Abstract
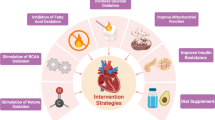
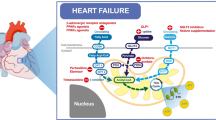
Myocardial substrate metabolism provides the energy needed for cardiac contraction and relaxation. The normal adult heart uses predominantly fatty acids (FAs) as its primary fuel source. However, the heart can switch and use glucose (and to a lesser extent, ketones, lactate, as well as endogenous triglycerides and glycogen), depending on the metabolic milieu and superimposed conditions. FAs are not a wholly better fuel than glucose, but they do provide more energy per mole than glucose. Conversely, glucose is the more oxygen-efficient fuel. Studies in animal models of heart failure (HF) fairly consistently demonstrate a shift away from myocardial fatty acid metabolism and toward glucose metabolism. Studies in humans are less consistent. Some show the same metabolic switch away from FA metabolism but not all. This may be due to differences in the etiology of HF, sex-related differences, or other mitigating factors. For example, obesity, insulin resistance, and diabetes are all related to an increased risk of HF and may complicate or contribute to its development. However, these conditions are associated with increased FA metabolism. This review will discuss aspects of human heart metabolism in systolic dysfunction as measured by the noninvasive, quantitative method—positron emission tomography. Continued research in this area is vital if we are to ameliorate HF by manipulating heart metabolism with the aim of increasing energy production and/or efficiency.



Similar content being viewed by others
References
Yuan CL, Sharma N, Gilge DA, Stanley WC, Li Y, Hatzoglou M, Previs SF (2008) Preserved protein synthesis in the heart in response to acute fasting and chronic food restriction despite reductions in liver and skeletal muscle. Am J Physiol Endocrinol Metab 295:E216–E222
Gill M, France J, Summers M, McBride BW, Milligan LP (1989) Simulation of the energy costs associated with protein turnover and Na+, K+-transport in growing lambs. J Nutr 119:1287–1299
Opie LH (1998) The heart: physiology, from cell to circulation. Lippincott-Raven, Philadelphia, 295 pp
Bing RJ (1965) Cardiac Metabolism. Physiol Rev 45:171–213
Peterson LR, Herrero P, McGill J, Schechtman KB, Kisrieva-Ware Z, Lesniak D, Gropler RJ (2008) Fatty acids and insulin modulate myocardial substrate metabolism in humans with type 1 diabetes. Diabetes 57:32–40
Kaijser L, Lassers BW, Wahlqvist ML, Carlson LA (1972) Myocardial lipid and carbohydrate metabolism in fasting men during prolonged exercise. J Appl Physiol 32:847–858
Gertz EW, Wisneski JA, Stanley WC, Neese RA (1988) Myocardial substrate utilization during exercise in humans. Dual carbon-labeled carbohydrate isotope experiments. J Clin Invest 82:2017–2025
Neely JR, Morgan HE (1974) Relationship between carbohydrate and lipid metabolism and the energy balance of heart muscle. Annu Rev Physiol 36:413–459
Kenchaiah S, Evans JC, Levy D, Wilson PW, Benjamin EJ, Larson MG, Kannel WB, Vasan RS (2002) Obesity and the risk of heart failure. N Engl J Med 347:305–313
Owan TE, Hodge DO, Herges RM, Jacobsen SJ, Roger VL, Redfield MM (2006) Trends in prevalence and outcome of heart failure with preserved ejection fraction. N Engl J Med 355:251–259
Peterson LR, Herrero P, Schechtman KB, Racette SB, Waggoner AD, Kisrieva-Ware Z, Dence C, Klein S, Marsala J, Meyer T, Gropler RJ (2004) Effect of obesity and insulin resistance on myocardial substrate metabolism and efficiency in young women. Circulation 109:2191–2196
Peterson LR, Soto PF, Herrero P, Mohammed BS, Avidan MS, Schechtman KB, Dence C, Gropler RJ (2008) Impact of gender on the myocardial metabolic response to obesity. JACC Cardiovasc Imaging 1:424–433
Kannel WB, McGee DL (1979) Diabetes and cardiovascular disease. The Framingham study. JAMA 241:2035–2038
Zhou YT, Grayburn P, Karim A, Shimabukuro M, Higa M, Baetens D, Orci L, Unger RH (2000) Lipotoxic heart disease in obese rats: implications for human obesity. Proc Natl Acad Sci USA 97:1784–1789
Listenberger LL, Ory DS, Schaffer JE (2001) Palmitate-induced apoptosis can occur through a ceramide-independent pathway. J Biol Chem 276:14890–14895
Herrero P, Peterson LR, McGill JB, Matthew S, Lesniak D, Dence C, Gropler RJ (2006) Increased myocardial fatty acid metabolism in patients with type 1 diabetes mellitus. J Am Coll Cardiol 47:598–604
McGill JB, LR Peterson, P Herrero, IM Saeed, C Recklein, AR Coggan, AJ Demoss, KB Schechtman, CS Dence, RJ Gropler (2011) Potentiation of abnormalities in myocardial metabolism with the development of diabetes in women with obesity and insulin resistance. J Nucl Cardiol 18:421-9; quiz 432-3
Peterson LR, Saeed IM, McGill JB, Herrero P, Schechtman KB, Gunawardena R, Recklein CL, Coggan AR, Demoss AJ, Dence CS, Gropler RJ (2011) Sex and type 2 diabetes: obesity-independent effects on LV substrate metabolism and relaxation in humans. Obesity (Silver Spring) 20(4):802–810
Barger PM, Kelly DP (1999) Fatty acid utilization in the hypertrophied and failing heart: molecular regulatory mechanisms. Am J Med Sci 318:36–42
Bishop SP, Altschuld RA (1970) Increased glycolytic metabolism in cardiac hypertrophy and congestive failure. Am J Physiol 218:153–159
Wittels B, Spann JFJ (1968) Defective lipid metabolism in the failing heart. J Clin Invest 47:1787–1794
Kantor PF, Robertson MA, Coe JY, Lopaschuk GD (1999) Volume overload hypertrophy of the newborn heart slows the maturation of enzymes involved in the regulation of fatty acid metabolism. J Am Coll Cardiol 33:1724–1734
Dávila-Román VG, Vedala G, Herrero P, de las Fuentes L, Rogers JG, Kelly DP, Gropler RJ (2002) Altered myocardial fatty acid and glucose metabolism in idiopathic dilated cardiomyopathy. J Am Coll Cardiol 40:271–277
Taylor M, Wallhaus TR, Degrado TR, Russell DC, Stanko P, Nickles RJ, Stone CK (2001) An evaluation of myocardial fatty acid and glucose uptake using PET with [18F]fluoro-6-thia-heptadecanoic acid and [18F]FDG in patients with congestive heart failure. J Nucl Med 42:55–62
Funada J, Betts TR, Hodson L, Humphreys SM, Timperley J, Frayn KN, Karpe F (2009) Substrate utilization by the failing heart by direct quantification using arterio-venous blood sampling. PLoS one 4:e7533
Tuunanen H, Engblom E, Naum A, Scheinin M, Nagren K, Airaksinen J, Nuutila P, Iozzo P, Ukkonen H, Knuuti J (2006) Decreased myocardial free fatty acid uptake in patients with idiopathic dilated cardiomyopathy: evidence of relationship with insulin resistance and LV dysfunction. J Card Fail 12:644–652
Shah A, Shannon RP (2003) Insulin resistance in dilated cardiomyopathy. Rev Cardiovasc Med 4(Suppl 6):S50–S57
Tuunanen H, Engblom E, Naum A, Nagren K, Hesse B, Airaksinen KE, Nuutila P, Iozzo P, Ukkonen H, Opie LH, Knuuti J (2006) Free fatty acid depletion acutely decreases cardiac work and efficiency in cardiomyopathic heart failure. Circulation 114:2130–2137
Neglia D, De Caterina A, Marraccini P, Natali A, Ciardetti M, Vecoli C, Gastaldelli A, Ciociaro D, Pellegrini P, Testa R, Menichetti L, L’Abbate A, Stanley WC, Recchia FA (2007) Impaired myocardial metabolic reserve and substrate selection flexibility during stress in patients with idiopathic dilated cardiomyopathy. Am J Physiol Heart Circ Physiol 293:H3270–H3278
Stanley WC, Lopaschuk GD, Hall JL, McCormack JG (1997) Regulation of myocardial carbohydrate metabolism under normal and ischaemic conditions. Potential for pharmacological interventions. Cardiovasc Res 33:243–257
de las Fuentes L, Herrero P, Peterson LR, Kelly DP, Gropler RJ, Dávila-Román VG (2003) Myocardial fatty acid metabolism: independent predictor of LV mass in hypertensive heart disease. Hypertension 41:83–87
Rijzewijk LJ, van der Meer RW, Lamb HJ, de Jong HW, Lubberink M, Romijn JA, Bax JJ, de Roos A, Twisk JW, Heine RJ, Lammertsma AA, Smit JW, Diamant M (2009) Altered myocardial substrate metabolism and decreased diastolic function in nonischemic human diabetic cardiomyopathy: studies with cardiac positron emission tomography and magnetic resonance imaging. J Am Coll Cardiol 54:1524–1532
Kates AM, Herrero P, Dence C, Soto P, Srinivasan M, Delano DG, Ehsani A, Gropler RJ (2003) Impact of aging on substrate metabolism by the human heart. J Am Coll Cardiol 41:293–299
Peterson LR, Soto PF, Herrero P, Schechtman KB, Dence C, Gropler RJ (2007) Sex differences in myocardial oxygen and glucose metabolism. J Nucl Cardiol 14:573–581
Wallhaus TR, Taylor M, DeGrado TR, Russell DC, Stanko P, Nickles RJ, Stone CK (2001) Myocardial free fatty acid and glucose use after carvedilol treatment in patients with congestive heart failure. Circulation 103:2441–2446
Eichhorn EJ, Heesch CM, Barnett JH, Alvarez LG, Fass SM, Grayburn PA, Hatfield BA, Marcoux LG, Malloy CR (1994) Effect of metoprolol on myocardial function and energetics in patients with nonischemic dilated cardiomyopathy: a randomized, double-blind, placebo-controlled study. J Am Coll Cardiol 24:1310–1320
Beanlands RS, Nahmias C, Gordon E, Coates G, deKemp R, Firnau G, Fallen E (2000) The effects of beta(1)-blockade on oxidative metabolism and the metabolic cost of ventricular work in patients with LV dysfunction: a double-blind, placebo-controlled, positron-emission tomography study. Circulation 102:2070–2075
Panchal AR, Stanley WC, Kerner J, Sabbah HN (1998) Beta-receptor blockade decreases carnitine palmitoyl transferase 1 activity in dogs with heart failure. J Card Fail 4:121–126
Yamauchi S, Takeishi Y, Minamihaba O, Arimoto T, Hirono O, Takahashi H, Miyamoto T, Nitobe J, Nozaki N, Tachibana H, Watanabe T, Fukui A, Kubota I (2003) Angiotensin—converting enzyme inhibition improves cardiac fatty acid metabolism in patients with congestive heart failure. Nucl Med Commun 24:901–906
Randle PJ, Garland PB, Hales CN, Newsholme EA (1963) The glucose fatty-acid cycle. Its role in insulin sensitivity and the metabolic disturbances of diabetes mellitus. Lancet 1:785–789
Jaswal JS, Keung W, Wang W, Ussher JR, Lopaschuk GD (2011) Targeting fatty acid and carbohydrate oxidation—a novel therapeutic intervention in the ischemic and failing heart. Biochim Biophys Acta 1813:1333–1350
Cottin Y, Lhuillier I, Gilson L, Zeller M, Bonnet C, Toulouse C, Louis P, Rochette L, Girard C, Wolf JE (2002) Glucose insulin potassium infusion improves systolic function in patients with chronic ischemic cardiomyopathy. Eur J Heart Fail 4:181–184
Vitale C, Wajngaten M, Sposato B, Gebara O, Rossini P, Fini M, Volterrani M, Rosano GM (2004) Trimetazidine improves LV function and quality of life in elderly patients with coronary artery disease. Eur Heart J 25:1814–1821
Fragasso G, Perseghin G, De Cobelli F, Esposito A, Palloshi A, Lattuada G, Scifo P, Calori G, Del Maschio A, Margonato A (2006) Effects of metabolic modulation by trimetazidine on LV function and phosphocreatine/adenosine triphosphate ratio in patients with heart failure. Eur Heart J 27:942–948
Di Napoli P, Taccardi AA, Barsotti A (2005) Long term cardioprotective action of trimetazidine and potential effect on the inflammatory process in patients with ischaemic dilated cardiomyopathy. Heart 91:161–165
El-Kady T, El-Sabban K, Gabaly M, Sabry A, Abdel-Hady S (2005) Effects of trimetazidine on myocardial perfusion and the contractile response of chronically dysfunctional myocardium in ischemic cardiomyopathy: a 24-month study. Am J Cardiovasc Drugs 5:271–278
Tuunanen H, Engblom E, Naum A, Nagren K, Scheinin M, Hesse B, Juhani Airaksinen KE, Nuutila P, Iozzo P, Ukkonen H, Opie LH, Knuuti J (2008) Trimetazidine, a metabolic modulator, has cardiac and extracardiac benefits in idiopathic dilated cardiomyopathy. Circulation 118:1250–1258
Chandler MP, Stanley WC, Morita H, Suzuki G, Roth BA, Blackburn B, Wolff A, Sabbah HN (2002) Short-term treatment with ranolazine improves mechanical efficiency in dogs with chronic heart failure. Circ Res 91:278–280
Sabbah HN, Chandler MP, Mishima T, Suzuki G, Chaudhry P, Nass O, Biesiadecki BJ, Blackburn B, Wolff A, Stanley WC (2002) Ranolazine, a partial fatty acid oxidation (pFOX) inhibitor, improves LV function in dogs with chronic heart failure. J Card Fail 8:416–422
Holubarsch CJ, Rohrbach M, Karrasch M, Boehm E, Polonski L, Ponikowski P, Rhein S (2007) A double-blind randomized multicentre clinical trial to evaluate the efficacy and safety of two doses of etomoxir in comparison with placebo in patients with moderate congestive heart failure: the ERGO (etomoxir for the recovery of glucose oxidation) study. Clin Sci (Lond) 113:205–212
Lee L, Campbell R, Scheuermann-Freestone M, Taylor R, Gunaruwan P, Williams L, Ashrafian H, Horowitz J, Fraser AG, Clarke K, Frenneaux M (2005) Metabolic modulation with perhexiline in chronic heart failure: a randomized, controlled trial of short-term use of a novel treatment. Circulation 112:3280–3288
Bansal M, Chan J, Leano R, Pillans P, Horowitz J, Marwick TH (2010) Effects of perhexiline on myocardial deformation in patients with ischaemic LV dysfunction. Int J Cardiol 139:107–112
Acknowledgments
The authors would like to acknowledge the grants from P20 HL113444 (NIH, Bethesda, MD), ICTS (Institute for Clinical and Translational Sciences, St. Louis, MO), DRTC (Diabetes Research and Training Center, St. Louis, MO).
Conflict of interest
Dr. Peterson is on the Merck Speaker’s Bureau. Drs. Coggan and Kadkhodayan have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kadkhodayan, A., Coggan, A.R. & Peterson, L.R. A “PET” area of interest: myocardial metabolism in human systolic heart failure. Heart Fail Rev 18, 567–574 (2013). https://doi.org/10.1007/s10741-012-9360-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-012-9360-9