Abstract
Background and Aims
Vitamin D deficiency in patients with inflammatory bowel disease (IBD) is associated with greater disease activity and lower quality of life. Intestinal fibrosis is a main complication of IBD. However, the effect of vitamin D on intestinal fibrosis remains unclear. We investigated the prophylactic effect and the underlying mechanism of vitamin D on the intestinal fibrosis in vitamin D-deficient mice with chronic colitis.
Methods
Vitamin D-deficient mice were randomized into two groups receiving the vitamin D-deficient or vitamin D-sufficient diet from weaning (week 4). Intestinal fibrosis was induced by six-weekly 2,4,6-trinitrobenzene sulfonic acid administrations from week 8. At week 14, the productions of extracellular matrix (ECM) and total collagen were measured in the colons, and TGF-β1/Smad3 signal transduction was examined in isolated colonic subepithelial myofibroblasts (SEMF). The expression of vitamin D receptor (VDR), α-SMA and Collagen I in normal SEMF and VDR-null SEMF exposed to TGF-β1 and/or 1,25(OH)2D3 was measured.
Results
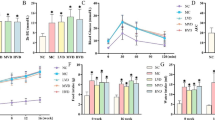
Vitamin D significantly reduced the histological scoring, ECM and collagen productions in the colons and decreased the levels of TGF-β1, Smad-3, p-Smad3 and Collagen I in SEMF. 1,25(OH)2D3-induced VDR expression and decreased TGF-β1-stimulated α-SMA and Collagen I expressions in SEMF. Knocking down VDR expression in SEMF abolished the effect of 1,25(OH)2D3.
Conclusions
Vitamin D has prophylactic effect on intestinal fibrosis in the vitamin D-deficient mice with chronic colitis, which may be associated with the inhibited activation of TGF-β1/Smad3 pathway in the SEMF via VDR induction.






Similar content being viewed by others
Abbreviations
- IBD:
-
Inflammatory bowel disease
- CD:
-
Crohn’s disease
- SEMF:
-
Subepithelial myofibroblasts
- VDR:
-
Vitamin D receptor
- ECM:
-
Extracellular matrix
- α-SMA:
-
α-Smooth muscle actin
- p-Smad3:
-
Smad3 phosphorylation
- Vit D:
-
Vitamin D
References
Malabanan A, Veronikis IE, Holick MF. Redefining vitamin D insufficiency. Lancet. 1998;351:805–806.
Ananthakrishnan AN. Environmental risk factors for inflammatory bowel disease. Gastroenterol Hepatol. 2013;9:367–374.
Ulitsky A, Ananthakrishnan AN, Naik A, et al. Vitamin D deficiency in patients with inflammatory bowel disease: association with disease activity and quality of life. J Parenter Enter Nutr. 2011;35:308–316.
Miheller P, Muzes G, Hritz I, et al. Comparison of the effects of 1,25 dihydroxyvitamin D and 25 hydroxyvitamin D on bone pathology and disease activity in Crohn’s disease patients. Inflamm Bowel Dis. 2009;15:1656–1662.
Rieder F, Fiocchi C. Intestinal fibrosis in IBD—a dynamic, multifactorial process. Nat Rev Gastroenterol Hepatol. 2009;6:228–235.
Ding N, Yu RT, Subramaniam N, et al. A vitamin D receptor/SMAD genomic circuit gates hepatic fibrotic response. Cell. 2013;153:601–613.
Ito I, Waku T, Aoki M, et al. A nonclassical vitamin D receptor pathway suppresses renal fibrosis. J Clin Investig. 2013;123:4579–4594.
Zhang Y, Kong J, Deb DK, Chang A, Li YC. Vitamin D receptor attenuates renal fibrosis by suppressing the renin-angiotensin system. J Am Soc Nephrol.. 2010;21:966–973.
De Silva P, Ananthakrishnan AN. Vitamin D and IBD: more pieces to the puzzle, still no complete picture. Inflamm Bowel Dis. 2012;18:1391–1393.
Andoh A, Bamba S, Brittan M, Fujiyama Y, Wright NA. Role of intestinal subepithelial myofibroblasts in inflammation and regenerative response in the gut. Pharmacol Ther. 2007;114:94–106.
Mora JR, Iwata M, von Andrian UH. Vitamin effects on the immune system: vitamins A and D take centre stage. Nat Rev Immunol. 2008;8:685–698.
Li YC. Investigating the role of vitamin D in IBD pathophysiology and treatment. Gastroenterol Hepatol. 2008;4:20–21.
Reagan-Shaw S, Nihal M, Ahmad N. Dose translation from animal to human studies revisited. FASEB J Off Publ Fed Am Soc Exp Biol. 2008;22:659–661.
Kuwata T, Wang IM, Tamura T, et al. Vitamin A deficiency in mice causes a systemic expansion of myeloid cells. Blood. 2000;95:3349–3356.
Lawrance IC, Wu F, Leite AZ, et al. A murine model of chronic inflammation-induced intestinal fibrosis down-regulated by antisense NF-kappa B. Gastroenterology. 2003;125:1750–1761.
Chakravarti S, Magnuson T, Lass JH, Jepsen KJ, LaMantia C, Carroll H. Lumican regulates collagen fibril assembly: skin fragility and corneal opacity in the absence of lumican. J Cell Biol. 1998;141:1277–1286.
Neurath MF, Fuss I, Kelsall BL, Stuber E, Strober W. Antibodies to interleukin 12 abrogate established experimental colitis in mice. J Exp Med. 1995;182:1281–1290.
Hogaboam CM, Chensue SW, Steinhauser ML, et al. Alteration of the cytokine phenotype in an experimental lung granuloma model by inhibiting nitric oxide. J Immunol. 1997;159:5585–5593.
Tao QS, Ren JA, Li JS. Triptolide suppresses IL-1beta-induced chemokine and stromelysin-1 gene expression in human colonic subepithelial myofibroblasts. Acta Pharmacol Sin. 2007;28:81–88.
Mahida YR, Beltinger J, Makh S, et al. Adult human colonic subepithelial myofibroblasts express extracellular matrix proteins and cyclooxygenase-1 and -2. Am J Physiol. 1997;273:G1341–G1348.
Paulin D, Li Z. Desmin: a major intermediate filament protein essential for the structural integrity and function of muscle. Exp Cell Res. 2004;301:1–7.
Fichtner-Feigl S, Fuss IJ, Young CA, et al. Induction of IL-13 triggers TGF-beta1-dependent tissue fibrosis in chronic 2,4,6-trinitrobenzene sulfonic acid colitis. J Immunol. 2007;178:5859–5870.
Liu W, Chen Y, Golan MA, et al. Intestinal epithelial vitamin D receptor signaling inhibits experimental colitis. J Clin Investig. 2013;123:3983–3996.
Lagishetty V, Misharin AV, Liu NQ, et al. Vitamin D deficiency in mice impairs colonic antibacterial activity and predisposes to colitis. Endocrinology. 2010;151:2423–2432.
Kong J, Zhang Z, Musch MW, et al. Novel role of the vitamin D receptor in maintaining the integrity of the intestinal mucosal barrier. Am J Physiol Gastrointest Liver Physiol. 2008;294:G208–G216.
Hart AL. Vitamin D and inflammatory bowel disease: chicken or egg? Inflamm Bowel Dis. 2013;19:459–460.
Cantorna MT, Zhu Y, Froicu M, Wittke A. Vitamin D status, 1,25-dihydroxyvitamin D3, and the immune system. Am J Clin Nutr. 2004;80:1717S–1720S.
Cantorna MT. Mechanisms underlying the effect of vitamin D on the immune system. Proc Nutr Soc. 2010;69:286–289.
Adorini L, Penna G. Control of autoimmune diseases by the vitamin D endocrine system. Nat Clin Pract Rheumatol. 2008;4:404–412.
Gocek E, Kielbinski M, Marcinkowska E. Activation of intracellular signaling pathways is necessary for an increase in VDR expression and its nuclear translocation. FEBS Lett. 2007;581:1751–1757.
Pramanik R, Asplin JR, Lindeman C, Favus MJ, Bai S, Coe FL. Lipopolysaccharide negatively modulates vitamin D action by down-regulating expression of vitamin D-induced VDR in human monocytic THP-1 cells. Cell Immunol. 2004;232:137–143.
Vallance BA, Gunawan MI, Hewlett B, et al. TGF-beta1 gene transfer to the mouse colon leads to intestinal fibrosis. Am J Physiol Gastrointest Liver Physiol. 2005;289:G116–G128.
Heldin CH, Miyazono K, ten Dijke P. TGF-beta signalling from cell membrane to nucleus through SMAD proteins. Nature. 1997;390:465–471.
Nakao A, Afrakhte M, Moren A, et al. Identification of Smad7, a TGFbeta-inducible antagonist of TGF-beta signalling. Nature. 1997;389:631–635.
Acknowledgments
This study was supported by grants from National Foundation for Natural Scientific Research of China (No 81000153) and Foundation for Natural Scientific Research of Jiangsu Province (BK2010415).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tao, Q., Wang, B., Zheng, Y. et al. Vitamin D Prevents the Intestinal Fibrosis Via Induction of Vitamin D Receptor and Inhibition of Transforming Growth Factor-Beta1/Smad3 Pathway. Dig Dis Sci 60, 868–875 (2015). https://doi.org/10.1007/s10620-014-3398-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-014-3398-6