Abstract
Background
Laparoscopic liver resection (LLR) has gained increasing acceptance for surgical treatment of malignant and benign liver tumors. LLR for intrahepatic cholangiocarcinoma (ICC) is not commonly performed because of the concern for the frequent need for major hepatectomy, vascular-biliary reconstructions, and lymph node dissection (LND). The aim of this present meta-analysis is to compare surgical and oncological outcomes of laparoscopic (LLR) versus open liver resection (OLR) for ICC.
Materials and methods
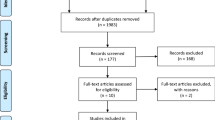
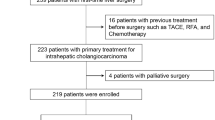
A systematic review was conducted using the PubMed, MEDLINE, and Cochrane library database of published studies comparing LLR and OLR up to October 2019. Two reviewers independently assessed the eligibility and quality of the studies. Dichotomous data were calculated by odds ratio (OR), and continuous data were calculated by mean difference (MD) with 95% confidence intervals (95% CI).
Results
Four retrospective observational studies describing 204 patients met the inclusion criteria. With respect to surgical outcomes, laparoscopic compared with open liver resection was associated with lower blood loss [MD − 173.86, (95% CI − 254.82, −92.91) p < 0.0001], less requirement of blood transfusion [OR 0.34, (95% CI 0.14, 0.82) p = 0.02], less need for Pringle maneuver [OR 0.17, (95% CI 0.07, 0.43) p = 0.0002], shorter hospital stay [MD − 3.77, (95% CI − 5.09, − 2.44; p < 0.0001], and less morbidity [OR 0.44, (95% CI 0.21, 0.94) p = 0.03]. With respect to oncological outcomes, the LLR group was prone to lower rates of lymphadenectomy [OR 0.12, (95% CI 0.06, 0.25) p < 0.0001], but surgical margins R0 and recurrence rate were not significantly different.
Conclusion
Laparoscopic liver resection for ICC seems to achieve better surgical outcomes, providing short-term benefits without negatively affecting oncologic adequacy in terms of R0 resections and disease recurrence. However, a higher LND rate was observed in the open group. Due to the risk of bias and the statistical heterogeneity between the studies included in this review, further RCTs are needed to reach stronger scientific conclusions.











Similar content being viewed by others
Abbreviations
- ICC:
-
Intrahepatic cholangiocarcinoma
- LLR:
-
Laparoscopic liver resection
- OLR:
-
Open liver resection
- MINORS:
-
Methodological index for non-randomized studies
- SD:
-
Standard deviation
- MD:
-
Mean difference
- CI:
-
Confidence interval
- OR:
-
Odds ratio
- RFS:
-
Recurrence free survival
- OS:
-
Overall survival
- LND:
-
Lymph node dissection/lymphadenectomy
References
Ratti F, Cipriani F, Ariotti R, Gagliano A, Paganelli M, Catena M, Aldrighetti L (2016) Safety and feasibility of laparoscopic liver resection with associated lymphadenectomy for intrahepatic cholangiocarcinoma: a propensity score-based case-matched analysis from a single institution. Surg Endosc 30(5):1999–2010
Waisberg DR, Pinheiro RS, Nacif LS, Rocha-Santos V, Martino RB, Arantes RM, Ducatti L, Lai Q, Andraus W, D’Albuquerque LC (2018) Resection for intrahepatic cholangiocellular cancer: new advances. Transl Gastroenterol Hepatol 3:60
Uy BJ, Han H-S, Yoon Y-S, Cho JY (2015) Laparoscopic liver resection for intrahepatic cholangiocarcinoma. J Laparoendosc Adv Surg Tech A 25(4):272–277
Bridgewater J, Galle PR, Khan SA, Llovet JM, Park J-W, Patel T, Pawlik TM, Gores GJ (2014) Guidelines for the diagnosis and management of intrahepatic cholangiocarcinoma. J Hepatol 60(6):1268–1289
Shaib YH, Davila JA, McGlynn K, El-Serag HB (2004) Rising incidence of intrahepatic cholangiocarcinoma in the United States: a true increase? J Hepatol 40(3):472–477
Nakanuma Y, Sato Y, Harada K, Sasaki M, Xu J, Ikeda H (2010) Pathological classification of intrahepatic cholangiocarcinoma based on a new concept. World J Hepatol 2(12):419–427
Uchiyama K, Yamamoto M, Yamaue H, Ariizumi S, Aoki T, Kokudo N, Ebata T, Nagino M, Ohtsuka M, Miyazaki M, Tanaka E, Kondo S, Uenishi T, Kubo S, Yoshida H, Unno M, Imura S, Shimada M, Ueno M, Takada T (2011) Impact of nodal involvement on surgical outcomes of intrahepatic cholangiocarcinoma: a multicenter analysis by the Study Group for Hepatic Surgery of the Japanese Society of Hepato-Biliary-Pancreatic Surgery. J Hepatobiliary Pancreat Sci 18(3):443–452
Amini N, Ejaz A, Spolverato G, Maithel SK, Kim Y, Pawlik TM (2014) Management of lymph nodes during resection of hepatocellular carcinoma and intrahepatic cholangiocarcinoma: a systematic review. J Gastrointest Surg 18(12):2136–2148
Lee W, Park J-H, Kim J-Y, Kwag S-J, Park T, Jeong S-H, Ju YT, Jung EJ, Lee YJ, Hong SC, Choi SK, Jeong CY (2016) Comparison of perioperative and oncologic outcomes between open and laparoscopic liver resection for intrahepatic cholangiocarcinoma. Surg Endosc 30(11):4835–4840
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS, Asbun H, O’Rourke N, Tanabe M, Koffron AJ, Tsung A, Soubrane O, Machado MA, Gayet B, Troisi RI, Pessaux P, Van Dam RM, Scatton O, Abu Hilal M, Belli G, Kwon CH, Edwin B, Choi GH, Aldrighetti LA, Cai X, Cleary S, Chen KH, Schön MR, Sugioka A, Tang CN, Herman P, Pekolj J, Chen XP, Dagher I, Jarnagin W, Yamamoto M, Strong R, Jagannath P, Lo CM, Clavien PA, Kokudo N, Barkun J, Strasberg SM (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261(4):619–629
Goossen K, Tenckhoff S, Probst P, Grummich K, Mihaljevic AL, Büchler MW, Diener MK (2018) Optimal literature search for systematic reviews in surgery. Langenbeck’s Arch Surg 403(1):119–129
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73(9):712–716
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13
Higgins JPT, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
Wei F, Lu C, Cai L, Yu H, Liang X, Cai X (2017) Can laparoscopic liver resection provide a favorable option for patients with large or multiple intrahepatic cholangiocarcinomas? Surg Endosc 31(9):3646–3655
Cipriani F, Ratti F, Cardella A, Catena M, Paganelli M, Aldrighetti L (2019) Laparoscopic versus open major hepatectomy: analysis of clinical outcomes and cost effectiveness in a high-volume center. J Gastrointest Surg 23:2163–2173. https://doi.org/10.1007/s11605-019-04112-4
Ratti F, Cipriani F, Ariotti R, Giannone F, Paganelli M, Aldrighetti L (2015) Laparoscopic major hepatectomies: current trends and indications. A comparison with the open technique. Updat Surg 67(2):157–167
Ratti F, Fiorentini G, Cipriani F, Paganelli M, Catena M, Aldrighetti L (2019) Perioperative and long-term outcomes of laparoscopic versus open lymphadenectomy for biliary tumors: a propensity-score-based, case-matched analysis. Ann Surg Oncol 26(2):564–575
Abu Hilal M, Badran A, Di Fabio F, Pearce NW (2011) Pure laparoscopic en bloc left hemihepatectomy and caudate lobe resection in patients with intrahepatic cholangiocarcinoma. J Laparoendosc Adv Surg Tech A 21(9):845–849
Takahashi M, Wakabayashi G, Nitta H, Takeda D, Hasegawa Y, Takahara T, Ito N (2013) Pure laparoscopic right hepatectomy by anterior approach with hanging maneuver for large intrahepatic cholangiocarcinoma. Surg Endosc 27(12):4732–4733
Reddy SK, Barbas AS, Turley RS, Steel JL, Tsung A, Marsh JW, Geller DA, Clary BM (2011) A standard definition of major hepatectomy: resection of four or more liver segments. HPB (Oxford) 13(7):494–502
Levi Sandri GB, Spoletini G, Mascianà G, Colasanti M, Lepiane P, Vennarecci G, D’Andrea V, Ettorre GM (2017) The role of minimally invasive surgery in the treatment of cholangiocarcinoma. Eur J Surg Oncol 43(9):1617–1621
Ciria R, Cherqui D, Geller DA, Briceno J, Wakabayashi G (2016) Comparative short-term benefits of laparoscopic liver resection: 9000 cases and climbing. Ann Surg 263(4):761–777
Hwang DW, Han H-S, Yoon Y-S, Cho JY, Kwon Y, Kim JH, Park JS, Yoon DS, Choi IS, Ahn KS, Kim YH, Kang KJ, Kim YH, Roh YH, Chu CW, Kim HC, Kang CM, Choi GH, Choi JS, Kim KS, Lee WJ, Yun SS, Kim HJ, Min SK, Lee HK, Song IS, Chun KS, Cho EH, Han SS, Park SJ (2013) Laparoscopic major liver resection in Korea: a multicenter study. J Hepatobiliary Pancreat Sci 20(2):125–130
Abu Hilal M, Di Fabio F, Teng MJ, Lykoudis P, Primrose JN, Pearce NW (2011) Single-centre comparative study of laparoscopic versus open right hepatectomy. J Gastrointest Surg 15(5):818–823
Mavros MN, Economopoulos KP, Alexiou VG, Pawlik TM (2014) Treatment and prognosis for patients with intrahepatic cholangiocarcinoma: systematic review and meta-analysis. JAMA Surg 149(6):565–574
Aldrighetti L, Guzzetti E, Pulitanò C, Cipriani F, Catena M, Paganelli M, Ferla G (2010) Case-matched analysis of totally laparoscopic versus open liver resection for HCC: short and middle term results. J Surg Oncol 102(1):82–86
Wakabayashi G, Cherqui D, Geller DA, Han H-S, Kaneko H, Buell JF (2014) Laparoscopic hepatectomy is theoretically better than open hepatectomy: preparing for the 2nd International Consensus Conference on Laparoscopic Liver Resection. J Hepatobiliary Pancreat Sci 21(10):723–731
Navarro J, Rho SY, Kang I, Choi GH, Min BS (2019) Robotic simultaneous resection for colorectal liver metastasis: feasibility for all types of liver resection. Langenbeck’s Arch Surg 404(7):895–908
Squires MH, Cloyd JM, Dillhoff M, Schmidt C, Pawlik TM (2018) Challenges of surgical management of intrahepatic cholangiocarcinoma. Expert Rev Gastroenterol Hepatol 12(7):671–681
Spolverato G, Yakoob MY, Kim Y, Alexandrescu S, Marques HP, Lamelas J, Aldrighetti L, Gamblin TC, Maithel SK, Pulitano C, Bauer TW, Shen F, Poultsides GA, Marsh JW, Pawlik TM (2015) The impact of surgical margin status on long-term outcome after resection for intrahepatic cholangiocarcinoma. Ann Surg Oncol 22(12):4020–4028
Bagante F, Spolverato G, Weiss M, Alexandrescu S, Marques HP, Aldrighetti L, Maithel SK, Pulitano C, Bauer TW, Shen F, Poultsides GA, Soubrane O, Martel G, Groot Koerkamp B, Guglielmi A, Itaru E, Pawlik TM (2018) Assessment of the lymph node status in patients undergoing liver resection for intrahepatic cholangiocarcinoma: the new eighth edition AJCC staging system. J Gastrointest Surg 22(1):52–59
Bagante F, Spolverato G, Weiss M, Alexandrescu S, Marques HP, Aldrighetti L, Maithel SK, Pulitano C, Bauer TW, Shen F, Poultsides GA, Soubrane O, Martel G, Groot Koerkamp B, Guglielmi A, Itaru E, Ruzzenente A, Pawlik TM (2018) Surgical management of intrahepatic cholangiocarcinoma in patients with cirrhosis: impact of lymphadenectomy on peri-operative outcomes. World J Surg 42(8):2551–2560
Fiorentini G, Ratti F, Cipriani F, Palombo D, Catena M, Paganelli M, Aldrighetti L (2017) Minimally invasive approach to intrahepatic cholangiocarcinoma: technical notes for a safe hepatectomy and lymphadenectomy. Ann Laparosc Endosc Surg 2. https://doi.org/10.21037/ales.2017.03.05
Giuliante F, Ardito F, Guglielmi A, Aldrighetti L, Ferrero A, Calise F, Giulini SM, Jovine E, Breccia C, De Rose AM, Pinna AD, Nuzzo G (2016) Association of lymph node status with survival in patients after liver resection for hilar cholangiocarcinoma in an Italian multicenter analysis. JAMA Surg 151(10):916–922
Guerrini GP, Lauretta A, Belluco C, Olivieri M, Forlin M, Basso S, Breda B, Bertola G, Di Benedetto F (2017) Robotic versus laparoscopic distal pancreatectomy: an up-to-date meta-analysis. BMC Surg 17(1):105
Nguyen KT, Marsh JW, Tsung A, Steel JJL, Gamblin TC, Geller DA (2011) Comparative benefits of laparoscopic vs open hepatic resection: a critical appraisal. Arch Surg 146(3):348–356
Halls MC, Cipriani F, Berardi G, Barkhatov L, Lainas P, Alzoubi M, D’Hondt M, Rotellar F, Dagher I, Aldrighetti L, Troisi RI, Edwin B, Abu Hilal M (2018) Conversion for unfavorable intraoperative events results in significantly worse outcomes during laparoscopic liver resection: lessons learned from a multicenter review of 2861 cases. Ann Surg 268(6):1051–1057
Hyder O, Hatzaras I, Sotiropoulos GC, Paul A, Alexandrescu S, Marques H, Pulitano C, Barroso E, Clary BM, Aldrighetti L, Ferrone CR, Zhu AX, Bauer TW, Walters DM, Groeschl R, Gamblin TC, Marsh JW, Nguyen KT, Turley R, Popescu I, Hubert C, Meyer S, Choti MA, Gigot JF, Mentha G, Pawlik TM (2013) Recurrence after operative management of intrahepatic cholangiocarcinoma. Surgery 153(6):811–818
Zhang X-F, Beal EW, Bagante F, Chakedis J, Weiss M, Popescu I, Marques HP, Aldrighetti L, Maithel SK, Pulitano C, Bauer TW, Shen F, Poultsides GA, Soubrane O, Martel G, Koerkamp BG, Itaru E, Pawlik TM (2018) Early versus late recurrence of intrahepatic cholangiocarcinoma after resection with curative intent. Br J Surg 105(7):848–856
Tamandl D, Herberger B, Gruenberger B, Puhalla H, Klinger M, Gruenberger T (2008) Influence of hepatic resection margin on recurrence and survival in intrahepatic cholangiocarcinoma. Ann Surg Oncol 15(10):2787–2794
Probst P, Zaschke S, Heger P, Harnoss JC, Hüttner FJ, Mihaljevic AL, Knebel P, Diener MK (2019) Evidence-based recommendations for blinding in surgical trials. Langenbeck’s Arch Surg 404(3):273–284
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Drs. Guerrini Gian Piero, Esposito Giuseppe, Tarantino Giuseppe, Serra Valentina, Olivieri Tiziana, Catellani Barbara, Assirati Giacomo, Guidetti Cristiano, Ballarin Roberto, Magistri Paolo, and Di Benedetto Fabrizio have no conflicts of interest or financial ties to disclose.
Ethical approval
The article is in accordance with ethical standards.
Research involving human participants and/or animals
This study does not contain any research with human participants performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Guerrini, G.P., Esposito, G., Tarantino, G. et al. Laparoscopic versus open liver resection for intrahepatic cholangiocarcinoma: the first meta-analysis. Langenbecks Arch Surg 405, 265–275 (2020). https://doi.org/10.1007/s00423-020-01877-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-020-01877-0