Abstract
Background
Osteogenesis imperfecta (OI) is a genetic connective tissue disorder characterized by skeletal deformity and increased risk of fracture. Independent mobility is of concern for OI patients as it is associated with the quality of life. The present study investigates the variation of kinetic and kinematic gait parameters of type IV OI subjects and compares them with age-matched healthy subjects.
Materials and Methods
Gait analysis is performed on five type IV OI patients and six age-matched normal subjects. Spatiotemporal, kinematic, and kinetic data are obtained using Helen Hayes marker placement protocol.
Results
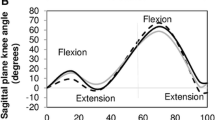
The results indicate an imprecise double-humped profile for vertical ground reaction force (GRF) with reduced ankle push off power and walking speed for OI subjects. Moreover, a comparison of vertical GRFs in OI subjects with that of healthy subjects suggests lower values for the former. The results encourage and motivate for further investigation with a bigger set of subjects.
Conclusion
This information may be useful in developing a better understanding of pathological gait in type IV OI subjects, which ultimately helps the design of subject-specific implants, surgical preplanning, and rehabilitation.
Similar content being viewed by others
References
Sillence DO, Rimoin DL. Classification of osteogenesis imperfect. Lancet 1978;1:1041–2.
Forlino A, Cabral WA, Barnes AM, Marini JC. New perspectives on osteogenesis imperfecta. Nat Rev Endocrinol 2011;7:540–57.
Forlino A, Marini JC. Osteogenesis imperfecta. Lancet 2016;387:1657–71.
Sillence DO, Senn A, Danks DM. Genetic heterogeneity in osteogenesis imperfecta. J Med Genet 1979;16:101–16.
Harris GF, Smith PA, editors. Pediatric Gait: A New Millennium in Clinical Care and Motion Analysis Technology. Institute of Electrical and Electronics Engineers (IEEE); 2000.
Rauch F, Glorieux FH. Osteogenesis imperfecta, current and future medical treatment. Am J Med Genet C Semin Med Genet 2005;139C: 31–7.
Rauch F, Travers R, Glorieux FH. Pamidronate in children with osteogenesis imperfecta: Histomorphometric effects of long term therapy. J Clin Endocrinol Metab 2006;91:511–6.
Rauch F, Travers R, Plotkin H, Glorieux FH. The effects of intravenous pamidronate on the bone tissue of children and adolescents with osteogenesis imperfecta. J Clin Invest 2002;110:1293–9.
Trejo P, Rauch F. Osteogenesis imperfecta in children and adolescents-new developments in diagnosis and treatment. Osteoporos Int 2016;27:3427–37.
Weber M, Roschger P, Fratzl-Zelman N, Schöberl T, Rauch F, Glorieux FH, et al. Pamidronate does not adversely affect bone intrinsic material properties in children with osteogenesis imperfecta. Bone 2006;39:616–22.
Murray D, Young BH. Osteogenesis imperfecta treated by fixation with intramedullary rod. South Med J 1960;53:1142–3.
Tiley F, Albright JA. Osteogenesis imperfecta: Treatment by multiple osteotomy and intramedullary rod insertion. Report on thirteen patients. J Bone Joint Surg Am 1973;55:701–13.
Stockley I, Bell MJ, Sharrard WJ. The role of expanding intramedullary rods in osteogenesis imperfecta. J Bone Joint Surg Br 1989;71:422–7.
Moreira CLM, Lima MAF, Cardoso MHC, Gomes Junior SCS, Lopes PB, Llerena Junior JC. Independent walk in osteogenesis imperfecta. Acta Ortop Bras 2011;19:312–5.
Vanz AP, van de Sande Lee J, Pinheiro B, Zambrano M, Brizola E, da Rocha NS, et al. Health-related quality of life of children and adolescents with osteogenesis imperfecta: A cross-sectional study using pedsQL™. BMC Pediatr 2018;18:95.
Hill CL, Baird WO, Walters SJ. Quality of life in children and adolescents with osteogenesis imperfecta: A qualitative interview based study. Health Qual Life Outcomes 2014;12:54.
Donnan L. Preoperative assessment for complex lower limb deformity. J Pediatr Orthop 2017;37 Suppl 2:S12–S17.
Feng J, Wick J, Bompiani E, Aiona M. Applications of gait analysis in pediatric orthopaedics. Curr Orthop Pract 2016;27:455–64.
Lofterød B, Terjesen T, Skaaret I, Huse AB, Jahnsen R. Preoperative gait analysis has a substantial effect on orthopedic decision making in children with cerebral palsy: Comparison between clinical evaluation and gait analysis in 60 patients. Acta Orthop 2007;78:74–80.
Thomason P, Rodda J, Sangeux M, Selber P, Graham K. Management of children with ambulatory cerebral palsy: An evidence-based review. Commentary by hugh Williamson gait laboratory staff. J Pediatr Orthop 2012;32 Suppl 2:S182–6.
Graf A, Hassani S, Krzak J, Caudill A, Flanagan A, Bajorunaite R, et al. Gait characteristics and functional assessment of children with type I osteogenesis imperfecta. J Orthop Res 2009;27:1182–90.
Garman CR, Graf A, Krzak J, Caudill A, Smith P, Harris G, et al. Gait deviations in children with osteogenesis imperfecta type I. J Pediatr Orthop 2017; DOI: 10.1097/BPO.0000000000001062, PMID: 28777275 (Ahead of print).
Graf A, Krzak J, Caudill A, Flanagan A, Smith P, Harris GF. Quantitative assessment of children with osteogenesis imperfecta. In: Smith P, Rauch F, Harris G, editors. Transitional Care in Osteogenesis Imperfecta: Advances in Biology, Technology, and Clinical Practice, 1st ed. Chicago: Shriners Hospitals for Children-Chicago; 2016. p. 217–32.
Samson MM, Crowe A, de Vreede PL, Dessens JA, Duursma SA, Verhaar HJ, et al. Differences in gait parameters at a preferred walking speed in healthy subjects due to age, height and body weight. Aging (Milano) 2001;13:16–21.
Modenese L, Phillips ATM. Prediction of hip contact forces and muscle activations during walking at different speeds. Multibody Syst Dyn 2012;28:157–68.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Badhyal, S., Dhole, S.R., Gopinathan, N.R. et al. Kinetic and Kinematic Analysis of Gait in Type IV Osteogenesis Imperfecta Patients: A Comparative Study. JOIO 53, 560–566 (2019). https://doi.org/10.4103/ortho.IJOrtho_291_18
Published:
Issue Date:
DOI: https://doi.org/10.4103/ortho.IJOrtho_291_18