Abstract
We evaluated the long-term glycemic control in children with type 1 diabetes, using continuous subcutaneous insulin infusion (CSII) for at least 5 years in three diabetes centers from three different countries: Canada, Italy and Spain. This was an observational retrospective multicenter cohort study. Subjects were included if they were followed at one of the participating centers, had type 1 diabetes, age 5–20 years at time of data collection and used CSII for more than 5 years. Data collected included gender, age, disease duration, age at CSII initiation, body mass index (BMI), hemoglobin A1c (HbA1c), insulin requirement and serious adverse events (SAE) at baseline and every 12 months during follow-up. One hundred fifteen patients were included in the study (55 % males), aged 5–20 years (mean: 13.5 ± 3.8 years), with mean diabetes duration of 6.3 ± 3.4 years, using CSII for mean of 6.9 ± 1.2 years (range 5–12 years.). HbA1c significantly improved after 1 year of CSII treatment and during follow-up (p = 0.02). When HbA1c was compared between countries, a difference was observed, with slightly lower values in Italy than in Canada and Spain (p = 0.04). When evaluated by gender, HbA1c was similar at baseline, but significantly improved only in males during all follow-up (p = 0.004). No significant differences were observed for BMI, insulin requirement or SAE. Insulin pump therapy is safe and effective in the pediatric population, although in this study, the major benefit in HbA1c was seen in males. The use of advanced pump features was associated with greater improvement in HbA1c.
Similar content being viewed by others
Introduction
Intensive insulin therapy may prevent or delay the progression of microvascular disease in patients with type 1 and type 2 diabetes [1, 2]. Furthermore, the Epidemiology of Diabetes Interventions and Complications study [3] established the fact that early control of diabetes will allow for continued protection against both microvascular and macrovascular complications 18 years after the Diabetes Control and Complications Trial (DCCT) was completed.
In children with type 1 diabetes, optimal glycemic control enhances growth and ensures normal pubertal development. Insulin pump therapy (CSII) represents an important advancement in diabetes technology that can facilitate optimal glycemic control in both adults [4] and children [5] with type 1 diabetes.
CSII is intensive insulin therapy which attempts to mimic physiologic insulin release by administration of a 24-h adjustable basal rate and flexible mealtime bolus doses [6].
While the benefits of CSII in the short term have been demonstrated [7], especially in adults and when using sensor-augmented pump [8], long-term (over 4 years) follow-up studies are still limited [9–14] and often have few patients.
The purpose of the present study has been to evaluate the usefulness and safety of insulin pump therapy in a large cohort of pediatric patients with type 1 diabetes mellitus, during 7-year follow-up, in 3 diabetes centers from 3 different countries: Canada, Italy and Spain (InPuTLog Study—Insulin Pump Therapy in the LOnG-term Study).
Methods
This was an observational retrospective multicenter cohort study. Each of the three centers participating in the study was tertiary care specialty clinics for the management of pediatric diabetes with long-term experience in CSII: Ospedale Luigi Sacco (Milano, Italy), Alberta Children’s Hospital (Calgary, Canada) and Hospital Sant Joan de Déu (Barcelona, Spain).
Inclusion criteria were as follows: patients followed in the participating pediatric diabetes centers, diagnosis of type 1 diabetes, age 5–20 years at the time of data collection and use of CSII for at least 5 years or more. Patients were excluded if they had other underlying conditions that could affect glycemic control, for example, uncontrolled thyroid disease, steroid usage, etc.
The study was approved by the local ethics committee at each participating center. The study was conducted according to the Declaration of Helsinki.
Data collection was conducted between January 2011 and December 2011. Chart reviews were conducted by a site investigator for each center and included the following data: date of birth, date of onset of diabetes, the age at which the pump therapy began, hemoglobin A1c (HbA1c), insulin requirement (U/kg/day), body mass index (BMI) and serious adverse events [severe hypoglycemia and diabetic ketoacidosis (DKA)]. Data were collected at CSII initiation and yearly throughout the follow-up. The usage of bolus calculator (BC), the number of boluses made with BC, the usage of different type of boluses (e.g., double-wave bolus, square-wave bolus) and the usage of temporary basal were also recorded when available. HbA1c determination was done in all three countries according to DCCT method [1].
Severe hypoglycemia was defined as an episode that required assistance from another person and preferably was accompanied by a confirmatory blood glucose value <50 mg/dl (<2.8 mmol/l). DKA was defined as blood glucose >250 mg/dl (>13.9 mmol/l) with either low serum bicarbonate (<15 mEq/l) or low pH (<7.3) and either ketonemia or ketonuria and requiring treatment within a health-care facility. Episodes of severe hypoglycemia and DKA were documented in an electronic health record in Canada and Italy; while in Spain, a structured, written health record was used to document these events.
The primary endpoint was the change in HbA1c between baseline and yearly throughout the follow-up. We also evaluated insulin requirement, BMI, serious adverse events and advanced pump features.
Continuous variables are displayed as frequencies or percentages. t-test, chi-square test and Fisher’s exact test were used to compare groups. ANOVA and paired t-test was used to analyze changes of continuous variables over time. A level of 0.05 determined statistical significance.
Results
Among the centers, we identified 121 patients with type 1 diabetes that met the inclusion criteria. After a careful evaluation of the data, 6 patients were excluded due to incomplete data available on the chart. The final analysis included 115 patients (mean age 13.5 ± 3.8 years, range 5–20 years; mean duration of diabetes 6.3 ± 3.4 years, range 0.6–14.5 years; mean follow-up period 6.9 ± 1.7 years, range 5–12 years).
Characteristics of all patients evaluated at baseline (CSII start) and at the last visit are summarized in Table 1.
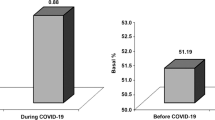
Data were analyzed as a group as well as by country and gender. HbA1c significantly improve after 1-year follow-up, showing a positive trend throughout the follow-up (p = 0.02) (Fig. 1a). When evaluating HbA1c according to different countries, HbA1c significantly improved after 1-year follow-up and showed different trends in each country (Fig. 1b). Interestingly, a significant difference has been observed between females and males in HbA1c values after 1-year follow-up and throughout all the follow-up (Fig. 1c).
(a) HbA1c values at baseline and throughout the follow-up in all pediatric subjects enrolled in the final analysis (n = 115). Data are expressed as mean ± standard deviation. Significant differences between baseline and each time point are shown. Analysis was done by Student’s t-test for paired data. (b) HbA1c values at baseline and throughout the follow-up according to different countries. Data are expressed as mean ± standard deviation. Significant differences between baseline and each time point among countries are shown. Analysis was done by ANOVA. (c) HbA1c values at baseline and throughout the follow-up according to gender. Data are expressed as mean ± standard deviation. Significant differences at baseline and each time point between genders are shown. Analysis was done by Student’s t-test for unpaired data
No differences were observed regarding insulin requirement neither at baseline nor throughout the follow-up, in the whole group, or according to country or gender.
BMI increased accordingly throughout the follow-up, matching the increase in both height and weight because of physiological growth in all children. However, when evaluated as BMI z-score, no difference has been observed at all. Interestingly, only at the last visit, we observed a significant higher BMI in girls when compared to boys (p = 0.032) (Table 1).
Severe hypoglycemia decreased from baseline to the end of follow-up (4 vs. 2.8 events/100 patient/years, p = ns). A significant difference was observed in DKA episodes during the follow-up (8.2 vs. 1.1 events/100 patient/years, p = 0.01).
We tested if different age (<13, 13–17, >17 years) or disease duration (<5 or >5 years) at CSII initiation had any influence on glycemic trend, and no association was found.
Lastly, a difference has been observed in a subgroup of patients (n = 60) using advanced features (BC, different boluses and temporary basal) when compared to patients that do not use them, with a significantly better HbA1c at the end of follow-up (7.82 ± 0.79 vs. 8.50 ± 0.80, p = 0.003). No difference was observed with insulin requirement and BMI between those who used advanced pump features and those who did not.
Discussion
After 7-year follow-up, CSII therapy seems an effective and safe therapy in children and adolescents with type 1 diabetes. This multicenter, international study including centers from Canada, Italy and Spain provides some new insights into CSII therapy in the pediatric population.
Although comparing the long-term follow-up of patients between three different centers from three different areas of the world may be difficult due to the non-homogeneous nature of the centers, there were still many important similarities between the sites. Prior to the study, each center completed a brief survey describing their diabetes team for CSII initiation and what approaches are followed. There was a little difference between the centers. All teams include a pediatric diabetologist, dietitian, psychologist and nurse; and in Spain and Canada, a social worker too. Prior to starting CSII, patients and their families need to participate in structured education programs entailing all aspects of insulin pump therapy (how the pump works, how to make insulin changes, carbohydrate counting, exercise, special occasions, how to manage hypo or hyperglycemia and illnesses, etc.). Initial education sessions were provided at CSII start and whenever the patient/families asked for a reinforcement.
Although the educational program pre-CSII was similar in all centers, there were some differences in the selection of patients for insulin pump therapy. Thus, it is possible to explain why HbA1c of patients in Spain was higher than that of Canadian or Italian ones. Moreover, as described in the literature [8], the higher the HbA1c at baseline, the greater the HbA1c decrease, especially in the first year of follow-up, as we have observed with patients from Spain when compared to patients from Canada and Italy.
It is harder to explain why we observed different glycemic trends among the 3 countries. Different dietary habits could be one explanation and deserve future investigation. Once again, different criteria for selection of patients for insulin pump initiation may also have contributed to the varied trends observed. The use of advanced pump features was associated with a significant improvement in HbA1c compared to those who did not use advanced pump features. This subgroup analysis only included patients from Italy and Spain since this information was not routinely recorded in the Canadian center’s chart. The use of advanced features of the pump, whose effectiveness has been shown [15–17] even if in the short run, needs to be reinforced, by ongoing education to the patients. Insulin pump therapy has the potential to mimic physiologic insulin secretion and should be tailored to the specific patient. For example, bolus timing [18, 19] or using different bolus for different meals [20] as this can improve glycemic control.
Although this study identified some statistically significant differences in HbA1c during the 7 years of uninterrupted insulin pump therapy, one could discuss whether these differences have clinical significance. The combined mean HbA1c of the three countries before pump versus after pump shows just a −0.04 % decrease in HbA1c which one could argue may not be cost-effective. When examining each country separately, HbA1c in Canada increased by +0.28 %, while Italy and Spain HbA1c decreased by −0.37 and −0.39 %, respectively, which is consistent with or even a bit better than previously published data [8–14]. Previous studies had a follow-up time from 1 to 4 years, while our data describe a 7-year observation time.
Other factors, such as a decrease in episodes of DKA and severe hypoglycemia as well as quality of life, need to be considered when reviewing the effectiveness of pump therapy in properly selected patients. A significant reduction in severe adverse events was seen following insulin pump initiation in our group. Quality of life measures were not done in the present study due to its retrospective nature, but further investigations would be useful. Indeed, in a recently published paper, Cherubini et al. [21] found that CSII therapy confers significant advantages in terms of health-related quality of life when compared to patients using multiple daily injections. Considering the non-randomized design of our study, we observe that our findings are in accordance with those already published in non-randomized trials [10, 14, 22–25].
Another interesting finding of our study was the significant difference observed between males and females regarding HbA1c (throughout the whole follow-up) and BMI (at the last visit). These findings are different from what Shalitin et al. [11] observed in their study, where the only difference between the two groups (females vs. males) was diabetes duration at CSII initiation, CSII duration and insulin requirement before CSII initiation. It is not clear in this study why males had better HbA1c values than females. The difficult relationship with their body and body image as well as the increased risk of depression could be a reason why HbA1c was more difficult to optimize in girls [26] and has been suggested as a risk factor for pump discontinuation [27]. In addition, the poorer HbA1c and significantly increased BMI in girls compared to boys may have had to do with the pubertal status of the girls given that the mean age of this cohort was 13.5 years. Unfortunately, Tanner staging was not routinely available in this retrospective review.
Insulin pump therapy is safe in the pediatric population not only after its initiation, as observed in large meta-analyses [4–6], but even after 7 years follow-up, as can be seen in the present study and other studies [9, 11, 12].
A limitation of the present study is its retrospective nature. Some things were not able to be assessed for the whole group, for example, advanced pump features and Tanner staging. Every effort was made to have a consistent and thorough evaluation of each chart by using a single-site investigator for the chart reviews and the final analysis only included those with complete data.
In conclusion, insulin pump therapy is safe and effective in the pediatric population, and in this study, the major benefit in HbA1c was seen in males. The use of advanced pump features was associated with greater improvement in HbA1c. Future prospective studies would be useful to evaluate the reasons for differences observed among the three countries such as different dietary habits, lifestyle and pump education.
References
The Diabetes Control Complication Trial (DCCT) Research Group (1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. New Engl J Med 329:977–986
UK Prospective Diabetes Study (UKPDS) Group (1998) Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes. Lancet 352:837–853
Nathan DM, Cleary PA, Backlund JY, Genuth SM, Lachin JM, Orchard TJ, Raskin P, Zinman B, Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications (DCCT/EDIC) Study Research Group (2005) Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes. N Engl J Med 353:2643–2652
Monami M, Lamanna C, Marchionni N, Mannucci E (2010) Continuous subcutaneous insulin infusion versus multiple daily insulin injections in type 1 diabetes: a meta-analysis. Acta Diabetol 47(Suppl 1):77–81
Misso ML, Egberts KJ, Page M, O’Connor D, Shaw J (2010) Continuous subcutaneous insulin infusion (CSII) versus multiple insulin injections for type 1 diabetes mellitus. Cochrane Database Syst Rev 20(1):CD005103
Weinzimer SA, Ternand C, Howard C, Chang CT, Becker DJ, Laffel LM, Insulin Aspart Pediatric Pump Study Group (2008) A randomized trial comparing continuous subcutaneous insulin infusion of insulin aspart versus insulin lispro in children and adolescents with type 1 diabetes. Diabetes Care 31:210–215
Ahern JA, Boland EA, Doane R, Ahern JJ, Rose P, Vincent M, Tamborlane WV (2002) Insulin pump therapy in pediatrics: a safe alternative to safely lower HbA1c levels across all age groups. Pediatr Diabetes 3:10–15
Yeh HC, Brown TT, Maruthur N et al (2012) Comparative effectiveness and safety of methods of insulin delivery and glucose monitoring for diabetes mellitus: a systematic review and meta-analysis. Ann Intern Med 157:336–347
Sulli N, Shashaj B (2006) Long-term benefits of continuous subcutaneous insulin infusion in children with Type 1 diabetes: a 4-year follow-up. Diabet Med 23:900–906
Scrimgeour L, Cobry E, McFann BS, Burdick P, Weimer C, Slover R, Chase HP (2007) Improved glycemic control after long-term insulin pump use in pediatric patients with type 1 diabetes. Diabetes Technol Ther 9:421–428
Shalitin S, Gil M, Nimri R, de Vries L, Gavan MY, Phillip M (2010) Predictors of glycemic control in patients with type 1 diabetes commencing continuous subcutaneous insulin infusion therapy. Diabet Med 27:339–347
Hughes CR, McDowell N, Cody D, Costigan C (2012) Sustained benefits of continuous subcutaneous insulin infusion. Arch Dis Child 97:245–247
Batajoo RJ, Messina CR, Wilson TA (2012) Long-term efficacy of insulin pump therapy in children with type 1 diabetes mellitus. J Clin Res Pediatr Endocrinol 4:127–131
Weinzimer SA, Ahern JH, Doyle EA, Vincent MR, Dziura J, Steffen AT, Tamborlane WV (2004) Persistence of benefits of continuous subcutaneous insulin infusion in very young children with type 1 diabetes: a follow-up study. Pediatrics 114:1601–1605
Walsh J, Roberts R, Bailey T (2011) Guidelines for optimal bolus calculator settings in adults. J Diabetes Sci Technol 5:129–135
O’Connell MA, Donath S, Cameron FJ (2011) Poor adherence to integral daily tasks limits the efficacy of CSII in youth. Pediatr Diabetes 12:556–559
Cukierman-Yaffe T, Konvalina N, Cohen O (2011) Key elements for successful intensive insulin pump therapy in individuals with type 1 diabetes. Diabetes Res Clin Pract 92:69–73
Scaramuzza AE, Iafusco D, Santoro L, Bosetti A, De Palma A, Spiri D, Mameli C, Zuccotti GV (2010) Timing of bolus in children with type 1 diabetes using continuous subcutaneous insulin infusion (TiBoDi Study). Diabetes Technol Ther 12:149–152
Luijf YM, van Bon AC, Hoekstra JB, DeVries JH (2010) Premeal injection of rapid-acting insulin reduces postprandial glycemic excursions in type 1 diabetes. Diabetes Care 33:2152–2155
De Palma A, Giani E, Iafusco D, Bosetti A, Macedoni M, Gazzarri A, Spiri D, Scaramuzza AE, Zuccotti GV (2011) Lowering postprandial glycemia in children with type 1 diabetes after Italian pizza ‘margherita’ (TyBoDi2 Study). Diabetes Technol Therap 13:483–487
Cherubini V, Gesuita R, Bonfanti R, Franzese A, Frongia AP, Iafusco D, Iannilli A, Lombardo F, Rabbone I, Sabbion A, Salvatoni A, Scaramuzza A, Schiaffini R, Sulli N, Toni S, Tumini S, Mosca A, Carle F; VIPKIDS Study Group. (2013) Health-related quality of life and treatment preferences in adolescents with type 1 diabetes. The VIPKIDS study. Acta Diabetol [Epub ahead of print]
Maniatis AK, Toig SR, Kingensmith GJ, Fay-Itzkowitz E, Chase HP (2001) Life with continuous subcutaneous insulin infusion (CSII) therapy: child and parental perspectives and predictors of metabolic control. Pediatr Diabetes 2:51–57
Ahern JA, Boland EA, Doane R, Ahern JJ, Vincent M, Tamborlane WV (2002) Insulin pump therapy in pediatrics: a therapeutic alternative to safely lower HbA1c levels across all age groups. Pediatr Diabetes 3:10–15
Plotnick LP, Clark LM, Brancati F, Erlinger T (2003) Diabetes Care 26:1142–1146
Willi SM, Planton J, Egede L, Schwarz S (2003) Benefits of continuous subcutaneous insulin infusion in children with type 1 diabetes. J Pediatr 143:796–801
De Wit M, Snoek FJ (2011) Depressive symptoms and unmet psychological needs of Dutch youth with type 1 diabetes: results of a web-survey. Pediatr Diabetes 12(3 pt 1):172–176
de Vries L, Grushka Y, Lebenthal Y, Shalitin S, Phillip M (2011) Factors associated with increased risk of insulin pump discontinuation in pediatric patients with type 1 diabetes. Pediatr Diabetes 12(5):506–512
Conflict of interest
A.E.S receives research support, and participates in advisory boards for Medtronic, no conflict of interest disclosed for this study; C.M., J.H., R.C.-H., L.S.-O., and G.V.Z. have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by Guido Pozza.
Rights and permissions
About this article
Cite this article
Mameli, C., Scaramuzza, A.E., Ho, J. et al. A 7-year follow-up retrospective, international, multicenter study of insulin pump therapy in children and adolescents with type 1 diabetes. Acta Diabetol 51, 205–210 (2014). https://doi.org/10.1007/s00592-013-0481-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-013-0481-y