Abstract
Purpose
To report the use of hyperdried cross-linked (HDCL) amniotic membrane (AM) patching with tissue adhesive as an initial therapy for corneal perforations.
Methods
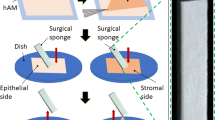
Cryopreserved AM was cross-linked with 0.1% glutaraldehyde and then dried using far-infrared rays and microwaves (hyperdry method). Three eyes of three patients with corneal perforations of up to 3 mm in diameter were included in this study. They were treated with a single-layer patch of HDCL-AM applied with a tissue adhesive (2-octyl-cyanoacrylate). We also evaluated the resistance of HDCL-AM to collagenases during in vitro digestion testing.
Results
In all three cases, the corneal perforations were repaired within 28 days (range, 17–28 days). No recurrence occurred during the follow-up period (3–6 months). In the collagenase digestion testing, the HDCL-AM did not dissolve until 48 h, whereas the cryopreserved AM completely dissolved within 60 min.
Conclusions
Three cases of corneal perforations were successfully managed using HDCL-AM patching with tissue adhesive. The HDCL-AM was resistant to collagenases during in vitro digestion testing. The HDCL-AM was a useful substrate for corneal perforations. This simple surgical technique may be one of the initial therapeutic options for corneal perforations.
Similar content being viewed by others
References
Hanada K, Shimazaki J, Shimmura S, Tsubota K. Multilayered amniotic membrane transplantation for severe ulceration of the cornea and sclera. Am J Ophthalmol 2001;131:324–331.
Prabhasawat P, Tesavibul N, Komolsuradej W. Single and multilayer amniotic membrane transplantation for persistent corneal epithelial defect with and without stromal thinning and perforation. Br J Ophthalmol 2001;85:1455–1463.
Chen HC, Tan HY, Hsiao CH, Huang SC, Lin KK, Ma DH. Amniotic membrane transplantation for persistent corneal ulcers and perforations in acute fungal keratitis. Cornea 2006;25:564–572.
Dua HS, Gomes JAP, King AJ, Maharajan SM. Amniotic membrane in ophthalmology. Surv Ophthalmol 2004;49:51–77.
Anderson RE, Kuns MD, Dresden MH. Collagenase activity in alkali-burned cornea. Ann Ophthalmol 1971;3:619–621.
Riley GP, Harrall RL, Watson PG, Cawston TE, Hazleman BL. Collagenase (MMP-1) and TIMP-1 in destructive ocular disease associated with rheumatoid arthritis. Eye 1995;9:703–718.
Vadillo-Ortega F, Gonzalez-Avila G, Chevez P, Abraham CR, Montano M, Selman-Lama M. A latent collagenase in human aqueous humor. Invest Ophthalmol Vis Sci 1989;30:332–335.
Berman MB. Collagenase inhibitors: rationale for their use in treating corneal ulcers. Int Ophthalmol Clin 1975;15:49–66.
Spoerl E, Wollensak G, Reber F, Pillunat L. Cross-linking of human amniotic membrane by glutaraldehyde. Ophthalmic Res 2004;36:71–77.
Toda A, Okabe M, Yoshida T, Nikaido T. The potential of amniotic membrane/amnion-derived cells for regeneration of various tissues. J Pharmacol Sci 2007;105:215–228.
Kitagawa K, Yanagisawa S, Watanabe K, et al. A hyperdry amniotic membrane patch using a tissue adhesive for corneal perforations and bleb leaks. Am J Ophthalmol 2009;148:383–389.
Lee S-H, Tseng SCG. Amniotic membrane transplantation for persistent epithelial defects with ulceration. Am J Ophthalmol 1997;23:303–312.
Fujisato T, Tomihara K, Tabata Y, Iwamoto Y, Burczak K, Ikada Y. Cross-linking of amniotic membranes. J Biomater Sci Polym Ed 1999;10:1171–1181.
Ballantyne B, Myers RC. The acute toxicity and primary irritancy of glutaraldehyde solutions. Vet Hum Toxicol 2001;43:193–202.
Rodriquez-Ares MT, Tourino R, Lopez-Valladares MJ, Gude F. Multilayer amniotic membrane transplantation in the management of corneal perforations. Cornea 2004;23:577–583.
Hick S, Demers PE, Brunette I, La C, Mabon M, Duchesne B. Amniotic membrane transplantation and fibrin glue in the management of corneal ulcers and perforations: a review of 33 cases. Cornea 2005;24:369–377.
Kim HK, Park HS. Fibrin glue-assisted augmented amniotic membrane transplantation for the treatment of large noninfectious corneal perforations. Cornea 2009;28:170–176.
Taravella MJ, Chang CD. 2-Octyl-cyanoacrylate medical adhesive in treatment of a corneal perforation. Cornea 2001;20:220–221.
Kim YM, Gupta BK. 2-Octyl cyanoacrylate adhesive for conjunctival wound closure in rabbits. J Pediatr Ophthalmol Strabismus 2003;40:152–155.
Bloomfield S, Bamert AH, Kanter P. The use of Eastman-910 monomer as an adhesive in ocular surgery. II. Effectiveness in closure of limbal wounds in rabbits. Am J Ophthalmol 1963;55:946–953.
Lin DT, Webster RG Jr, Abbot RL. Repair of corneal lacerations and perforations. Int Ophthalmol Clin 1988;28:69–75.
Aronson SB, McMaster PR, Moore TE Jr, Coon MA. Toxicology of the cyanoacrylates. Arch Ophthalmol 1970;84:342–349.
Sharma A, Kaur R, Kumar S, et al. Fibrin glue versus N-butyl-2-cyanoacrylate in corneal perforations. Ophthalmology 2003;110: 291–298.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Kitagawa, K., Okabe, M., Yanagisawa, S. et al. Use of a hyperdried cross-linked amniotic membrane as initial therapy for corneal perforations. Jpn J Ophthalmol 55, 16–21 (2011). https://doi.org/10.1007/s10384-010-0903-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-010-0903-0