Abstract
Introduction
Breast conserving surgery of impalpable breast lesions requires safe and effective localisation techniques. Wire localisation has traditionally been used, but has limitations. Newer techniques are now being introduced to mitigate this. The iBRA-NET group aims to robustly evaluate these new techniques in well-designed prospective studies. We report the first phase of this evaluation, a survey to establish current practice and service provision of breast localisation techniques in the UK.
Methods
A national practice questionnaire was designed using ‘SurveyMonkey®’ and was circulated to UK breast surgeons via the Association of Breast Surgery and the Mammary Fold. The questionnaire was live from 6th October 2018 to 6th April 2019. Only one response per unit was requested to reflect the unit’s practice.
Results
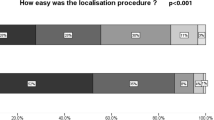
Complete responses were received from 98 breast units across the UK. Wires were the mostly commonly used localisation technique (n = 82) with fewer units using Magseed® (n = 9), Radioguided Occult Lesion Localisation (n = 5) and Radioiodine Seed Localisation (n = 2). There was significant variation in practice and logistics involved. Frequent delays and theatre overruns were reported in 39 and 16 units, respectively. The median satisfaction score of the current technique was 7 out of 10. The main perceived limitation of existing localisation methods was logistics affecting theatre scheduling and the main barrier to introducing a new technique was cost.
Conclusion
Wires are currently the most commonly used localisation technique but are associated with significant logistical issues. Newer techniques may offer a better solution but will need robust evaluation before they are adopted to ensure safety and efficacy.

Similar content being viewed by others
References
Welch HG, Prorok PC, O’Malley AJ, Kramer BS (2016) Breast-cancer tumor size, overdiagnosis, and mammography screening effectiveness. N Engl J Med 375:1438–1447. https://doi.org/10.1056/NEJMoa1600249
Golshan M, Cirrincione CT, Sikov WM, Berry DA, Jasinski S, Weisberg TF et al (2015) Impact of neoadjuvant chemotherapy in Stage II–III triple negative breast cancer on eligibility for breast-conserving surgery and breast conservation rates. Ann Surg 262:434–439. https://doi.org/10.1097/SLA.0000000000001417
Golshan M, Cirrincione CT, Sikov WM, Carey LA, Berry DA, Overmoyer B et al (2016) Impact of neoadjuvant therapy on eligibility for and frequency of breast conservation in stage II-III HER2-positive breast cancer: surgical results of CALGB 40601 (Alliance). Breast Cancer Res Treat 160:297–304. https://doi.org/10.1007/s10549-016-4006-6
Franceschini G, Di Leone A, Natale M, Sanchez MA, Masett R (2018) Conservative surgery after neoadjuvant chemotherapy in patients with operable breast cancer. Ann Ital Chir 89:290
Dodd GD, Fry K, Delany W (1965) Preoperative localization of occult carcinoma of the breast. In: Nealon TF (ed) Management of the patient with cancer. Saunders, Philadelphia, pp 88–113
Rahusen FD, Bremers AJA, Fabry HFJ, van Amerongen AHMT, Boom RPA, Meijer S (2002) Ultrasound-guided lumpectomy of nonpalpable breast cancer versus wire-guided resection: a randomized clinical trial. Ann Surg Oncol 9:994–998
Lovrics PJ, Goldsmith CH, Hodgson N, McCready D, Gohla G, Boylan C et al (2011) A multicentered, randomized, controlled trial comparing radioguided seed localization to standard wire localization for nonpalpable, invasive and in situ breast carcinomas. Ann Surg Oncol 18:3407–3414. https://doi.org/10.1245/s10434-011-1699-y
Rampaul RS, Bagnall M, Burrell H, Pinder SE, Evans AJ, Macmillan RD (2004) Randomized clinical trial comparing radioisotope occult lesion localization and wire-guided excision for biopsy of occult breast lesions. Br J Surg 91:1575–1577. https://doi.org/10.1002/bjs.4801
Sajid MS, Parampalli U, Haider Z, Bonomi R (2012) Comparison of radioguided occult lesion localization (ROLL) and wire localization for non-palpable breast cancers: a meta-analysis. J Surg Oncol 105:852–858. https://doi.org/10.1002/jso.23016
Sharek D, Zuley ML, Zhang JY, Soran A, Ahrendt GM, Ganott MA (2015) Radioactive seed localization versus wire localization for lumpectomies: a comparison of outcomes. Am J Roentgenol 204:872–877. https://doi.org/10.2214/AJR.14.12743
Pavlicek W, Walton HA, Karstaedt PJ, Gray RJ (2006) Radiation safety with use of I-125 seeds for localization of nonpalpable breast lesions. Acad Radiol 13:909–915. https://doi.org/10.1016/J.ACRA.2006.03.017
Jakub J, Gray R (2015) Starting a radioactive seed localization program. Ann Surg Oncol 22:3197–3202. https://doi.org/10.1245/s10434-015-4719-5
Mayo RC, Kalambo MJ, Parikh JR (2019) Preoperative localization of breast lesions: current techniques. Clin Imaging 56:1–8. https://doi.org/10.1016/j.clinimag.2019.01.013
Gulland A (2016) Staff shortages are putting UK breast cancer screening “at risk”, survey finds. BMJ 353:i2350. https://doi.org/10.1136/bmj.i2350
Hayes MK (2017) Update on preoperative breast localization. Radiol Clin North Am 55:591–603. https://doi.org/10.1016/j.rcl.2016.12.012
Acknowledgements
Prof. Chris Holcombe, Royal Liverpool University Hospital, for contributions to the design of the national practice questionnaire
Funding
Association of Breast Surgery grant awarded to Mr. James Harvey to conduct this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Not applicable.
Research involving human participants and/or animals
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Somasundaram, S.K., Potter, S., Elgammal, S. et al. Impalpable breast lesion localisation, a logistical challenge: results of the UK iBRA-NET national practice questionnaire. Breast Cancer Res Treat 185, 13–20 (2021). https://doi.org/10.1007/s10549-020-05918-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-020-05918-6