Abstract
Background
Determining the risk stratification of nonvariceal upper gastrointestinal bleeding (NVUGIB) plays a vital role in treating upper gastrointestinal bleeding (UGIB). Traditional scores like Glasgow–Blatchford score (GBS), Rockall score (RS), and AIMS65 score have been widely utilized in UGIB practice, however exhibiting limited practical use due to relative lack of user-friendly characters. Prealbumin as a nutritional indicator and d-dimer as a fibrinolytic activity monitor, are generally used to evaluate the overall nutritional and fibrinolytic condition in UGIB patients.
Aims
Here, we explored the predictive value of these two markers in NVUGIB for evaluating severity and prognosis including rebleeding and surgery intervention.
Methods
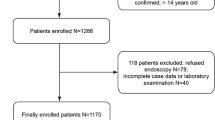
One hundred and eighty-five patients suffering NVUGIB were enrolled. Their GBS, RS, and AIMS65 score, routine laboratory test results including prealbumin and d-dimer were determined after admission. Multivariate regression analysis was performed to define the independent predictors of rebleeding. ROC curves were generated to compare the suitability of prealbumin, d-dimer, and scores for rebleeding prediction.
Results
The NVUGIB patients with rebleeding exhibited higher scores, white blood cell counts, d-dimer, CRP, proportion of surgery intervention, and longer hospital stay, but lower hematocrit, hemoglobin, calcium, prealbumin, and fibrinogen than those without rebleeding. The multivariate regression analysis demonstrated that prealbumin and d-dimer were independent predictors for rebleeding. Values of prealbumin and d-dimer were correlated with hospital stay, ulcer degrees, and surgery demand. The ROC curve analyses showed that prealbumin and d-dimer exhibited superior prediction value over the scoring systems.
Conclusions
Prealbumin and d-dimer are promising predictors for severity and prognosis in NVUGIB practice.





Similar content being viewed by others
References
Cesaro P, Kohn A, Petruziello L, et al. A survey on mortality from non-variceal upper gastrointestinal bleeding: is the emergency referral system adequate. Dig Liver Dis. 2013;45:953–956.
Rockall TA, Logan RF, Devlin HB, Northfield TC. Risk assessment after acute upper gastrointestinal haemorrhage. Gut. 1996;38:316–321.
Gralnek IM, Dumonceau JM, Kuipers EJ, et al. Diagnosis and management of nonvariceal upper gastrointestinal hemorrhage: European Society of Gastrointestinal Endoscopy (ESGE) guideline. Endoscopy. 2015;47:a1–a46.
Horibe M, Kaneko T, Yokogawa N, et al. A simple scoring system to assess the need for an endoscopic intervention in suspected upper gastrointestinal bleeding: a prospective cohort study. Dig Liver Dis. 2016;48:1180–1186.
Chaikitamnuaychok R, Patumanond J. Clinical risk characteristics of upper gastrointestinal hemorrhage severity: a multivariable risk analysis. Gastroenterol Res. 2012;5:149–155.
Iino C, Mikami T, Igarashi T, et al. Evaluation of scoring models for identifying the need for therapeutic intervention of upper gastrointestinal bleeding: a new prediction score model for Japanese patients. Dig Endosc. 2016;28:714–721.
Kaya E, Karaca MA, Aldemir D, Ozmen MM. Predictors of poor outcome in gastrointestinal bleeding in emergency department. World J Gastroenterol. 2016;22:4219–4225.
Hwang S, Jeon SW, Kwon JG, et al. The novel scoring system for 30-day mortality in patients with non-variceal upper gastrointestinal bleeding. Dig Dis Sci. 2016;61:2002–2010. https://doi.org/10.1007/s10620-016-4087-4.
Kumar NL, Claggett BL, Cohen AJ, Nayor J, Saltzman JR. Association between an increase in blood urea nitrogen at 24 hours and worse outcomes in acute nonvariceal upper GI bleeding. Gastrointest Endosc. 2017;86:1022–1027.
Al-Naamani K, Alzadjali N, Barkun AN, Fallone CA. Does blood urea nitrogen level predict severity and high-risk endoscopic lesions in patients with nonvariceal upper gastrointestinal bleeding? Can J Gastroenterol. 2008;22:399–403.
Tomizawa M, Shinozaki F, Hasegawa R, et al. Patient characteristics with high or low blood urea nitrogen in upper gastrointestinal bleeding. World J Gastroenterol. 2015;21:7500–7505.
Ebrahimi BH, Morteza BHR, Rahmani F, Shahsavari NK, Ettehadi A. Clinical scoring systems in predicting the outcome of acute upper gastrointestinal bleeding; a narrative review. Emergency. 2017;5:e36.
Fattah SA, El-Hamshary NK, Kilany YF, et al. Prognostic and predictive values of MELD score, platelet count and pre-albumin in patients with compensated and decompensated liver cirrhosis with acute variceal bleeding. J Egypt Soc Parasitol. 2012;42:443–452.
Vreeburg EM, Levi M, Rauws EA, et al. Enhanced mucosal fibrinolytic activity in gastroduodenal ulcer haemorrhage and the beneficial effect of acid suppression. Aliment Pharmacol Ther. 2001;15:639–646.
Violl F, Basili S, Ferro D, Quintarelli C, Alessandril C, Cordova C. Association between high values of D-dimer and tissue-plasminogen activator activity and first gastrointestinal bleeding in cirrhotic patients. CALC Group. Thromb Haemost. 1996;76:177–183.
Gutiérrez A, Sánchez-Payá J, Marco P, Pérez-Mateo M. Prognostic value of fibrinolytic tests for hospital outcome in patients with acute upper gastrointestinal hemorrhage. J Clin Gastroenterol. 2001;32:315–318.
Anchu AC, Mohsina S, Sureshkumar S, Mahalakshmy T, Kate V. External validation of scoring systems in risk stratification of upper gastrointestinal bleeding. Indian J Gastroenterol. 2017;36:105–112.
Mokhtare M, Bozorgi V, Agah S, et al. Comparison of Glasgow–Blatchford score and full Rockall score systems to predict clinical outcomes in patients with upper gastrointestinal bleeding. Clin Exp Gastroenterol. 2016;9:337–343.
Stanley AJ, Laine L, Dalton HR, et al. Comparison of risk scoring systems for patients presenting with upper gastrointestinal bleeding: international multicentre prospective study. BMJ. 2017;356:i6432.
Zhong M, Chen WJ, Lu XY, Qian J, Zhu CQ. Comparison of three scoring systems in predicting clinical outcomes in patients with acute upper gastrointestinal bleeding: a prospective observational study. J Dig Dis. 2016;17:820–828.
Stanley AJ. Update on risk scoring systems for patients with upper gastrointestinal haemorrhage. World J Gastroenterol. 2012;18:2739–2744.
Yaka E, Yılmaz S, Doğan NÖ, Pekdemir M. Comparison of the Glasgow–Blatchford and AIMS65 scoring systems for risk stratification in upper gastrointestinal bleeding in the emergency department. Acad Emerg Med. 2015;22:22–30.
Laine L, Jensen DM. Management of patients with ulcer bleeding. Am J Gastroenterol. 2012;107:345–360.
Han YJ, Cha JM, Park JH, et al. Successful endoscopic hemostasis is a protective factor for rebleeding and mortality in patients with nonvariceal upper gastrointestinal bleeding. Dig Dis Sci. 2016;61:2011–2018. https://doi.org/10.1007/s10620-016-4082-9.
Cieniawski D, Kuzniar E, Winiarski M, Matlok M, Kostarczyk W, Pedziwiatr M. Prognostic value of the Rockall score in patients with acute nonvariceal bleeding from the upper gastrointestinal tract. Przegladlekarski. 2012;70:1–5.
Yang HM, Jeon SW, Jung JT, et al. Comparison of scoring systems for nonvariceal upper gastrointestinal bleeding: a multicenter prospective cohort study. J Gastroenterol Hepatol. 2016;31:119–125.
Acknowledgments
This work was supported by Grants from the National Natural Science Foundation of China (No. 81630016, to Jie Liu).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yue, W., Liu, Y., Jiang, W. et al. Prealbumin and D-dimer as Prognostic Indicators for Rebleeding in Patients with Nonvariceal Upper Gastrointestinal Bleeding. Dig Dis Sci 66, 1949–1956 (2021). https://doi.org/10.1007/s10620-020-06420-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06420-1