Abstract
Objective
Percutaneous biliary interventions (PBIs) can be associated with a high patient radiation dose, which can be reduced when national diagnostic reference levels (DRLs) are kept in mind. The aim of this multicentre study was to investigate patient radiation exposure in different percutaneous biliary interventions, in order to recommend national DRLs.
Methods
A questionnaire asking for the dose area product (DAP) and the fluoroscopy time (FT) in different PBIs with ultrasound- or fluoroscopy-guided bile duct punctures was sent to 200 advanced care hospitals. Recommended national DRLs are set at the 75th percentile of all DAPs.
Results
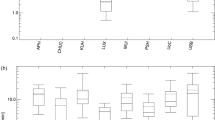
Twenty-three facilities (9 interventional radiology depts. and 14 gastroenterology depts.) returned the questionnaire (12%). Five hundred sixty-five PBIs with 19 different interventions were included in the analysis. DAPs (range 4–21,510 cGy·cm2) and FTs (range 0.07–180.33 min) varied substantially depending on the centre and type of PBI. The DAPs of initial PBIs were significantly (p < 0.0001) higher (median 2162 cGy·cm2) than those of follow-up PBIs (median 464 cGy·cm2). There was no significant difference between initial PBIs with ultrasound-guided bile duct puncture (2162 cGy·cm2) and initial PBIs with fluoroscopy-guided bile duct puncture (2132 cGy·cm2) (p = 0.85). FT varied substantially (0.07–180.33 min).
Conclusions
DAPs and FTs in percutaneous biliary interventions showed substantial variations depending on the centre and the type of PBI. PBI with US-guided bile duct puncture did not reduce DAP, when compared to PBI with fluoroscopy-guided bile duct puncture. National DRLs of 4300 cGy·cm2 for initial PBIs and 1400 cGy·cm2 for follow-up PBIs are recommended.
Key Points
• DAPs and FTs in percutaneous biliary interventions showed substantial variations depending on the centre and the type of PBI.
• PBI with US-guided bile duct puncture did not reduce DAP when compared to PBI with fluoroscopy-guided bile duct puncture.
• DRLs of 4300 cGy·cm2for initial PBIs (establishing a transhepatic tract) and 1400 cGy·cm2for follow-up PBIs (transhepatic tract already established) are recommended.






Similar content being viewed by others
Abbreviations
- ALARA:
-
‘As low as [is] reasonably achievable’
- cGy:
-
Centigray
- cm:
-
Centimetre
- DAP:
-
Dose area product (= kerma air product)
- DRL:
-
Diagnostic reference level
- ERCP:
-
Endoscopic retrograde pancreaticocholangiography
- FT:
-
Fluoroscopy time
- ICR:
-
Interquartile range
- ICRP:
-
International Commission on Radiological Protection
- kg:
-
Kilogramme
- mSv:
-
Millisievert
- PBI:
-
Percutaneous biliary intervention
- SD:
-
Standard deviation
- US:
-
Ultrasound
References
European Medical ALARA Network (2013) (2013) http://www.eman-network.eu/. Accessed 20 Mar 2019
Miller DL, Balter S, Dixon RG et al (2009) SIR Safety and Health Committee; CIRSE Standards of Practice Committee. Guidelines for patient radiation dose management. J Vasc Interv Radiol 20:S 263–S 273
ICRP (1996) Radiological protection and safety in medicine, ICRP publication 73, Ann. ICRP 26
ICRP (2017) Diagnostic reference levels in medical imaging. ICRP Publication 135, Ann. ICRP 46
European Commission (1997) Council Directive 97/43/EURATOM on health protection of individuals against the dangers of ionizing radiation in relation to medical exposure. Available via https://publications.europa.eu/en/publication-detail/-/publication/aa7564fa-fd07-4872-943c-66df8f4f1099/language-en. Accessed 20 Mar 2019
European Commission (2013) Council Directive 2013/59/EURATOM, which lays down basic safety standards for protection against the dangers arising from exposure to ionizing radiation. Available via. https://eurlex.europa.eu/legal-content/EN/TXT/?uri=CELEX%3A32013L0059. Accessed 20 Mar 2019
European Commission (2014) Radiation Protection N° 178. Referral guidelines for medical imaging. Availability and Use in the European Union. Available via https://ec.europa.eu/energy/sites/ener/files/documents/178.pdf. Accessed 20 Mar 2019
Schegerer AA (2016) Announcement of the updated diagnostic reference levels in diagnostic and interventional X-ray applications. Federal Office of Radiation Protection
Hart D, Wall BF (2004) UK population dose from medical X-ray examinations. Eur J Radiol 50:285–291
Hart D, Shrimpton PC (2012) Fourth review of the UK national patient dose database. Br J Radiol 85:1018
Stratakis J, Damilakis J, Hatzidakis A et al (2006) Radiation dose and risk from fluoroscopically guided percutaneous transhepatic biliary procedures. J Vasc Interv Radiol 17:77–84
Schmitz D, Weller N, Rudi J et al (2018) An improved method of percutaneous transhepatic biliary drainage combining ultrasoundguided bile duct puncture with metal stent implantation by fluoroscopic guidance and endoscopic visualisation as a one step-procedure: a retrospective cohort study. J Clin Int Rad
Schegerer AA, Nagel HD, Stamm G et al (2017) Current CT practice in Germany: results and implications of a nationwide survey. Eur J Radiol 90:114–128
Etard C, Bigand E, Salvat C et al (2017) Patient dose in interventional radiology: a multicentre study of the most frequent procedures in France. Eur Radiol 27:4281–4290
Perez-Johnston R, Deipolyi AR, Covey AM (2018) Percutaneous biliary interventions. Gastroenterol Clin North Am 47:621–641
Ruiz-Cruces R, Vano E, Carrera-Magariño F et al (2016) Diagnostic reference levels and complexity indices in interventional radiology: a national program. Eur Radiol 26:4268–4276
Marshall NW, Chapple CL, Kotre CJ (2000) Diagnostic reference levels in interventional radiology. Phys Med Biol 45:3833–3846
Miller DL, Balter S, Cole PE et al (2003) Radiation doses in interventional radiology procedures: the RAD-IR study: part I: overall measures of dose. J Vasc Interv Radiol 14:711–727
Aroua A, Rickli H et al (2007) How to set up and apply reference levels in fluoroscopy at a national level? Eur Radiol 17:1621–1633
Kloeckner R, Bersch A, dos Santos DP et al (2012) Radiation exposure in nonvascular fluoroscopy-guided interventional procedures. Cardiovasc Intervent Radiol 5:613–620
Lee W, Kim GC, Kim JY et al (2008) Ultrasound and fluoroscopy-guided percutaneous transhepatic biliary drainage in patients with nondilated bile ducts. Abdom Imaging 33:555–559
Miller DL, Balter S, Dixon RG et al (2012) Society of Interventional Radiology Standards of Practice Committee. Quality improvement guidelines for recording patient radiation dose in the medical record for fluoroscopically-guided procedures. J Vasc Interv Radiol 23:11–18
Heilmaier C, Niklaus Z, Berthold C et al (2015) Improving patient safety: implementing dose monitoring software in fluoroscopically-guided interventions. J Vasc Interv Radiol 26:1699–1709
Miller DL, Balter S, Schueler BA et al (2010) Clinical radiation management for fluoroscopically-guided interventional procedures. Radiology 257:321–332
Vano E, Järvinen H, Kosunen A et al (2008) Patient dose in interventional radiology: a European survey. Radiat Prot Dosimetry 129:39–45
European Society of Radiology (2017) Common strategic research agenda for radiation protection in medicine. Insights Imaging 8:183–197
Johnson PB, Borrego D, Balter S et al (2011) Skin dose mapping for fluoroscopically-guided interventions. Med Phys 38:5490–5499
den Boer A, de Feijter PJ, Serruys PW et al (2001) Real-time quantification and display of skin radiation during coronary angiography and intervention. Circulation 104:1779–1784
Ichimoto E, Kadohira T, Nakayama T et al (2018) Efficacy of radiation dose reduction due to real-time monitoring and visualisation of peak skin dose during coronary angiography and percutaneous coronary intervention. Catheter Cardiovasc Interv 91:717–722
Borrego D, Siragusa DA, Balter S et al (2017) A hybrid phantom system for patient skin and organ dosimetry in fluoroscopically guided interventions. Med Phys 44:4928–4942
European Society of Radiology (2013) ESR statement on radiation protection: globalisation, personalised medicine and safety (the GPS approach). Insights Imaging 4:737–739
Acknowledgements
The study was kindly supported by the German Society for Digestive and Metabolic Diseases (DGVS), president: Prof Dr. Med. F. Lammert. Special thanks are due to Dr. A. A. Schegerer (Federal Office of Radiation Protection, Department for Radiation Protection and Health), Prof Dr. J. Rudi (Theresienkrankenhaus and St Hedwig Hospital Mannheim) and Prof Dr. T. Vogl (University Hospital Frankfurt, Institute for Diagnostic and Interventional Radiology) for proofreading the manuscript.
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Alexander A. Schegerer.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
The Biomathmatics and Information Processing Department of Mannheim University Hospital kindly provided statistical advice for this manuscript.
Informed consent
Written informed consent was not required for this study because the retrospectively collected data were acquired routinely in all percutaneous biliary interventions and documented data were completely anonymised for this manuscript.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• observational study
• multicentre study
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Schmitz, D., Vogl, T., Nour-Eldin, NE.A. et al. Patient radiation dose in percutaneous biliary interventions: recommendations for DRLs on the basis of a multicentre study. Eur Radiol 29, 3390–3400 (2019). https://doi.org/10.1007/s00330-019-06208-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-019-06208-6