Abstract
Introduction
Sarcopenia is a clinical syndrome characterized by the reduction in muscle mass, strength and physical ability. Although proximal femur fractures are one of the major burdens affecting the ageing population, distal radius fractures are equally important for frequency, clinical and social consequences. The aim of this study is to evaluate the incidence of sarcopenia in distal radius fractures and clinical implications in functional recovery.
Materials and methods
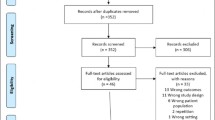
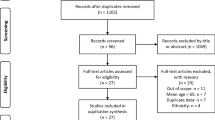
Scopus and PubMed search was performed to find relationship between sarcopenia and distal radius fractures. Literature search was performed between 2009 and 2019 including clinical trials and clinical studies related to “sarcopenia and distal radius fracture” and “sarcopenia and wrist fracture”. After identification, studies were screened and analysed through the Oxford Level of Evidence.
Results
According to the inclusion and exclusion criteria, five articles were included. Four articles analysed the incidence of sarcopenia and its role as a risk factor in patients with distal radial fractures, while one article focused on sarcopenia and clinical results of surgical treatment of distal radius fractures.
Incidence of sarcopenia in patients older than 50 years with distal radius fracture varied between 29.7% and 31.7%. Patients with distal radial fractures did not show a significant inferior muscle mass than control group in examined population. Functional results of surgery were significantly inferior in sarcopenic patients than control group (no sarcopenia).
Conclusions
About 30% of patients older than 50 years with distal radius fracture suffered by sarcopenia; sarcopenic patients surgically treated had worse clinical results than no sarcopenic patients. Further studies with larger samples are needed to confirm these preliminary results.

Similar content being viewed by others
References
Morley JE, Baumgartner RN, Roubenoff R et al (2001) Sarcopenia. J Lab Clin Med 137:231–243. https://doi.org/10.1067/mlc.2001.113504
Lang T, Streeper T, Cawthon P et al (2010) Sarcopenia: etiology, clinical consequences, intervention, and assessment. Osteoporos Int 21:543–559
Brioche T, Pagano AF, Py G, Chopard A (2016) Muscle wasting and aging: Experimental models, fatty infiltrations, and prevention. Mol Aspects Med 50:56–87. https://doi.org/10.1016/j.mam.2016.04.006
Crabtree NJ, Kibirige MS, Fordham JN et al (2004) The relationship between lean body mass and bone mineral content in paediatric health and disease. Bone 35:965–972. https://doi.org/10.1016/j.bone.2004.06.009
Tarantino U, Piccirilli E, Fantini M et al (2015) Sarcopenia and fragility fractures: molecular and clinical evidence of the bone-muscle interaction. J Bone Jt Surg-Am 97:429–437
Iolascon G, Di Pietro G, Gimigliano F et al (2014) Physical exercise and sarcopenia in older people: position paper of the Italian society of orthopaedics and medicine (OrtoMed). Clin Cases Miner Bone Metab 11:215–221. https://doi.org/10.11138/ccmbm/2014.11.3.215
Il YJ, Kim H, Ha YC et al (2018) Osteosarcopenia in patients with hip fracture is related with high mortality. J Korean Med Sci. https://doi.org/10.3346/jkms.2018.33.e27
Hong W, Cheng Q, Zhu X et al (2015) Prevalence of sarcopenia and its relationship with sites of fragility fractures in elderly Chinese men and women. PLoS ONE. https://doi.org/10.1371/journal.pone.0138102
Wu JC, Strickland CD, Chambers JS (2019) Wrist fractures and osteoporosis. Orthop Clin North Am 50:211–221
Wagner P, Chapurlat R, Ecochard R, Szulc P (2018) Low muscle strength and mass is associated with the accelerated decline of bone microarchitecture at the distal radius in older men: the prospective strambo study. J Bone Miner Res 33:1630–1640. https://doi.org/10.1002/jbmr.3456
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 62:e1–34. https://doi.org/10.1016/j.jclinepi.2009.06.006
Group OL of EW (2011) The Oxford 2011 levels of evidence
Roh YH, Do KY, Noh JH et al (2017) Evaluation of sarcopenia in patients with distal radius fractures. Arch Osteoporos. https://doi.org/10.1007/s11657-016-0303-2
Yoon B-H, Lee J-K, Choi D-S, Han S-H (2018) Prevalence and associated risk factors of sarcopenia in female patients with osteoporotic fracture. J Bone Metab. https://doi.org/10.11005/jbm.2018.25.1.59
Roh YH, Noh JH, Gong HS, Baek GH (2017) Effect of low appendicular lean mass, grip strength, and gait speed on the functional outcome after surgery for distal radius fractures. Arch Osteoporos. https://doi.org/10.1007/s11657-017-0335-2
Lee J-K, Yoon B-H, Oh CH et al (2018) Is sarcopenia a potential risk factor for distal radius fracture? analysis using propensity score matching. J bone Metab 25:99–106. https://doi.org/10.11005/jbm.2018.25.2.99
Hirschfeld HP, Kinsella R, Duque G (2017) Osteosarcopenia: where bone, muscle, and fat collide. Osteoporos Int 28:2781–2790
Levinger I, Phu S, Duque G (2016) Sarcopenia and osteoporotic fractures. Clin Rev Bone Miner Metab 14:38–44
Øyen J, Brudvik C, Gjesdal CG et al (2011) Osteoporosis as a risk factor for distal radial fractures: a case-control study. J Bone Jt Surg - Ser A 93:348–356. https://doi.org/10.2106/JBJS.J.00303
Fitzpatrick SK, Casemyr NE, Zurakowski D et al (2012) The effect of osteoporosis on outcomes of operatively treated distal radius fractures. J Hand Surg Am 37:2027–2034. https://doi.org/10.1016/j.jhsa.2012.06.025
Roh YH, Lee BK, Noh JH et al (2014) Factors delaying recovery after volar plate fixation of distal radius fractures. J Hand Surg Am 39:1465–1470. https://doi.org/10.1016/j.jhsa.2014.04.033
Choi WS, Lee HJ, Kim DY et al (2015) Does osteoporosis have a negative effect on the functional outcome of an osteoporotic distal radial fracture treated with a volar locking plate? Bone Jt J 97:229–234. https://doi.org/10.1302/0301-620X.97B2.34613
Funding
No funding was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflict of interest related to the topic of the manuscript.
Ethics approval
No ethical approval is needed for this type of manuscript.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Artiaco, S., Fusini, F., Pennacchio, G. et al. Sarcopenia in distal radius fractures: systematic review of the literature and current findings. Eur J Orthop Surg Traumatol 30, 1251–1255 (2020). https://doi.org/10.1007/s00590-020-02697-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-020-02697-0