Abstract
Summary
Proximal femoral fractures affect elderly people, showing high morbidity and mortality incidence resulting in a major economic burden on national healthcare systems. Understanding the causes of these injuries is of paramount importance to prevent the serious consequences of these fractures.
Introduction
Hip osteoarthritis and proximal femoral fractures mainly affect elderly patients. Several authors, in their studies, tried to document a correlation between these conditions, but the results are conflicting. The aim of this study was to evaluate the relationship between hip osteoarthritis and the fracture site. Secondly, to evaluate if the grade of osteoarthritis could influence the fracture pattern.
Methods
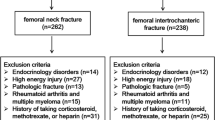
A retrospective study on 320 patients admitted for hip fracture between June 2015 and December 2016 was carried on. Radiographic images were evaluated, assessing the type of fracture, presence and grade of osteoarthritis according to Kellgren-Lawrence and Tönnis classifications, and their correlations.
Results
Osteoarthritis was found to affect the fracture site showing a higher prevalence among subjects with extracapsular than those with intracapsular fractures (p < 0.00001). Patients with radiographic signs of arthritis had mainly trochanteric fracture. Conversely, patients without arthritis more frequently presented a femoral neck fracture. This correlation was even more significant as the severity of the OA increased.
Conclusions
Results support the hypothesis that hip osteoarthritis could represent a protective factor for intracapsular fractures and a risk factor for trochanteric ones. The severity of arthritis is also associated with the fracture pattern.





Similar content being viewed by others
References
Zhang Y, Jordan JM (2010) Epidemiology of osteoarthritis. Clin Geriatr Med 26(3):355–369. https://doi.org/10.1016/j.cger.2010.03.001
Belo JN, Berger MY, Reijman M, Koes BW, Bierma-Zeinstra SMA (2007) Prognostic factors of progression of osteoarthritis of the knee: a systematic review of observational studies. Arthritis Rheum 57(1):13–26. https://doi.org/10.1002/art.22475
Schmidt AH, Swiontkowski MF (2002) Femoral neck fractures. Orthop Clin North Am 33(1):97–111. https://doi.org/10.1016/S0030-5898(03)00074-9
Dall’Oca C, Maluta T, Moscolo A, Lavini F, Bartolozzi P (2010) Cement augmentation of intertrochanteric fractures stabilised with intramedullary nailing. Injury 41(11):1150–1155. https://doi.org/10.1016/j.injury.2010.09.026
Foss MV, Byers PD (1972) Bone density, osteoarthrosis of the hip, and fracture of the upper end of the femur. Ann Rheum Dis 31:259–264. https://doi.org/10.1136/ard.31.4.259
Chudyk AM, Ashe MC, Gorman E, Al Tunaiji HO, Crossley KM (2012) Risk of hip fracture with hip or knee osteoarthritis: a systematic review. Clin Rheumatol 31:749–757. https://doi.org/10.1007/s10067-012-1970-z
Arden NK, Nevitt MC, Lane NE, Gore LR, Hochberg MC, Scott JC et al (1999) Osteoarthritis and risk of falls, rates of bone loss, and osteoporotic fractures. Study of Osteoporotic Fractures Research Group. Arthritis Rheum 42(7):1378–1385. https://doi.org/10.1002/1529-0131(199907)42:7%3C1378::AID-ANR11%3E3.0.CO;2-I
Dretakis EK, Steriopoulos KA, Kontakis GM, Giaourakis G, Economakis G, Dretakis KE (1998) Cervical hip fractures do not occur in arthrotic joints. A clinicoradiographic study of 256 patients. Acta Orthop Scand 69(4):384–386. https://doi.org/10.3109/17453679808999051
Robstad B, Frihagen F, Nordsletten L (2012) The rate of hip osteoarthritis in patients with proximal femoral fractures versus hip contusion. Osteoporos Int 23(3):901–905. https://doi.org/10.1007/s00198-011-1628-8
Calderazzi F, Groppi G, Ricotta A, Ceccarelli F (2014) Does hip osteoarthritis have a protective effect against proximal femoral fractures? A retrospective study. Hip Int 24(3):231–236. https://doi.org/10.530/hipint.5000116
Garden RS, Preston E (1961) Low angle fixation in fractures of the femoral neck. Surger 101:647
Kellgren J, Lawrence J (1957) Radiological assessment of osteoarthritis. Ann Rheum Dis 16:494–502
Tönnis D, Heinecke A, Nienhaus R, Thiele J (1979) Läßt sich das Auftreten von Arthrose, Schmerz und Bewegungseinschränkung des Huftgelenkes bei Huftdysplasie vorausberechnen. Z Orthop 117:808–815
Van Embden D, Rhemrev SJ, Genelin F, Meylaerts SAG, Roukema GR (2012) The reliability of a simplified Garden classification for intracapsular hip fractures. Orthop 98:405–408. https://doi.org/10.1016/j.otsr.2012.02.003
Wright RW, MARS Group (2014) Osteoarthritis classification scales: interobserver reliability and arthoscopic correlation. J Bone Joint Surg Am 96(14):1145–1151. https://doi.org/10.2016/JBJS.M.00929
Aguado-Maestro I, Panteli M, Garcia-Alonso M, Garcia-Cepeda GPV (2017) Hip osteoarthritis as a predictor factor of the fracture pattern in proximal femur fractures. Injury 48S:S41–S46. https://doi.org/10.1016/j.injury.2017.08.037
Yamamoto Y, Turkiewicz A, Wingstrand H, Englund M (2015) Fragility fractures in patients with rheumatoid arthritis and osteoarthritis compared with the general population. J Rheumatol 42(11):2055–2058. https://doi.org/10.3899/jrheum.150325
Franklin J, Englund M, Ingvarsson T, Lohmander S (2010) The association between hip fracture and hip osteoarthritis: a case-control study. BMC Musculoskelet Disord 11(274). https://doi.org/10.1186/1471-2474-11-274
Cumming RG, Klineberg RJ (1994) Fall frequency and characteristics and the risk of hip fractures. J Am Geriatr Soc 42(7):774–778. https://doi.org/10.1111/j.1532-5415.1994.tb06540.x
Cummings SR, Nevitt MC (1994) Non-skeletal determinants of fractures: the potential importance of the mechanics of falls. Osteoporos Int 4(1):s67–s70. https://doi.org/10.1007/BF01623439
Aizen E, Shugaev I, Lenger R (2007) Risk factors and characteristics of falls during inpatient rehabilitation of elderly patients. Arch Gerontol Geriatr 44:1–12. https://doi.org/10.1016/j.archger.2006.01.005
McDonough CM, Jette AM (2010) The contribution of osteoarthritis to functional limitation and disability. Clin Geriatr Med 26(3):387–399. https://doi.org/10.1016/j.cger.2010.04.001
Wolf O, Ström H, Milbrink J, Larsson S, Mallmin H (2009) Differences in hip bone mineral density may explain the hip fracture pattern in osteoarthritic hips. Acta Orthop 80(3):308–313. https://doi.org/10.3109/17453670903039528
Li B, Aspden RM (1997) Material properties of bone from the femoral neck and calcar femorale of patients with osteoporosis or osteoarthritis. Osteoporos Int 7(5):450–456. https://doi.org/10.1007/s001980050032
Stewart A, Black AJ (2000) Bone mineral density in osteoarthritis. Curr Opin Rheumatol 12:464–467. https://doi.org/10.1097/00002281-200009000-00021
Blain H, Chavassieux P, Portero-Muzy N, Bonnel F, Canovas F, Chammas M, Maury P, Delmas PD (2008) Cortical and trabecular bone distribution in the femoral neck in osteoporosis and osteoarthritis. Bone 43(5):862–868. https://doi.org/10.1016/j.bone.2008.07.236
Kuhns BD, Weber AE, Levy DM, Wuerz TH (2015) The natural history of femoroacetabular impingement. Front Surg 2(58). https://doi.org/10.3389/fsurg.2015.00058
Iolascon G, Gravina P, Luciano F, Palladino C, Gimigliano F (2013) Characteristics and circumstances of falls in hip fractures. Aging Clin Exp Res 25(1):133–135. https://doi.org/10.1007/s40520-013-0115-9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Maluta, T., Toso, G., Negri, S. et al. Correlation between hip osteoarthritis and proximal femoral fracture site: could it be protective for intracapsular neck fractures? A retrospective study on 320 cases. Osteoporos Int 30, 1591–1596 (2019). https://doi.org/10.1007/s00198-019-05015-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05015-5