squamous cell carcinoma (SCC) cells via regulation of A20. PLoS One. 2014;9(4), e95337.
Schon M, Bong AB, Drewniok C, Herz J, Geilen CC, Reifenberger J, et al. Tumor-selective induction of apoptosis and the small-molecule immune response modifier imiquimod. J Natl Cancer Inst. 2003;95(15):1138–49.
Huang SW, Chang CC, Lin CC, Tsai JJ, Chen YJ, Wu CY, et al. Mcl-1 determines the imiquimod-induced apoptosis but not imiquimod-induced autophagy in skin cancer cells. J Dermatol Sci. 2012;65(3):170–8.
Mossalam M, Matissek KJ, Okal A, Constance JE, Lim CS. Direct induction of apoptosis using an optimal mitochondrially targeted p53. Mol Pharm. 2012;9(5):1449–58.
Archibald M, Pritchard T, Nehoff H, Rosengren RJ, Greish K, Taurin S. A combination of sorafenib and nilotinib reduces the growth of castrate-resistant prostate cancer. Int J Nanomedicine. 2016;11:179–200.
Jayakrishnan K, Anupama R, Koshy A, Raju R. Endometrial carcinoma in a young subfertile woman with polycystic ovarian syndrome. J Hum Reprod Sci. 2010;3(1):38–41.
Kullander S. Treatment of endometrial cancer with GnRH analogs. Recent Results Cancer Res. 1992;124:69–73.
Krasner C. Aromatase inhibitors in gynecologic cancers. J Steroid Biochem Mol Biol. 2007;106(1–5):76–80.
Gressel GM, Parkash V, Pal L. Management options and fertility-preserving therapy for premenopausal endometrial hyperplasia and early-stage endometrial cancer. Int J Gynaecol Obstet. 2015;131(3):234–9.
Coleman RL, Sill MW, Bell-McGuinn K, Aghajanian C, Gray HJ, Tewari KS, et al. A phase II evaluation of the potent, highly selective PARP inhibitor veliparib in the treatment of persistent or recurrent epithelial ovarian, fallopian tube, or primary peritoneal cancer in patients who carry a germline BRCA1 or BRCA2 mutation - An NRG Oncology/Gynecologic Oncology Group study. Gynecol Oncol. 2015;137(3):386–91.
Reinbolt RE, Hays JL. The role of PARP inhibitors in the treatment of gynecologic malignancies. Front Oncol. 2013;3:237.
Fraser M, Zhao H, Luoto KR, Lundin C, Coackley C, Chan N, et al. PTEN deletion in prostate cancer cells does not associate with loss of RAD51 function: implications for radiotherapy and chemotherapy. Clin Cancer Res. 2012;18(4):1015–27.
Janzen DM, Paik DY, Rosales MA, Yep B, Cheng D, Witte ON, et al. Low levels of circulating estrogen sensitize PTEN-null endometrial tumors to PARP inhibition in vivo. Mol Cancer Ther. 2013;12(12):2917–28.
Rixe O, Fojo T. Is cell death a critical end point for anticancer therapies or is cytostasis sufficient? Clin Cancer Res. 2007;13(24):7280–7.
Meden H, Rath W, Kuhn W. Taxol--a new cytostatic drug for therapy of ovarian and breast cancer. Geburtshilfe Frauenheilkd. 1994;54(4):187–93.
Ulrichs K, Yu MY, Duncker D, Muller-Ruchholtz W. Immunosuppression by cytostatic drugs? Behring Inst Mitt. 1984;74:239–49.
Theisen ER, Gajiwala S, Bearss J, Sorna V, Sharma S, Janat-Amsbury M. Reversible inhibition of lysine specific demethylase 1 is a novel anti-tumor strategy for poorly differentiated endometrial carcinoma. BMC Cancer. 2014;14:752.
Schon MP, Wienrich BG, Drewniok C, Bong AB, Eberle J, Geilen CC, et al. Death receptor-independent apoptosis in malignant melanoma induced by the small-molecule immune response modifier imiquimod. J Invest Dermatol. 2004;122(5):1266–76.
Otsuki Y, Misaki O, Sugimoto O, Ito Y, Tsujimoto Y, Akao Y. Cyclic bcl-2 gene expression in human uterine endometrium during menstrual cycle. Lancet. 1994;344(8914):28–9.
Bhargava V, Kell DL, van de Rijn M, Warnke RA. Bcl-2 immunoreactivity in breast carcinoma correlates with hormone receptor positivity. Am J Pathol. 1994;145(3):535–40.
McDonnell TJ, Troncoso P, Brisbay SM, Logothetis C, Chung LW, Hsieh JT, et al. Expression of the protooncogene bcl-2 in the prostate and its association with emergence of androgen-independent prostate cancer. Cancer Res. 1992;52(24):6940–4.
Laban M, Ibrahim E, Agur W, Ahmed A. Bcl-2 may play a role in the progression of endometrial hyperplasia and early carcinogenesis, but not linked to further tumorigenesis. J Microscopy Ultrastructure. 2015;3(1):19–24.
Kandalaft LE, Singh N, Liao JB, Facciabene A, Berek JS, Powell Jr DJ, et al. The emergence of immunomodulation: combinatorial immunochemotherapy opportunities for the next decade. Gynecol Oncol. 2010;116(2):222–33.
Coosemans A, Vanderstraeten A, Tuyaerts S, Verschuere T, Moerman P, Berneman ZN, et al. Wilms’ Tumor Gene 1 (WT1)--loaded dendritic cell immunotherapy in patients with uterine tumors: a phase I/II clinical trial. Anticancer Res. 2013;33(12):5495–500.
Santin AD, Hermonat PL, Ravaggi A, Bellone S, Cowan C, Coke C, et al. Development and therapeutic effect of adoptively transferred T cells primed by tumor lysate-pulsed autologous dendritic cells in a patient with metastatic endometrial cancer. Gynecol Obstet Invest. 2000;49(3):194–203.
Jung IK, Kim SS, Suh DS, Kim KH, Lee CH, Yoon MS. Tumor-infiltration of T-lymphocytes is inversely correlated with clinicopathologic factors in endometrial adenocarcinoma. Obstet Gynecol Sci. 2014;57(4):266–73.
ACKNOWLEDGMENTS AND DISCLOSURES
This research was supported in part by a Faculty and Creative Grant and Department of Obstetrics and Gynecology at the University of Utah, National Cancer Institute under award number R01-CA140348-01, and The Huntsman Cancer Institute’s Women’s Disease-Oriented Teams Research Funding. We would like to thank Dr. Victoria Bae-Jump, University of North Carolina at Chapel Hill for providing Ishikawa cells, Chieh-Hsiang Yang, Jesus Arellano, and Cameron Neilson for assisting with animal studies and data collection, and Benjamin J. Bruno, Dr. Andrew Dixon, and Dr. Sebastien Taurin for scientific discussions and help with data analyses.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 127 kb)
Rights and permissions
About this article
Cite this article
Almomen, A., Jarboe, E.A., Dodson, M.K. et al. Imiquimod Induces Apoptosis in Human Endometrial Cancer Cells In vitro and Prevents Tumor Progression In vivo . Pharm Res 33, 2209–2217 (2016). https://doi.org/10.1007/s11095-016-1957-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-016-1957-6