Summary
Abstract
Troglitazone is the first of a new group of oral antidiabetic drugs, the thiazolidinediones, and is indicated for the treatment of patients with type 2 (non-insulin-dependent) diabetes mellitus. Troglitazone acts by enhancing the effects of insulin at peripheral target sites and, unlike the sulphonylurea drugs, is not associated with hypoglycaemia when administered as monotherapy.
Clinical trials with troglitazone (usually 200 to 600 mg/day) in patients with type 2 diabetes mellitus consistently showed marked improvement in glycaemic control, as well as reductions in fasting serum insulin, C-peptide and triglyceride levels. Comparative studies with either glibenclamide (glyburide) or metformin indicated similar glycaemic control with troglitazone or these agents. Serum insulin levels were lower with troglitazone than with glibenclamide. Clinical trials of up to approximately 2 years’ duration showed that glycaemic control is maintained with troglitazone on a long term basis.
In general, troglitazone is well tolerated by the majority of patients. However, discontinuation of troglitazone because of elevated liver enzyme levels occurs in approximately 2% of patients receiving the drug, and frequent monitoring of liver enzymes is required (e.g. at least 11 times during the first year of therapy). Among patients who started troglitazone therapy in 1998 (after the incorporation of a boxed warning and increased monitoring requirements in the product labelling), the estimated risk of liver-related death is approximately 1 in 100 000.
Conclusions: Troglitazone improves the ability of target cells to respond to insulin. The drug has been shown to improve glycaemic control in patients with type 2 diabetes mellitus when used as monotherapy or in combination with other oral antidiabetic drugs or insulin, and its efficacy is similar to that of glibenclamide or metformin. Although troglitazone is generally well tolerated, close monitoring of liver enzyme function is required to minimise the rare occurrence of serious hepatic dysfunction. Drug acquisition and liver function monitoring costs, as well as potential adverse effects, are important factors that may ultimately determine the precise place of troglitazone in the management of type 2 diabetes mellitus. Nevertheless, as the first member of a new class of oral antidiabetic agents, the thiazolidinediones, troglitazone offers an effective treatment option in patients with type 2 diabetes mellitus through its action of improving insulin sensitivity.
Overview of Type 2 Diabetes Mellitus
The prevalence of type 2 diabetes mellitus is approximately 5% in North America and Europe, and increases with age. Diabetes mellitus is even more common among certain populations, such as Native North Americans and African Americans. Multiple mechanisms appear to be involved in the pathogenesis of type 2 diabetes mellitus, including impaired insulin secretion by pancreatic β cells, increased hepatic gluconeogenesis, and reduced glucose uptake by skeletal muscle and adipose tissue (peripheral insulin resistance). These effects lead to hyperglycaemia in the short term, and to micro- and macrovascular complications in the long term. Available evidence suggests that improving glycaemic control reduces the risk of diabetic complications, although this relationship is more clear for microvascular complications such as retinopathy and nephropathy than for macrovascular complications such as coronary heart disease.
Pharmacodynamic Properties and Mechanism of Action
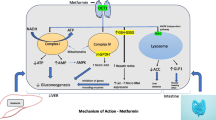
Troglitazone enhances the effects of insulin at peripheral tissue sites (skeletal muscle and adipose tissue), thereby increasing insulin-dependent glucose disposal. Some studies have also shown that troglitazone moderately reduces hepatic glucose production, although this effect has not been consistently demonstrated. Unlike sulphonylurea agents, troglitazone does not directly stimulate the release of insulin from pancreatic β cells. The improved insulin sensitivity demonstrated with troglitazone in patients with type 2 diabetes mellitus was accompanied by improvements in glycaemic control and reduced serum insulin levels. Troglitazone has a significant antihyperglycaemic effect in animal models of both genetic and non-genetic insulin resistance, but not in animal models of insulin deficiency. The mechanism of action of troglitazone at the cellular level has not been fully elucidated. One hypothesis is that binding of troglitazone to peroxisome proliferator-activated receptor-γ (PPARγ) may lead to regulation of the transcription of a number of insulin-responsive genes intimately involved in the control of glucose and lipid metabolism. Other actions may also be involved in the cellular mechanism of troglitazone.
Pharmacokinetic Properties
In healthy volunteers, troglitazone 200 to 600 mg/day achieves peak plasma drug concentrations of 0.9 to 2.8 mg/L approximately 2 to 3 hours after oral administration. It is extensively bound to plasma protein (>99%) and has a steady-state volume of distribution of 2.5 L/kg. The elimination half-life of troglitazone is 9 to 34 hours, allowing for once daily administration of the drug. Troglitazone is extensively metabolised by the liver to 3 main metabolites: the sulphate conjugate (present at a plasma concentration approximately 7 to 10 times that of the parent drug), the quinone metabolite (plasma concentration approximately equal to that of troglitazone) and the glucuronide metabolite (low or negligible plasma concentrations). Animal data indicate that the quinone metabolite has modest pharmacological activity, although the clinical relevance of this finding is unclear. Almost none of an administered dose of troglitazone is eliminated unchanged in the urine.
Therapeutic Use
In clinical trials of patients with type 2 diabetes mellitus, administration of troglitazone, alone or in combination with other antidiabetic agents, was consistently associated with improved glycaemic control compared with placebo or baseline. Statistically and clinically significant reductions were achieved in fasting serum or plasma glucose (FSG or FPG) levels and glycosylated haemoglobin (HbA1c) values. Fasting serum insulin, C-peptide and triglyceride levels were also typically reduced (by 13 to 26% from baseline in the case of triglyceride levels).
In large (n > 100) clinical trials conducted in North America in which troglitazone was administered as monotherapy (typically 200 to 800 mg/day for 12 to 26 weeks), FSG was reduced by approximately 11 to 33% and HbA1c by about 5 to 15% (relative reduction) compared with placebo or baseline values. Although a clear overall dose-response pattern was not evident, troglitazone was consistently effective over its recommended dosage range (200 to 600 mg/day in the US). The effects of troglitazone on glycaemic control were maintained for ≥1 year in a trial in which dosage adjustments were allowed after a 6-month fixed dosage interval. Results of a large study in elderly patients (mean age 75 years) with type 2 diabetes mellitus were similar to those of studies conducted in patients not selected by age. In comparative trials, troglitazone 600 or 800 mg/day had similar efficacy to glibenclamide (glyburide) titrated to response, in terms of glycaemic control, although only troglitazone was associated with reductions in serum insulin levels. Comparisons between troglitazone and metformin in commonly used dosage regimens also showed similar effects on glycaemic control. Results of studies with troglitazone monotherapy conducted in Japan were very similar to those conducted in Europe and North America.
Concomitant treatment with troglitazone 200 to 600 mg/day, plus either glibenclamide 12 mg/day (n = 545) or metformin 1000mg twice daily (n = 28) was more effective at achieving glycaemic control than monotherapy with these drugs. An open-label extension of troglitazone plus glibenclamide therapy demonstrated that glycaemic control was maintained with combined therapy on a long term basis (116 weeks). Other trials of up to 1 year’s duration also showed significantly greater reductions in FPG and HbA1c when troglitazone was added to sulphonylurea therapy compared with sulphonylurea monotherapy.
The addition of troglitazone 200 to 600 mg/day to insulin therapy (≥30 U/day) in patients with type 2 diabetes mellitus reduced FSG levels, insulin dosage requirements and HbAic values, with glycaemic control maintained for up to 23 months in an extension of the largest study (n = 286 for the long term extension).
Tolerability
In clinical trials, the incidence and type of adverse events associated with troglitazone were broadly similar to those observed with placebo. Tolerability data have been pooled from studies conducted in North American patients with type 2 diabetes mellitus receiving troglitazone (n = 1450) or placebo (n = 492). The most frequently reported adverse events with both troglitazone and placebo were infection (18 vs 22%), headache (11 vs 11%) and pain (10 vs 14%). Other adverse events included accidental injury, asthenia, dizziness, back pain, nausea, rhinitis, diarrhoea, urinary tract infection, peripheral oedema and pharyngitis; these were reported in 5 to 8% of troglitazone recipients and 4 to 7% of placebo recipients. The rate of treatment withdrawal during clinical trials was approximately 4% for both troglitazone and placebo. Unlike sulphonylurea drugs, troglitazone is not associated with hypoglycaemic reactions when administered as monotherapy.
Reversible elevations in serum liver enzymes (ALT levels >3 times the upper limit of normal) were noted in 1.9% of patients receiving troglitazone and 0.6% of placebo recipients in North American trials. Since its market launch, troglitazone has been associated with a number of reports of idiosyncratic liver dysfunction which, in a small number of cases, has led to death or the need for liver transplantation. Thus, although approximately 2% of patients receiving troglitazone can be expected to discontinue therapy because of elevated liver enzymes, the overall incidence of permanent liver damage leading to death or liver transplantation is estimated to be about 1 case in every 50 000 to 60 000 patients treated with troglitazone in the US. The manufacturer has introduced a series of labelling changes for the drug, requiring frequent monitoring of liver enzymes (e.g. at least 11 times during the first year of therapy) as well as careful monitoring of clinical signs of liver dysfunction. This appears to have reduced the risk of permanent liver damage: recent estimates focusing specifically on the risk of death related to liver dysfunction among patients who started troglitazone therapy in the US in 1998 indicate a risk of approximately 1 in 100 000.
Drug Interactions
Troglitazone appears to induce drug metabolism by the cytochrome P450 (CYP) 3A isoenzyme pathway, and concomitant administration with a variety of CYP3A substrates has resulted in decreased plasma concentrations of these drugs. Such substrates include terfenadine, cyclosporin and components of oral contraceptives (ethinylestradiol and norethindrone; potentially leading to loss of contraceptive efficacy). Concurrent administration of troglitazone and cholestyramine is not recommended because cholestyramine markedly reduces the absorption of troglitazone.
Dosage and Administration
Troglitazone is administered orally and should be taken with a meal, since this enhances absorption of the drug. The recommended dosage regimen of troglitazone in the US is 200 to 600mg once daily, with the usual dosage being 400mg once daily. If there is no response to the maximum dosage after 1 month, the drug should be discontinued in favour of alternative therapy. In Japan, the recommended dosage regimen of troglitazone is 200mg twice daily (after meals in the morning and evening).
When troglitazone is added to insulin therapy, it should be initiated at a dosage of 200mg once daily and the current insulin dosage should be continued (but may subsequently need to be reduced depending on glucose-lowering response). The dosage of troglitazone may be increased after 2 to 4 weeks for patients not responding adequately to this combined therapy. Dosage adjustment of troglitazone in patients with renal insufficiency is not necessary. Troglitazone is not recommended in patients with hepatic impairment. All patients receiving troglitazone should be monitored closely for laboratory and clinical signs of liver damage.
Similar content being viewed by others
References
Spencer CM, Markham A. Troglitazone. Drags 1997 Jul; 54: 89–101
Harris MI. Diabetes in America (2nd edition). NIH Publication No. 95-1468, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda (MD), 1995
Cowie CC, Eberhardt MS, editors. Diabetes 1996 vital statistics. Alexandria (VA): American Diabetes Association, 1996. 1–102
Tan GH, Nelson RL. Pharmacologic treatment options for non-insulin-dependent diabetes mellitus. Mayo Clin Proc 1996 Aug; 71: 763–8
Songer TJ, Zimmet PZ. Epidemiology of type II diabetes. An International perspective. Pharmacoeconomics 1995; 8 Suppl. 1: 1–11
McKeigue PM, Marmot MG, Syndercombe-Court YD, et al. Diabetes, hyperinsulinaemia and coronary risk factors in Bangladeshis in east London. Br Heart J 1988; 60: 990–6
The pharmacological treatment of hyperglycemia in NIDDM. Diabetes Care 1996 Jan; 19 Suppl. 1: 54–61
O’Rahilly S. Non-insulin dependent diabetes mellitus: the gathering storm. BMJ 1997 Mar 29; 314: 955–9
Hodge AM, Dowse GK, Zimmet PZ, et al. Prevalence and secular trends in obesity in Pacific and Indian Ocean island populations. Obesity Research 1995; 3 Suppl. 2: 77s–87s
Bressler R, Johnson DG. Oral antidiabetic drug use in the elderly. Drugs Aging 1996 Dec; 9: 418–37
Kuehnle HF. New therapeutic agents for the treatment of NIDDM. Exp Clin Endocrinol Diabetes 1996; 104(2): 93–101
Saltiel AR, Olefsky JM. Thiazolidinediones in the treatment of insulin resistance and type II diabetes. Diabetes 1996 Dec; 45: 1661–9
Francisco Jr GE, Brooks PJ. Diabetes mellitus. In: DiPiro JT et al., editors. Pharmacotherapy: a pathophysiologic approach. 2nd ed. Norwalk (CT): Appleton & Lange, 1993: 1121–45
Savage PJ. Cardiovascular complications of diabetes mellitus: what we know and what we need to know about their prevention. Ann Intern Med 1996 Jan 1; 124 (Pt 2): 123–6
Dean JD, Durrington PN. Treatment of dyslipoproteinaemia in diabetes mellitus. Diabetic Med 1996 Apr; 13: 297–312
Orchard TJ, Forrest KY-Z, Ellis D, et al. Cumulative glycemic exposure and microvascular complications in insulin-dependent diabetes mellitus. Arch Intern Med 1997; 157 (1851-1856)
UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet 1998 Sep 12; 352: 837–53
UK Prospective Diabetes study (UKPDS) Group. Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet 1998 Sep 12; 352: 854–65
University Group Diabetes Program. Effects of hypoglycemic agents on vascular complications in patients with adult-onset diabetes VII: mortality and selected nonfatal events with insulin treatment. JAMA 1978; 240: 37–42
Nathan DM. Some answers, more controversy, from UKPDS [commentary]. Lancet 1998 Sept 12; 352: 832–3
The Diabetes Control and Complications Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993; 329: 977–86
Saltiel AR, Horikoshi H. Thiazolidinediones are novel insulin-sensitizing agents. Curr Opin Endocrinol Diabetes 1995; 2: 341–7
Whitcomb RW, Saltiel AR. Thiazolidinediones. Expert Opin Invest Drug 1995 Dec; 4: 1299–309
Martin G, Schoonjans K, Staels B, et al. PPARγ activators improve glucose homeostasis by stimulating fatty acid uptake in the adipocytes. Atherosclerosis 1998; 137 Suppl: S75–80
Lehmann JM, Moore LB, Smith-Oliver TA, et al. An anti-diabetic thiazolidinedione is a high affinity ligand for peroxisome proliferator-activated receptorγ (PPARγ). J Biol Chem 1995; 270(22): 12953–6
Berger J, Bailey P, Biswas C, et al. Thiazolidinediones produce a conformational change in peroxisomal proliferator-activated receptor-γ: binding and activation correlated with anti-diabetic actions in db/db mice. Endocrinology 1996; 137(10): 4189–95
Wilson TM, Cobb JE, Cowan DJ, et al. The structure-activity relationship between peroxisome proliferator-activated receptor γ agonism and the antihyperglycemic activity of thiazolidinediones. J Med Chem 1996; 39: 665–8
Corrêa JCN, Hilsted J, Eckland D, et al. Investigation of twice or three times daily dose regimen of troglitazone, an insulin action enhancer, in patients with non insulin dependent diabetes mellitus. Eur J Clin Res 1997; 9: 151–65
Fonseca VA, Valiquett TR, Huang SM, et al. Troglitazone monotherapy improves glycemic control in patients with type 2 diabetes mellitus: a randomized, controlled study. J Clin Endocrinol Metab 1998; 83: 3169–76
Kumar S, Boulton AJM, Beck-Nielsen H, et al. Troglitazone, an insulin action enhancer, improves metabolic control in NIDDM patients. Diabetologia 1996 Jun; 39: 701–9
Leutenegger M, Sacca L, Alderton C, et al. Double-masked, placebo-controlled, dose-ranging study of troglitazone 10 to 200 mg once daily in non—insulin-dependent diabetes mellitus. Curr Ther Res Clin Exp 1997 Jul; 58: 403–16
Fujiwara T, Yoshioka S, Yoshioka T, et al. Characterization of new oral antidiabetic agent CS-045. Studies in KK and ob/ob mice and Zucker fatty rats [in English]. Diabetes 1988 Nov; 37: 1549–58
Fürnsinn C, Neschen S, Noe C, et al. Acute non-insulin-like stimulation of rat muscle glucose metabolism by troglitazone in vitro. Br J Pharmacol 1997 Dec; 122: 1367–74
Kreutter DK, Andrews KM, Gibbs EM, et al. Insulin-like activity of new antidiabetic agent CP68722 in 3T3-L1 adipocytes. Diabetes 1990; 39: 1414–9
Lee MK, Olefsky JM. Acute effects of troglitazone on in vivo insulin action in normal rats. Metabolism 1995 Sep; 44: 1166–9
Okuno A, Ikeda K, Shiota M, et al. Acute effect of troglitazone on glucose metabolism in the absence or presence of insulin in perfused rat hindlimb. Metabolism 1997 Jun; 46: 716–21
Park KS, Ciaraldi TP, Abrams-Carter L, et al. Troglitazone regulation of glucose metabolism in human skeletal muscle cultures from obese type II diabetic subjects. J Clin Endocrinol Metab 1998 May; 83: 1636–43
Szalkowski D, White-Carrington S, Berger J, et al. Antidiabetic thiazolidinediones block the inhibitory effect of tumor necrosis factor-α on differentiation, insulin-stimulated glucose uptake, and gene expression in 3T3-L1 cells. Endocrinology 1995 Apr; 136: 1474–81
Cominacini L, Garbin U, Pastorino AM, et al. Effects of troglitazone on invitrooxidation of LDL and HDL induced by copper ions and endothelial cells. Diabetologia 1997 Feb; 40: 165–72
Steinberg D. Lewis A. Conner Memorial Lecture. Oxidative modification of LDLandatherogenesis. Circulation 1997; 95: 1062–71
Jiang C, Ting AT, Seed B. PPAR-γ agonists inhibit production of monocyte inflammatory cytokines. Nature 1998 Jan 1; 391: 82–6
Tontonoz P, Nagy L, Alvarez JG, et al. PPARgamma promotes monocyte/macrophage differentiation and uptake of oxidized LDL. Cell 1998; 93(2): 241–52
Nagy L, Tontonoz P, Alvarez JG, et al. Oxidized LDLregulates macrophage gene expression through ligand activation of PPARgamma. Cell 1998; 93(2): 229–40
Inoue I, Katayama S, Takahashi K, et al. Troglitazone has a scavenging effect on reactive oxygen species. Biochem Biophys Res Commum 1997; 235: 113A-6A
Miles PDG, Romeo OM, Higo K, et al. TNF-α-induced insulin resistance in vivo and its prevention by troglitazone. Diabetes 1997 Nov; 46: 1678–83
Cominacini L, Young MMR, Capriati A, et al. Troglitazone increases the resistance of low density lipoprotein to oxidation in healthy volunteers. Diabetologia 1997 Oct; 40: 1211–8
Cominacini L, Garbin U, Fratta-Pasini A, et al. Troglitazone reduces LDL oxidation and lowers plasma E-selectin concentration in NIDDM patients. Diabetes 1998 Jan; 47: 130–3
Tack CJJ, Smits P, Demacker PNM, et al. Troglitazone decreases the proportion of small, dense LDL and increases the resistance of LDL to oxidation in obese subjects. Diabetes Care 1998 May; 21: 796–9
Hwang S-J, Ballantyne CM, Sharrett AR, et al. Circulating adhesion molecules VCAM-1, ICAM-1 and E-selectin in carotid atherosclerosis and incident coronary heart disease cases. The Atherosclerosis Risk in Communities (ARIC) Study. Circulation 1997; 96: 4219–25
Fujiwara T, Okuno A, Yoshioka S, et al. Suppression of hepatic gluconeogenesis in long-term troglitazone treated diabetic KK and C57BL/KsJ-db/db mice. Metabolism 1995 Apr; 44: 486–90
Horikoshi H, Fujiwara T, Yoshioka T, et al. Pharmacological characteristics of new antidiabetic agent CS-045 in diabetic animals. In: Shafrir E, editor. Frontiers in diabetes research. Lessons from animal diabetes III.: Smith-Gordon, 1990: 320-4
Inoue I, Takahashi K, Katayama S, et al. Effect of troglitazone (CS-045) and bezafibrate on glucose tolerance, liver glycogen synthase activity, and β-oxidation in fructose-fed rats. Metabolism 1995 Dec; 44: 1626–30
Khoursheed M, Miles PD, Gao KM, et al. Metabolic effects of troglitazone on fat-induced insulin resistance in the rat. Metabolism 1995 Nov; 44: 1489–94
Lee M-K, Miles PDG, Khoursheed M, et al. Metabolic effects of troglitazone on fructose-induced insulin resistance in the rat. Diabetes 1994 Dec; 43: 1435–9
Yagi N, Takasu N, Higa S, et al. Effect of troglitazone, a new oral antidiabetic agent, on fructose-induced insulin resistance. Horm Metab Res 1995 Oct; 27: 439–41
Nagai T, Yasunami Y, Nagata N, et al. Amelioration of hyperglycemia in streptozotocin-induced diabetic rats receiving a marginal mass of islet grafts by troglitazone, an oral antidiabetic agent. Pancreas 1996; 13(4): 381–7
Tominaga M, Igarashi M, Daimon M, et al. Thiazolidinediones (AD-4833 and CS-045) improve hepatic insulin resistance in streptozotocin-induced diabetic rats. Endocr J 1993 Jun; 40: 343–9
Fujiwara T, Wade M, Fukuda K, et al. Characterization of SC-045, a new oral antidiabetic agent. II. Effects on glycemic control and pancreatic islet structure at a late stage of the diabetic syndrome in C57BL/KSJ-db/db mice. Metabolism 1991; 40: 1213–8
Prigeon RL, Kahn SE, Porte JD. Effect of troglitazone on B cell function, insulin sensitivity, and glycemic control in subjects with type 2 diabetes mellitus. J Clin Endocrinol Metab 1998 Mar; 83: 819–23
Inzucchi SE, Maggs DG, Spollett GR, et al. Efficacy and metabolic effects of metformin and troglitazone in type II diabetes mellitus. N Engl J Med 1998 Mar 26; 338: 867–72
Maggs DG, Buchanan TA, Burant CF, et al. Metabolic effects of troglitazone monotherapy in type 2 diabetes mellitus: a randomized, double-blind, placebo-controlled trial. Ann Intern Med 1998 Feb 1; 128: 176–85
Suter SL, Nolan JJ, Wallace P, et al. Metabolic effects of new oral hypoglycemic agent CS-045 in NIDDM subjects. Diabetes Care 1992 Feb; 15: 193–203
Nolan JJ, Ludvik B, Beerdsen P, et al. Improvement in glucose tolerance and insulin resistance in obese subjects treated with troglitazone. N Engl J Med 1994 Nov 3; 331: 1188–93
Loi C-M, Young M, Randinitis E, et al. Clinical pharmacokinetics of troglitazone. Ann Arbor (MI): Department of Pharmacokinetics, Dynamics and Metabolism, Parke-Davis Pharmaceutical Research Division, Warner-Lambert Company, 1999. (Data on file)
Parke-Davis. Rezulin (troglitazone) tablets. Prescribing information. Morris Plains, New Jersey, USA: Parke-Davis, 1997
Shibata H, Nii S, Kobayashi M, et al. Phase I study of a new hypoglycemic agent CS-045 in healthy volunteers. Safety and pharmacokinetics in single administration [in Japanese]. Rinsho Iyaku 1993; 9(7): 1503–18
Young MA, Williams ZV, Eastmond R. Similar pharmacokinetics of troglitazone in young and elderly subjects [abstract]. Diabetologia 1996 Aug; 39 Suppl. 1: A233
Loi C-M, Randinitis EJ, Vassos AB, et al. Lack of effect of type II diabetes on the pharmacokinetics of troglitazone in a multiple-dose study. J Clin Pharmacol 1997 Dec; 37: 1114–20
Kawai K, Kawasaki-Tokui Y, Odaka T, et al. Disposition and metabolism of the new oral antidiabetic drug troglitazone in rats, mice and dogs. Arzneimittel Forschung 1997 Apr; 47: 356–68
Shibukawa A, Sawada T, Nakao C, et al. High-performance frontal analysis for the study of protein binding of troglitazone (CS-045) in albumin solution and in human plasma. J Chromatogr A 1995 Apr 21; 697: 337–43
Yamanouchi T, Shinohara T, Tagaya T, et al. Pharmacokinetics study of a new oral hypoglycemic agent CS-045 in patients with non-insulin dependent diabetes mellitus [in Japanese]. Rinsho Iyaku 1995; 11(11): 2325–39
Ott P, Ranek L, Young MA. Pharmacokinetics of troglitazone, a PPAR-γ agonist, in patients with hepatic insufficiency. Eur J Clin Pharmacol 1998; 54: 567–71
Young MA, Lettis S, Eastmond R. Improvement in the gastrointestinal absorption of troglitazone when taken with, or shortly after, food. Br J Clin Pharmacol 1998 Jan; 45: 31–5
Dunaif A, Scott D, Finegood D, et al. The insulin-sensitizing agent troglitazone improves metabolic and reproductive abnormalities in the polycystic ovary syndrome. J Clin Endocrinol Metab 1996 Sep; 81: 3299–306
Ehrmann DA, Schneider DJ, Sobel BE, et al. Troglitazone improves defects in insulin action, insulin secretion, ovarian steroidogenesis, and fibrinolysis in women with polycystic ovary syndrome. J Clin Endocrinol Metab 1997 Jul; 82: 2108–16
Izumino K, Sakamaki H, Ishibashi M, et al. Troglitazone ameliorates insulin resistance in patients with Werner’s syndrome. J Clin Endocrinol Metab 1997 Aug; 82: 2391–5
Takino H, Okuno S, Uotani S, et al. Increased insulin responsiveness after CS-045 treatment in diabetes associated with Werner’s syndrome. Diabetes Res Clin Pract 1994 Jul; 24: 167–72
Karam JH, Salber PR, Forsham PH. Pancreatic hormones & diabetes mellitus. In: Greenspan FS, editor. Basic and clinical endocrinology. 3rd ed. Morwalk (CT): Appleton & Lange, 1991: 592–650
Reaven GM. Role of insulin resistance in human disease. Diabetes 1988; 37: 1595–607
Després J-P, Lamarche B, Mauriège P, et al. Hyperinsulinemia as an independent risk factor for ischemic heart disease. N Engl J Med 1996; 334: 952–7
Hansen AP, Troglitazone Study Group. Effects of troglitazone, a thiazolidinedione, in elderly non-insulin-dependent diabetic patients [abstract]. Diabetologia 1995; 38 Suppl. 1: A200
Kumar S, Prange A, Schulze J, et al. Troglitazone, an insulin action enhancer, improves glycaemic control and insulin sensitivity in elderly type 2 diabetic patients. Diabetic Med 1998; 15: 772–9
Okamoto M, Okamoto M, Taniguchi T, et al. Efficacy of troglitazone in young and elderly patients with NIDDM [abstract]. Diabetes 1998 May; 47 Suppl. 1: A97
Claudi T, Starkie M, Frith L, et al. Troglitazone improves cardiovascular risk profile compared with glibenclamide [abstract]. Diabetic Med 1997; 14 Suppl. 4: 30
Ghazzi MN, Perez JE, Antonucci TK, et al. Cardiac and glycemic benefits of troglitazone treatment in NIDDM. Diabetes 1997 Mar; 46: 433–9
Levin K, Thye-Rønn P, Foot E, et al. Metabolic effects of troglitazone in NIDDM patients [abstract]. Diabetes 1996 May; 45 Suppl. 2: 18A
Robinson ACJ, Gray RG, Bannister PA, et al. The effects of troglitazone on lipolysis, fatty acid mobilization, and glucose turnover in NIDDM [abstract]. Diabetic Med 1998; 15 Suppl. 1: S66
Rosinson ACJ, Gray RG, Bannister PA, et al. Troglitgazone (600 mg daily) reduces the rate of very low density synthesis and pool size in patients with NIDDM [abstract]. Diabetic Med 1998; 15 Suppl. 1: S29
Serrano-Rios M, Kler L, Frith L, et al. Troglitazone improves insulin resistance compared to metformin [abstract]. Diabetic Med 1997; 14 Suppl. 4: 22
Sironi AM, Vichi S, Gastaldelli A, et al. Effects of troglitazone on insulin action and cardiovascular risk factors in patients with non-insulin-dependent diabetes. Clin Pharmacol Ther 1997 Aug; 62: 194–202
Troglitazone Study Group. The metabolic effects of troglitazone in non-insulin dependent diabetes [abstract]. Diabetologia 1997 Jun; 40 Suppl. 1: 149A
Valiquett T, Balagtas C, Whitcomb R. Troglitazone dose-response study in patients with NIDDM [abstract]. Diabetes 1995 May; 44 Suppl. 1: 109A
Valiquett T, Huang S, Ghazzi M. Troglitazone monotherapy: long term efficacy in patients with type 2 diabetes [abstract]. Diabetes 1998; 47 Suppl. 1: A17
Akanuma Y, Kosaka K, Kuzuya T. Long-term study of a new oral hypoglycemic agent CS-045 in patients with non-insulin dependent diabetes mellitus [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 127–49
Akanuma Y, Kosaka K, Kuzuya T, et al. Clinical evaluation of a new oral hypoglycemic agent CS-045 in patients with non-insulin dependent diabetes mellitus poorly controlled by diet alone. A dose-finding study by dose increasing method [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 19–37
Ikeda Y, Yamada H, Ohno M. Clinical evaluation of a new oral hypoglycemic drug, CS-045, in patients with obese non-insulin dependent diabetes mellitus [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 179–90
Iwamoto Y, Kuzuya T, Matsuda A, et al. Effect of new oral antidiabetic agent CS-045 on glucose tolerance and insulin secretion in patients with NIDDM. Diabetes Care 1991 Nov; 14: 1083–6
Iwamoto Y, Kosaka K, Kuzuya T, et al. Effects of troglitazone: a new hypoglycemic agent in patients with NIDDM poorly controlled by diet therapy. Diabetes Care 1996 Feb; 19: 151–6
Kuzuya T, Iwamoto Y, Kosaka K, et al. An early phase II clinical trial of a new oral hypoglycemic drug, CS-045, in patients with non-insulin dependent diabetes mellitus [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 3–18
Maruyama H, Hirose H, Shimada A, et al. Clinical evaluation of a new oral hypoglycémie agent CS-045 in patients with non-insulin dependent diabetes mellitus. Study with 100mg tablet [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 205–15
Mimura K, Umeda F, Hiramatsu S, et al. Effects of a new oral hypoglycaemic agent (CS-045) on metabolic abnormalities and insulin resistance in type 2 diabetes. Diabetic Med 1994 Aug–Sep; 11: 685–91
Nakano K, Yasuda T, Kitagawa Y, et al. Clinical evaluation of a new oral hypoglycemic drug, CS-045, on daily profile of blood glucose in patients with non-insulin dependent diabetes mellitus [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 151–64
Ogihara T, Rakugi H, Ikegami H, et al. Enhancement of insulin sensitivity by troglitazone lowers blood pressure in diabetic hypertensives. Am J Hypertens 1995 Mar; 8: 316–20
Yamada N, Akanuma Y, Murase T, et al. Clinical evaluation of a new oral hypoglycemic drug CS-045 in patients with non-insulin dependent diabetes mellitus accompanying hypertriglyceridemia [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 165–78
Young MA, Eckland DJA, Eastmond R. Establishing the dose response curve for metabolic control with troglitazone, an insulin action enhancer, in type 2 diabetes patients. Ann Med 1998 Apr; 30: 206–12
Kuzuya T, Kosaka K, Akanuma Y, et al. Baseline factors affecting the efficacy of troglitazone on plasma glucose in Japanese patients with non-insulin-dependent diabetes mellitus. Diabetes Res Clin Pract 1998; 41: 121–9
Draznin B, Driscoll J, Sievers J, et al. Troglitazone plus sulfonylurea combination: long term efficacy in patients with type 2 diabetes [abstract]. Diabetes 1998 May; 47 Suppl. 1: A85
Foot EA, Patel J, Williams ZV, et al. Improved metabolic control by addition of troglitazone to glibenclamide therapy in non-insulin-dependent diabetics [abstract]. Diabetologia 1995 Aug; 38 Suppl. 1: A44
Horton ES, Whitehous F, Ghazzi MN, et al. Troglitazone in combination with sulfonylurea restores glycemic control in patients with type 2 diabetes. Diabetes Care 1998; 21(9): 1462–9
Akanuma Y, Kosaka K, Kuzuya T, et al. Clinical evaluation of a new oral hypoglycemic agent CS-045 in patients with non-insulin dependent diabetes mellitus poorly controlled by sulfonylureas. A dose-finding study by dose increasing method [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 39–60
Iwamoto Y, Kosaka K, Kuzuya T, et al. Effect of combination therapy of troglitazone and sulphonylureas in patients with type 2 diabetes who were poorly controlled by sulphonylurea therapy alone. Diabetic Med 1996 Apr; 13: 365–70
Scino Y, Ishida H, Kurahachi H, et al. Clinical evaluation of a new oral hypoglycemic drug CS-045 in patients with non-insulin dependent diabetes mellitus poorly controlled with sulfonylureas. Study with 100mg tablet [in Japanese]. Rinsho Iyaku 1993; 9 Suppl. 3: 191–203
Schwartz S, Raskin P, Fonseca V, et al. Effect of troglitazone in insulin-treated patients with type II diabetes mellitus. Troglitazone and Exogenous Insulin Study Group. N Engl J Med 1998 Mar 26; 338: 861–6
Buse JB, Gumbiner B, Mathias NP, et al. Troglitazone use in insulin-treated type 2 diabetic patients. Diabetes Care 1998; 21: 1455–61
Fonseca V, Graveline J, Nissel J. Long term experience with troglitazone in combination with insulin in type 2 diabetes mellitus [abstract]. Diabetes 1998 May; 47 Suppl. 1: A90
Akanuma Y, Kosaka K, Toyoda T, et al. Clinical evaluation of a new oral hypoglycemic agent CS-045 in combination with insulin [abstract]. Diabetologia 1996 Aug; 39 Suppl. 1: A232
Fukuda T, Nakano O, Amano M, et al. Aclinical study of a new hypoglycemic agent, troglitazone, in type 2 diabetes patients who are unsatisfactorily-controlled with insulin [in Japanese]. Rinsho Iyaku 1995; 11(10): 2055–62
Harris MI. Impaired glucose tolerance in the U.S. population. Diabetes Care 1989; 12: 464–74
Kjos SL, Peters RK, Xiang A, et al. Predicting future diabetes in Latino women with gestational diabetes. Utility of early postpartum glucose tolerance teting. Diabetes 1995; 44: 586–91
Yamada T, Aizawa T, Nagasawa Y, et al. Ten-year follow-up of Japanese overweight subjects with impaired glucose tolerance: identification of a diabetes-prone subpopulation. Intern Med 1992; 31: 877–84
Antonucci T, Whitcomb R, McLain R, et al. Impaired glucose tolerance is normalized by treatment with the thiazolidinedione troglitazone. Diabetes Care 1997 Feb; 20: 188–93
Berkowitz K, Peters R, Kjos SL, et al. Effect of troglitazone on insulin sensitivity and pancreatic β-cell function in women at high risk for NIDDM. Diabetes 1996 Nov; 45: 1572–9
Driscoll J, Ghazzi M, Perez J, et al. A 96-week follow-up on cardiac safety in patients with type II diabetes treated with troglitazone [abstract]. Diabetes 1997 May; 46 Suppl. 1: 149A
Diabetes Drug Pulled Back in UK [online]. Available from: URL: http://www.newspage.com/cgi-bin/pnp [Accessed 1997 Dec 4]
Glaxo Wellcome suspends troglitazone availability. Marketletter 1997 Dec 8; 24: 21
Warner Lambert Press Releases. Response of Parke-Davis to public citizen health research group’s petition regarding rezulin (troglitazone) tablets. Available from URL: http://www.warner-lambert.com/rezulin.html [Accessed 1999 Jan 13]
FDA Talk Paper [online]. Available from: URL: http://www.fda.gov/bbs/topics/ANSWERS/ANS00831.html [Accessed 1997 Nov 7]
Liver damage warnings for troglitazone. Scrip 1997 Nov 7 (2282): 21
FDA warns about diabetes drug [online]. Available from: URL: http://www.newspage.com/cgi-bin/pnp [Accessed 1997 Dec 4]
Rezulin under renewed fire as label changes. Marketletter 1998 Aug 3; 25: 19
Kuramoto K, Shimizu N, Toda G. Liver dysfunction associated with troglitazone (Noscal) [in Japanese]. Rinsho Iyaku 1998; 14(3): 461–6
Vella A, de Groen PC, Dinneen SF. Fatal hepatotoxicity associated with troglitazone [letter]. Ann Intern Med 1998; 129(12): 1080
Warner-Lambert Rezulin arm in NIH diabetes prevention trial is being retained; Glaxo troglitazone withdrawal in U.K. prompts re-evaluation of U.S. status. FDC Pink 1997 Dec 8; 59: 5–6
Call to ban troglitazone in US. Scrip 1998 Jul 31 (2357): 22
Rezulin monitoring program to be watched closely at FDA -Woodcock. Pink Sheet 1999 Jan 4; 61 (1): 14-5
Kaplan B, Friedman G, Jacobs M, et al. Potential interaction of troglitazone and cyclosporine. Transplantation 1998 May 27; 65: 1399–400
Loi C-M, Knowlton PW, Stern R, et al. Effect of troglitazone on steady-state pharmacokinetics of digoxin. J Clin Pharmacol 1998 Feb; 38: 178–83
Burgess SJ, Singer GG, Brennan DC. Effect of troglitazone on cyclosporine whole blood levels. Transplantation 1998 Jul 27; 66: 272
Frantz RP. Rezulin (troglitazone) greatly increases cyclosporine metabolism [letter]. J Heart Lung Transplant 1998; 17(10): 1037–8
Park MH, Pelegrin D, Haug III MT, et al. Troglitazone, a new antidiabetic agent, decreases cyclosporine level [letter]. J Heart Lung Transplant 1998; 17(11): 1139–40
Püchler K, Sasahara K, Witte PU, et al. Lack of pharmacokinetic interaction between troglitazone and glibenclamide in NIDDM patients [abstract]. Diabetologia 1996 Aug; 39 Suppl. 1: A232
Plowman BK, Morreale AR Possible troglitazone-warfarin interaction. Am J Health System Pharm 1998 May 15; 55: 1071
Foot EA, Eastmond R. Good metabolic and safety profile of troglitazone alone and following alcohol in NIDDM subjects. Diabetes Res Clin Pract 1997 Oct; 38: 41–51
Young MA, Lettis S, Eastmond R. Concomitant administration of cholestyramine influences the absorption of troglitazone. Br J Clin Pharmacol 1998 Jan; 45: 37–40
Young MA, Lettis S, Eastmond R. Coadministration of acetaminophen and troglitazone: pharmacokinetics and safety. J Clin Pharmacol 1998; 38: 819–24
Koup JR, Anderson G, Loi CM. Effect of troglitazone on urinary excretion of cortisol and 6-β-hydroxycortisol. J Clin Pharmacol 1998; 38: 815–8
Fleishaker JC, Pearson LK, Peters GR. Phenytoin causes a rapid increase in 6-β-hydroxycortisol urinary excretion in humans - a putative measure of CYP3A induction. J Pharm Sci 1995; 84: 292–4
Ged C, Rouillon JM, Pichard L, et al. The increase in urinary excretion of 6-beta-hydroxycortisol as a marker of human hepatic cytochrome P450IIIA induction. Br J Clin Pharmacol 1989; 28: 373–87
Lloyd AC, Williams Z, Lacey LA, et al. Impact of type II diabetes on employment status and work productivity [abstract no. 761]. Diabetologia 1996 Suppl. 1: A201
Warner DC, McCandless RR, De Nino LA, et al. Costs of diabetes in Texas, 1992. Diabetes Care 1996 Dec; 19: 1416–9
Troglitazone for non-insulin-dependent diabetes mellitus. Med Lett Drugs Ther 1997 May 23; 39: 49–51
Petrie J, Small M, Connell J. Glitazones, a prospect for non-insulin-dependent diabetes. Lancet 1997 Jan 11; 349: 70–1
O’Shea SJ, Lloyd AC, Keech ML, et al. Costs of hypoglycaemia in type II diabetics treated with oral hypoglycaemic agents [abstract no. 871]. Diabetologia 1996 Suppl. 1: A230
Balfour JA, Clissold SP. Management of non—insulin-dependent diabetes mellitus: defining the role of metformin. Dis Manage Health Outcomes 1997 Jan; 1: 49–59
Johnson MD, Campbell LK, Campbell RK. Troglitazone: review and assessment of its role in the treatment of patients with impaired glucose tolerance and diabetes mellitus. Ann Pharmacother 1998 Mar; 32: 337–48
Sartor G, Schertsten B, Carlstrom S, et al. Ten-year follow-up of subjects with impaired glucose tolerance: prevention of diabetes by tolbuamide and diet regulation. Diabetes 1980; 29(1): 41–9
Yoshioka K, Yokoo S, Yoshida T, et al. Is troglitazone a real indication for obese subjects with impaired glucose tolerance? [letter]. Diabetes Care 1997 Aug; 20: 1340–1
Whitcomb R. Is troglitazone a real indication for obese subjects with impaired glucose tolerance? Reply [letter]. Diabetes Care 1997 Aug; 20: 1341
US NIH halts Rezulin trial for diabetes prevention. Marketletter 1998 Jun 15; 25: 21
Author information
Authors and Affiliations
Corresponding author
Additional information
Various sections of the manuscript reviewed by: A. Anwar, Department of Medicine, Birmingham Heartlands Hospital, Birmingham, England; R. Bressler, College of Medicine, University of Arizona, Tucson, Arizona, USA; L. Cominacini, Istituto di Semeiotica e Nefrologia Medica, Università di Verona, Ospedale Policlinico, Verona, Italy; J.C.N. Corrêa, Serviço de Endocrinologia, Hospital Curry Cabral, Lisbon, Portugal; C. Fürnsinn, Department of Medicine III, Division of Endocrinology and Metabolism, University of Vienna, Vienna, Austria; I. Inoue, Fourth Department of Internal Medicine, Saitama Medical School, Saitama, Japan; S.E. Inzucchi, Section of Endocrinology, Yale University School of Medicine, New Haven, Connecticut, USA; S. Kumar, Department of Medicine, Birmingham Heartlands Hospital, Birmingham, England; M. Leutenegger, Clinique Médicale, Hôpital Robert Debré, Reims, France; J.R. Petrie, Department of Medicine and Therapeutics, Western Infirmary, Glasgow, Scotland; M. Tominaga, Department of Laboratory Medicine, Yamagata University School of Medicine, Yamagata, Japan.
Data Selection
Sources: Medical literature published in any language since 1966 on troglitazone, identified using AdisBase (a proprietary database of Adis International, Auckland, New Zealand), Medline and EMBASE. Additional references were identified from the reference lists of published articles. Bibliographical information, including contributory unpublished data, was also requested from the company developing the drug.
Search strategy: AdisBase search terms were ‘troglitazone’, ‘CI-991’, ‘CS-045’, ‘GR-92132’ and ‘GR-92132X’. Medline and EMBASE search terms were ‘troglitazone’, ‘CI-991’, ‘CS-045’, ‘GR-92132’, ‘GR-92132X’ and ‘97322-887-7’. Searches were last updated 11 February 1999.
Selection: Studies in patients with type 2 diabetes mellitus or impaired glucose tolerance who received troglitazone. Inclusion of studies was based mainly on the methods section of the trials. When available, large, well controlled trials with appropriate statistical methodology were preferred. Relevant pharmacodynamic and pharmacokinetic data are also included.
Index terms: Troglitazone, thiazolidinediones, diabetes mellitus, insulin resistance, pharmacodynamics, pharmacokinetics, therapeutic use.
Rights and permissions
About this article
Cite this article
Plosker, G.L., Faulds, D. Troglitazone. Drugs 57, 409–438 (1999). https://doi.org/10.2165/00003495-199957030-00014
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-199957030-00014