Abstract
Purpose
The objective of this study was to compare patient comfort between MR-guided in-bore prostate biopsy (IB-GB) and MRI/ultrasound fusion-guided prostate biopsy (FUS-GB) with additional systematic 12-core transrectal ultrasound (TRUS)-guided biopsy within a prospective randomized trial.
Methods
Two hundred and ten consecutive patients were randomly assigned in a 1:1 ratio to receive either IB-GB and prior intrarectal instillation of a 2 % lidocaine gel (n = 106) or FUS-GB plus additional systematic 12-core TRUS-guided biopsy and prior application of a periprostatic nerve block (PPNB) with 2 % mepivacaine (n = 104). The maximal procedural pain (MPP) on a 0–10 visual analog scale and the operating room time were recorded for each biopsy session.
Results
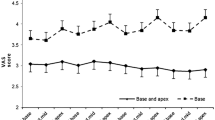
Baseline characteristics and mean number of targeted biopsy cores (5.6 ± 0.8 vs 5.4 ± 1.2 for IB-GB and FUS-GB, respectively; p = 0.278) were similar in both study arms. In relation to the IB-GB arm, the total number of biopsy cores in the FUS-GB arm, including the systematic 12-core TRUS-guided biopsy, was significantly higher (17.4 ± 1.2; p < 0.001). Patients with IB-GB had significantly higher MPP scores (2.95 ± 2.15) compared with subjects with FUS-GB (1.95 ± 1.56; p < 0.001). FUS-GB required significantly less time (28.22 ± 11.61 min) in comparison with IB-GB (42.09 ± 11.37 min; p < 0.001).
Conclusions
The PPNB can easily be administered just prior to performing FUS-GB. Thus, patients have significantly lower pain levels in comparison with IB-GB, which is usually done with intrarectal anesthetic gels. Although the addition of a systematic 12-core TRUS-guided biopsy significantly increases the number of biopsy cores, FUS-GB still requires significantly less time in comparison with IB-GB.
Similar content being viewed by others
References
Overduin CG, Fütterer JJ, Barentsz JO (2013) MRI-guided biopsy for prostate cancer detection: a systematic review of current clinical results. Curr Urol Rep 14:209–213
Pinto PA, Chung PH, Rastinehad AR et al (2011) Magnetic resonance imaging/ultrasound fusion guided prostate biopsy improves cancer detection following transrectal ultrasound biopsy and correlates with multiparametric magnetic resonance imaging. J Urol 186:1281–1285
Hadaschik BA, Kuru TH, Tulea C et al (2011) A novel stereotactic prostate biopsy system integrating pre-interventional magnetic resonance imaging and live ultrasound fusion. J Urol 186:2214–2220
Arsov C, Blondin D, Rabenalt R, Antoch G, Albers P, Quentin M (2012) Standardised scoring of a multi-parametric 3-T MRI for a targeted MRI-guided prostate biopsy. Urol A 51:848–856
Schimmöller L, Quentin M, Arsov C et al (2013) Inter-reader agreement of the ESUR score for prostate MRI using in-bore MRI-guided biopsies as the reference standard. Eur Radiol 23:3185–3190
Barentsz JO, Richenberg J, Clements R et al (2012) ESUR prostate MR guidelines 2012. Eur Radiol 22:746–757
Marks L, Young S, Natarajan S (2013) MRI-ultrasound fusion for guidance of targeted prostate biopsy. Curr Opin Urol 23:43–50
Nash PA, Bruce JE, Indudhara R, Shinohara K (1996) Transrectal ultrasound guided prostatic nerve blockade eases systematic needle biopsy of the prostate. J Urol 155:607–609
von Knobloch R, Weber J, Varga Z, Feiber H, Heidenreich A, Hofmann R (2002) Bilateral fine-needle administered local anaesthetic nerve block for pain control during TRUS-guided multi-core prostate biopsy: a prospective randomised trial. Eur Urol 41:508–514
Adamakis I, Mitropoulos D, Haritopoulos K, Alamanis C, Stravodimos K, Giannopoulos A (2004) Pain during transrectal ultrasonography guided prostate biopsy: a randomized prospective trial comparing periprostatic infiltration with lidocaine with the intrarectal instillation of lidocaine-prilocain cream. World J Urol 22:281–284
Song SH, Kim JK, Song K, Ahn H, Kim CS (2006) Effectiveness of local anaesthesia techniques in patients undergoing transrectal ultrasound-guided prostate biopsy: a prospective randomized study. Int J Urol 13:707–710
Heidenreich A, Bastian PJ, Bellmunt J et al (2014) EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and local treatment with curative intent-update 2013. Eur Urol 65:124–137
Hambrock T, Somford DM, Hoeks C et al (2010) Magnetic resonance imaging guided prostate biopsy in men with repeat negative biopsies and increased prostate specific antigen. J Urol 183:520–527
Franiel T, Stephan C, Erbersdobler A et al (2011) Areas suspicious for prostate cancer: MR-guided biopsy in patients with at least one transrectal US-guided biopsy with a negative finding–multiparametric MR imaging for detection and biopsy planning. Radiology 259:162–172
Fiard G, Hohn N, Descotes JL, Rambeaud JJ, Troccaz J, Long JA (2013) Targeted MRI-guided prostate biopsies for the detection of prostate cancer: initial clinical experience with real-time 3-dimensional transrectal ultrasound guidance and magnetic resonance/transrectal ultrasound image fusion. Urology 81:1372–1378
Rastinehad AR, Turkbey B, Salami SS et al (2014) Improving detection of clinically significant prostate cancer: MRI/TRUS fusion-guided prostate biopsy. J Urol 191:1749–1754
Siddiqui MM, Rais-Bahrami S, Truong H et al (2013) Magnetic resonance imaging/ultrasound-fusion biopsy significantly upgrades prostate cancer versus systematic 12-core transrectal ultrasound biopsy. Eur Urol 64:713–719
Bomers JG, Yakar D, Overduin CG et al (2013) MR imaging-guided focal cryoablation in patients with recurrent prostate cancer. Radiology 268:451–460
Oto A, Sethi I, Karczmar G et al (2013) MR imaging-guided focal laser ablation for prostate cancer: phase I trial. Radiology 267:932–940
Awsare NS, Green JA, Aldwinckle B, Hanbury DC, Boustead GB, McNicholas TA (2007) The use of propofol sedation for transrectal ultrasonography-guided prostate biopsy is associated with high patient satisfaction and acceptability. Eur J Radiol 63:94–95
Horinaga M, Nakashima J, Nakanoma T (2006) Efficacy compared between caudal block and periprostatic local anesthesia for transrectal ultrasound-guided prostate needle biopsy. Urology 68:348–351
Adsan O, Inal G, Ozdoğan L, Kaygisiz O, Uğurlu O, Cetinkaya M (2004) Unilateral pudendal nerve blockade for relief of all pain during transrectal ultrasound-guided biopsy of the prostate: a randomized, double-blind, placebo-controlled study. Urology 64:528–531
Obek C, Ozkan B, Tunc B, Can G, Yalcin V, Solok V (2004) Comparison of 3 different methods of anesthesia before transrectal prostate biopsy: a prospective randomized trial. J Urol 172:502–505
Mutaguchi K, Shinohara K, Matsubara A, Yasumoto H, Mita K, Usui T (2005) Local anesthesia during 10 core biopsy of the prostate: comparison of 2 methods. J Urol 173:742–745
Giannarini G, Autorino R, Valent F et al (2009) Combination of perianal-intrarectal lidocaine-prilocaine cream and periprostatic nerve block for pain control during transrectal ultrasound guided prostate biopsy: a randomized, controlled trial. J Urol 181:585–591
Bingqian L, Peihuan L, Yudong W, Jinxing W, Zhiyong W (2009) Intraprostatic local anesthesia with periprostatic nerve block for transrectal ultrasound guided prostate biopsy. J Urol 182:479–483
Alvarez-Múgica M, González Alvarez RC et al (2007) Tolerability and complications of ultrasound guided prostate biopsies with intrarectal lidocaine gel. Arch Esp Urol 60:237–244
Bastide C, Lechevallier E, Eghazarian C, Ortega JC, Coulange C (2003) Tolerance of pain during transrectal ultrasound-guided biopsy of the prostate: risk factors. Prostate Cancer Prostatic Dis 6:239–241
Mariappan P, Chong WL, Sundram M, Mohamed SR (2004) Increasing prostate biopsy cores based on volume vs the sextant biopsy: a prospective randomized controlled clinical study on cancer detection rates and morbidity. BJU Int 94:307–310
Sur RL, Borboroglu PG, Roberts JL, Amling CL (2004) A prospective randomized comparison of extensive prostate biopsy to standard biopsy with assessment of diagnostic yield, biopsy pain and morbidity. Prostate Cancer Prostatic Dis 7:126–131
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
The present study has been approved by the ethics committee of Heinrich-Heine University Düsseldorf. The study has been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. All patients gave their informed consent prior to their inclusion in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Arsov, C., Rabenalt, R., Quentin, M. et al. Comparison of patient comfort between MR-guided in-bore and MRI/ultrasound fusion-guided prostate biopsies within a prospective randomized trial. World J Urol 34, 215–220 (2016). https://doi.org/10.1007/s00345-015-1612-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-015-1612-6