Abstract
Purpose
The aim of the study was to compare plasma concentrations of rifampicin (RMP), isoniazid (INH) and pyrazinamide (PZA) between tuberculosis (TB) patients with and without diabetes mellitus (DM).
Methods
Two-hour post-dosing concentrations of RMP, INH and PZA were determined in adult TB patients that were studied with (n = 452) and without DM (n = 1460), treated with a thrice-weekly regimen in India. Drug concentrations were estimated by HPLC.
Results
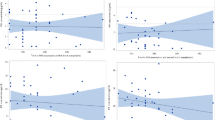
The median (IQR) INH [6.6 (3.9–10.0) and 7.8 (4.6–11.3)] and PZA [31.0 (22.3–38.0) and 34.1 (24.6–42.7)] microgram per milliliter concentrations were significantly lower in diabetic than non-diabetic TB patients (p < 0.001 for both drugs). Blood glucose was negatively correlated with plasma INH (r = −0.09, p < 0.001) and PZA (r = −0.092, p < 0.001). Multiple linear regression analysis showed RMP, INH and PZA concentrations were influenced by age and drug doses, INH and PZA by DM, RMP by alcohol use and PZA by gender and category of ATT. DM reduced INH and PZA concentrations by 0.8 and 3.0 μg/ml, respectively.
Conclusions
TB patients with DM had lower INH and PZA concentrations. Negative correlation between blood glucose and drug concentrations suggests delayed absorption/faster elimination of INH and PZA in the presence of elevated glucose.

Similar content being viewed by others
References
Hu FB, Manson JE, Stampfer MJ, Colditz G, Liu S, Solomon CG, Willett WC (2001) Diet, lifestyle, and the risk of type 2 diabetes mellitus in women. New Engl J Med 345:790–797
Van Dam RM, Rimm EB, Willett WC, Stampfer MJ, Hu FB (2002) Dietary patterns and risk for type 2 diabetes mellitus in US men. Ann Intern Med 136:201–209
Popkin BM (2008) Will China’s nutrition transition overwhelm in health care system and slow economic growth? Health Aff (Milwood) 27:1064–1076
Mozaffarian D, Kamineni A, Carnethon M, Djousse L, Mukamal KJ, Siscovick D (2009) Lifestyle risk factors and new-onset diabetes mellitus in older adults: the cardiovascular health study. Arch Intern Med 169:798–807
Dooley KE, Chaisson RE (2009) Tuberculosis and diabetes mellitus: convergence of two epidemics. Lancet Infect Dis 9:737–746
Bashar M, Alcabes P, Rom WN, Condos R (2001) Increased incidence of multidrug-resistant tuberculosis in diabetic patients on the Bellevue Chest Service, 1987 to 1997. Chest 120:1514–1519
Fishet-Hosch SP, Whitney E, McCormick JB, Crespo G, Smith B, Rahbar MH, Restrepo BI (2008) Type 2 diabetes and multidrug-resistant tuberculosis. Scand J Infect Dis 40:888–893
Nijland HMJ, Ruslami R, Stalenhost JE, Alisjahbana B, Nelwan RH, van der Ven AJ, Danusantoso H, Aarnoutse RE, van Crevel R (2006) Exposure to rifampicin is strongly reduced in patients with tuberculosis and type 2 diabetes. Clin Infect Dis 43:848–854
Babalik A, Ulus IH, Bakirci N, Kuyuca T, Arpag H, Dagyildizi L, Capaner E (2013) Plasma concentrations of isoniazid and rifampin are decreased in adult pulmonary tuberculosis patients with diabetes mellitus. Antimicrob Agents Chemother:5740–5742
Revised National TB Control Programme, Annual status report (2011) Central TB Division, Government of India. TB India. 98–101
Abdullah A, Peloquin CA (2014) Therapeutic drug monitoring in the treatment of tuberculosis: an update. Drugs 74:839–854
Hemanth Kumar AK, Immanuel C, Ramachandran G, Chelvi KS, Lalitha V, Prema G (2004) A validated high performance liquid chromatography method for the determination of rifampicin and desacetyl rifampicin in plasma and urine. Indian J Pharmacol 36:231–233
Hemanth Kumar AK, Sudha V, Ramachandran G (2012) Simple and rapid liquid chromatography method for simultaneous determination of isoniazid and pyrazinamide in plasma. SAARC J TB Lung diseases & HIV/AIDS 9:13–18
Hemanth Kumar AK, Kannan T, Chandrasekaran V, Sudha V, Vijayakumar A, Ramesh K, Lavanya J, Swaminathan S, Ramachandran G (2016) Pharmacokinetics of thrice weekly rifampicin, isoniazid and pyrazinamide in adult tuberculosis patients in India. Int J Tuberc Lung Dis 20(9):1236–1241
Singla R, Khan N, Al-Sharif N, Al-Sayegh MO, Shaikh MA, Osman MM (2006) Influence of diabetes on manifestations and treatment outcome of pulmonary TB patients. Int J Tuberc Lung Dis 10:74–79
Wang CS, Yang HC, Chen HC, Chuang SH, Chong IW, Hwang JJ, Huang MS (2009) Impact of type 2 diabetes on manifestations and treatment outcome of pulmonary tuberculosis. Epid Infect 137:203–210
Chang JT, Dou HY, Yen CL, Wu YH, Huang RM, Lin HJ, Su IJ, Shieh CC (2011) Effect of type 2 diabetes mellitus on the clinical severity and treatment outcome in patients with pulmonary tuberculosis: a potential role in the emergence of multi-drug resistance. J Formos Med Assoc 110:372–381
Ruslami R, Nijland HMJ, Adhiarta IGN, Kariadi HKS, Alisjahbana B, Aarnoutse RE, van Crevel R (2010) Pharmacokinetics of antituberculosis drugs in pulmonary tuberculosis patients with type 2 diabetes. Antimicrob Agents Chemother 54:1068–1074
Requena-Mendez A, Davies G, Ardrey A, Jave O, Lopez-Romero SL, Ward SA, Moore DA (2012) Pharmacokinetics of rifampicin in Peruvian tuberculosis patients with and without comorbid diabetes or HIV. Antimicrob Agents Chemother 6:2357–2363
Matuski Y, Katakuse Y, Matsuura H, Kiwada H, Goromaru T (1991) Effects of glucose and ascorbic acid on absorption and first pass metabolism of isoniazid in rats. Chem Pharmaceut Bull (Tokyo) 39:445–448
Banu Rekha VV, Balasubramaninan R, Swaminathan S, Ramachandran R, Rahman F, Sundaram V, Thyagarajan K, Selvakumar N, Adhilakshmi AR, Iliyas S, Narayanan PR (2007) Sputum conversion at the end of intensive phase of category-I regimen in the treatment of pulmonary tuberculosis patients with diabetes mellitus or HIV infection: an analysis of risk factors. Indian J Med Res 126:452–458
Balasubramanian R, Ramanathan U, Thyagarajan K, Ramachandran R, Rajaram K, Bhaskar D, Shantharam Hariharan RS, Narayanan PR (2007) Evaluation of an intermittent six-month regimen in new pulmonary tuberculosis patients with diabetes mellitus. Indian J Tub 54:168–176
Viswanathan V, Vigneswari A, Selvan K, Satyavani K, Rajeswari R, Kapur A (2014) Effect of diabetes on treatment outcome of smear-positive pulmonary tuberculosis—a report from South India. J Diab Complic 28:162–165
Alisjahbana B, Sahiratmadja E, Nelwan EJ, Purwa AM, Ahmad Y, Ottenhoff TH, Nelwan RH, Parwati I, van der Meer JW, van Crevel R (2007) The effect of type 2 diabetes mellitus on the presentation and treatment response of pulmonary tuberculosis. Clin Infect Dis 45:428–435
Dooley KE, Tang T, Golub JE, Dorman SE, Cronin W (2009) Impact of diabetes mellitus on treatment outcomes of patients with active tuberculosis. AmJTrop Med Hyg 80:634–639
Zhang Q, Xiao H, Sugawara I (2009) Tuberculosis complicated by diabetes mellitus at Shanghai Pulmonary Hospital, China. Jap J Infect Dis 62:390–391
Chang MJ, Chae J, Yun HY, Lee JI, Choi HD, Kim J, Park JS, Cho YJ, Yoon HI, Lee CT, Shin WG, Lee JH (2015) Effects of type 2 diabetes mellitus on the population pharmacokinetics of rifampicin in tuberculosis patients. Tuberculosis 95:54–59
Heysell SK, Moore JL, Keller SJ, Houpt ER (2010) Therapeutic drug monitoring for slow response to tuberculosis treatment in a state control program, Virginia, USA. Emerg Infect Dis 16:1546–1553
Acknowledgments
The authors thank the patients who took part in the study, staff of the clinical biochemistry laboratory for blood glucose estimations, data entry operators, field investigators engaged in patient recruitment, staff at the RNTCP treatment centres in the Chennai Corporation and financial support by the United States Agency for International Development through World Health Organisation, SEARO, New Delhi, India.
Authors’ contributions
GR designed the study and developed the protocol, AKH and GR conducted the study, GR obtained regulatory approvals, AKH supervised drug estimations, VS carried out drug estimations by HPLC, LM and JL recruited study patients, VC and TK performed statistical analysis, GR drafted the manuscript and SS provided critical inputs and overall guidance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study commenced after obtaining approval from the Institutional Ethics Committee of the National Institute for Research in Tuberculosis (NIRT).
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Kumar, A.K.H., Chandrasekaran, V., Kannan, T. et al. Anti-tuberculosis drug concentrations in tuberculosis patients with and without diabetes mellitus. Eur J Clin Pharmacol 73, 65–70 (2017). https://doi.org/10.1007/s00228-016-2132-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-016-2132-z