Abstract
Background
To investigate the long-term neurodevelopmental outcome in children after hemolytic uremic syndrome (HUS) and to compare outcome dependent on central nervous system (CNS) involvement during HUS.
Methods
A single-center retrospective cohort of 47 children was examined at a median age of 10.6 (range 6–16.9) years and a median follow-up of 7.8 (range 0.4–15.3) years after having had HUS. Intellectual performance was assessed with the German version of the Wechsler Intelligence Scale 4th version and neuromotor performance with the Zurich Neuromotor Assessment (ZNA). The occurrence of neurological symptoms during the acute phase of HUS was evaluated retrospectively.
Results
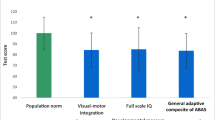
Mean IQ of the whole study population fell within the normal range (median full scale IQ 104, range 54–127). Neuromotor performance was significantly poorer in the domains “adaptive fine,” “gross motor,” “static balance” (all p < 0.05) and “associated movements” (p < 0.001); only the “pure motor” domain was within the normal reference range. Neurological findings occurred in 16/47 patients (34 %) during acute HUS. Neurodevelopmental outcome was not significantly different between children with or without CNS involvement.
Conclusions
Our follow-up of children after HUS showed a favorable cognitive outcome. However, neuromotor outcome was impaired in all study participants. Neurological impairment during acute HUS was not predictive of outcome.
Similar content being viewed by others
References
Andreoli SP (2009) Acute kidney injury in children. Pediatr Nephrol 24:253–263
Schifferli A, von Vigier RO, Fontana M, Spartà G, Schmid H, Bianchetti MG, Rudin C, (SPSU) TSPSU (2010) Hemolytic-uremic syndrome in Switzerland: a nationwide surveillance 1997–2003. Eur J Pediatr 169:591–598
Garg AX, Suri RS, Barrowman N, Rehman F, Matsell D, Rosas-Arellano MP, Salvadori M, Haynes RB, Clark WF (2003) Long-term renal prognosis of diarrhea-associated hemolytic uremic syndrome: a systematic review, meta-analysis, and meta-regression. JAMA 290:1360–1370
Copelovitch L, Kaplan BS (2008) Streptococcus pneumoniae-associated hemolytic uremic syndrome. Pediatr Nephrol 23:1951–1956
Fremeaux-Bacchi V, Fakhouri F, Garnier A, Bienaime F, Dragon-Durey M-A, Ngo S, Moulin B, Servais A, Provot F, Rostaing L, Burtey S, Niaudet P, Deschenes G, Lebranchu Y, Zuber J, Loirat C (2013) Genetics and outcome of atypical hemolytic uremic syndrome: a nationwide French series comparing children and adults. Clin J Am Soc Nephrol 8:554–562
Noris M, Remuzzi G (2009) Atypical hemolytic-uremic syndrome. N Engl J Med 361:1676–1687
Loirat C, Saland J, Bitzan M (2012) Management of hemolytic uremic syndrome. Presse Med 41:e115–e135
Scheiring J, Rosales A, Zimmerhackl LB (2010) Clinical practice. Today’s understanding of the haemolytic uraemic syndrome. Eur J Pediatr 169:7–13
Rosales A, Hofer J, Zimmerhackl L-B, Jungraithmayr TC, Riedl M, Giner T, Strasak A, Orth-Höller D, Würzner R, Karch H, Group G-AHS (2012) Need for long-term follow-up in enterohemorrhagic Escherichia coli-associated hemolytic uremic syndrome due to late-emerging sequelae. Clin Infect Dis 54:1413–1421
Waters AM, Kerecuk L, Luk D, Haq MR, Fitzpatrick MM, Gilbert RD, Inward C, Jones C, Pichon B, Reid C, Slack MPE, Van’t Hoff W, Dillon MJ, Taylor CM, Tullus K (2007) Hemolytic uremic syndrome associated with invasive pneumococcal disease: the United kingdom experience. J Pediatr 151:140–144
Siegler RL (1994) Spectrum of extrarenal involvement in postdiarrheal hemolytic-uremic syndrome. J Pediatr 125:511–518
Scheiring J, Andreoli SP, Zimmerhackl LB (2008) Treatment and outcome of Shiga-toxin-associated hemolytic uremic syndrome (HUS). Pediatr Nephrol 23:1749–1760
Constantinescu AR, Bitzan M, Weiss LS, Christen E, Kaplan BS, Cnaan A, Trachtman H (2004) Non-enteropathic hemolytic uremic syndrome: causes and short-term course. Am J Kidney Dis 43:976–982
Brandt J, Wong C, Mihm S, Roberts J, Smith J, Brewer E, Thiagarajan R, Warady B (2002) Invasive pneumococcal disease and hemolytic uremic syndrome. Pediatrics 110:371–376
Fitzpatrick MM, Walters MDS, Trompeter RS, Dillon MJ, Barratt TM (1993) Atypical (non-diarrhea-associated) hemolytic-uremic syndrome in childhood. J Pediatr 122:532–537
Nathanson S, Kwon T, Elmaleh M, Charbit M, Launay EA, Harambat J, Brun M, Ranchin B, Bandin F, Cloarec S, Bourdat-Michel G, Pietrement C, Champion G, Ulinski T, Deschenes G (2010) Acute neurological involvement in diarrhea-associated hemolytic uremic syndrome. Clin J Am Soc Nephrol 5:1218–1228
Schlieper A, Orrbine E, Wells GA, Clulow M, McLaine PN, Rowe PC (1999) Neuropsychological sequelae of haemolytic uraemic syndrome. Investigators of the HUS Cognitive Study. Arch Dis Child 80:214–220
Qamar IU, Ohali M, MacGregor DL, Wasson C, Krekewich K, Marcovitch S, Arbus GS (1996) Long-term neurological sequelae of hemolytic-uremic syndrome: a preliminary report. Pediatr Nephrol 10:504–506
Bauer A, Loos S, Wehrmann C, Horstmann D, Donnerstag F, Lemke J, Hillebrand G, Lobel U, Pape L, Haffner D, Bindt C, Ahlenstiel T, Melk A, Lehnhardt A, Kemper MJ, Oh J, Hartmann H (2014) Neurological involvement in children with E. coli O104:H4-induced hemolytic uremic syndrome. Pediatr Nephrol 29:1607–1615
Besbas N, Karpman D, Landau D, Loirat C, Proesmans W, Remuzzi G, Rizzoni G, Taylor CM, Van de Kar N, Zimmerhackl LB, HUS EPRGf (2006) A classification of hemolytic uremic syndrome and thrombotic thrombocytopenic purpura and related disorders. Kidney Int 70:423–431
Zipfel PF, Wolf G, John U, Kentouche K, Skerka C (2011) Novel developments in thrombotic microangiopathies: is there a common link between hemolytic uremic syndrome and thrombotic thrombocytic purpura? Pediatr Nephrol 26:1947–1956
Barbour T, Johnson S, Cohney S, Hughes P (2012) Thrombotic microangiopathy and associated renal disorders. Nephrol Dial Transplant 27:2673–2685
Wechsler D (2003) Manual for the Wechsler Intelligence Scale for Children. The Psychological Corporation, New York
Schwartz GJ, Munoz A, Schneider MF, Mak RH, Kaskel F, Warady BA, Furth SL (2009) New equations to estimate GFR in children with CKD. J Am Soc Nephrol 20:629–637
Hajnal BL, Sahebkar-Moghaddam F, Barnwell AJ, Barkovich AJ, Ferriero DM (1999) Early prediction of neurologic outcome after perinatal depression. Pediatr Neurol 21:788–793
Largo RH, Pfister D, Molinari L, Kundu S, Lipp A, Duc G (1989) Significance of prenatal, perinatal and postnatal factors in the development of AGA preterm infants at five to seven years. Dev Med Child Neurol 31:440–456
Wechsler D (2002) Wechsler Preschool and Primary Scale of Intelligence. The Psychological Corporation, San Antonio
Largo RH, Caflisch JA, Hug F, Muggli K, Molnar AA, Molinari L, Sheehy A, Gasser T (2001) Neuromotor development from 5 to 18 years. Part 1: timed performance. Dev Med Child Neurol 43:436–443
Largo RH, Caflisch JA, Hug F, Muggli K, Molnar AA, Molinari L (2001) Neuromotor development from 5 to 18 years. Part 2: associated movements. Dev Med Child Neurol 43:444–453
Steinborn M, Leiz S, Rüdisser K, Griebel M, Harder T, Hahn H (2004) CT and MRI in haemolytic uraemic syndrome with central nervous system involvement: distribution of lesions and prognostic value of imaging findings. Pediatr Radiol 34:805–810
Seitz J, Jenni OG, Molinari L, Caflisch J, Largo RH, Latal Hajnal B (2006) Correlations between motor performance and cognitive functions in children born <1250 g at school age. Neuropediatrics 37:6–12
von Rhein M, Dimitropoulos A, Valsangiacomo Buechel ER, Landolt MA, Latal B (2012) Risk factors for neurodevelopmental impairments in school-age children after cardiac surgery with full-flow cardiopulmonary bypass. J Thorac Cardiovasc Surg 144:577–583
Cimolai N, Morrison BJ, Carter JE (1992) Risk factors for the central nervous system manifestations of gastroenteritis-associated hemolytic-uremic syndrome. Pediatrics 90:616–621
Banerjee R, Hersh AL, Newland J, Beekmann SE, Polgreen PM, Bender J, Shaw J, Copelovitch L, Kaplan BS, Shah SS (2011) Streptococcus pneumoniae-associated hemolytic uremic syndrome among children in North America. Pediatr Infect Dis J 30:736–739
Chen S-Y, Wu C-Y, Tsai I-J, Tsau Y-K, Su Y-T (2011) Nonenteropathic hemolytic uremic syndrome: the experience of a medical center. Pediatr Neonatol 52:73–77
Magnus T, Rother J, Simova O, Meier-Cillien M, Repenthin J, Moller F, Gbadamosi J, Panzer U, Wengenroth M, Hagel C, Kluge S, Stahl RK, Wegscheider K, Urban P, Eckert B, Glatzel M, Fiehler J, Gerloff C (2012) The neurological syndrome in adults during the 2011 northern German E. coli serotype O104:H4 outbreak. Brain 135:1850–1859
Johnson RJ, Warady BA (2013) Long-term neurocognitive outcomes of patients with end-stage renal disease during infancy. Pediatr Nephrol 28:1283–1291
Donnerstag F, Ding X, Pape L, Bültmann E, Lücke T, Zajaczek J, Hoy L, Das AM, Lanfermann H, Ehrich J, Hartmann H (2012) Patterns in early diffusion-weighted MRI in children with haemolytic uraemic syndrome and CNS involvement. Eur Radiol 22:506–513
Tureczek I, Caflisch J, Moehrlen U, Natalucci G, Bernet V, Latal B (2012) Long-term motor and cognitive outcome in children with congenital diaphragmatic hernia. Acta Paediatr 101:507–512
Schaefer C, von Rhein M, Knirsch W, Huber R, Natalucci G, Caflisch J, Landolt MA, Latal B (2013) Neurodevelopmental outcome, psychological adjustment, and quality of life in adolescents with congenital heart disease. Dev Med Child Neurol 55(12):1143–1149
Acknowledgments
We thank all the children, adolescents and their parents who participated in this study. We also thank Luciano Molinari, PhD, and Burkhardt Seifert, PhD, for support with the statistical analysis and Christina Schaefer, MD, University Children’s Hospital Zurich, for performing the neurodevelopmental assessment. The honorarium of Kathrin Buder was supported by the Swiss Society of Nephrology and by the foundation “Kinder für Kinder”.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Buder, K., Latal, B., Nef, S. et al. Neurodevelopmental long-term outcome in children after hemolytic uremic syndrome. Pediatr Nephrol 30, 503–513 (2015). https://doi.org/10.1007/s00467-014-2950-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-014-2950-0