Abstract
Objective
This is a retrospective study to evaluate the effectiveness of endoscopic third ventriculostomy (ETV) performed in children with posterior fossa tumors and hydrocephalus in an attempt to classify the selected cases who could benefit from ETV as a permanent CSF diversion procedure.
Methods
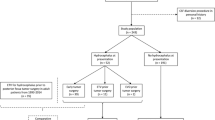
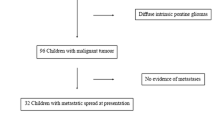
During the period between January 2008 and December 2008, 40 patients with posterior fossa tumors and associated hydrocephalus were treated inside the Children’s Cancer Hospital, Egypt (CCHE)—with ETV in order to relieve the increased intracranial pressure while awaiting their definite tumor surgery.
Results
ETV was successful in relieving hydrocephalus clinically and radiologically in 26 patients with different posterior fossa pathologies, with the highest success rate in glioma (100%), followed by 50% in ependymoma and 47.6% in medulloblatoma. In the other 14 cases, preoperative ETV failed in permanently resolving hydrocephalus and patients required the insertion of a ventriculoperitoneal (VP) shunt after their posterior fossa surgery and during their follow-up period.
Conclusion
ETV should be considered as an alternative procedure to VP shunt in controlling severe hydrocephalus related to posterior fossa tumors, to relieve symptoms quickly during the preoperative period while patients await their definite tumor excision. Patients with ependymomas and gliomas, with totally excised tumors, are better candidates for ETV than those with medulloblastomas. However, ETV cannot always prevent postoperative hydrocephalus in all cases of posterior fossa tumor, the thing that makes using postoperative VP shunt an alternative.

Similar content being viewed by others
References
Ruggiero C, Cinalli G, Spennato P, Aliberti F, Cianciulli E, Trischitta V, Maggi G (2004) Endoscopic third ventriculostomy in the treatment of hydrocephalus in posterior fossa tumors in children. Childs Nerv Syst 20:828–833
Li KW, Nelson C, Suk I, Jallo GI (2005) Neuroendoscopy: past, present, and future. Neurosurg Focus 19(1):E1
Albright L, Reigel DH (1977) Management of hydrocephalus secondary to posterior fossa tumors. J Neurosurg 46:52–55
Muszynski CA, Laurent JP, Cheek WR (1994) Effect of ventricular drainage and dural closure on cerebro-spinal fluid leaks after posterior fossa tumor surgery. Pediatr Neurosurg 21:227–231
Schmid UD, Seiler RW (1986) Management of obstructive hydrocephalus secondary to posterior fossa tumors by steroids and subcutaneous ventricular catheter reservoir. J Neurosurg 65:649–653
Jones RF, Stening WA, Brydon M (1990) Endoscopic third ventriculostomy. Neurosurgery 26:86–91
Epstein F, Murali R (1978) Pediatric posterior fossa tumors: hazards of the “preoperative” shunt. Neurosurgery 3:348–350
Hoffman HJ, Hendrick EB, Humphreys RP (1976) Metastasis via ventriculoperitoneal shunt in patients with medulloblastoma. J Neurosurg 44:462–466
Fiorillo A, Maggi G, Martone A, Migliorati R, D’Amore R, Alfieri E, Greco N, Cirillo S, Marano I (2001) Shunt-related abdominal metastases in an infant with medulloblastoma:long-term remission by systemic chemotherapy and surgery. J Neurooncol 52:273–276
Rappaport ZH, Shalit MN (1989) Perioperative hydrocephalus secondary to infratentorial brain tumors. Acta Neurochir(Wien) 96:118–121
McNatt SA, Kim A, Hohuan D, Krieger M, McComb JG (2008) Pediatric shunt malfunction without ventricular dilatation. Pediatr Neurosurg 44:128–132
Lim ME, Hoffman JA, Kim KS (1999) Recurrent ventriculoperitoneal shunt infection due to nontypeable Haemophilus influenzae. Clin Infect Dis 28:147–148
Bryant MS, Bremer AM, Tepas JJ, Mollitt DL, Nquyen TQ, Talbert JL (1988) Abdominal complications of ventriculoperitoneal shunts. Case reports and review of the literature. Am Surg 54:50–55
Bhatia R, Tahir M, Chandler CL (2009) The management of hydrocephalus in children with posterior fossa tumours: the role of pre-resectional endoscopic third ventriculostomy. Pediatr Neurosurg 45:186–191
Sainte-Rose C, Cinalli G, Roux FE, Maixner R, Chumas PD, Mansour M, Carpentier A, Bourgeois M, Zerah M, Pierre-Kahn A, Renier D (2001) Management of hydrocephalus in pediatric patients with posterior fossa tumors: the role of endoscopic third ventriculostomy. J Neurosurg 95:791–797
Hopf NJ, Grunert P, Fries G, Resch KD, Perneczky A (1999) Endoscopic third ventriculostomy: outcome analysis of 100 consecutive procedures. Neurosurgery 44:795–806
Bognar L, Borgulya G, Benke P, Madarassy G (2003) Analysis of CSF shunting procedure requirement in children with posterior fossa tumors. Childs Nerv Syst 19:332–336
Morelli D, Pirotte B, Lubansu A, Detemmerman D, Aeby A, Fricx C, Berré J, David P, Brotchi J (2005) Persistent hydrocephalus after early surgical management of posterior fossa tumors in children: is routine preoperative endoscopic third ventriculostomy justified? J Neurosurg 103:247–252
Tamburrini G, Pettorini BL, Massimi L, Caldarelli M, Di Rocco C (2008) Endoscopic third ventriculostomy: the best option in the treatment of persistent hydrocephalus after posterior cranial fossa tumour removal? Chils Nerv Syst 24:1405–1412
Tamburrini G, Massimi L, Caldarelli M, Di Rocco C (2008) Antibiotic impregnated external ventricular drainage and third ventriculostomy in the management of hydrocephalus associated with posterior cranial fossa tumours. Acta Neurochir (Wien) 150:1049–1056
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
El Beltagy, M.A., Kamal, H.M., Taha, H. et al. Endoscopic third ventriculostomy before tumor surgery in children with posterior fossa tumors, CCHE experience. Childs Nerv Syst 26, 1699–1704 (2010). https://doi.org/10.1007/s00381-010-1180-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-010-1180-4