Abstract
Introduction
Injury to the pancreas may lead to significant morbidity and mortality. We aim to assess pancreatic endocrine and exocrine functions and evaluated morphological regenerations of pancreas following partial pancreatectomy in patients with pancreatic trauma.
Methods
The study was performed between June 2016 and December 2017. Endocrine functions were assessed at the time of admission and at 6 months follow-up with 75 g oral glucose tolerance test (OGTT), serum insulin and C-peptide levels and HbA1c estimation and exocrine functions were assessed with fecal elastase test. Pancreatic volumetry was done with imaging scan at 1 month and 6 months post discharge.
Results
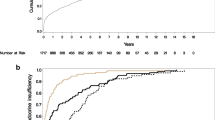
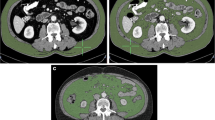
Twenty patients were studied with a median age of 30 years (range18–48) at the time of injury. All the patients were normoglycemic on admission; only one patient who underwent pancreatic resection developed diabetes mellitus at follow-up. Eight patients (40%) were found to be prediabetic by American Diabetes Association (ADA) criteria. Eleven patients (55%) had pancreatic exocrine insufficiency. Pancreatic volume increment, from the mean pancreatic volume of 48.65 to 54.29 cm3, was noted in patients who underwent partial pancreatectomy.
Conclusions
Patients with pancreatic trauma may develop biochemical endocrine and exocrine insufficiencies following pancreatic resection. Pancreatic volume increment requires further research in a larger study.





Similar content being viewed by others
References
Global status report on road safety 2018: summary. Geneva: World Health Organization; (WHO/NMH/NVI/18.20). Licence: CC BY-NC-SA 3.0 IGO.2018.
Ahmed N, Vernick JJ. Pancreatic injury. South Med J. 2009;102(12):1253–6. https://doi.org/10.1097/SMJ.0b013e3181c0dfca.
Petrone P, Moral Álvarez S, González Pérez M, Ceballos Esparragón J, Marini CP. Pancreatic trauma: management and literature review Traumatismos de páncreas: manejo y revisión de la literatura. Cir Esp. 2017;95(3):123–30. https://doi.org/10.1016/j.ciresp.2016.05.011.
Debi U, Kaur R, Prasad KK, Sinha SK, Sinha A, Singh K. Pancreatic trauma: a concise review. World J Gastroenterol. 2013;19(47):9003–11. https://doi.org/10.3748/wjg.v19.i47.9003.
Akhrass R, Yaffe MB, Brandt CP, Reigle M, Fallon WF Jr, Malangoni MA. Pancreatic trauma: a ten-year multi-institutional experience. Am Surg. 1997;63(7):598–604.
Yasugi H, Mizumoto R, Sakurai H, Honjo I. Changes in carbohydrate metabolism and endocrine function of remnant pancreas after major pancreatic resection. Am J Surg. 1976;132(5):577–80. https://doi.org/10.1016/0002-9610(76)90346-9.
Liu A, Carmichael KA, Schallom ME, Klinkenberg WD. Retrospective review of postoperative glycemic control in patients after distal pancreatectomy. Int J Surg. 2017;41:86–90. https://doi.org/10.1016/j.ijsu.2017.03.060.
Burkhart RA, Gerber SM, Tholey RM, et al. Incidence and severity of pancreatogenic diabetes after pancreatic resection. J Gastrointest Surg. 2015;19(2):217–25. https://doi.org/10.1007/s11605-014-2669-z.
Hirata K, Nakata B, Amano R, Yamazoe S, Kimura K, Hirakawa K. Predictive factors for change of diabetes mellitus status after pancreatectomy in preoperative diabetic and nondiabetic patients. J Gastrointest Surg. 2014;18(9):1597–603. https://doi.org/10.1007/s11605-014-2521-5.
Pearson KW, Scott D, Torrance B. Effects of partial surgical pancreatectomy in rats. I. Pancreatic regeneration. Gastroenterology. 1977;72(3):469–73.
Plachot C, Movassat J, Portha B. Impaired beta-cell regeneration after partial pancreatectomy in the adult Goto-Kakizaki rat, a spontaneous model of type II diabetes. Histochem Cell Biol. 2001;116(2):131–9. https://doi.org/10.1007/s004180100302.
Moore EE, Cogbill TH, Malangoni MA, et al. Organ injury scaling, II: pancreas, duodenum, small bowel, colon, and rectum. J Trauma. 1990;30(11):1427–9.
American Diabetes Association.2. Classification and diagnosis of diabetes: standards of medical care in diabetes—2018. Diabetes Care. 2018;41(Suppl 1):S13–27. https://doi.org/10.2337/dc18-S002.
den Biggelaar LJ, Sep SJ, Eussen SJ, et al. Discriminatory ability of simple OGTT-based beta cell function indices for prediction of prediabetes and type 2 diabetes: the CODAM study. Diabetologia. 2017;60(3):432–41. https://doi.org/10.1007/s00125-016-4165-3.
Phillips DIW, Clark PM, Hales CN, Osmond C. Understanding oral glucose tolerance: comparison of glucose or insulin measurements during the oral glucose tolerance test with specific measurements of insulin resistance and secretion. Diabet Med. 1994;11:286–92.
Faulenbach MV, Wright LA, Lorenzo C, et al. Impact of differences in glucose tolerance on the prevalence of a negative insulinogenic index. J Diabet Complicat. 2013;27:158–61.
Utzschneider KM, Prigeon RL, Faulenbach MV, et al. Oral disposition index predicts the development of future diabetes above and beyond fasting and two hour glucose levels. Diabet Care. 2009;32:335–41.
Löser C, Möllgaard A, Fölsch UR. Faecal elastase 1: a novel, highly sensitive, and specific tubeless pancreatic function test. Gut. 1996;39(4):580–6. https://doi.org/10.1136/gut.39.4.580.
Geraghty EM, Boone JM, McGahan JP, Jain K. Normal organ volume assessment from abdominal CT. Abdom Imaging. 2004;29(4):482–90. https://doi.org/10.1007/s00261-003-0139-2.
Patton JH Jr, Fabian TC. Complex pancreatic injuries. Surg Clin N Am. 1996;76(4):783–95. https://doi.org/10.1016/s0039-6109(05)70480-1.
Degiannis E, Glapa M, Loukogeorgakis SP, Smith MD. Management of pancreatic trauma. Injury. 2008;39(1):21–9. https://doi.org/10.1016/j.injury.2007.07.005.
Menahem B, Lim C, Lahat E, et al. Conservative and surgical management of pancreatic trauma in adult patients. Hepatobiliary Surg Nutr. 2016;5(6):470–7. https://doi.org/10.21037/hbsn.2016.07.01.
Sharpe JP, Magnotti LJ, Weinberg JA, et al. Impact of a defined management algorithm on outcome after traumatic pancreatic injury. J Trauma Acute Care Surg. 2012;72(1):100–5. https://doi.org/10.1097/TA.0b013e318241f09d.
Young PR Jr, Meredith JW, Baker CC, Thomason MH, Chang MC. Pancreatic injuries resulting from penetrating trauma: a multi-institution review. Am Surg. 1998;64(9):838–44.
Al-Ahmadi K, Ahmed N. Outcomes after pancreatic trauma: experience at a single institution. Can J Surg. 2008;51(2):118–24.
Steele M, Sheldon GF, Blaisdell FW. Pancreatic injuries. Methods of management. Arch Surg. 1973;106(4):544–9. https://doi.org/10.1001/archsurg.1973.01350160156026.
Sturim HS. Surgical management of traumatic transection of the pancreas: review of nine cases and literature review. Ann Surg. 1966;163(3):399–407. https://doi.org/10.1097/00000658-196603000-00012.
Anane-Sefah J, Norton LW, Eiseman B. Operative choice and technique following pancreatic injury. Arch Surg. 1975;110(2):161–6. https://doi.org/10.1001/archsurg.1975.01360080027004.
Yellin AE, Vecchione TR, Donovan AJ. Distal pancreatectomy for pancreatic trauma. Am J Surg. 1972;124(2):135–42. https://doi.org/10.1016/0002-9610(72)90004-9.
Morita T, Takasu O, Sakamoto T, et al. Long-term outcomes of pancreatic function following pancreatic trauma. Kurume Med J. 2017;63(3):53–60. https://doi.org/10.2739/kurumemedj.MS00001.
Mansfield N, Inaba K, Berg R, et al. Early pancreatic dysfunction after resection in trauma: an 18-year report from a level I trauma center. J Trauma Acute Care Surg. 2017;82(3):528–33. https://doi.org/10.1097/TA.0000000000001327.
Lim PW, Dinh KH, Sullivan M, et al. Thirty-day outcomes underestimate endocrine and exocrine insufficiency after pancreatic resection. HPB. 2016;18(4):360–6. https://doi.org/10.1016/j.hpb.2015.11.003.
Bouwens L, Rooman I. Regulation of pancreatic beta-cell mass. Physiol Rev. 2005;85(4):1255–70. https://doi.org/10.1152/physrev.00025.2004.
Paris M, Tourrel-Cuzin C, Plachot C, Ktorza A. Review: pancreatic beta-cell neogenesis revisited. Exp Diabesity Res. 2004;5(2):111–21. https://doi.org/10.1080/15438600490455079.
Banerjee M, Kanitkar M, Bhonde RR. Approaches towards endogenous pancreatic regeneration. Rev Diabet Stud. 2005;2(3):165–76. https://doi.org/10.1900/RDS.2005.2.165.
Acknowledgements
None
Funding
None.
Author information
Authors and Affiliations
Contributions
Drs.LC, SK, NT, PKG and AK conceptualized the research, and were involved in execution, analysis, manuscript preparation and final approval of the publication of this work. Drs.SS and AG helped with initial planning, preparation of manuscript and final approval of the publication of this work. Dr.NG helped in the initial planning and supervised the laboratory work of this research and helped in manuscript editing and final approval of the publication of this work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Rights and permissions
About this article
Cite this article
Colney, L., Tandon, N., Garg, P.K. et al. Exocrine and endocrine functions and pancreatic volume in patients with pancreatic trauma. Eur J Trauma Emerg Surg 48, 97–105 (2022). https://doi.org/10.1007/s00068-021-01638-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-021-01638-8