Abstract
Purpose
Moyamoya disease (MMD) commonly leads to neurocognitive impairment. This study was carried out to show that temporal encephaloduroarteriosynangiosis (EDAS) has a positive neuropsychological impact on pediatric MMD patients.
Methods
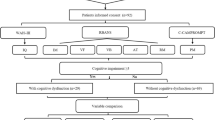
Fifty-five participants diagnosed with MMD from 2008 to 2014 were included in this retrospective study. The mean age at the preoperative evaluation was 9.5 years and the mean age at postoperative evaluation was 10.4. The average interval of initial and follow-up test was 10 months. K-WISC-III, Rey-Kim memory test, Children’s Color Trails test (CCTT), Wisconsin Card Sorting Test (WCST), and Advanced Test of Attention (ATA) were used to evaluate patient’s neurocognitive profile.
Results
In this study, preoperative and postoperative neuropsychological fields were compared. Prior operation, pediatric MMD patients showed 54.2% deficit of inattention but only around 2.5% deficit in verbal memory recall function. There was a significant increase of performance IQ and PO score component of PIQ improved almost 10 scores after surgery. For memorial function, there was an improvement of approximately 10 scores in MQ after the surgery. This study also showed parietal activation following surgical treatment which enhanced the ability to interpret visual materials, to register and to retrieve visual information. Interestingly, despite the parietal cover surgery, there was a significant improvement of performance on WCST and CCTT measuring the prefrontal executive function. Concerning failure to maintain set, no significant postoperative improvements were made. However, simple and selective visual attention on ATA was significantly improved postoperatively.
Conclusions
The results from neuropsychological field comparison testifies the effectiveness of temporal EDAS in pediatric MMD patients. The surgery not only enhances the blood flow in operative regions, but it also improves the broad cerebral function including frontoparietal domains. Such alteration leads to overall advancement in cognitive function which are impaired due to MMD.

Similar content being viewed by others
References
Scott RM, Smith ER (2009) Moyamoya disease and moyamoya syndrome. N Engl J Med 360:1226–1237
Suzuki J, Takaku A (1969) Cerebrovascular “moyamoya” disease. Disease showing abnormal net-like vessels in base of brain. Arch Neurol 20:288–299
Kuroda S, Houkin K, Ishikawa T, Nakayama N, Ikeda J, Ishii N, Kamiyama H, Iwasaki Y (2004) Determinants of intellectual outcome after surgical revascularization in pediatric moyamoya disease: a multivariate analysis. Childs Nerv Syst 20:302–308
Smith JL (2009) Understanding and treating moyamoya disease in children. Neurosurg Focus 26:E4
Imaizumi C, Imaizumi T, Osawa M, Fukuyama Y, Takeshita M (1999) Serial intelligence test scores in pediatric moyamoya disease. Neuropediatrics 30:294–299
Williams TS, Westmacott R, Dlamini N, Granite L, Dirks P, Askalan R, Macgregor D, Moharir M, Deveber G (2012) Intellectual ability and executive function in pediatric moyamoya vasculopathy. Dev Med Child Neurol 54:30–37
Shim KW, Park EK, Kim JS, Kim DS (2015) Cognitive outcome of pediatric moyamoya disease. J Korean Neurosurg Soc 57:440–444
Kim SK, Cho BK, Phi JH, Lee JY, Chae JH, Kim KJ, Hwang YS, Kim IO, Lee DS, Lee J, Wang KC (2010) Pediatric moyamoya disease: an analysis of 410 consecutive cases. Ann Neurol 68:92–101
Matsushima Y, Aoyagi M, Nariai T, Takada Y, Hirakawa K (1997) Long-term intelligence outcome of post-encephalo-duro-arterio-synangiosis childhood moyamoya patients. Clin Neurol Neurosurg 99(Suppl 2):S147–S150
Matsushima Y, Aoyagi M, Masaoka H, Suzuki R, Ohno K (1990) Mental outcome following encephaloduroarteriosynangiosis in children with moyamoya disease with the onset earlier than 5 years of age. Childs Nerv Syst 6:440–443
Nakashima H, Meguro T, Kawada S, Hirotsune N, Ohmoto T (1997) Long-term results of surgically treated moyamoya disease. Clin Neurol Neurosurg 99(Suppl 2):S156–S161
Park SE, Kim JS, Park EK, Shim KW, Kim DS (2017) Direct versus indirect revascularization in the treatment of moyamoya disease. J Neurosurg:1–10
Gonzalez N, Dusick J, Connolly M, Bounni F, Martin N, Van de Wiele B, Liebeskind D, Saver J (2015) Encephaloduroarteriosynangiosis for adult intracranial arterial steno-occlusive disease: long-term single-center experience with 107 operations. J Neurosurg 12:1–8
Matsushima T, Fujiwara S, Nagata S, Fujii K, Fukui M, Kitamura K, Hasuo K (1989) Surgical treatment for paediatric patients with moyamoya disease by indirect revascularisation procedures (EDAS, EMS, EMAS). Acta Neurochir 98:135–140
Dusick JR, Gonzalez NR, Martin NA (2011) Clinical and angiographic outcomes from indirect revascularization surgery for moyamoya disease in adults and children: a review of 63 procedures. Neurosurgery 68:34–43; discussion 43
Flanagan DP, Kaufman AS (2009) Essentials of Wisc-iv Assessment. Wiley, Hoboken
Kim H (2001) Assessment of memory disorders using Rey-Kim Memory Test. J Rehabil Psychol 8:29–48
McMillian SG, Rees CS, Pestel C (2013) An investigation of executive functioning, attention and working memory in compulsive hoarding. Behav Cogn Psychother 41:610–625
Figueroa IJ, Youmans RJ (2013) Failure to maintain set: a measure of distractibility or cognitive flexibility?. Proceedings Of The Human Factors And Ergonomics Society 57th Annual Meeting
Kang CG, Chun MH, Kang JA, Do KH, Choi SJ (2017) Neurocognitive dysfunction according to hypoperfusion territory in patients with moyamoya disease. Ann Rehabil Med 41:1–8
Lei Y, Li YJ, Guo QH, Liu XD, Liu Z, Ni W, Su JB, Yang H, Jiang HQ, Xu B, Gu YX, Mao Y (2017) Postoperative executive function in adult moyamoya disease: a preliminary study of its functional anatomy and behavioral correlates. J Neurosurg 126:527–536
Kurokawa T, Tomita S, Ueda K, Narazaki O, Hanai T, Hasuo K, Matsushima T, Kitamura K (1985) Prognosis of occlusive disease of the circle of Willis (moyamoya disease) in children. Pediatr Neurol 1:274–277
Trahan LH, Stuebing KK, Fletcher JM, Hiscock M (2014) The Flynn effect: a meta-analysis. Psychol Bull 140:1332–1360
Jones-Gotman M, Smith M, Zatorre R (1993) Neuropsychological testing for localizing and lateralizing the epileptogenic region. In: Engel J Jr (ed) Surgical treatment of epilepsies. Raven Press, New York, pp 245–261
Hearne LJ, Mattingley JB, Cocchi L (2016) Functional brain networks related to individual differences in human intelligence at rest. Sci Rep 6:32328
Song M, Liu Y, Zhou Y, Wang K, Yu C, Jiang T (2009) Default network and intelligence difference. Conf Proc IEEE Eng Med Biol Soc 2009:2212–2215
Cole MW, Yarkoni T, Repovs G, Anticevic A, Braver TS (2012) Global connectivity of prefrontal cortex predicts cognitive control and intelligence. J Neurosci 32:8988–8999
van den Heuvel MP, Stam CJ, Kahn RS, Hulshoff Pol HE (2009) Efficiency of functional brain networks and intellectual performance. J Neurosci 29:7619–7624
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kim, W., Lee, EY., Park, Se. et al. Neuropsychological impacts of indirect revascularization for pediatric moyamoya disease. Childs Nerv Syst 34, 1199–1206 (2018). https://doi.org/10.1007/s00381-018-3804-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-018-3804-z